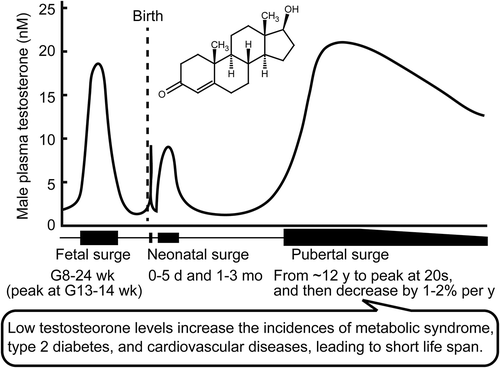
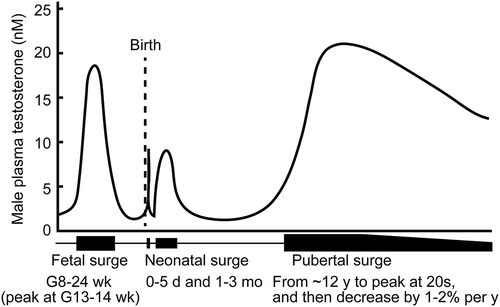
Figures & data
Table 1. Summary of meta-analyses and a large-cohort studies of testosterone and metabolic disorders.
Table 2. Summary of the metabolic changes in androgen receptor knockout male mice.