Figures & data
Figure 1 Schematic diagram of subtypes of lung macrophages during allergic immune responses after exposure to allergen.
Notes: Exposure to allergens activates lung epithelial cells and other innate immune cells. The activated cells release a variety of cytokines and distinctly affect AM polarization and migration. Classically activated macrophages (M1 cells) can be activated by IFN-γ and LPS, inducing nonallergic immune responses through releasing TNF-α and IL-1 β. Alternatively, activated macrophages (M2 cells) are divided into M2a and M2c cells. M2a cells can be activated by IL-4, IL-13, and IL-33, inducing allergic immune responses through releasing IL-4 and IL-13. M2c cells can be activated by IL-10 and TGF-β, inducing lung inflammation resolution and tissue repair through releasing IL-10. Bone marrow-derived stromal cells and regulatory T cells also drive M2c cell polarization through IDO and IL-10. M2c cells have low activation markers and are more potent in phagocytosis of invading pathogens than other macrophage phenotypes.
Abbreviations: AM, alveolar macrophage; LPS, lipopolysaccharide; IDO, indoleamine 2,3-dioxygenase.
Abbreviations: AM, alveolar macrophage; LPS, lipopolysaccharide; IDO, indoleamine 2,3-dioxygenase.
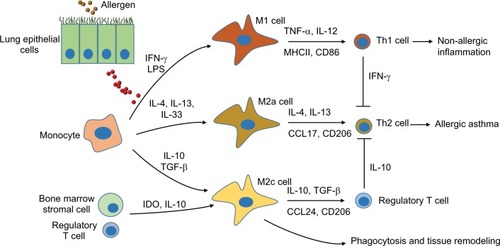
Table 1 Characteristics and molecular release from activated macrophages
