Abstract
In South Africa inequalities in health have been extensively reported. The poor suffer more ill health than the rich. This paper discusses the need to understand the historical, social and political contexts and power relations that have shaped inequalities in South Africa. This can be achieved in part through a cohesive intersectoral approach that addresses ‘the causes of the causes’. Yet more fundamentally, the authors suggest that success in tackling inequalities in health will only come when existing power structures in South African society are acknowledged.
1. Introduction
The link between absolute or average income levels and health has long been documented (Narayan et al., Citation2000; Deaton, Citation2002, Citation2003; Wagstaff, Citation2002). Low income levels (poverty) and ill health reinforce each other. There is also a growing body of evidence on the link between a broadly defined socioeconomic status and health (Mackenbach, Citation1992; Gwatkin, Citation2000; Mackenbach et al., Citation2008; Ataguba et al., Citation2011), education and health (Ross & Wu, Citation1995), and social protection and health (ADB et al., Citation2011). Generally, lower socioeconomic status, poorer educational attainment and absence of social protection are associated with poorer health and health outcomes. On this Deaton writes: ‘mortality and morbidity rates are inversely related to many correlates of socioeconomic status such as income, wealth, education, or social class’ (2002:13). While this link has been documented, the relationship between income inequality and health (or health outcomes) remains disputed (Coburn, Citation2000, Citation2004; Wagstaff & Van Doorslaer, Citation2000; Deaton, Citation2003; Macinko et al., Citation2003; Lynch et al. Citation2004a, Citation2004b; Wilkinson & Pickett, Citation2006).
A review by Macinko et al. Citation(2003) of about 50 studies revealed that, while about 70% of the studies reported significant evidence of a strong negative relationship between income inequality and health and health outcomes, about 30% did not. A more recent review by Wilkinson & Pickett Citation(2006), based on 168 analyses, found that even though some relationships were not statistically significant, a sizeable proportion of analyses support the inverse relationship between income inequality and health. In these authors' view this is related less to the link between income distribution and health and more to the degree of social stratification or social class differences. Thus they conclude that
income distribution is related to health where it serves as a measure of the scale of social class differences in a society … In small areas, where income inequality is unlikely to reflect the degree of social stratification in the wider society, it is [as the authors show] less likely to be related to health. The overwhelmingly positive evidence of studies of larger areas suggests that this interpretation is correct. The fact that social stratification is such a fundamental feature of social organisation explains why there are so many socioeconomic factors correlated with inequality. (Wilkinson & Pickett, Citation2006:1778)
In the context of South Africa, we argue for a broader, holistic and integrated approach to addressing health inequalities that recognises the social, political and economic determinants of health and, more particularly still, relates this to issues of mal-distribution and imbalances in power in South African society. We contend that too little attention has been paid both to understanding the underlying causes of income inequality (Coburn, Citation2000; Macinko et al., Citation2003) and deciding what interpretation is to be placed on income inequality. We agree with Coburn's argument that more attention should be paid to ‘understanding the causes of income inequalities and not just to its effects’ and that ‘understanding the contextual causes of inequality may also influence our notion of the causal pathways involved in inequality-health status relationships (and vice versa)’ (2000:135). The need to emphasise ‘the causes of the causes’ has also been echoed by the World Health Organisation (WHO) (Krech, Citation2011).
2. Beyond describing the social determinants of health
The WHO Commission on Social Determinants of Health (CSDH) was launched in 2005 to tackle increasing health inequities by compiling scientific evidence on the social determinants of health (WHO, Citation2009). These determinants are the social, political, economic, environmental and cultural factors that affect health status (Halfon et al., Citation2010). The CSDH recommends a collaborative and intersectoral policy action that would involve improving daily living conditions; tackling the inequitable distribution of power, money and resources; measuring and understanding the problem; and assessing the impact of action (CSDH, Citation2008; WHO, 2009, Citation2011).
While these areas of action are important, we argue that in South Africa we need to go further and first examine and secondly address the causes of inequalities in health. If we fail to understand the causes, the prospects of identifying appropriate specific strategies are diminished. Coburn Citation(2000), Wilkinson & Pickett Citation(2006), Navarro Citation(2007), and Mooney Citation(2009) identify class as the cause in western societies. We argue that in South Africa the cause is essentially inequalities in power. Though power can be defined in different ways, it is essentially related to domination and control of resources. Class and power are therefore linked. The class-domination theory, for instance, is linked to different bases or sources of power, including the Marxian economic basis (Domhoff & Webber, Citation2011). Other power bases are political, military, ideological and religious.
South Africa has pursued predominantly neoliberal policies since apartheid ended in 1994 (see Bond et al., Citation1997). While neoliberalism can be understood in different ways, it is essentially ‘built on a single, fundamental principle: the superiority of individualized, market-based competition over other modes of organization’ (Mudge, Citation2008:706–7). It is an ideology based on the market system and has generally led to cuts in public spending on social services. International evidence suggests that neoliberalism can be detrimental to population health and could decrease social cohesion (see for example Coburn, Citation2000; McGregor, Citation2001; Navarro, Citation2007) and increase health inequality. This neoliberal ideology has not only exacerbated inequality in incomes in South Africa but also led to major deficiencies in social and health services and a concentration of power in a small elite which is in alliance with large corporations, especially in the mining and energy sectors (Williams & Taylor, Citation2000; Hallowes & Munnik, Citation2007; Baker, Citation2010). It has also fuelled the rapid growth in the private health sector, which caters for less than 20% of the population, and a decline in government commitment to health care (McIntyre et al., Citation2007). While apartheid is formally a thing of the past, in terms of education, health and social services there remains a major divide between black and white. Though inequalities in education, health and access to social services can be argued to go beyond racial divides (Seekings & Nattrass, Citation2002), it is still the case that race matters. The former white elite, even if not there in government, remain powerful especially in a neoliberal state in which there are such strong links between government and corporations.
Inequalities in health in South Africa have been extensively reported (Eyob & McIntyre, Citation2003; Zere & McIntyre, Citation2003; Ataguba et al., Citation2011). The poor suffer more ill health than the rich. These inequalities are of course not restricted to health and health care, as the poor suffer from multiple deprivations. According to Klasen, they ‘suffer from lack of access to education, quality health care, basic infrastructure, transport, are heavily indebted, have little access to productive resources, and are heavily dependent on remittances and social transfers, particularly social pensions and disability grants’ (Citation1997:51). These problems, to a large extent, can be linked to history.
During the apartheid era, the South African health care sector was segregated. Health policy aimed to maintain economic and political power and a better quality of life for the minority white population (McIntyre et al., Citation2007). Health services for the black majority were severely underfunded and rural areas were neglected (Kale, Citation1995; McIntyre & Gilson, Citation2002). The same was true of the educational system that was described as the pillar of the apartheid system (Thomas, Citation1996). Though the current systems are evolving to address the existing inequities caused by the apartheid legacy, significant gaps still remain (DoH, Citation2011; Lam et al., Citation2011). A recent study using a nationally representative sample shows that the health system is inequitable (Ataguba & McIntyre, Citation2012), as the use of health services does not follow the distribution of need for such services.
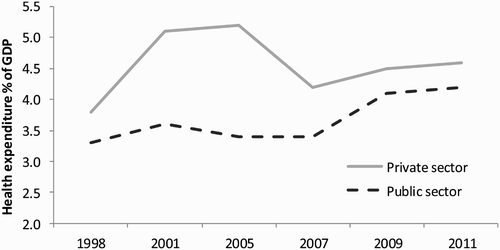
In South Africa, capital is noted to retain ‘enormous power, not because of the voting power of capitalists in elections but because of their importance to the economy’ (Seekings & Nattrass, Citation2002:2). The implication of this is the development of capitalist institutions that have backed the growth of the private health sector in the country. Total private sector expenditure as a proportion of GDP has continued to exceed that of the public sector (see ). On this, Coovadia et al., for instance, write that the development of the private health sector:
was largely stimulated by corporate capital, particularly the mining houses. These capitalist institutions are far more powerful and have influenced the political economy of South Africa and its health system to a greater extent than in most other post-colonial African and Asian countries. (2009:826)
More recently, uneven and unfair distribution of social power and relationships, and poverty and rural–urban differences have also been noted as underlying some of the existing inequalities in access to health care in South Africa (Harris et al., Citation2011).
A major challenge faced by the South African health sector has been the public–private mix (McIntyre et al., Citation2012), which is inextricably linked to the neoliberal policies of the country and the capitalist institutions. Coovadia et al. Citation(2009) note that before the 1970s, private medical schemes in South Africa catered for the health care needs of white mine workers, with membership being restricted to white people. While this refers to the ‘old’ South Africa, a recent study using a nationally representative dataset also shows that a white South African has a significantly higher likelihood of being a medical scheme member and that blacks are disproportionately less represented as scheme members (Ataguba & Goudge, Citation2012). Membership of a medical scheme also follows income and employment levels: the poorest and the non-formally employed South Africans are almost invariably not scheme members (Ataguba & Goudge, Citation2012).
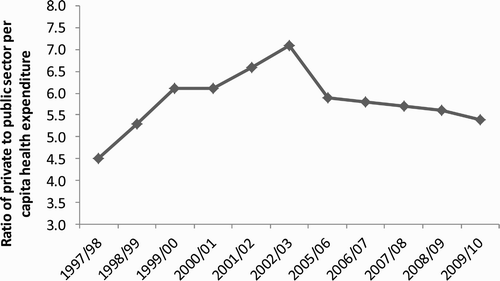
One can well argue that private medical schemes are not the same as public schemes or programmes and should not be viewed as such, and further, that public health services are available to cater for the majority of South Africans. However, these arguments need to be placed in the context of the current resource distribution between both sectors of the health system. Private medical schemes alone account for over 43% of total health care financing, while less than one sixth of the population, mainly the richest, are scheme members (McIntyre et al., Citation2007). The disparities in expenditure between the public and private sectors relative to the population they serve have widened over time, as reflected in the gap in per capita expenditure between the sectors (McIntyre et al., Citation2012). As shows, the ratio of private to public sector per capita health expenditure has been greater than 5 for the most part between 1997 and 2010.
Williams and Taylor write that in South Africa the:
adoption of neoliberal principles has exacerbated inequality and increased the concentration of wealth in the hands of the privileged few. Apart from the ethically odious (and increasingly dangerous) prospect of living in one of the world's most unequal economies, such a polarised environment is fertile ground for social and political instability. (2000:37)
The WHO notes that inequity in power ‘interacts across four main dimensions – political, economic, social, and cultural – together constituting a continuum along which groups are, to varying degrees, excluded or included’ within or across countries (2008:2). Though this issue is broader than the issue of political power, Drèze & Sen Citation(1989) have noted elsewhere within the context of poverty and deprivation that the skewed concentration of political power in the hands of a few is the major driver of severe neglect of the basic needs of disadvantaged groups. These issues of power are not easy to address, especially as they are so often shaped by time and history (Young, Citation2010) and in the case of Africa generally still influenced by the power relations of colonial times (Ichoku et al., Citation2012). We argue that recognising these power relations and their distribution is critical to reducing health inequalities in pluralistic societies like South Africa. This will require that, as health economists, we turn more and more to the political economy of health to understand these issues.
Mooney, for instance, drawing on Navarro's development of a national health policy (2007), argues that there is a ‘need to embrace policies aimed at reducing inequalities in any national health policy’ and that, more fundamentally, a national health policy ‘must address issues of power’ (2009:178). He stresses that a national health policy is not just social but also political. And so also is public health (Navarro, Citation2011). If in our analyses we fail to consider society's power structures, much of our work will be in vain. It is these power structures that can be used to encourage policies that promote or hinder population health.
More generally, the importance of universal health coverage (Carrin et al., Citation2008; Garrett et al., Citation2009; Harris et al., Citation2011) has been stressed for tackling health inequalities. This has been embraced by South Africa in the form of a proposed national health insurance (NHI) (DoH, 2011), which would focus on the health care sector with only limited linkage to other relevant social service sectors. Largely separate and independent efforts exist in education, public works, and other social service sectors. The complementarity of sectors, through a coherent intersectoral approach, is required if we are to achieve significant reductions in health inequalities (Whitehead, Citation1992). For example, social and political forces affect health inequalities (Navarro & Shi, Citation2001). It is also the case that the educated, those who live in clean environments, the empowered, and those with better life opportunities, generally enjoy better health (Grossman, Citation1972; Wagstaff, Citation1993; Deaton, Citation2002).
While there is some recognition of these issues in the literature generally (Navarro & Shi, Citation2001; Ataguba et al., Citation2011), in South Africa, as in many other developing countries, there is yet to be a coherent and well-structured policy that draws on the existing evidence and builds on the existing structures and institutions to combat health inequalities. Though not explicitly acknowledging the social determinants of health, Deaton argues that the ‘U.S. system pays too much attention to health care delivery and to drugs and too little to the effects on health of the “upstream” social and economic arrangements’ (2002:27). Some of the problems in South Africa, as noted earlier, can be traced to its apartheid history and the struggles then and since faced by different racial and gender groups. South Africa can build on the social determinants of health (Marmot, Citation2011) and the NHI while recognising the underlying power distribution that has shaped health inequalities.
The anticipated gains from the NHI in South Africa can only be consolidated by strengthening and integrating other structures beyond the health sector. The broader determinants of health must be recognised, but it must also be acknowledged that it is the existing power structures that are driving these inequalities. Going down this route offers greater promise of reducing overall health inequalities in South Africa.
3. Conclusion
Deaton writes that any policy ‘cannot be intelligently conducted without an understanding of mechanisms; correlations are not enough’ (2002:15). We need to go beyond analysing the distribution of inequalities and also their correlations and use this as a starting point for addressing health inequalities in South Africa. While this is relevant, though, we insist that there is a need to get yet further than Deaton proposes. What we need is to understand the historical, social and political contexts and power relations that have shaped inequalities in South Africa and also how these have shaped the policies that have been used to address them. This further requires a coherent intersectoral approach that will account for the interrelatedness of factors that are associated with health inequalities in South Africa. Inequalities in power need also to be acknowledged. We contend that this is a better strategy to adopt in seeking to redress health inequalities than focusing on the health care sector or on other related sectors in isolation.
Acknowledgements
The authors acknowledge the invaluable comments and suggestions made by Gavin Mooney.
Notes
References
- ADB, UNECA, AU & UNDP (African Development Bank, UN Economic Commission for Africa, African Union & United Nations Development Programme), 2011. Assessing progress in Africa toward the Millennium Development Goals: MDG Report 2011. http://web.undp.org/africa/mdg/report.pdf Accessed 24 August 2012.
- Ataguba , J E and Goudge , J . 2012 . The impact of health insurance on health care utilisation and out-of-pocket payments in South Africa . The Geneva Papers on Risk and Insurance: Issues and Practice , 37 ( 4 ) : 633 – 654 . (doi:10.1057/gpp.2012.35)
- Ataguba , J E and McIntyre , D . 2012 . Who benefits from health services in South Africa? . Health Economics, Policy and Law , advance online publication 2 April, doi: 10.1017/S1744133112000060
- Ataguba , J E , Akazili , J and McIntyre , D . 2011 . Socioeconomic-related health inequality in South Africa: Evidence from General Household Surveys . International Journal for Equity in Health , 10 ( 1 ) : 48 (doi:10.1186/1475-9276-10-48)
- Baker , P A . 2010 . From apartheid to neoliberalism: Health equity in post-apartheid South Africa . International Journal of Health Services , 40 ( 1 ) : 79 – 95 . (doi:10.2190/HS.40.1.e)
- Bond , P , Pillay , Y G and Sanders , D . 1997 . The state of neoliberalism in South Africa: Economic, social, and health transformation in question . International Journal of Health Services , 27 ( 1 ) : 25 – 40 . (doi:10.2190/6RRJ-NYGL-X8LE-7UC5)
- Carrin , G , Mathauer , I , Xu , K and Evans , D B . 2008 . Universal coverage of health services: Tailoring its implementation . Bulletin of the World Health Organization , 86 ( 11 ) : 857 – 63 . (doi:10.2471/BLT.07.049387)
- Coburn , D . 2000 . Income inequality, social cohesion and the health status of populations: The role of neo-liberalism . Social Science & Medicine , 51 ( 1 ) : 135 – 46 . (doi:10.1016/S0277-9536(99)00445-1)
- Coburn , D . 2004 . Beyond the income inequality hypothesis: Class, neo-liberalism, and health inequalities . Social Science & Medicine , 58 ( 1 ) : 41 – 56 . (doi:10.1016/S0277-9536(03)00159-X)
- Coovadia , H , Jewkes , R , Barron , P , Sanders , D and McIntyre , D . 2009 . The health and health system of South Africa: Historical roots of current public health challenges . The Lancet , 374 ( 9692 ) : 817 – 34 . (doi:10.1016/S0140-6736(09)60951-X)
- CSDH (Commission on Social Determinants of Health), 2008. Closing the gap in a generation: Health equity through action on the social determinants of health. Final Report of the Commission on Social Determinants of Health, World Health Organization, Geneva.
- Deaton , A . 2002 . Policy implications of the gradient of health and wealth . Health Affairs , 21 ( 2 ) : 13 – 30 . (doi:10.1377/hlthaff.21.2.13)
- Deaton , A . 2003 . Health, inequality, and economic development . Journal of Economic Literature , 41 ( 1 ) : 113 – 58 . (doi:10.1257/002205103321544710)
- DoH (Department of Health) . 2011 . National Health Insurance in South Africa , Pretoria : National Department of Health .
- Domhoff , G W and Webber , MJ . 2011 . Class and Power in the New Deal: Corporate Moderates, Southern Democrats, and the Liberal–Labour Coalition , Stanford : Stanford University Press .
- Drèze , J and Sen , A K . 1989 . Hunger and Public Action , Oxford : Oxford University Press .
- Eyob , Z and McIntyre , D . 2003 . Inequities in under-five child malnutrition in South Africa . International Journal for Equity in Health , 2 : e7 (doi:10.1186/1475-9276-2-7)
- Garrett , L , Chowdhury , A and Pablos-Méndez , A . 2009 . All for universal health coverage . The Lancet , 374 ( 9697 ) : 1294 – 99 . (doi:10.1016/S0140-6736(09)61503-8)
- Gilson , L and McIntyre , D . 2005 . Removing user fees for primary care in Africa: The need for careful action . British Medical Journal , 331 ( 7519 ) : 762 – 5 . (doi:10.1136/bmj.331.7519.762)
- Grossman , M . 1972 . On the concept of health capital and the demand for health . Journal of Political Economy , 80 ( 2 ) : 223 – 55 . (doi:10.1086/259880)
- Gwatkin , D R . 2000 . Health inequalities and the health of the poor: What do we know? What can we do? . Bulletin of the World Health Organization , 78 ( 1 ) : 3 – 18 .
- Halfon , N , Larson , K and Russ , S . 2010 . Why social determinants? . Healthcare Quarterly , 14 : 9 – 20 .
- Hallowes , D and Munnik , V . 2007 . Peak Poison: The Elite Energy Crisis and Environmental Justice , Pietermaritzburg : groundWork .
- Harris , B , Goudge , J , Ataguba , J E , McIntyre , D , Nxumalo , N , Jikwana , S and Chersich , M . 2011 . Inequities in access to health care in South Africa . Journal of Public Health Policy , 32 ( Suppl. 1 ) : S102 – 23 . (doi:10.1057/jphp.2011.35)
- Ichoku , H E , Fonta , WM and Ataguba , J E . 2012 . Political economy and history: Making sense of health financing in sub-Saharan Africa . Journal of International Development , advance online publication 10 May, doi: 10.1002/jid.2842
- Kale , R . 1995 . Impressions of health in the new South Africa: A period of convalescence . British Medical Journal , 310 ( 6987 ) : 1119 – 22 . (doi:10.1136/bmj.310.6987.1119)
- Kawachi , I and Kennedy , B P . 1997 . Health and social cohesion: Why care about income inequality? . British Medical Journal , 314 ( 7086 ) : 1037 – 40 . (doi:10.1136/bmj.314.7086.1037)
- Kawachi , I , Kennedy , B P , Lochner , K and Prothrow-Stith , D . 1997 . Social capital, income inequality, and mortality . American Journal of Public Health , 87 ( 9 ) : 1491 – 8 . (doi:10.2105/AJPH.87.9.1491)
- Klasen , S . 1997 . Poverty, inequality and deprivation in South Africa: An analysis of the 1993 SALDRU survey . Social Indicators Research , 41 ( 1 ) : 51 – 94 . (doi:10.1023/A:1006892216864)
- Krech , R . 2011 . Social determinants of health: Practical solutions to deal with a well-recognized issue . Bulletin of the World Health Organization , 89 ( 10 ) : 703 (doi:10.2471/BLT.11.094870)
- Lam , D , Ardington , C and Leibbrandt , M . 2011 . Schooling as a lottery: Racial differences in school advancement in urban South Africa . Journal of Development Economics , 95 ( 2 ) : 121 – 36 . (doi:10.1016/j.jdeveco.2010.05.005)
- Lynch , J , Smith , G D , Harper , S and Hillemeier , M . 2004a . Is income inequality a determinant of population health? Part 2. US national and regional trends in income inequality and age- and cause-specific mortality . Milbank Quarterly , 82 ( 2 ) : 355 – 400 . (doi:10.1111/j.0887-378X.2004.00312.x)
- Lynch , J , Smith , G D , Harper , S , Hillemeier , M , Ross , N , Kaplan , G A and Wolfson , M . 2004b . Is income inequality a determinant of population health? Part 1. A systematic review . Milbank Quarterly , 82 ( 1 ) : 5 – 99 . (doi:10.1111/j.0887-378X.2004.00302.x)
- Macinko , J A , Shi , L , Starfield , B and Wulu , J T . 2003 . Income inequality and health: A critical review of the literature . Medical Care Research and Review , 60 ( 4 ) : 407 – 52 . (doi:10.1177/1077558703257169)
- Mackenbach , J . 1992 . Socio-economic health differences in the Netherlands. A review of recent empirical findings . Social Science & Medicine , 34 ( 3 ) : 213 – 26 . (doi:10.1016/0277-9536(92)90264-Q)
- Mackenbach , J P , Stirbu , I , Roskam , AJ R , Schaap , MM , Menvielle , G , Leinsalu , M and Kunst , A E . 2008 . Socioeconomic inequalities in health in 22 European countries . New England Journal of Medicine , 358 ( 23 ) : 2468 – 81 . (doi:10.1056/NEJMsa0707519)
- Marmot , M . 2011 . Global action on social determinants of health . Bulletin of the World Health Organization , 89 ( 10 ) : 702 (doi:10.2471/BLT.11.094862)
- McGregor , S . 2001 . Neoliberalism and health care . International Journal of Consumer Studies , 25 ( 2 ) : 82 – 9 . (doi:10.1111/j.1470-6431.2001.00183.x)
- McIntyre , D and Gilson , L . 2002 . Putting equity in health back onto the social policy agenda: Experience from South Africa . Social Science & Medicine , 54 ( 11 ) : 1637 – 56 . (doi:10.1016/S0277-9536(01)00332-X)
- McIntyre , D , Doherty , J E and Ataguba , J E . 2012 . “ Health care financing and expenditure: Post-1994 progress and remaining challenges ” . In Health and Health Care in South Africa , Edited by: Van Rensburg , HC J . Pretoria : Van Schaik .
- McIntyre , D , Thiede , M , Nkosi , M , Mutyambizi , V , Castillo-Riquelme , M , Gilson , L , Erasmus , E and Goudge , J . 2007 . “ A critical analysis of the current South African health system ” . In Health Economics Unit, University of Cape Town and Centre for Health Policy , Cape Town : University of the Witwatersrand .
- Mooney , G . 2009 . Challenging Health Economics , New York : Oxford University Press .
- Mudge , S L . 2008 . What is neo-liberalism? . Socio-Economic Review , 6 ( 4 ) : 703 – 31 . (doi:10.1093/ser/mwn016)
- Narayan , D , Patel , R , Schafft , K , Rademacher , A and Koch-Schulte , S . 2000 . Voices of the Poor: Can Anyone Hear Us? , New York : Oxford University Press .
- Navarro , V . 2007 . Neoliberalism, Globalization, and Inequalities: Consequences for Health and Quality of Life. Baywood New York
- Navarro , V . 2011 . Why we don't spend enough on public health: An alternative view . International Journal of Health Services , 41 ( 1 ) : 117 – 20 . (doi:10.2190/HS.41.1.h)
- Navarro , V and Shi , L . 2001 . The political context of social inequalities and health . Social Science & Medicine , 52 ( 3 ) : 481 – 91 . (doi:10.1016/S0277-9536(00)00197-0)
- Ross , C E and Wu , C . 1995 . The links between education and health . American Sociological Review , 60 : 719 – 45 . (doi:10.2307/2096319)
- Seekings , S and Nattrass , N . 2002 . Class, distribution and redistribution in post-apartheid South Africa . Transformation , 50 : 1 – 30 . (doi:10.1353/trn.2003.0014)
- Thomas , D . 1996 . Education across generations in South Africa . The American Economic Review , 86 ( 2 ) : 330 – 4 .
- Wagstaff , A . 1993 . The demand for health: An empirical reformulation of the Grossman model . Health Economics , 2 ( 2 ) : 189 – 98 . (doi:10.1002/hec.4730020211)
- Wagstaff , A . 2002 . Poverty and health sector inequalities . Bulletin of the World Health Organization , 80 : 97 – 105 .
- Wagstaff , A and Van Doorslaer , E . 2000 . Income inequality and health: What does the literature tell us? . Annual Review of Public Health , 21 ( 1 ) : 543 – 67 . (doi:10.1146/annurev.publhealth.21.1.543)
- Whitehead , M . 1992 . The concepts and principles of equity and health . International Journal of Health Services , 22 ( 3 ) : 429 – 45 . (doi:10.2190/986L-LHQ6-2VTE-YRRN)
- Wilkinson , R G . 1992 . Income distribution and life expectancy . British Medical Journal , 304 ( 6820 ) : 165 – 8 . (doi:10.1136/bmj.304.6820.165)
- Wilkinson , R G and Pickett , KE . 2006 . Income inequality and population health: A review and explanation of the evidence . Social Science & Medicine , 62 ( 7 ) : 1768 – 84 . (doi:10.1016/j.socscimed.2005.08.036)
- Williams , P and Taylor , I . 2000 . Neoliberalism and the political economy of the ‘new’ South Africa . New Political Economy , 5 ( 1 ) : 21 – 40 . (doi:10.1080/13563460050001961)
- WHO (World Health Organization) . 2008 . Social determinants of health: Key concepts , Geneva : WHO . www.who.int/social_determinants/final_report/key_concepts_en.pdf Accessed 24 August 2012
- WHO (World Health Organization) . 2009 . “ World Health Assembly 62.9 ” . In Commission on Social Determinants of Health , Geneva : WHO . http://apps.who.int/gb/ebwha/pdf_files/A62/A62_9-en.pdf Accessed 9 January 2012
- WHO (World Health Organization) . Rio political declaration on social determinants of health . Presented at WHO World Conference on Social Determinants of Health . 19–21 October . Rio de Janeiro . www.who.int/sdhconference/declaration/Rio_political_declaration.pdf Accessed 15 January 2012
- Young , A R . 2010 . Perspectives on the changing global distribution of power: Concepts and context . Politics , 30 ( s1 ) : 2 – 14 . (doi:10.1111/j.1467-9256.2010.01390.x)
- Zere , E and McIntyre , D . 2003 . Equity in self-reported adult illness and use of health service in South Africa: Inter-temporal comparison . Journal of Health, Population and Nutrition , 21 ( 3 ) : 205 – 15 .