 ?Mathematical formulae have been encoded as MathML and are displayed in this HTML version using MathJax in order to improve their display. Uncheck the box to turn MathJax off. This feature requires Javascript. Click on a formula to zoom.
?Mathematical formulae have been encoded as MathML and are displayed in this HTML version using MathJax in order to improve their display. Uncheck the box to turn MathJax off. This feature requires Javascript. Click on a formula to zoom.ABSTRACT
The effects of electronic-cigarette use (vaping), marketed as a healthier alternative to cigarette smoking (CS), on lung function remain equivocal. Therefore, this study assessed and compared the effects of vaping and CS on maximum respiratory pressures (MRP), respiratory function and carboxyhaemoglobin levels. Forty-four young healthy participants were recruited: vapers (n = 12), cigarette smokers (n = 14), and people who had never vaped nor smoked (control) group (n = 18). Spirometry, MRP and carboxyhaemoglobin levels were measured. Both smokers and vapers had a lower Forced expiratory volume in the first second (FEV1), Peak expiratory flow, FEV1/Forced vital capacity (FEV1/FVC), Forced expiratory flow at 25%, 25–75% of FVC, FEF25-75pred% and higher carboxyhaemoglobin% than controls (p < 0.05). In smokers, but not in vapers, FEV1pred% was lower than in controls (p < 0.01). MRP did not differ significantly between the three groups. Vaping has similar detrimental effects as CS on pulmonary function and may thus not be a healthier alternative to smoking.
Introduction
Cigarette smoking is a well-known risk factor for the development of cancer, cardiovascular diseases and respiratory disorders, such as lung cancer and chronic obstructive pulmonary disease (COPD) (Barengo et al., Citation2019). Smokers are very much aware of these dangers and many of them seek to quit smoking. Electronic cigarettes (e-cigarette) are marketed as a healthier alternative to cigarette smoking, as they are devices that do not burn tobacco, yet may deliver nicotine, and contain fewer than the more than 4000 toxic chemicals in cigarette smoke (Glantz & Forbes, Citation1996; Ling & Glantz, Citation2005; Richter et al., Citation2008). In the United Kingdom (UK) e-cigarettes are marketed as a smoke cessation product, whereas in the United States (US) they are marketed to young adults as an alternative for those who do not smoke (Mantey et al., Citation2016). It was reported that vaping prevalence has substantially increased among youth (Levy et al., Citation2019). This raise concerns about the creation of a new generation of nicotine-dependent population who could easily change to cigarette smoking. The success of e-cigarettes to help quit smoking is reflected by the fact that 54% of e-cigarette users in the UK are ex-smokers (Action on Smoking and Health, Citation2019).
An e-cigarette is a battery-powered device that consists of a vaporizing chamber, a cartridge/tank that contains the vaping liquid (e-liquid) and an atomizer that heats, rather than burns, the e-liquid that consists of vegetable glycerine, propylene glycol and other chemicals, and may contain nicotine. When the e-liquid is heated, it produces the aerosolized vapour that is inhaled by the vaper. Because vaping is a relatively new phenomenon, the impact of vaping on health has not yet thoroughly been investigated. However, the few studies that have investigated vaping indicate that e-cigarettes have detrimental effects on human health in general and on lung function in particular (Antoniewicz et al., Citation2019; Chaumont et al., Citation2019; Coppeta et al., Citation2018; Mohammad Z. Darabseh et al., Citation2020; Meo et al., Citation2019). Interestingly, some reports found that vaping is linked with lung injury, named ‘E-cigarette, or vaping product use-associated lung injury’ (EVALI) including inducing pneumonia, hypersensitivity pneumonitis, lipoid pneumonia and diffuse alveolar damage (Henry et al., Citation2020; Landman et al., Citation2019). This problem can not be ignored, as reflected by the 2,807 hospitalized EVALI, mostly young adults and/or teenagers, cases or deaths that have been reported in the US, and the 244 suspected adverse reactions reported, including two fatal outcomes, in the UK (Centers for Disease Control Prevention & Information, Citation2020; UK Medicines and Healthcare products Regulatory Agency, Citation2020). Thus, although Public Health England claimed that e-cigarettes are 95% safer than cigarette smoking (McNeill et al., Citation2015) and the prevailing idea is that vaping is not only safer, but also helps in smoking cessation (McNeill et al., Citation2015), it is far from clear that vaping is a healthier alternative than smoking. Therefore, the aim of this study was to compare the effects of vaping and smoking on lung function. It was hypothesized that vaping has less detrimental effects on pulmonary function than smoking.
Methods
Study design
This was a laboratory-based, cross-sectional, observational study to compare pulmonary function in i) vapers, ii) cigarette smokers and iii) people who neither smoked nor vaped (controls). Ethical approval was obtained from the Science and Engineering Research Ethics and Governance Committee at Manchester Metropolitan University (EthOS reference number: 5944). All procedures adhered to the principles stated in the Declaration of Helsinki and all participants provided written informed consent before participating.
Participants
The sample size was based on the work of (Polosa et al., Citation2017) who compared vapers with smokers. Using their numbers, 7 participants per group were needed to detect a 12% difference in Forced Expiratory Volume in one second (FEV1) with a power of 80% and a type-I error (alpha) of 0.05 (5%).
Participants were recruited from the local community and Manchester Metropolitan University through posters, social media channels and snowball sampling. The inclusion criteria were: 18- to 55-year-old men and women, and cigarette smokers and vapers had to have smoked/vaped for ≥1 year. Exclusion criteria were: neuromuscular disease; severe musculoskeletal injuries; any lower limb injury; any diagnosed mental health disorder; treatment for chronic respiratory complaints; a known history of heart disease; smokers who mix cigarette and vape; water pipe (shisha) smokers. Vaping and smoking history and volume were assessed by a questionnaire. The smoking volume (SV) was given as pack years, calculated as:
Where Ncig is the current number of cigarettes smoked per day, and S the number of years smoked.
Participant characteristics
Demographic data including age, sex, height, body mass, body mass index (BMI) and occupation of participants was recorded. Height and body mass were assessed using a stadiometer and digital scales, respectively. Body composition was assessed using bioelectrical impedance (BodyStat 1500, BodyStat, Douglas, UK).
Carboxyhaemoglobin
HbCO, which is the percentage of the haemoglobin (Hb) oxygen binding sites occupied by carbon monoxide (CO), was measured with a hand-held CO metre (Micro Smokerlyzer, Bedfont Scientific Ltd.; Kent, UK) according to the recommendations of the manufacturer (Hajek & Belcher, Citation1991). Participants exhaled to residual volume and then quickly inhaled until total lung capacity. After a 15-s breath-hold, the participants were asked to exhale slowly through a disposable mouthpiece attached to the carbon monoxide metre for at least 10 s. The measured HbCO level was expressed as percentage (HbCO%).
Spirometry
Spirometry was conducted using a Micro Medical Spiro USB Spirometer and analysed with Spida 5 software (Cardinal Health, UK). FEV1, Forced Vital Capacity (FVC), FEV1/FVC ratio, Peak Expiratory Flow (PEF), maximum mid-expiratory flow between 25% and 75% of the FVC (FEF25-75%) and predicted values of FVC, FEV1, FEF25-75% were recorded. The spirometry was completed in accordance with the American Thoracic Society/European Respiratory Society (ATS/ERS) guidelines (Miller et al., Citation2005). Predicted values were calculated by the Spida 5 software based on body mass index, age, sex and ethnicity according ATS/ERS guidelines. Each participant had a nose clip and completed a minimum of three manoeuvres with at least 1–2 min rest between each manoeuvre. Manoeuvres were rejected if: participants prematurely stopped exhalation, coughed during the first second of exhalation, lips were not fully sealed around the mouthpiece, the mouthpiece was obstructed by the teeth or tongue and/or the effort appeared submaximal. The test session was concluded when the largest two FEV1 and the largest two FVC were each within 0.15 L of each other in at least 3 manoeuvres (Miller et al., Citation2005). If these criteria were not met, the manoeuvres were repeated until the criteria were met, eight manoeuvres had been attempted, or if the participant did not want to continue. Participants were instructed not to eat heavy meals or to smoke or vape and to refrain from vigorous physical activity for at least two hours before the test.
Respiratory pressure
The maximal inspiratory pressure (MIP), maximal expiratory pressure (MEP) and sniff nasal inspiratory pressure (SNIP) were determined using a portable mouth pressure device (MicroRPM, Cardinal Healthcare, UK). The participants were asked to inhale (MIP/SNIP) or exhale (MEP) as forcefully as possible after full exhalation or inhalation, respectively into the portable MicroRPM. To determine SNIP, participants placed a probe in one of their nostrils, and with the other nostril closed inhaled as forceful as possible via the nose (Lofaso et al., Citation2006). For all manoeuvres, attempts were repeated, with a 30-s interval between each attempt to prevent the development of respiratory muscle fatigue, until a maximum value was reached.
Statistics
Statistical analyses were performed using SPSS 24.0 (IBM Corporation, NY, US). Data was assessed for normality with the Shapiro-Wilk tests. If the data were not normally distributed an Analysis of variance (ANOVA) was performed on the log-transformed data. Differences between vapers, smokers and controls, and sexes were tested using two-way univariate ANOVA with as between factors group and sex. If a significant group effect or a group * sex interaction were found, a Tukey 2-sided post-hoc test was performed to locate the significant differences. Predicted spirometry values were compared between pure vapers (who never smoked), vapers who were ex-smokers and controls with a two-way ANOVA and Tukey-corrected post-hoc tests to locate the differences. A stepwise regression analysis was performed to assess to what extent spirometry parameters were affected by sex, and vaping or smoking duration or volume. Differences and correlations were considered significant at p < 0.05. All data are presented as mean±SD unless stated otherwise.
Results
Men were taller and heavier than women, and women had a higher fat percentage than men (p < 0.05), irrespective of being vapers, smokers or controls (). All vapers had used e-cigarettes daily for ≥ 1 year (1.67 ± 1.00 years). Eleven of the twelve vapers were using nicotine-containing e-liquids with a concentration ranging between 3 to 18 mg/mL. The puffs per e-cigarette were 8.30 ± 5.23. Seven out of twelve vapers were former smokers. All cigarette smokers had smoked daily for 4.86 ± 2.49 years, consumed 9.00 ± 4.78 cigarettes/day and had a smoking history of 2.29 ± 1.88 pack years. No group-sex interactions were found for any outcome measure, indicating that all the observed effects of smoking and vaping were similar in men and women.
Table 1. Participant characteristics
Men had higher FEV1, FVC, PEF, FEF25%, FEF50%, FEF25-75%, MIP and MEP than woman (p < 0.05) ( and ). FEV1pred%, FEV1/FVC, FEF75%, FEF25-75pred%, SNIP and HbCO% did, however, not differ significantly between men and women ( and ), but the FVCpred% was higher in women than men (; p < 0.03).
Table 2. Forced vital capacity, maximal respiratory pressures and carboxyhaemoglobin in male and female vapers, smokers and controls
Figure 1. A) FEV1/FVC: Forced expiratory volume in one second/ forced vital capacity; b) FEV1: Forced expiratory volume in one second; c) FEV1 predicted: Forced expiratory volume in one second predicted %; d) PEF: Peak expiratory flow; * sex difference at p < 0.001; α: significantly different from control at p ≤ 0.008
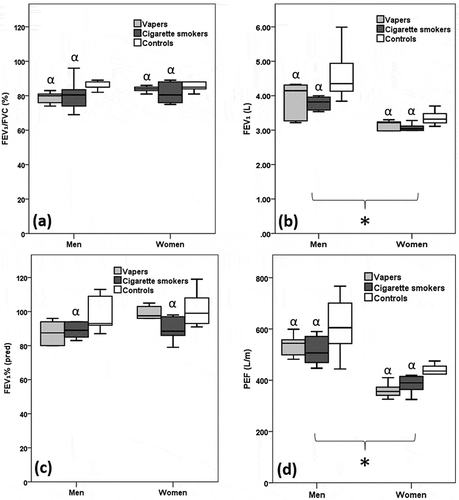
Figure 2. A) FEF25%-75%: Forced expiratory flow at 25%-75%; b) FEF25%: Forced expiratory flow at 25%; c) FEF25%-75% (pred): Forced expiratory flow at 25%-75% predicted %; d) FEF75%: Forced expiratory flow at 75%; * sex difference at p ≤ 0.013; α: different from control at p ≤ 0.008
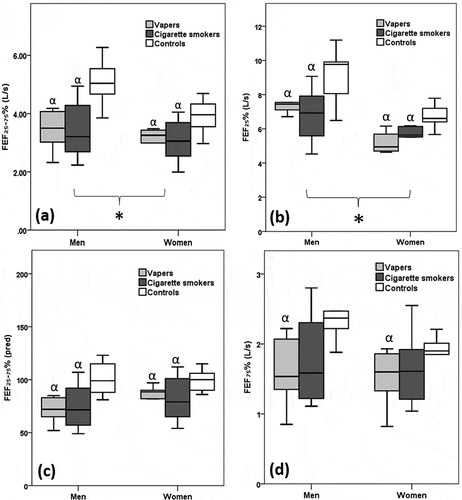
Vapers and cigarette smokers had lower FEV1, PEF, FEV1/FVC, FEF25%, FEF50%, FEF25-75%, FEF25-75pred% and higher HbCO% than controls (p < 0.05) ( and ). The FEV1pred% was lower in smokers than controls (p < 0.01), but there was no significant difference between vapers and controls (p = 0.054) (). Vapers had a lower FEF75% than controls (p < 0.009), but there was no significant difference in FEF75% between smokers and controls (p = 0.064) ().There were no significant differences in FEV1, FEV1pred%, PEF, FEV1/FVC, FEF25%, FEF50%, FEF75%, FEF25-75%, FEF25-75pred% and HbCO% between vapers and smokers ( and ). The FVC, FVCpred%, MIP, MEP and SNIP did not differ significantly between vapers, smokers and controls (). The FEV1/FVC (p ≤ 0.033), FEF25-75pred% (p ≤ 0.009) and HbCO% (p < 0.001) were lower in pure vapers and vapers who were ex-smokers than controls, with no significant difference in these parameters between pure vapers and vapers who were ex-smokers ().
Table 3. Pure vapers and vapers who were ex-smokers vs. controls
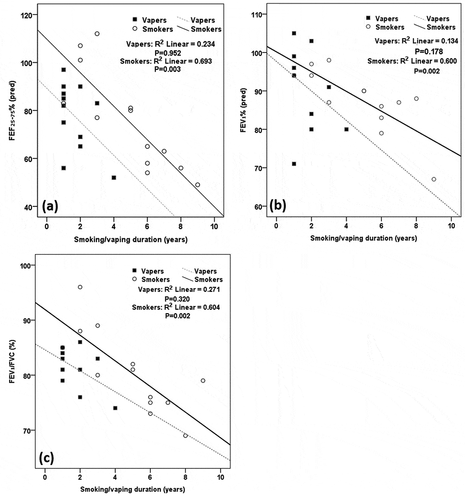
A stepwise linear regression was performed to assess to what extent the respiratory parameters were determined by sex, height, body mass, smoking duration, smoking volume, or for vapers, vaping duration and number of puffs. Smoking duration was the primary determinants of FEV1pred% (R2adj = 0.564; p = 0.002), FEV1/FVC (R2adj = 0.568; p = 0.002), FEF50% (R2adj = 0.412; p = 0.011), FEF25-75% (R2adj = 0.528; p = 0.003), FEF25-75pred% (R2adj = 0.665; p < 0.001) (). Vaping duration and number of puffs were not significant determinants of pulmonary function ().
Figure 3. Relationship between respiratory parameters and smoking/vaping duration. a) FEF25%-75% (pred): Forced expiratory flow at 25%-75% predicted; b) FEV1pred%: Forced expiratory volume in one second predicted%; c) FEV1/FVC: Forced expiratory volume in the first second/ forced vital capacity. p-value significant at p < 0.05
Discussion
The main observation of this study was that smokers and vapers had a similarly lower respiratory function compared to people who neither smoked nor vaped, irrespective of sex. This was not related to respiratory muscle weakness, as reflected by similar maximal respiratory pressures in all groups. In addition, the HbCO content was similarly elevated in smokers and vapers. These data indicate that vaping and smoking may cause a similar degree of airway obstruction.
In this study we confirmed that men have higher spirometric values, such as FEV1 and FVC, than women, as reported previously (Mohammad Z Darabseh et al., Citation2021; Mead, Citation1980; Zakaria et al., Citation2019). Although it has been reported that cigarette smoking affects pulmonary function more in women than in men (Xu et al., Citation1994), the absence of any significant group-sex interaction indicated that in our study the effects of smoking and vaping described below were similar in men and women.
Previous studies have also shown that vaping reduces lung function to a similar extent as smoking (Antoniewicz et al., Citation2019; Coppeta et al., Citation2018; Mohammad Z. Darabseh et al., Citation2020; Meo et al., Citation2019), but other studies have reported no changes in pulmonary function parameters after vaping (Polosa et al., Citation2017; Staudt et al., Citation2018; Vardavas et al., Citation2012). The discrepancy between these studies might be due to the duration of e-cigarette use (i.e. years), whether participants were former smokers and/or the duration of smoking or frequency/intensity of vaping. Here we found that the duration of smoking was associated with a decline in respiratory function, but this was not the case for vaping. In fact, we observed that people who had been vaping for as little as 1.67 years had a similar decrement in lung function as those who had smoked for 4.86 years. This decline was not attributable to a previous smoking history in the vapers, as we found that there was no significant difference in spirometry between pure vapers and vapers who were ex-smokers. These decrements in spirometry measures are indicative of mild airway obstruction (McFadden & Linden, Citation1972; Stockley et al., Citation2017). The increase in airflow resistance may be due to small airway narrowing consequent to mucosal oedema, smooth muscle contraction and/or local secretions as seen in long-term smokers (Vardavas et al., Citation2012) and may thus be an early sign of potential progression into obstructive lung diseases.
Another explanation for low airflow could be reduced respiratory muscle strength. However, there were no significant differences between controls and vapers/cigarette smokers in maximal inspiratory and expiratory pressures. These findings suggest that the reduced airflow during smoking/vaping is a consequence of obstruction of the airways rather than lower respiratory muscles strength. We have seen previously that elevated HbCO results in an earlier onset of muscle fatigue (Morse et al., Citation2008) and it can therefore not be excluded that during exercise respiratory muscle fatigue may impair lung function in smokers and vapers.
Limitations of this study include the small sample size, although power calculations indicated that the sample size was large enough to detect 12% differences in FEV1. Perhaps a larger problem is that some of the participants were ex-smokers. However, even in vapers who had no smoking history the FEV1/FVC and FEF25-75%pred were lower than that in controls. Further studies are needed to compare vapers who never smoked with smokers and assess the effects of smoking and vaping cessation on ventilatory function.
Conclusion
While neither vaping nor smoking had a significant impact on respiratory muscle strength, both vaping and smoking led to a similar obstruction of the airways, independent of sex. The elevated HbCO in both vapers and smokers may further compromise respiratory function during exercise. These observations indicate that vaping has similar detrimental effects on pulmonary function as smoking and suggest that one should treat the suggestion that vaping is 95% healthier than smoking with caution (McNeill et al., Citation2015). In addition, increasing vaping uptake among youth could stimulate uptake of cigarette smoking, creating a smoking-dependent generation.
Disclosure statement
No potential conflict of interest was reported by the author(s)
Availability of data and material
The anonymised data that support the findings of this study are available from the corresponding author, MD, upon reasonable request.
Additional information
Notes on contributors
Mohammad Z. Darabseh
Mohammad Z. Darabseh is a Physiotherapist, and a final year PhD candidate in Physiotherapy in Manchester Metropolitan University in the United Kingdom. Darabseh has an international clinical and research experience in physiotherapy including cardiorespiratory physiotherapy and exercise physiology. Darabseh’s research areas focus on cardiorespiratory assessment, rehabilitation and management including COPD risk factors management, smoking and vaping cessation.
James Selfe
James Selfe I have been qualified as a physiotherapist for over thrty years and worked in a variety of places. Being a physiotherapist has given me the opportunity to travel widely and I have made a number of good friends around the world. When I am not working I like mountain walking and have climbed all the Scottish Munros.
Christopher I. Morse
Dr Christopher I. Morse is a reader in exercise physiology with a research interest in neuromuscular and cardiorespiratory physiology within clinical populations.
Hans Degens
Hans Degens Professor of Muscle Physiology and the main academic interest is age-related changes in skeletal muscle morphology and function.
References
- Action on Smoking and Health. (2019). Use of e‐cigarettes (vapourisers) among adults in Great Britain. Accessed 13 Feb.2021 from https://ash.org.uk/wp-content/uploads/2019/09/Use-of-e-cigarettes-among-adults-2019.pdf
- Antoniewicz, L., Brynedal, A., Hedman, L., Lundbäck, M., & Bosson, J. A. (2019). Acute Effects of Electronic Cigarette Inhalation on the Vasculature and the Conducting Airways. Cardiovascular Toxicology, 19(5), 1–10. https://doi.org/https://doi.org/10.1007/s12012-019-09516-x
- Barengo, N. C., Antikainen, R., Harald, K., & Jousilahti, P. (2019). Smoking and cancer, cardiovascular and total mortality among older adults: The Finrisk Study. Preventive Medicine Reports, 14, 100875. https://doi.org/https://doi.org/10.1016/j.pmedr.2019.100875
- Centers for Disease Control Prevention. (2020, Information accessed 23 May 2020). Outbreak of lung injury associated with the use of e-cigarette, or vaping, products. Centers for Disease Control Prevention. Accessed 13 Feb 2021 from https://www.cdc.gov/tobacco/basic_information/e-cigarettes/severe-lung-disease.html
- Chaumont, M., Van De Borne, P., Bernard, A., Van Muylem, A., Deprez, G., Ullmo, J., Starczewska, E., Briki, R., De Hemptinne, Q., Zaher, W., & Debbas, N. (2019). Fourth generation e-cigarette vaping induces transient lung inflammation and gas exchange disturbances: Results from two randomized clinical trials. American Journal of Physiology. Lung Cellular and Molecular Physiology, 316(5), L705–L719. https://doi.org/https://doi.org/10.1152/ajplung.00492.2018
- Coppeta, L., Magrini, A., Pietroiusti, A., Perrone, S., & Grana, M. (2018). Effects of smoking electronic cigarettes on pulmonary function and environmental parameters. The Open Public Health Journal, 11(1), 360–368. https://doi.org/https://doi.org/10.2174/1874944501811010360
- Darabseh, M. Z., Maden-Wilkinson, T. M., Welbourne, G., Wüst, R. C., Ahmed, N., Aushah, H., Selfe, J., Morse, C. I., & Degens, H. (2021). Fourteen days of smoking cessation improves muscle fatigue resistance and reverses markers of systemic inflammation. Scientific Reports, 11(1), 1–11. https://doi.org/https://doi.org/10.1038/s41598-021-91510-x
- Darabseh, M. Z., Selfe, J., Morse, C. I., & Degens, H. (2020). Is vaping better than smoking for cardiorespiratory and muscle function? Multidisciplinary Respiratory Medicine, 15(1). https://doi.org/https://doi.org/10.4081/mrm.2020.674
- Glantz, S. A., & Forbes, E. R. (1996). The cigarette papers (Vol. 17). University of California Press Berkeley.
- Hajek, P., & Belcher, M. (1991). Improved CO monitors for validating smoking abstinence by expired‐air carbon monoxide level. British Journal of Addiction, 86(8), 1029–1030. https://doi.org/https://doi.org/10.1111/j.1360-0443.1991.tb01864.x
- Henry, T. S., Kligerman, S. J., Raptis, C. A., Mann, H., Sechrist, J. W., & Kanne, J. P. (2020). Imaging findings of vaping-associated lung injury. AJR. American Journal of Roentgenology, 214(3), 498–505. https://doi.org/https://doi.org/10.2214/AJR.19.22251
- Landman, S. T., Dhaliwal, I., Mackenzie, C. A., Martinu, T., Steele, A., & Bosma, K. J. (2019). Life-threatening bronchiolitis related to electronic cigarette use in a Canadian youth. CMAJ, 191(48), E1321–E1331. https://doi.org/https://doi.org/10.1503/cmaj.191402
- Levy, D. T., Warner, K. E., Cummings, K. M., Hammond, D., Kuo, C., Fong, G. T., Thrasher, J. F., Goniewicz, M. L., & Borland, R. (2019). Examining the relationship of vaping to smoking initiation among US youth and young adults: A reality check. Tobacco Control, 28(6), 629–635. https://doi.org/https://doi.org/10.1136/tobaccocontrol-2018-054446
- Ling, P. M., & Glantz, S. A. (2005). Tobacco industry consumer research on socially acceptable cigarettes. Tobacco Control, 14(5), e3–e3. https://doi.org/https://doi.org/10.1136/tc.2005.011239
- Lofaso, F., Nicot, F., Lejaille, M., Falaize, L., Louis, A., Clement, A., Raphael, J., Orlikowski, D., & Fauroux, B. (2006). Sniff nasal inspiratory pressure: What is the optimal number of sniffs? European Respiratory Journal, 27(5), 980–982. https://doi.org/https://doi.org/10.1183/09031936.06.00121305
- Mantey, D. S., Cooper, M. R., Clendennen, S. L., Pasch, K. E., & Perry, C. L. (2016). E-cigarette marketing exposure is associated with e-cigarette use among US youth. The Journal of Adolescent Health : Official Publication of the Society for Adolescent Medicine, 58(6), 686–690. https://doi.org/https://doi.org/10.1016/j.jadohealth.2016.03.003
- McFadden, E., Jr, & Linden, D. A. (1972). A reduction in maximum mid-expiratory flow rate: A spirographic manifestation of small airway disease. The American Journal of Medicine, 52(6), 725–737. https://doi.org/https://doi.org/10.1016/0002-9343(72)90078-2
- McNeill, A., Brose, L., Calder, R., Hitchman, S., Hajek, P., & McRobbie, H. (2015). E-cigarettes: An evidence update. Public Health England, 3, 6. https://www.nicopure.com/wp-content/uploads/2016/01/Ecigarettes_an_evidence_update_A_report_commissioned_by_Public_Health_England_FINAL.pdf
- Mead, J. (1980). Dysanapsis in normal lungs assessed by the relationship between maximal flow, static recoil, and vital capacity. The American Review of Respiratory Disease, 121(2), 339–342. https://doi.org/https://doi.org/10.1164/arrd.1980.121.2.339
- Meo, S. A., Ansary, M. A., Barayan, F. R., Almusallam, A. S., Almehaid, A. M., Alarifi, N. S., Alsohaibani, T. A., & Zia, I. (2019). Electronic cigarettes: Impact on lung function and fractional exhaled nitric oxide among healthy adults. American Journal of Men’s Health, 13(1), 1557988318806073. https://doi.org/https://doi.org/10.1177/1557988318806073
- Miller, M. R., Hankinson, J., Brusasco, V., Burgos, F., Casaburi, R., Coates, A., Crapo, R., Enright, P. V., Van Der Grinten, C., & Gustafsson, P. (2005). Standardisation of spirometry. European Respiratory Journal, 26(2), 319–338. https://doi.org/https://doi.org/10.1183/09031936.05.00034805
- Morse, C. I., Pritchard, L., Wüst, R. C., Jones, D. A., & Degens, H. (2008). Carbon monoxide inhalation reduces skeletal muscle fatigue resistance. Acta Physiologica, 192(3), 397–401. https://doi.org/https://doi.org/10.1111/j.1748-1716.2007.01757.x
- Polosa, R., Cibella, F., Caponnetto, P., Maglia, M., Prosperini, U., Russo, C., & Tashkin, D. (2017). Health impact of E-cigarettes: A prospective 3.5-year study of regular daily users who have never smoked. Scientific Reports, 7(1), 13825. https://doi.org/https://doi.org/10.1038/s41598-017-14043-2
- Richter, P., Pechacek, T., Swahn, M., & Wagman, V. (2008). Reducing levels of toxic chemicals in cigarette smoke: A new Healthy People 2010 objective. Public Health Reports, 123(1), 30–38. https://doi.org/https://doi.org/10.1177/003335490812300105
- Staudt, M. R., Salit, J., Kaner, R. J., Hollmann, C., & Crystal, R. G. (2018). Altered lung biology of healthy never smokers following acute inhalation of E-cigarettes. Respiratory Research, 19(1), 78. https://doi.org/https://doi.org/10.1186/s12931-018-0778-z
- Stockley, J. A., Ismail, A. M., Hughes, S. M., Edgar, R., Stockley, R. A., & Sapey, E. (2017). Maximal mid-expiratory flow detects early lung disease in α1 -antitrypsin deficiency. European Respiratory Journal, 49(3), 1602055. https://doi.org/https://doi.org/10.1183/13993003.02055-2016
- UK Medicines and Healthcare products Regulatory Agency. (2020). E-cigarette use or vaping: Reporting suspected adverse reactions, including lung injury. Medicines & healthcare products regulatory agency, Accessed 13 Feb 2021 from https://www.gov.uk/drug-safety-update/e-cigarette-use-or-vaping-reporting-suspected-adverse-reactions-including-lung-injury#context
- Vardavas, C. I., Anagnostopoulos, N., Kougias, M., Evangelopoulou, V., Connolly, G. N., & Behrakis, P. K. (2012). Short-term pulmonary effects of using an electronic cigarette: Impact on respiratory flow resistance, impedance, and exhaled nitric oxide. Chest, 141(6), 1400–1406. https://doi.org/https://doi.org/10.1378/chest.11-2443
- Xu, X., Li, B., & Wang, L. (1994). Gender difference in smoking effects on adult pulmonary function. European Respiratory Journal, 7(3), 477–483. https://doi.org/https://doi.org/10.1183/09031936.94.07030477
- Zakaria, R., Harif, N., Al-Rahbi, B., Aziz, C. B. A., & Ahmad, A. H. (2019). Gender differences and obesity influence on pulmonary function parameters. Oman Medical Journal, 34(1), 44. https://doi.org/https://doi.org/10.5001/omj.2019.07
