Abstract
Identification of factors causing acute renal failure (ARF) and its associated poor prognosis in critically ill patients can help in planning strategies to prevent ARF and to prioritize the utilization of sparse and expensive therapeutic modalities. Most of the studies in such patients have been done in the developed world, and similar data from the developing world is sparse.
We analyzed 45 consecutive patients who developed ARF in the intensive care unit (ICU) during a 12-month period. Demographic and detailed biochemical profile, previous chronic illness, precipitating factors, number of failed organs, type of ARF (oliguric/nonoliguric), and need for and type of renal replacement therapy (RRT) received were recorded at the time of admission to ICU and during the course of illness. The mean age of these patients was 43.1 years, with 75.6% being males. Hypotension, sepsis, and use of nephrotoxic drugs were common precipitating factors for ARF in these patients. However, multiple precipitating factors were present in the majority (80%): 81.5% had at least one organ failure prior to development of ARF, 71.1% had oliguria, and 71.1% required RRT. Intermittent hemodialysis was the most common form of RRT given. Patient mortality was 64.4%, with 15 of the 16 surviving patients becoming dialysis independent. We observed an increase in mortality from 0% to 100%, depending on the number of failed organs from one to six. On comparing the predictor outcomes between survivors and nonsurvivors by multivariate analysis, only the number of failed organs at the time of ARF (2.6 ± 0.9 vs. 4.5 ± 0.8) and serum albumin <3.0 g/dL were found to be statistically significant.
To conclude, ARF in critically ill patients is multifactorial in origin and carries a high mortality. Mortality in these patients increases with increasing numbers of failed organs and with a serum albumin of <3.0 g/dL.
INTRODUCTION
Acute renal failure (ARF) is a common and serious complication in critically ill patients. The reported incidence of ARF in intensive care unit (ICU) varies from 3% to 25%, depending on the population studied and criteria used to define ARF.Citation[1–4] The mortality in these patients continues to be high despite advances made in renal replacement therapy (RRT) and in the management of metabolic and infective complications.Citation[1],Citation[4–13] Possible explanation for this finding could be the fact that ICU patients today are more debilitated then before and have multiple organ failure syndrome (MOF).Citation[14],Citation[15] Development of ARF has also been shown to have a significant negative impact on patient outcome irrespective of the degree of renal dysfunction.Citation[16] Most of the studies pertaining to the epidemiologic and prognostic profile of ARF in critically ill patients have been performed in the developed world. Because a recent multicenter trial has documented a wide variation in the spectrum of ARF among different centers,Citation[17] it is therefore important to look into the epidemiologic and prognostic profile of critically ill ARF patients in India. Such a profile would be important in guiding us to plan strategies to prevent ARF, prognosticate the patients, and prioritize the utilization of sparse and expensive therapeutic modalities. The aim of this single center study was to determine the incidence and cause of ARF in ICU patients, delineate important precipitating factors, and define the prognostic factors affecting the outcome of these patients.
PATIENTS AND METHODS
This study was carried out in a tertiary care state-run hospital providing speciality and superspecialty care. We analyzed 45 consecutive patients developing ARF in ICUs from January 1, 2003 to December 31, 2003. The ICUs included were general surgery ICU, medical ICU, neurosurgery ICU, and cardiothoracic ICU. Clinical and biochemical profile and the predictor variables under study were identified at the time of admission to ICU and at the time of development and subsequent course of ARF.
Renal replacement therapy (RRT) was begun whenever needed on clinical grounds. Intermittent hemodialysis (IHD) was performed in hemodynamically stable patients using volumetrically controlled, bicarbonate-based machines using biocompatible hemodialyzers. Due to constraints of resources, peritoneal dialysis (PD) using an acute PD catheter was performed as the preferred modality in patients with hemodynamic instability if there was no specific contraindication. Hemodynamically unstable patients in whom PD was contraindicated or had failed due to technical reasons were subjected to continuous venovenous hemodiafiltration (CVVHD).
Variables studied
Demographic profile, presumed precipitating factors, medical/surgical/obstetric ARF, and preexisting medical conditions such as hypertension, diabetes, coronary artery disease, malignancy, and renal disease were recorded. A record of the number of failed organs at the time of ICU admission and during subsequent course, oliguric or nonoliguric renal failure, peak serum creatinine, need for RRT, and type of RRT given was also kept.
Definitions
ARF was defined as a rise of serum creatinine to >2 mg/dL or a 25% rise of serum creatinine from the baseline in patients with chronic kidney disease (CKD). Oliguria was defined as urine output <400 mL/24 h. Mortality was defined as death of the patient in the hospital, independent of whether renal function was restored. Sepsis was defined according to the ACCP/SCCM Consensus.Citation[18] Organ system failures were defined as per standard criteria and are shown in .Citation[19] CKD was defined as a documented serum creatinine of >1.8 mg/dL prior to onset of the present illness.
Table 1 Criteria for organ failureCitation[19]
To see association between various study variables among the survivors and nonsurvivors by univariate analysis, a chi-square test was applied for all variables. P value of <0.05 was taken as statistically significant value. Multivariate stepwise logistic analysis was performed for variables found significant on univariate analysis.
RESULTS
Forty five patients (34 males and 11 females) were recorded as having ARF in the ICUs during the study period. shows the demographic and baseline profile of these patients. The mean age of study population was 43.1 ± 19.9 years (range 13–84 years). Six patients (13.2%) were less than 20 years of age, and 10 (22.1%) were older than 60 years of age. Thirty one patients (68.7%) had ARF due to medical causes that were usually multifactorial. Eleven (24.3%) had ARF following surgical procedure (3 each following cardiovascular, neurologic, and gastrointestinal surgery and 2 following orthopedic surgery). Three patients (6.7%) had ARF following obstetric complications (2 due to septic abortion, 1 due to antepartum hemorrhage). Thirty two (71.1%) had oliguric renal failure, where as 13 (29%) had nonoliguric ARF. The ratio of oliguric to nonoliguric renal failure was thus 2.5 : 1. Of the 10 patients who were having CKD, 3 patients had CKD due to presumed chronic glomerulonephritis; 2 patients each had CKD due to diabetic nephropathy, hypertensive nephrosclerosis, and presumed chronic interstitial nephritis; and 1 patient had CKD due to amyloidosis. The major factors precipitating ARF were hypotension (75.6%), sepsis (73.2%), use of nephrotoxic drugs (53.2%), and dehydration (22.1%). Among drugs, aminoglycosides were offending agents in 12 (50%) cases, followed by amphotericin B in 6 (25%) cases, nonsteroidal anti-inflammatory drugs in 4 (16.7%) cases, and contrast agents in 2 (8.2%) cases. Eighty percent of patients had more than one precipitating factor at the same time. There was no significant difference in etiology of ARF in the age groups of 21 to 59 and >60 years. Medical causes accounted for 69% and 60% cases, where as surgical causes accounted for 20.7% and 40% cases in these two groups, respectively. Among the precipitating factors, hypotension, sepsis, nephrotoxic drug use, and dehydration were responsible in 72.3%, 75.9%, 55.2%, and 17.1% cases of ARF in age group of 21 to 59 years and 80%, 80%, 60%, and 30% cases, respectively, in patients ages >60 years. Thirty two patients (71.1%) required dialytic support. Seven patients (21.9%) were given only PD, 19 (59.4%) were given only IHD, 5 patients (15.5%) were given PD followed by IHD, and 1 patient (3.1%) was given PD followed by CVVHD.
Table 2 Demographic and baseline profile of study population
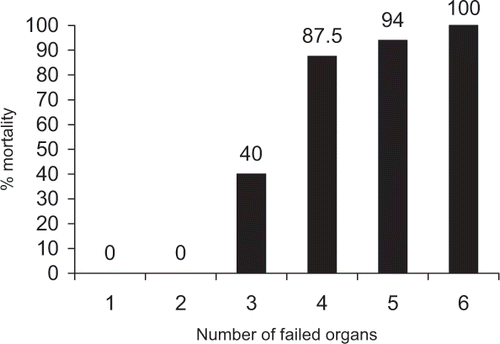
We observed a mortality of 64.4% (29 patients). Of the 16 patients who survived, 15 became dialysis independent and 1 patient remained dialysis dependent at discharge. The mean duration of dialysis in 15 patients who became dialysis independent was 26.4 ± 7.2 days (range 5–40 days). and show the predictor variables among the survivors and nonsurvivors at the time of admission to ICU and at development and course of ARF, respectively. The factors found to be significantly associated with increased mortality on univariate analysis at the time of admission to ICU were age >60 years; prior history of diabetes; hematologic, cardiovascular, and respiratory failure; and presence of sepsis. At the time of development of ARF, hematologic, cardiovascular, central nervous system, and respiratory failure; presence of sepsis; oliguria; use of nephrotoxic drugs; and serum albumin <3.0 g/dL were found to be significantly associated with increased mortality on univariate analysis. However, on multivariate analysis, the factors that were found to be significantly associated with increased mortality were number of failed organs at time of ARF development (2.6 ± 0.9 vs. 4.5 ± 0.8 in survivors vs. nonsurvivors, P value = 0.018) and serum albumin of <3.0 g/dL (p value = 0.01). The mortality increased from 0% to 100% as the number of failed organs increased from one to six ().
Table 3 Presence of predictor variables for outcome at time of admission to ICU (univariate analysis)
Table 4 Presence of predictor variables for outcome at time of detection and during course of ARF (univariate analysis)
DISCUSSION
In this study, we have analyzed the spectrum, precipitating, and prognostic factors of ARF in ICU patients in a tertiary care specialty/superspecialty hospital from a developing world. The mean age of patients developing ARF was 43.1 years, with 76.5% of them being males. Medical causes accounted for majority of cases (68.8%) followed by surgical (24.4%) and obstetric causes (6.7%). The principal factors precipitating ARF were hypotension (75.6%), sepsis (73.2%), use of nephrotoxic drugs (53.2%), and dehydration (22.1%). 80.5% of patients were having at least one organ failure prior to onset of ARF. The spectrum of ARF in critically ill patients has not been clearly delineated in our country. In the only other study from India, Sural et al.Citation[13] found that of the patients developing ARF in their ICU, 70% had had a surgical procedure, in particular cardiac and pancreatic surgery. Sural et al., however, had conducted their study in a super speciality care hospital not directly dealing with medical, obstetric, and general surgery specialties, which could explain the difference in causes of ARF. Observed male preponderance in our study corresponds well with the majority of studies in literature.Citation[1],Citation[4],Citation[6],Citation[20] The mean age of our study population is, however, much lower than several other studies from the developed world,Citation[1],Citation[6],Citation[20] which have reported a mean age of 56.4 to 60.3 years. The different spectrum of ARF in our population and preferential admission of younger patients to ICU due to limited intensive care facilities and resources could explain this discrepancy. Hypotension, sepsis, use of nephrotoxic drugs, and dehydration were found to be major precipitating factors for ARF, with most of the patients having one or more of these. The crucial role that these factors play in the development of ARF is well documented.Citation[7],Citation[21] However, the presence of these factors in high percentage of our patients could be due to the fact that refractory hypotension induced by sepsis and MOF requires the use of aggressive antibiotics and antifungal medications, which can be nephrotoxic.
Similar studies in high-risk critically ill patients have reported a mortality ranging from 43% to 75%,Citation[3–12] which corresponds well with the mortality of 64.5% observed in our study. Although a number of studies analyzing factors determining outcome in ARF have been carried out, these studies are difficult to compare because of difference in patient population and definition of clinical factors and outcome measures.Citation[13],Citation[22] Most of these studies have been retrospective and only a few have used the powerful statistical tool of multivariate analysis. Also, multivariate analysis of survival factors based on a time-to-event occurrence as done in our study is more appropriate in evaluating the dynamics between different factors, rather than a single-point assessment as done in most studies. On multivariate analysis, there was a significant association between the number of failed organs and increased mortality. We observed an increase in the mortality from 0% to 100%, depending on the number of organ failure from one to six. Similar result was found in a study from TaiwanCitation[23] in which a mortality of 0%, 18.2%, 53.3%, 83.3%, 89.5%, and 100% was reported with increasing numbers of organ failures from one to six. Although only 18.2% patients with sepsis at enrollment survived as compared with 84.4% in patients without sepsis, it was not found to be statistically significant on multivariate analysis. Similarly, patients having hypotension had a mortality of 91.1% as compared with 33.3% in patients without hypotension, which again was not statistically significant on multivariate analysis. Interdependence of sepsis and hypotension with other determinants such as respiratory failure and disseminated intravascular coagulation (DIC) could explain these findings.
The only other factor found to be significantly associated with increased mortality on multivariate analysis was a serum albumin of less than 3.0 g/dL. Obialo et al.Citation[24] observed that mortality in their ARF patients was 52% among patients with serum albumin <3.5 g/dL as compared with 18% with serum albumin >3.5 g/dL (p = 0.06 on multivariate analysis). Similarly, Fiaccadori et al.Citation[25] noted mortality to be significantly higher in malnourished as compared with well-nourished ARF patients (odds ratio 2.02; 95% CI 1.50–2.71, p < 0.001). Thus, the increased mortality with low serum albumin observed in our series of ARF in critically ill patients could be due to preexisting malnutrition in these patients and/or cytokine-mediated inflammatory response.Citation[24],Citation[25] This, however, requires further confirmation in larger series.
Our study has a few limitations. Because this study was conducted in an academic medical center that serves as a referral center for more complex and severe disease, we may therefore have overestimated the associated comorbidities and severity of illness relative to what would be expected across institutions providing mainly primary and community-based care.
To conclude, our study analyses the spectrum of ARF in ICU of a tertiary care hospital in India and identifies the predictor outcomes in these patients using multivariate analysis. We found that presence of hypotension, sepsis, and use of nephrotoxic drugs are important precipitating factors in these patients. We confirm that such patients continue to have high mortality, and the number of failed organs and low serum albumin are robust prognostic indicators of increased mortality in these patients.
REFERENCES
- Groeneveld AB, Tran DD, Van dr Meulen J, Nauta JJ, Thijs LG. Acute renal failure in the medical intensive care unit: predisposing, complicating factors and outcome. Nephron 1991; 59: 602–610, [PUBMED], [INFOTRIEVE]
- Schaefer JH, Jochimsen F, Keller F, Wegscheider K, Dister A. Outcome predictors of acute renal failure in medical intensive care. Intensive Care Med 1991; 17: 19–24, [PUBMED], [INFOTRIEVE], [CROSSREF]
- Schwilk B, Wiedeck H, Stein B, Reinelt H, Treiber H, Bothner U. Epidemiology of acute renal failure and outcome of hemodiafiltration in intensive care. Intensive Care Med 1997; 23: 1204–1211, [PUBMED], [INFOTRIEVE], [CROSSREF]
- de Mendonca A, Vincent JL, Suter PM, et al. Acute renal failure in the ICU: risk factors and outcome evaluated by the SOFA score. Intensive Care Med 2000; 26: 915–921, [PUBMED], [INFOTRIEVE], [CROSSREF]
- Levy EM, Viscoli CM, Horwitz RI. The effect of acute renal failure on mortality. A cohort analysis. JAMA 1996; 275: 1489–1494, [PUBMED], [INFOTRIEVE], [CROSSREF]
- Brivet FG, Kleinknecht DJ, Loirat P, Landais PJ. Acute renal failure in intensive care units—causes, outcome and prognostic factors of hospital mortality; a prospective, multicenter study. French Study Group on Acute Renal Failure. Crit Care Med 1996; 24: 192–198, [PUBMED], [INFOTRIEVE], [CROSSREF]
- Liano F, Pascual J. Epidemiology of acute renal failure: a prospective multicenter, community based study. Madrid Acute Renal Failure Study Group. Kidney Int 1996; 50: 811–818, [PUBMED], [INFOTRIEVE]
- Neveu H, Kleinknecht D, Brivet F, Loirat P, Landais P. Prognostic factors in acute renal failure due to sepsis. Results of a prospective multicentre study. The French Study Group on Acute Renal Failure. Nephrol Dial Transplant 1996; 11(2)293–299, [PUBMED], [INFOTRIEVE]
- Barretti P, Soares VA. Acute renal failure: clinical outcome and causes of death. Ren Fail 1997; 19: 253–257, [PUBMED], [INFOTRIEVE]
- Mangano CM, Diamondstone LS, Ramsay JG, Aggarwal A, Herskowitz A, Mangano DT. Renal dysfunction after myocardial revascularization: risk factors, adverse outcomes and hospital resource utilization. The Multicenter Study of Perioperative Ischemia Research Group. Ann Intern Med 1998; 128: 198–203
- Lombardi R, Zampedri L, Rodriguez I, Alegre S, Ursu M, Di Fabio M. Prognosis in acute renal failure of septic origin: a multivariate analysis. Ren Fail 1998; 20: 725–732, [PUBMED], [INFOTRIEVE]
- Vivino G, Antonelli M, Moro ML, et al. Risk factors for acute renal failure in trauma patients. Intensive Care Med 1998; 24: 808–814, [PUBMED], [INFOTRIEVE], [CROSSREF]
- Sural S, Sharma RK, Singhal MK, et al. Acute renal failure in an internsive care unit in India—prognostic factors and outcome. J Nephrol 1999; 12: 390–394, [PUBMED], [INFOTRIEVE]
- McCarthy JT. Prognosis of patients with acute renal failure in the intensive care unit: a tale of two eras. Clin Proc 1996; 71: 117–126
- Yuasa S, Takahashi N, Shoji T, et al. A simple and early prognostic index for acute renal failure patients requiring renal replacement therapy. Artif Organs 1998; 22: 273–278, [PUBMED], [INFOTRIEVE], [CROSSREF]
- Clermont G, Acker CG, Angus DC, Sirio CA, Pinsky MR, Johnson JP. Renal failure in the ICU: comparison of the impact of acute renal failure and end stage renal disease on ICU outcomes. Kidney Int 2002; 62: 986–996, [PUBMED], [INFOTRIEVE], [CROSSREF]
- Mehta RL, Pascual MT, Soroko S, et al. Spectrum of acute renal failure in the intensive care unit: the PICARD experience. Kidney Int 2004; 66: 1613–1621, [PUBMED], [INFOTRIEVE], [CROSSREF]
- Bone RC, Balk RA, Cerra FB, et al. Definitions for sepsis and organ failure and guidelines for the use of innovative therapies in sepsis. The ACCP/SCCM Consensus Conference Committee. American College of Chest Physicians/Society of Critical Care Medicine. Chest 1992; 101: 1644–1655, [PUBMED], [INFOTRIEVE]
- Fagon JY, Chastre J, Novara A, Medioni P, Gilbert C. Characterization of intensive care unit patients using a model based on the presence or absence of organ dysfunctions and/or infection. Intensive Care Med 1993; 19: 137–144, [PUBMED], [INFOTRIEVE], [CROSSREF]
- Liano F, Junco E, Pascual J, Madero R, Verde E. The spectrum of acute renal failure in the intensive care unit compared with that seen in other settings. The Madrid Acute Renal Failure Study Group. Kidney Int 1998; 53(suppl 66)S16–S24
- Shusterman N, Storm BL, Murray TG, Morrison G, West SL, Maislin G. Risk factors and outcome of hospital acquired acute renal failure: clinical epidemiologic study. Am J Med 1987; 83: 65–71, [PUBMED], [INFOTRIEVE], [CROSSREF]
- Batista PB, Cendorogolo Neto M, dos Santos OF, Carvalho Bacelar AC, Batista Campos G, dos Santos ES. Evaluation of prognostic indexes in critical acute renal failure patients. Ren Fail 2004; 26: 545–552, [PUBMED], [INFOTRIEVE], [CROSSREF]
- Chen YC, Chen CY, Tien YC, Fang JT, Huang CC. Organ system failures prediction model in intensive care patients with acute renal failure treated with dialysis. Ren Fail 2001; 23: 207–215, [PUBMED], [INFOTRIEVE], [CROSSREF]
- Obialo CI, Okonofua EC, Nzerue MC, Tayade AS, Ritey LJ. Role of hypoalbuminemia and hypocholesterolemia as copredictors of mortality in acute renal failure. Kidney Int 1999; 56: 1058–1063, [PUBMED], [INFOTRIEVE], [CROSSREF]
- Fiaccadori E, Lombardi M, Leonardi S, Rotelli CF, Tortorella G, Borgheti A. Prevalence and clinical outcome associated with preexisting malnutrition in acute renal failure: a prospective cohort study. J Am Soc Nephrol 1999; 10: 581–593, [PUBMED], [INFOTRIEVE]