Abstract
Personnel in swimming pool facilities typically experience ocular, nasal, and respiratory symptoms due to water chlorination and consequent exposure to disinfection by-products in the air. The aim of the study was to investigate exposure to trichloramine and trihalomethanes (chloroform, bromodichloromethane, dibromochloromethane, and bromoform) from the perspective of adverse health effects on the personnel at Swedish habilitation and rehabilitation swimming pools. The study included 10 habilitation and rehabilitation swimming pool facilities in nine Swedish cities. The study population comprised 24 exposed swimming pool workers and 50 unexposed office workers. Personal and stationary measurements of trichloramine and trihalomethanes in air were performed at all the facilities. Questionnaires were distributed to exposed workers and referents. Spirometry, fraction of exhaled nitric oxide (FENO), and peak expiratory flow (PEF) were measured. Personal and stationary measurements yielded trichloramine levels of 1–76 µg/m3 (average: 19 µg/m3) and 1–140 µg/m3 (average: 23 µg/m3), respectively. A slightly higher, but not significant, prevalence of reported eye- and throat-related symptoms occurred among the exposed workers than among the referents. A significantly increased risk of at least one ocular symptom was attributed to trichloramine exposure above the median (20 µg/m3). Lung function (FVC and FEV1) was in the normal range according to the Swedish reference materials, and no significant change in lung function before and after shift could be established between the groups. Average FENO values were in the normal range in both groups, but the difference in the values between the exposed workers and referents showed a significant increase after shift. Hourly registered PEF values during the day of the investigation did not show any unusual individual variability. In conclusion, the increased risk of developing at least one ocular symptom at personal trichloramine concentrations over 20 µg/m3 combined with an increase in the difference in FENO during the work shift of the exposed workers should not be neglected as an increased risk of respiratory inflammation in the habilitation and rehabilitation swimming pool environment.
Introduction
Owing to its positive health effects, aquatic therapy is used for rehabilitation and habilitation purposes. Exercising in water is beneficial because the water is weight bearing, promotes relaxation, increases the range of motion, and reduces the risk of injury compared with exercising on land.[Citation1] Most Swedish county councils offers aquatic therapy in indoor swimming pools where physical therapists and assistant nurses treat patients individually or in groups. Compared with conventional indoor swimming pools, habilitation and rehabilitation pool facilities are often smaller and have a higher water temperature for therapeutic purposes.
The water in indoor swimming pools is commonly chlorinated to prevent the spread of pathogens. In the disinfection process, chlorine can react with nitrogen-containing organic matter (such as urea, sweat, dandruff, and skin flakes), forming unwanted by-products, such as mono-, di-, and trichloramines.[Citation2,Citation3] Trichloramine (NCl3) is the most volatile chloramine and thus most likely to be found at the highest concentration in indoor swimming pool air, leading to exposure by inhalation.[Citation4] Trihalomethanes (THMs) constitute another group of by-products formed when chlorine reacts with organic materials in swimming pool water.[Citation5] Chloroform (CHCl3), bromodichloromethane (CHCl2Br), dibromochloromethane (CHClBr2), and bromoform (CHBr3) are the most common THMs in swimming pool atmospheres.[Citation5–7] THM exposure occurs mainly via inhalation, but dermal uptake may also occur.[Citation8] The emission of unwanted by-products from the pool water into the indoor air depends on different factors such as the concentration in the water and their volatility, the number of bathers and their behavior, ventilation, water temperature and water circulation.[Citation2,Citation9–12]
The International Agency for Research on Cancer (IARC) has classified chloroform and bromodichloromethane as possibly carcinogenic to humans (group 2B).[Citation13] Moreover, the threshold limit value (TLV) set by the American Conference of Governmental Industrial Hygienists (ACGIH®) and the Swedish occupational exposure limit value (OEL) for chloroform are 50,000 µg/m3 and 10,000 µg/m3,[Citation14,Citation15] respectively.
Personnel in swimming pool facilities typically experience ocular and respiratory symptoms.[Citation11,Citation16–19] Irritative ocular and upper airway symptoms among swimming pool employees have been associated with varying levels of trichloramine, namely, 17–150 µg/m3[Citation20] and 200–300 µg/m3.[Citation21] Swimming pool workers have also experienced symptoms associated with the lower respiratory tract and an increased risk of asthma.[Citation22] Trichloramine levels of 100 or 570 µg/m3 have been associated with work-related asthma in personnel working at indoor swimming pools.[Citation12] Trichloramine exposure and the occurrence of asthma among swimming pool employees have also been described by Rosenman, Millerick-May, and Reilly et al.[Citation23]
At present, there is no OEL for trichloramine adopted in Sweden. The World Health Organization[Citation24] proposed a reference value of 500 µg/m3 for trichloramine in indoor swimming pools. Parrat, Donze, Iseli, Perret, Tomicic, and Schenk[Citation21] suggested an exposure limit of 300 µg/m3 for trichloramine in indoor swimming pool air, and France adopted the same level for trichloramine exposure.[Citation25] OELs have traditionally been based on personal measurements, but reference values for trichloramine have, to date, been based on stationary measurements. Westerlund, Graff, Bryngelsson, Westberg, Eriksson, and Lofstedt[Citation26] examined the relationship between personal and stationary sampling of trichloramine and found that during personal measurements, worker exposure was approximately half as high as that associated with stationary measurements.
The aim of the study was to investigate the exposure to trichloramine and THMs in habilitation and rehabilitation swimming pools from the perspective of adverse health effects on the personnel at these premises. Personal and stationary measurements of trichloramine and THMs were performed, and the occurrence of ocular, nasal, and respiratory symptoms as well as lung function, nitric monoxide (NO) in the exhaled air, and peak expiratory flow (PEF) were investigated. The relation between personal and stationary measurements was also analyzed to validate the relation stated by Westerlund, Graff, Bryngelsson, Westberg, Eriksson, and Lofstedt.[Citation26]
Methods
Study design
A cross-sectional study design was used to investigate air concentrations of trichloramine and THMs and a possible correlation with ocular, nasal, and respiratory symptoms among employees in Swedish habilitation and rehabilitation swimming pools. Personal and stationary measurements of these concentrations and medical examinations were performed on the same day in the swimming pool facilities. Exposed swimming pool workers and unexposed office workers (see “Study Population”) completed a questionnaire and performed spirometry and nitric monoxide (NO) measurements in exhaled air before and after a work shift. The swimming pool employees also underwent PEF measurements once every hour during the day of the investigation. Sensitization to inhalable allergens was examined via Phadiatop analysis.
Facilities
The study included 10 habilitation and rehabilitation swimming pool facilities in nine Swedish cities and was performed from 2012–2014. Each facility had one to two swimming pools with sizes of 15–100 m2 and a water temperature of 31–34 °C. The water in each pool was disinfected with calcium or sodium hypochlorite. As a complement to hypochlorite, seven out of 10 facilities used ultraviolet (UV) light, and one used ozone. UV light and ozone disinfection was conducted in a closed system in a delimited room outside the pool area. The main activities offered in the facilities were physiotherapy and flexibility training as an individual or group activity.
Study population
The criterion for inclusion in the study was that the employee worked for at least 4 hr per day in the swimming pool facility (equivalent to at least 50% of their workday). On the day of the investigation, 24 swimming pool employees were included in the study as they were working full time (8 hr per day) and had a potential exposure to emissions of chlorinated by-products. The study population consisted of assistant nurses working as habilitation or rehabilitation assistants (n = 22), but an auxiliary nurse and a rehabilitation instructor also worked in the pool area. In addition, most facilities had staff who worked only a few hours per week in the swimming pool area and they were not included in the study. The swimming pool employees executed their work tasks from the pool side and were not required to be in the water during a normal working day. The work tasks in the swimming pool area consisted of helping visitors to get in and out of the water and assist them in their aquatic therapy session. In addition, the swimming pool workers also had administrative duties outside of the pool area. For comparison, 50 unexposed municipal office workers were also included in the study. Exposed swimming pool workers and unexposed office workers are hereafter called exposed workers and referents. The exposed workers were all recruited by study officials at work meetings in the indoor swimming pool facilities, whereas the referent group members were recruited with help from the municipal human resource department. None of the participants had visited an indoor swimming pool facility in the 2 days preceding the investigation.
Exposure assessment
Personal sampling of trichloramine and THM concentrations in air was performed in the breathing zone of exposed workers during an 8-hr day shift (as described below). During the exposure assessment, each worker kept a work diary to provide information about work tasks and duration. Parallel to the personal sampling, stationary air sampling of trichloramine and THMs was performed during an 8-hr day. The stationary samplers were placed at different fixed positions around the pool facilities at ∼1.5 m above the floor level. Stationary sampling was conducted in the reception area and at distances of 0–1 m from the poolside.
Air sampling and analysis of trichloramine
Trichloramine in air was sampled using the method proposed by Hery et al.[Citation2] The three-piece 37-mm closed face plastic cassette contained two glass fiber filters (Whatman Grade QM-A, diameter: 37 mm; Whatman, Maidstone, UK) impregnated with a solution of sodium carbonate and diarsenic trioxide. The second filter was a back-up filter used to determine possible overload of trichloramine on the first filter. To prevent water droplets from contaminating the filters, Hery et al.[Citation2] used a Teflon filter prior to the arsenic impregnated filter. Preliminary tests showed that Teflon filters had no effect on the results in our setup; hence, measurements were performed without the use of these filters. The sampler was attached to a twin-port sampler (MSA Gemini, MSA Inc., Grand Rapids, MI) and connected to an air sampling pump (SKC AirChek 5000, SKC Inc., Eighty Four, PA) with an airflow rate of 0.25 L/min. The maximum sampling time of each sampler was 10 hr.
Trichloramine was collected on the impregnated filters and reduced to chloride ions (Cl−). In the initial stage of the analysis, the sampled filters were placed in a glass beaker desorbed in 10 mL of double distilled water. The beaker was then placed in an ultrasonic bath for 10 min. The solution was then filtered through a 13-mm syringe filter (IC Acrodisc, PALL Corporation, Port Washington, NY), and the chlorides were analyzed in a suppressed ion chromatography system (Triatlon 900 Autosampler, Spark Holland, Emmen, the Netherlands); ICSep AN1, Anion column (CETAC, Omaha, NE); SCX membrane suppressor column (Sequant, Umeå, Sweden); and JD-21 conductivity detector (Costech Microanalytical Ltd., Tallin, Estonia). The eluent consisted of 10 mM NaOH with 25% acetone, and 50 mM H2SO4 was used as the suppressor. Two control samples with chloride concentrations of 0.5 and 3.0 mg/L and at least two blanks were run with the samples. Chloride concentrations detected in the blanks were subtracted from the concentrations in the samples. The limit of detection (LOD) was defined as a signal-to-noise ratio of three.[Citation27] A LOD of 0.213 µg/sample yielded air concentration levels of 0.014–0.002 µg/m3 based on a flow rate of 0.25 L/min and a sampling time of 7–9 hr. Trichloramine was analyzed in the laboratory of the Department of Occupational and Environmental Medicine at Umeå University, Sweden.
Air sampling and analysis of trihalomethanes
The sampling and analysis of THMs in air were based on the EPA method TO-17.[Citation28] Sampling was executed with multibed thermal desorption tubes (Carbotrap 300, PerkinElmer, Waltham, MA) connected to a twin-port sampler (MSA Gemini, MSA Inc., Grand Rapids, MI) and an air sampling pump (SKC AirChek 5000, SKC Inc., Eighty Four, PA) operating at an airflow rate of 0.01 L/min. The maximum sampling time for each tube was 4 hr. When the sampling time reached 4 hr, the tube was replaced by a new one. The sampled tubes were desorbed using an automatic thermal desorption unit (ATD TurboMatrix 650, Perkin Elmer, Waltham, MA) and injected into a gas chromatograph (GC 6890, Hewlett Packard, Pallo Alto, CA). The GC consisted of a Rxi-1 ms column (60 m × 0.25 mm, film thickness: 1.0 µm, Restek Corporation, Bellefonte, PA) and a mass spectrometry detector (MS; 5973, Agilent, Santa Clara, CA). Helium was used as a carrier gas. Each sample was desorbed for 5 min at 250 °C with a helium gas flow of 50 mL/min and cryofocused at -30 °C on a cold trap containing Tenax TA. The sample was then split injected (outlet split, 10 mL/min; desorb flow, 50 mL/min) onto the GC by heating the cold trap to 250 °C for 4 min. The sample was separated in the GC with the following temperature program: 1 min at 30 °C, with 5 °C/min to 125 °C, 15 min isotherm. Detection of the four THMs was made by acquisition in single-ion monitoring (SIM) mode (m/z for chloroform/bromodichloromethane: 82.9, 84.9; dibromochloromethane: 126.8, 128.8; and bromoform: 172.8, 174.8) with the ion source operating at 230 °C and 70 eV. The chromatograms were integrated and evaluated using computer software (G1701DA MSD ChemStation Version D.00.00.38, Agilent Technologies, Santa Clara, CA). The limit of quantification (LOQ) was defined as a signal-to-noise ratio (S/N) of 10.[Citation27] The LOQ for the THMs corresponded to a S/N of >10, except for bromodichloromethane (S/N: 4.7). The LOQ was 0.75 ng/sample for chloroform and 0.10 ng/sample for bromodichloromethane, dibromochloromethane, and bromoform. A flow rate of 0.01 L/min and a sampling time of 4 hr yielded air concentrations of 0.30 µg/m3 for chloroform and 0.04 µg/m3 for bromodichloromethane, dibromochloromethane, and bromoform. The THMs were analyzed in the laboratory of the Department of Occupational and Environmental Medicine at Örebro University Hospital, Sweden. The laboratory has been accredited by the Swedish Board of Accreditation and Conformity Assessment (SWEDAC).
Assessment of adverse health effects
The participants completed a questionnaire on the day of the investigation. Some questions, which were originally stated in English, were translated for use in Swedish studies.[Citation29] The questionnaire consisted of questions covering work tasks, exposure during work and leisure activities, tobacco habits, and health status, focusing on respiratory symptoms. Questions concerning ocular, nasal, and respiratory symptoms during the 12 months, 3 months, and 1 week preceding the investigation were also included.
Lung function was investigated using a hand-held personal computer (PC)-based spirometry flow sensor capable of bi-directional ultrasound transit time analysis (Spirare, Diagnostica, Oslo, Norway) in accordance with the American Thoracic Society guidelines.[Citation30] The exposed group underwent spirometry the day prior to the investigation as well as before and after the following day shift. For the referent group, spirometry was performed only before and after a day shift. The results were expressed as a percentage of the predicted forced vital capacity (FVC) and the forced expiratory volume in 1 sec (FEV1) using gender-specific Swedish reference materials.[Citation31,Citation32]
Exhaled NO concentration was used as an indicator of primarily eosinophilic inflammation in the respiratory tract.[Citation33] The concentration of NO in exhaled air was investigated using a NIOX Mino (Aerocrine AB, Solna, Sweden) with a flow rate of 50 mL/s.[Citation34] The NO measurements in exhaled air were performed immediately before each spirometry procedure and were expressed as a fraction (in parts per billion, ppb) of the exhaled NO (FENO). The normal range of FENO is set to 25–50 ppb.[Citation35] Each subject answered questions regarding factors prior to testing (such as smoking, infections, and recent food intake) that affect FENO concentrations.
The peak expiratory airflow (PEF) of each swimming pool employee was investigated using a Mini Wright Peak Flow Meter (Airmed, London, UK). Every hour, three serial measurements were performed with the individual in an upright position after maximal inhalation. The highest value of the three registered measurements was used in the analysis, and each person served as his or her own control. A diurnal variability of <20% in PEF among adults was considered normal.[Citation36]
ImmunoCAP Phadiatop (Phadia AB, Uppsala, Sweden) was analyzed as an indicator of atopy.[Citation37] Serum immunoglobulin E (IgE)-levels ≥35 kU/l were regarded as positive.
The study was approved by the Regional Ethical Review Board of Uppsala (decision no. 2006/349). Informed consent was obtained from each participant.
Statistical methods
Demographic data from the questionnaire were summarized using descriptive statistics. Categorical variables are expressed as percentages, and continuous variables are expressed in terms of the arithmetic mean (AM), standard deviation (SD), median, and range. Differences in characteristics between the exposed workers and referents were analyzed by chi-square tests for categorical variables, and continuous variables were analyzed by an independent t-test for statistical significance.
Data from samples of trichloramine were divided according to the personal and stationary measurements summarized for each facility. Measured trichloramine concentrations are expressed in terms of the AM, SD, geometric mean (GM), geometric standard deviation (GSD), and range. For air concentrations of trichloramine below the LOD, LOD/√2 was used for the calculations.[Citation38] Comparison of measured air concentrations of trichloramine between the swimming pool facilities was made by a Mann-Whitney U test. Prediction of personal exposure to trichloramine from stationary measurements was made possible by investigating the correlation between personal and stationary sampling of trichloramine via linear regression analysis. In the analysis, the AM of personal trichloramine exposure and the AM of stationary trichloramine sampling from 8-hr measurements conducted in the swimming pool area at each facility were used. Only samples from personnel who spent more than 50% of their workday in the pool area were included and correlated with parallel stationary samples. Personal and stationary measurements of THMs were summarized for all facilities and are expressed in terms of AM. For air concentrations of THMs below the LOQ, LOQ/√2 was used for the calculations.[Citation38] To estimate the correlation between trichloramine and chloroform, a Spearman’s rank-order correlation was performed.
Symptoms reported in the questionnaire were summarized using descriptive statistics and are expressed as percentages. Symptoms reported the last week were also categorized as ocular, nasal or respiratory and are expressed as percentages. The estimation of risk for developing symptoms among exposed workers compared to referents was analyzed by calculating relative risk (RR) with a 95% confidence interval (CI). To quantify the relationship between personal trichloramine concentrations and at least one ocular, nasal or respiratory symptom occurring during the last week, a multiple Poisson regression with robust error variance was used to estimate risk ratio (RR) with a 95% CI. Trichloramine concentrations were dichotomized at the median, and the analyses were adjusted for age and smoking.
The lung function (FVC and FEV1) and FENO characteristics were summarized using descriptive statistics and are expressed in terms of the AM, SD, and range. To assess whether there were any differences in lung function and FENO over shift between exposed workers and referents, multiple linear regression analysis was performed. Correlations between personal trichloramine concentrations and lung function and FENO were also calculated using multiple linear regression analysis. Trichloramine concentrations were dichotomized at the median, and lung function was adjusted for asthma, body mass index (BMI), phadiatop, and smoking, while FENO was adjusted for asthma and smoking. The average daily variability of PEF was calculated and is expressed as a percentage.
p < 0.05 was considered statistically significant. All statistical analyses were performed using SPSS for Windows 22.0 (IBM, New York, NY).
Results
Demographics
One of the exposed workers did not complete the questionnaire leaving demographics of 23 exposed workers and 50 referents which are listed in . The groups did not differ significantly according to gender, smoking habits, BMI, time in present job (years), asthma at any time, allergic symptoms during childhood or IgE-mediated sensitization (verified by Phadiatop). However, the average age was significantly higher among the exposed workers (50 years) than among the referents (39 years) (p < 0.001).
Table 1. Description of demographics among exposed workers and referents.
Trichloramine and THMs
A total of 24 personal and 35 stationary samples of trichloramine in air were collected. One personal sample were excluded due to water contamination and five samples, two personal and three stationary, were destroyed in the analysis resulting in 21 personal and 32 stationary trichloramine concentrations in air, shown in . Personal and stationary measurements yielded mean concentrations of 19 µg/m3 and 23 µg/m3, respectively. The highest concentrations (personal: 76 µg/m3, stationary: 140 µg/m3) were measured at facility 2 (p = 0.002 and p = 0.02). To predict personal exposure to trichloramine from parallel stationary measurements, linear regression analysis was performed on personal trichloramine levels of personnel spending more than 50% of their working day in the pool area (n = 8) and those obtained from corresponding stationary measurements at the pool side (n = 14). Personnel who spent more than 50% of their working day in the pool area were found in five out of 11 facilities resulting in five different arithmetic means used in the analysis. The resulting coefficient of determination (R2 = 0.97) indicated ∼97% explained variance and a significant regression coefficient (β = 0.45; 95% CI: 0.31–0.59; p = 0.002) (). Trihalomethanes (chloroform, bromodichloromethane, dibromochloromethane, and bromoform) in air were also measured at all facilities. Four personal samples were excluded due to water contamination. With average concentrations of 15 µg/m3 and 12 µg/m3 for personal measurements (n = 20) and stationary measurements (n = 35), respectively, chloroform constituted the dominant THM. No correlation was found between trichloramine and chloroform concentrations for either personal or stationary measurements.
Figure 1. Relationship between personal measures of trichloramine from personnel that spent more than 50% of their work day in the pool area and parallel stationary sampling measures of trichloramine, with line fitted using linear regression.
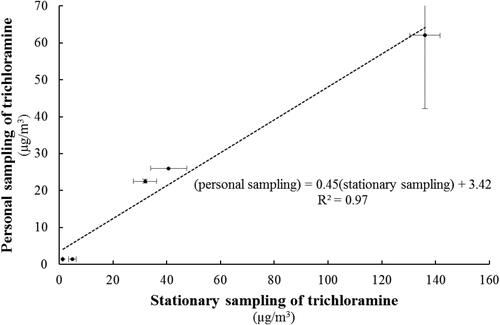
Table 2. Trichloramine concentrations in air (µg/m3) determined via personal and stationary sampling in indoor swimming pool facilities.
Ocular, nasal, and respiratory symptoms
The exposed and referent groups reported ocular, nasal, and respiratory symptoms during the last 12 months (data not shown), 3 months, and 1 week. The groups experienced similar symptoms during the last 3 months and week (). No significant difference could be established between the groups. During the last 3 months, 39% of the exposed workers experienced itchy, smarting, and irritated eyes, whereas 33% of the referents experienced these symptoms (RR: 1.2; 95% CI: 0.6–2.2). Regarding throat-related symptoms, such as hoarseness and dryness, 37% of the exposed workers had experienced at least one of these symptoms within the last 3 months compared to 27% among referents (RR: 1.3; 95% CI: 0.6–2.7). Of the symptoms experienced during the last week, the prevalence of dry eyes and red eyes among the exposed workers was 30% and 13%, respectively, whereas the prevalence of dry eyes and red eyes among the referents was 24% (RR: 1.3; 95% CI: 0.6–2.8) and 8% (RR: 1.6; 95% CI: 0.4–6.7), respectively. Compared with the referents, the exposed workers were more likely, but not significantly likely, to attribute their reported symptoms experienced during the last 12 months, 3 months, and 1 week to their work environment. The categorization of the symptoms into ocular, nasal or respiratory showed that 39% in the exposed group reported at least one ocular symptom during the last week compared to 36% among the referents (RR: 1.1; 95% CI: 0.6–2.2). However, at least one nasal symptom and one respiratory symptom during the last week were less common in the exposed group than in the referent group (35% vs. 46% and 35% vs. 40%, respectively) (RR: 0.8; 95% CI: 0.4–1.4 and RR: 0.9; 95% CI: 0.5–1.7).
Table 3. Prevalence (%) of ocular, nasal, and respiratory symptoms among exposed workers and referents during the last 3 months and the last week.
In facility 2, where the highest trichloramine concentrations were measured, a higher, but not significant, risk of developing at least one ocular symptom (RR: 2.4; 95% CI: 1.0–5.7), one nasal symptom (RR: 1.6; 95% CI: 0.5–5.2) or one respiratory symptom (RR: 1.6; 95% CI: 0.5–5.2) during the last week was found among exposed workers than among referents.
The multiple Poisson regression with robust error variance showed that after adjusting for confounding factors, trichloramine exposure that was higher than the median (20 µg/m3) was associated with a significantly increased risk of developing at least one ocular symptom during the last week (RR: 1.2; 95% CI: 1.1–1.4).
Lung function, FENO, and PEF
The lung function characteristics (FVC and FEV1) of exposed workers and referents before and after a work shift are shown in . Three exposed workers did not complete the lung function test. Subjects from both the exposed and referent groups had lower lung function prior to their work shift than those expected based on the reference values.[Citation31,Citation32] Multiple linear regression analysis revealed negligible changes during the work shifts of both groups and negligible differences between the groups. shows the FENO values of exposed workers and referents prior to the work shift and changes in these values during the shift. One of the exposed workers did not participate in the FENO-measurement. The mean FENO before the shift differed between the groups (exposed: 18.0 ppb; referents: 16.1 ppb), and multiple linear regression analysis revealed that the difference increased significantly after the shift (exposed: 17.9 ppb; referents: 14.3 ppb) (β = 0.27; 95% CI: 0.30–3.67: p = 0.02). The FENO values of one subject from the referent group were larger than those in the normal range, at 25–50 ppb.[Citation35] The lung function and measured FENO levels appeared to be independent of the personal trichloramine concentrations found in this study. The highest PEF value determined every hour during the day of the investigation of the exposed group varied from 1–5% for each subject.
Table 4. Lung function (FVC and FEV1) prior to the work shift and change during the work shift of exposed workers and referents.
Table 5. Nitric monoxide in exhaled air (FENO; ppb) prior to the work shift and change during the work shift of exposed workers and referents.
Discussion
To our knowledge, this is the first study in which personal and stationary air measurements of trichloramine and THMs in habilitation and rehabilitation swimming pools were combined with an investigation of ocular, nasal, and respiratory health effects.
The levels of trichloramine determined via personal measurements were ∼50% of those determined via stationary measurements. Furthermore, compared with referents, the exposed workers experienced more, but not significant, eye- and throat-related symptoms and attributed these symptoms mainly to their work environment. The intergroup difference in FENO increased significantly after a work shift. Evaluation of the dose-response relationship revealed that personal trichloramine concentrations greater than the median concentration (20 µg/m3) were associated with a significantly increased risk of developing at least one ocular symptom.
The personal measurements were considered representative of normal daily activity in habilitation and rehabilitation swimming pools. THM samples were analyzed in an accredited laboratory, and spirometry and FENO examinations were performed in accordance with ATS guidelines.[Citation30,Citation34] Compared with the referent group, the exposed group had a longer average time in the present job, but the healthy worker effect could constitute a selection bias. To avoid confounding factors, the analyses were adjusted for age, asthma, BMI, phadiatop, and smoking. However, evaluating casual associations between exposure and health effects may have been rendered difficult owing to the cross-sectional study design.
Trichloramine and THMs
Personal and stationary measurements yielded trichloramine levels of 1–76 µg/m3 (average: 19 µg/m3) and 1–140 µg/m3 (average: 23 µg/m3), respectively, which were considerably lower than the WHO-recommended reference value (500 µg/m3). However, these concentrations occurred either in the same range or were lower than those reported in previous studies. Previous studies reported that trichloramine levels of 17–150 µg/m3 and 200–300 µg/m3 were associated with ocular and upper airway symptoms, respectively, among swimming pool employees.[Citation20,Citation21] Chloroform was the dominant THM, but the average concentrations measured in this study (personal: 15 µg/m3, stationary: 12 µg/m3) were lower than those specified in the current Swedish OEL (10,000 µg/m3). The mixed exposure of several different THMs in the swimming pool environment could give rise to an additive effect, but as the measured levels of all THMs were low, it is considered not applicable in this study. The lower air concentrations of trichloramine and THMs in this study (compared with those reported in previous studies) may be attributed to smaller facilities as well as fewer visitors and activities associated with public indoor swimming pools. These fewer activities result in less vigorous water movement in habilitation and rehabilitation swimming pools than that occurring in public pools.
In previous studies, reference values and OELs proposed and set for trichloramine exposure have been based on stationary measurements, whereas occupational exposure limits have typically been based on personal sampling. In this study, a linear regression analysis was used to determine the correlation between personal exposure and the trichloramine levels obtained via stationary sampling. This analysis revealed that during personal measurements, subjects were exposed to trichloramine levels that were approximately half as high as those of stationary measurements. Similar findings were reported by Westerlund et al.[Citation26] This difference in air concentrations implies that more personal measurements are needed when discussing an OEL for trichloramine.
Ocular, nasal, and respiratory symptoms
No significant difference in reported ocular, nasal, and respiratory symptoms could be established between exposed and referents, but some trends could be seen. The exposed habilitation and rehabilitation swimming pool workers (i) experienced more eye- and throat-related symptoms during the last week and the last 3 months and (ii) more often attributed the reported ocular, nasal, and respiratory symptoms to their work environment. This finding concurred with the results of previous studies in which ocular and respiratory symptoms were reported among swimming pool workers.[Citation11,Citation16–19] Lofstedt et al.[Citation19] investigated health effects and trichloramine exposure in public indoor swimming pools using the same group of referents and questionnaire as those employed in this study. They found that compared with the referents: (i) a significantly higher fraction of the exposed experienced at least one ocular and one nasal symptom during the last week and (ii) the exposed group was more likely to have experienced these symptoms during the last 3 months.
Lung function, FENO, and PEF
Lung function (FVC and FEV1) values were lower than expected among the exposed workers and referents but were still in the normal range stipulated for the Swedish reference materials.[Citation31,Citation32] The lung function of both groups did not change significantly during the shift. The average FENO values of both groups were in the normal range, but in the exposed group, they did not decline as expected during the day.[Citation39] This increased intergroup difference was significant after the shift, indicating an increased risk of respiratory inflammation in the swimming pool environment. Similar findings were reported for public swimming pool employees.[Citation19] These findings concurred with those of a previous study[Citation40] that reported mild eosinophilic airway inflammation for highly trained swimmers. Indistinguishable FENO levels have also been reported for swimming pool environments. For example, compared with the FENO levels detected among referents, the same FENO levels were detected among adolescent and adult swimmers.[Citation41–43] Fornander et al.[Citation44] confirmed that indoor swimming pool employees experienced airway irritation without the occurrence of increased FENO concentrations associated with average trichloramine levels of 200 µg/m3. Hourly registered PEF values during the day of the investigation seemed normal, and unusual individual variability that could be associated with peak exposure was absent.
Dose-response relationship
In this study, the highest trichloramine concentrations were measured at facility 2 and could also be associated with a higher, but not significant, risk of developing at least one ocular, nasal, or respiratory symptom during the last week compared with referents. However, personal trichloramine concentrations over the median concentration (20 µg/m3) were found to be associated with a statistically significant increased risk of developing at least one ocular symptom during the last week when adjusting for confounding factors. These findings are in accordance with that of Lofstedt et al.,[Citation19] who reported an increased risk of ocular, nasal, and respiratory symptoms occurring during the last week among exposed swimming pool workers. Also, Parrat et al.[Citation21] found that the occurrence of eye and nose irritation was connected with trichloramine exposure. However, the average trichloramine concentration in that study (114 µg/m3) was significantly higher than both the average value reported by Lofstedt et al.[Citation19] (71 µg/m3) and the average value in this study (19 µg/m3).
Although the trichloramine exposure among swimming pool employees in the study by Lofstedt et al.[Citation19] was higher (71 µg/m3) than the trichloramine exposure measured in the habilitation and rehabilitation swimming pools in the current study (19 µg/m3), some of the described symptoms had similar trends. For example, (i) the highest fractions of reported red eyes, sneezing, and dry throat during the last week were found among public swimming pool workers examined by Lofstedt et al.[Citation19]; (ii) a lower fraction of the habilitation and rehabilitation swimming pool workers experienced the same symptoms and were exposed to lower levels of trichloramine; and (iii) the lowest fraction of subjects reporting these symptoms occurred in the case of unexposed referents. These findings in combination with the statistically significant increased risk of ocular symptoms at trichloramine exposure over 20 µg/m3 found in the current study are indicative of a possible correlation between the air concentration of trichloramine and the occurrence of ocular, nasal, and respiratory symptoms.
Conclusions
The personal air concentrations of trichloramine and THMs measured in this study were low compared to international standards. A slightly higher, but not significant, prevalence of reported eye- and throat-related symptoms occurred among the exposed workers than among the referents. However, the increased risk of developing at least one ocular symptom at personal trichloramine concentrations over 20 µg/m3 combined with an increase in the difference in FENO during the work shift of the habilitation and rehabilitation swimming pool employees should not be neglected. To further investigate the trends presented in this study, a longitudinal study design with a cohort of swimming pool workers could provide additional information.
Acknowledgments
The authors extend their gratitude to the participating swimming pool facilities and their employees. We are also grateful to Göte Mölleby for medical investigations and Niclas Johansson for exposure measurements.
References
- Iannucci, L.: Making waves with aquatic therapy. PT Motion. Alexandria: American Physical Therapy Association, 2012.
- Hery, M., G. Hecht, J.M. Gerber, J.C. Gendre, and G. Hubert: Exposure to chloramines in the atmosphere of indoor swimming pools. Ann. Occup. Hyg. 39:427–439 (1995).
- Hailin, G., G.G. Wallace, and R.A.J. O'Halloran: Determination of trace amounts of chloramines by liquid chromatographic separation and amperometric detection. Analyt. Chim. Acta. 237:149–153 (1990).
- Holzwarth, G., R.G. Balmer, and L. Soni: The fate of chlorine and chloramines in cooling towers. Water Res. 18:1421–1427 (1984).
- Lahl, U., K. Bätjer, J.v. Düszeln, B. Gabel, B. Stachel, and W. Thiemann: Distribution and balance of vaolatile halogenated hydrocarbons in the water and air of covered swimming pools using chlorine for water disinfiction. Water Res. 15:803–814 (1981).
- Aggazzotti, G., G. Fantuzzi, E. Righi, and G. Predieri: Blood and breath analyses as biological indicators of exposure to trihalomethanes in indoor swimming pools. Sci. Total Environ. 217:155–163 (1998).
- Fantuzzi, G., E. Righi, G. Predieri, G. Ceppelli, F. Gobba, and G. Aggazzotti: Occupational exposure to trihalomethanes in indoor swimming pools. Sci. Total Environ. 264:257–265 (2001).
- Erdinger, L., K.P. Kuhn, F. Kirsch, et al.: Pathways of trihalomethane uptake in swimming pools. Int. J. Hyg. Environ. Health 207:571–575 (2004).
- Aggazzotti, G., G. Fantuzzi, P. L. Tartoni, and G. Predieri: Plasma chloroform concentrations in swimmers using indoor swimming pools. Arch. Environ. Health 3:175–179 (1990).
- Aggazzotti, G., G. Fantuzzi, E. Righi, and G. Predieri: Environmental and biological monitoring of chloroform in indoor swimming pools. J. Chromatogr. A 1:181–190 (1995).
- Massin, N., A.B. Bohadana, P. Wild, M. Hery, J.P. Toamain, and G. Hubert: Respiratory symptoms and bronchial responsiveness in lifeguards exposed to nitrogen trichloride in indoor swimming pools. Occup. Environ. Med. 55:258–263 (1998).
- Thickett, K.M., J.S. McCoach, J.M. Gerber, S. Sadhra, and P.S. Burge: Occupational asthma caused by chloramines in indoor swimming-pool air. Eur. Respir. J. 19:827–832 (2002).
- International Agency for Research on Cancer (IARC): Re-evaluation of some organic chemicals, hydrazine and hydrogen peroxide (part three). Chlorodibromomethane. In IARC Monographs on the Evaluation of Carcinogenic Risks to Humans. Lyon, France: World Health Organization, 1999. pp. 1331–1338.
- Association Advancing Occupational and Environmental Health (ACGIH): Threshold Limit Values for Chemical Substances and Physical Agents & Biological Exposure Indices. Cincinnati, OH: ACGIH, 2015.
- SWEA: Occupational Exposure Limits and Measures against Air Contaminants (in Swedish) AFS 2015:7. Stockholm, Sweden: Swedish Work Environment Authority, 2015.
- Jacobs, J.H., S. Spaan, G.B. van Rooy, et al.: Exposure to trichloramine and respiratory symptoms in indoor swimming pool workers. Eur. Respir. J. 29:690–698 (2007).
- Dang, B., L. Chen, C. Mueller, et al.: Ocular and respiratory symptoms among lifeguards at a hotel indoor waterpark resort. J. Occup. Environ. Med. 52:207–213 (2010).
- Fantuzzi, G., E. Righi, G. Predieri, P. Giacobazzi, K. Mastroianni, and G. Aggazzotti: Prevalence of ocular, respiratory and cutaneous symptoms in indoor swimming pool workers and exposure to disinfection by-products (DBPs). Int. J. Environ. Res. Publ. Health. 7:1379–1391 (2010).
- Lofstedt, H., J. Westerlund, P. Graff, et al.: Respiratory and ocular symptoms among employees at Swedish indoor swimming pools. J. Occup. Environ. Med. 58:1190–1195 (2016).
- Chu, T.S., S.F. Cheng, G.S. Wang, and S.W. Tsai: Occupational exposures of airborne trichloramine at indoor swimming pools in Taipei. Sci. Total Environ. 461–462:317–322 (2013).
- Parrat, J., G. Donze, C. Iseli, D. Perret, C. Tomicic, and O. Schenk: Assessment of occupational and public exposure to trichloramine in Swiss indoor swimming pools: A proposal for an occupational exposure limit. Ann. Occup. Hyg. 56:264–277 (2012).
- Nordberg, G.F., N.G. Lundstrom, B. Forsberg, et al.: Lung function in volunteers before and after exposure to trichloramine in indoor pool environments and asthma in a cohort of pool workers. BMJ Open. 2:1–9 (2012).
- Rosenman, K.D., M. Millerick-May, M.J. Reilly, et al.: Swimming facilities and work-related asthma. J. Asthma 52:52–58 (2015).
- World Health Organization (WHO): Guidelines for Recreational Water Environments. Volume 2. Swimming Pools and Similar Environments. Geneva, Switzerland: World Health Organization, 2006.
- ANSES: Évaluation des Risques Sanitaires liés aux Piscines. Partie I: Piscines Réglementées. Maisons-Alfort, France: French Agency for Food, Environmental and Occupational Health & Safety, 2012.
- Westerlund, J., P. Graff, I.L. Bryngelsson, H. Westberg, K. Eriksson, and H. Lofstedt: Occupational exposure to trichloramine and trihalomethanes in Swedish indoor swimming pools: Evaluation of personal and stationary monitoring. Ann. Occup. Hyg. 59:1074–1084 (2015).
- EURACHEM: Guidance Document. Accreditation for Chemical Laboratories. No. 1. Teddington, UK: EURACHEM/WELAC, 1993.
- US Environmental Protection Agency: Method TO-17: Determination of Volatile Organic Compounds in Ambient Air Using Active Sampling onto Sorbent Tubes. Cincinnati, OH: U.S. EPA, 1999.
- Nielsen, J., H. Welinder, B. Jonsson, A. Axmon, L. Rylander, and S. Skerfving: Exposure to hexahydrophthalic and methylhexahydrophthalic anhydrides—Dose-response for sensitization and airway effects. Scand. J. Work Environ. Health 27:327–334 (2001).
- Miller, M.R., J. Hankinson, V. Brusasco, et al.: Standardisation of spirometry. Eur. Respir. J. 26:319–338 (2005).
- Hedenström, H., P. Malmberg, and K. Agarwal: Reference values for lung function tests in females. Regression equations with smoking variables. Bull. Eur. Physiopathol. Respir. 21:551–557 (1985).
- Hedenström, H., P. Malmberg, and H.V. Fridriksson: Reference values for lung function tests in men: Regression equations with smoking variables. Upsala J. Med. Sci. 91:299–310 (1986).
- Malmberg, L.P., H. Turpeinen, P. Rytila, S. Sarna, and T. Haahtela: Determinants of increased exhaled nitric oxide in patients with suspected asthma. Allergy 60:464–468 (2005).
- American Thoracic Society, European Respiratory Society: ATS/ERS recommendations for standardized procedures for the online and offline measurement of exhaled lower respiratory nitric oxide and nasal nitric oxide, 2005. Am. J. Respir. Crit. Care Med. 171:912–930 (2005).
- Dweik, R.A., P.B. Boggs, S.C. Erzurum, et al.: An official ATS clinical practice guideline: Interpretation of exhaled nitric oxide levels (FENO) for clinical applications. Am. J. Respir. Crit. Care Med. 184:602–615 (2011).
- Quackenboss, J.J., M.D. Lebowitz, and M. Krzyzanowski: The normal range of diurnal changes in peak expiratory flow rates. Relationship to symptoms and respiratory disease. Am. Rev. Respir. Dis. 143:323–330 (1991).
- Vidal, C., F. Gude, O. Boquete, et al.: Evaluation of the phadiatop test in the diagnosis of allergic sensitization in a general adult population. J. Investig. Allergol. Clin. Immunol. 15:124–130 (2005).
- Hornung, R.W., and L.D. Reed: Estimation of average concentration in the presence of nondetectable values. Appl. Occup. Environ. Hyg. 5:46–51 (1990).
- Antosova, M., A. Bencova, A. Psenkova, D. Herle, and E. Rozborilova: Exhaled nitric oxide -Circadian variations in healthy subjects. Eur. J. Med. Res. 4:6–8 (2009).
- Helenius, I., P. Rytila, S. Sarna, et al.: Effect of continuing or finishing high-level sports on airway inflammation, bronchial hyperresponsiveness, and asthma: A 5-year prospective follow-up study of 42 highly trained swimmers. J. Allergy Clin. Immunol. 109:962–968 (2002).
- Carraro, S., M.F. Pasquale, M. Da Fre, et al.: Swimming pool attendance and exhaled nitric oxide in children. J. Allergy Clin. Immunol. 118:958–960 (2006).
- Piacentini, G.L., E. Rigotti, A. Bodini, D. Peroni, and A.L. Boner: Airway inflammation in elite swimmers. J. Allergy Clin. Immunol. 119:1559–1560 (2007).
- Pedersen, L., T.K. Lund, P.J. Barnes, S.A. Kharitonov, and V. Backer: Airway responsiveness and inflammation in adolescent elite swimmers. J. Allergy Clin. Immunol. 122:322–327 (2008).
- Fornander, L., B. Ghafouri, M. Lindahl, and P. Graff: Airway irritation among indoor swimming pool personnel: Trichloramine exposure, exhaled NO and protein profiling of nasal lavage fluids. Int. Arch. Occup. Environ. Health. 86:571–580 (2013).

