Abstract
Objectives
Hypermetabolism is associated with clinical prognosis of cancer patients. The aim of this study was to explore the association between basal metabolic rate (BMR) and postoperative clinical outcomes in gastric cancer patients.
Methods
We collected data of 958 gastric cancer patients admitted at our center from June 2014 to December 2018. The optimal cutoff value of BMR (BMR ≤1149 kcal/day) was obtained using the X-tile plot. Logistic and Cox regression analyses were then performed to evaluate the relevant influencing factors of clinical outcomes. Finally, R software was utilized to construct the nomogram.
Results
A total of 213 patients were defined as having a lower basal metabolic rate (LBMR). Univariate and multivariate analyses showed that gastric cancer patients with LBMR were more prone to postoperative complications and had poor long-term overall survival (OS). The established nomogram had good predictive power to assess the risk of OS in gastric cancer patients after radical gastrectomy (c-index was 0.764).
Conclusions
Overall, LBMR on admission is associated with the occurrence of postoperative complications in gastric cancer patients, and this population has a poorer long-term survival. Therefore, there should be more focus on the perioperative management of patients with this risk factor before surgery.
Introduction
Although the incidence of gastric cancer has declined steadily over the past decades, it is still the fifth most common cancer worldwide and the third leading cause of cancer-related mortality.Citation1 The adverse clinical outcomes of gastric cancer patients after radical gastrectomy cannot be ignored by surgeons in the comprehensive diagnosis and treatment of the disease.Citation2,Citation3 Studies have revealed that early identification of patients with poor prognosis after surgery and timely appropriate interventions can improve the prognosis of this population.Citation4,Citation5
It has previously been reported that hypermetabolism is positively correlated with cancer risk.Citation6 Notably, the hypermetabolism state is associated with cachexia and leads to a decline in the long-term survival rate of cancer patients.Citation7 In our previous clinical work, we found that gastric cancer patients who had a lower basal metabolic rate (LBMR) when they were admitted to the hospital were more prone to postoperative complications. In addition, their long-term prognosis was worse compared to patients with higher basal metabolic rate (HBMR) in the follow-up. To date, no study has explored whether there is a correlation between basal metabolic rate (BMR) on admission and surgical outcomes of gastric cancer. Herein, we hypothesized that BMR on admission can be used to assess the health status of a patient and it affects the postoperative clinical outcomes of gastric cancer. The main aim of this study was to evaluate whether BMR correlates with clinical outcomes in patients who had undergone radical gastrectomy.
Patients and Methods
Participants
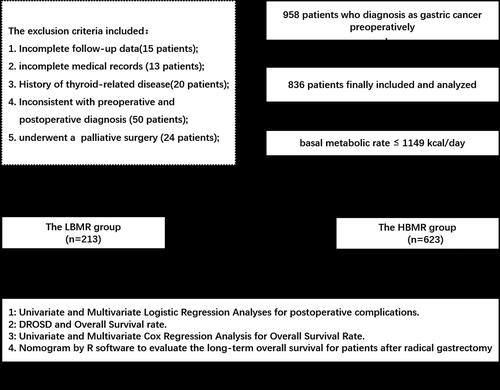
The study included 958 patients who underwent radical gastrectomy at our center from June 2014 to December 2018. The exclusion criteria were as follows:Citation1 Incomplete follow-up data (15 patients),Citation2 incomplete medical records (13 patients),Citation3 history of thyroid-related disease (20 patients),Citation4 inconsistent with preoperative and postoperative diagnosis (50 patients), andCitation5 underwent a palliative surgery (24 patients). Finally, 836 patients were enrolled for further analysis. shows the detailed experimental grouping flow chart. Notably, this retrospective study was approved by the ethics committee and signed informed consent was obtained from all participants prior to the study. The treatment process was conducted in accordance with the Japanese gastric cancer treatment guidelines.Citation8
Data Collection
The following clinical data were extracted from the hospital’s medical database: age; body mass index (BMI); gender; preoperative albumin and hemoglobin concentration; hypertension; diabetes mellitus; Charlson Comorbidity Index (CCI); the American Society of Anesthesiologists grade (ASA grade); Nutritional Risk Screening-2002 score (NRS score); pathological type; tumor location; tumor size; TNM stage; surgical method; total gastrectomy; combined resection; reconstruction methods; time of operation; postoperative complications; hospital stay; hospitalization expense; and long-term overall survival.
Measuring and Defining the BMR
The following Harris–Benedict equation was used to calculate the predicted BMR:Citation9
Males: 666 + (13.7*weight) + (5*height) − (6.8*age);
Females: 655 + (9.6*weight) + (1.8*height) − (4.7*age).
Next, all participants were stratified into two groups based on the cutoff value of BMR (<1149 kcal/day) using the X-tile.
Follow-up
After surgery, all patients were required to visit their doctor and undergo relevant examinations within the first month and every three months thereafter. The follow-up mainly recorded the current general condition of the patients, whether alive, and if dead the time and cause of death. By the end of follow-up, overall survival (OS) was defined as the percentage of patients alive after radical gastrectomy. Postoperative complications within one month were documented and graded according to the Clavien–Dindo (CD) Classification.Citation10 Notably, the last follow-up occurred in September 2020.
Statistical Analysis
The description of the related variables at the table, means, and standard deviations were used for continuous variables that conform to normal distribution, whereas the median and interquartile range were used for non-normal variables. For categorical variables, percentages and numbers were used to summarize the distribution. The Kolmogorov–Smirnov test was performed to calculate the normality of continuous variables. The Student’s t-test, Mann–Whitney U test, and Pearson chi-squared test or Fisher’s exact test were used to compare the data that conform to normal distribution, non-normally distributed data, and categorical data, respectively. Kaplan–Meier survival curves were generated to determine the overall survival, and the difference in survival between subgroups was analyzed by the log-rank test. Multivariate Cox proportional hazards regression analysis was utilized to screen out independent risk factors associated with long-term overall survival.
All analyses were carried out with a two-tailed test and p-value <0.05 was considered statistically significant.
Results
Baseline Characteristics
A total of 213 (25.5%) patients met the criteria for LBMR (). Results showed that the common profile of patients with LBMR included being older, female, having a lower BMI, lower preoperative albumin and hemoglobin level, higher NRS score, undergoing laparoscopy, and a worse tumor stage than those with HBMR (all p < 0.05).
Table 1. Patient demographic and clinical characteristics.
Number and Frequency of Each Type of Complication
A total of 220 (26.2%) patients experienced 322 grade IIa or higher postoperative complications (PCs) events (). Intra-abdominal infection, pulmonary infection, postoperative bleeding, thrombosis, and bowel obstruction were the most frequently observed PCs.
Table 2. Actual number and frequency of each complication (grade ≥ II).
Logistic Regression Analysis of the PCs
Univariate analysis results showed that age, hypoalbuminemia, anemia, Charlson Comorbidity Index, ASA grade, NRS 2002 score, hypertension (p = 0.008), diabetes mellitus, tumor size, tumor location, TNM stages, total gastrectomy, combined resection, laparoscopy-assisted, reconstruction methods, and BMR were closely associated with PCs (all p < 0.05, ). Meanwhile, only age (OR = 1.71, p < 0.01), anemia (OR = 1.67, p < 0.01), CCI, laparoscopy-assisted (OR = 0.59, p = 0.01), and BMR (OR = 1.63, p = 0.01) were independently associated with PCs.
Table 3. Univariate and multivariate analysis associated with postoperative complications.
The Association between BMR and OS
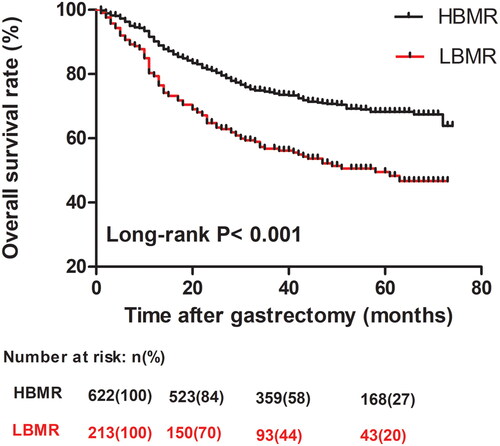
Analysis of the follow-up data of the study population showed that the median follow-up time was 42 (26–60) months. A total of 287 gastric cancer patients had died by the last follow-up. Results revealed that patients with LBMR had higher risk of poorer OS than patients with HBMR (p < 0.01; ). The 1-, 3-, and 5-year overall survival rates were 79.3, 56.8, and 49.5%, respectively, for patients with LBMR, and 90.2, 74.4, and 68.2%, respectively, for patients with HBMR. In addition, the median OS of gastric cancer patients with LBMR was significantly shorter compared to patients with HBMR (35 vs. 60 months), and the difference was statistically significant (p < 0.01; ).
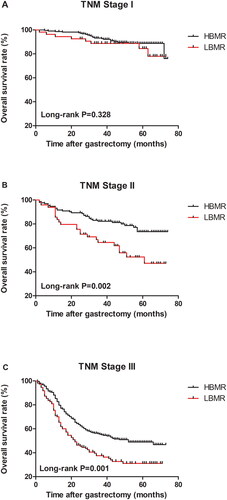
Moreover, this study explored the correlation between BMR levels and long-term prognoses of patients at various TNM stages. shows that the OS of the LBMR group was significantly lower than that of the HBMR group at TNM stages II (p < 0.01; ) and III (p < 0.01; ), but not at TNM stage I (p = 0.33; ).
Univariate and Multivariate Cox Regression Analysis for OS
Univariate analysis showed significant correlations between OS and age (p < 0.001), gender (p = 0.04), BMI (p = 0.04), hypoalbuminemia (p < 0.01), anemia (p < 0.01), NRS 2002 scores (p < 0.01), Charlson Comorbidity Index (p = 0.07), ASA grade (p < 0.01), hypertension (p = 0.03), differentiation of tumor (p < 0.01), tumor location (p < 0.01), tumor size (p < 0.01), TNM stage (p < 0.01), total gastrectomy (p < 0.01), combined resection (p < 0.01), laparoscopy-assisted surgery (p < 0.01), type of reconstruction (p < 0.01), C–D Classification (p < 0.01), and BMR (p < 0.01) (). On the other hand, the multivariate Cox regression analysis () demonstrated that gender (HR = 1.66, p < 0.01), differentiation of tumor, tumor size ≥ 4.75 cm (HR = 1.36, p = 0.03), TNM stage (p < 0.01), total gastric resection (HR = 1.31, p < 0.01), combined resection (HR = 1.45, p = 0.04), C–D complication classification ≥2 (HR = 1.68, p < 0.01), and LBMR (HR = 1.92, p < 0.01) were independent risk factors for lower OS.
Table 4. Univariate and multivariate analysis of factors associated with overall survival.
Establishment and Validation of a Nomogram for Predicting OS
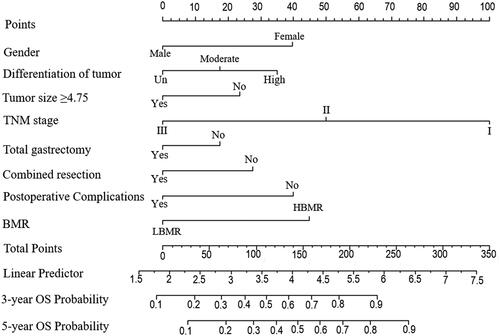
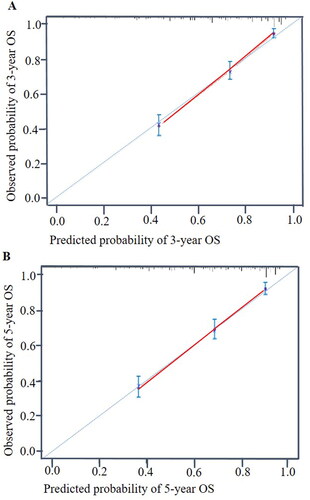
The above independent risk factors associated with long-term OS were subsequently included in the analysis, and R software was then utilized to construct a new nomogram for predicting the 3- and 5-year OS (). Results showed that the nomogram had good predictive power to assess the risk of OS (c-index was 0.764). On this basis, we further verified the validity of the nomogram. As shown in , the subsequent calibration plots also demonstrated good agreement between the predicted OS probability and the actual situation.
Discussion
Previous studies have demonstrated that hypermetabolism is associated with an increased risk of developing certain types of cancer.Citation11,Citation12 However, few studies have explored the correlation between BMR and prognosis for a certain cancer type. In the present study, it was found that BMR levels can be used to predict the clinical outcome of gastric cancer patients. Results showed that gastric cancer patients with LBMR were more prone to postoperative complications (OR = 1.63, p < 0.01), and the OS of this population was significantly lower than that of gastric cancer patients with HBMR (HR = 1.92, p < 0.01).
To the best of our knowledge, this is the first study to examine the association between levels of BMR at admission and postoperative complications and long-term outcomes in gastric cancer. A person’s basic metabolic rate (BMR) provides information about their overall metabolism.Citation13 Although gastric cancer patients are in a state of high metabolism,Citation7 which requires more energy intake, they suffer from loss of appetite, nausea or vomiting, and even difficulty to eat.Citation14 The provision of nutritional support has become an indispensable component of multidisciplinary comprehensive treatment for gastric cancer. During hospitalization, the implementation of reasonable and effective nutritional support exerts a positive impact on enhancing the prognosis and quality of life among patients. Long-term nutritional deficiencies can lead to weight loss, weakness, and ultimately cachexia. Early identification of patients’ nutritional risks and personalized nutritional interventions can contribute to improving their appetite and nutritional status, enhancing treatment tolerance, as well as promoting overall prognosis.Citation15 This is consistent with a previous study which reported that LBMR is associated with sarcopenia or loss of muscle mass.Citation16 We speculate that the level of BMR may reflect the nutritional status of patients on admission, that is, low BMR and worse nutritional status. Malnourished patients are prone to developing immune dysfunction,Citation17 altered inflammatory responses, and delayed or failed wound healing, which leads to postoperative complications.Citation18 Moreover, immune dysfunction due to malnutrition can increase the risk of postoperative tumor metastasis, thereby negatively affecting the long-term prognosis of gastric cancer patients.Citation19 Therefore, we propose that BMR levels be employed as one of the indicators for rapid assessment of patients’ nutritional status upon admission. For gastric cancer patients exhibiting lower basal metabolic rate (LBMR) upon admission, greater attention should be paid to their dietary needs while appropriate nutritional supplements based on the results from nutrition screening to maximize clinical outcomes.
Reasonable, effective, and standardized perioperative management can reduce PCs, shorten hospital stay and save medical expenses, and ultimately achieve the purpose of accelerated recovery.Citation20,Citation21 Compared to other indicators,Citation22,Citation23 BMR is easy to obtain, simple to calculate, and does not increase the economic burden, which is meaningful for the perioperative management of patients. Therefore, we recommend incorporating BMR into one of the routine evaluations, and more attention should be paid to the perioperative management of patients with this risk factor before surgery. Based on this, we included the independent risk factors associated with long-term prognosis into the analysis and then used R software to establish a new nomogram for predicting OS. Results showed that the nomogram had good predictive power (the C-index was 0.756), and subsequent calibration plots also showed good agreement between the predicted survival probability and the actual situation.
Interestingly, the OS of the LBMR group was significantly lower than that of the HBMR group at TNM stages II and III (all p < 0.05), but not at TNM stage I (p > 0.05, ). We speculate that this is associated with the relatively good long-term prognosis of patients in this stage and thus there is a need to further extend the follow-up time. In addition, results indicated that age was not an independent risk factor for long-term prognosis, which may be related to the inclusion of age indicators in BMR, thus, it was excluded as a confounding factor in multivariate analysis.
Furthermore, we found that men and patients that underwent laparotomy or had postoperative complications were at increased risk of poor OS. The association between gender and prognosis of gastric cancer can be attributed to the differences in hormone levels,Citation24 but much of the research focused on intestinal tumors. It is worth noting that laparoscopic surgery is more delicate and less traumatic, and has obvious advantages over open surgery.Citation25,Citation26 This study also suggests that surgeons should pay more attention to the management of patients with PCs.Citation27 Other clinical features, such as differentiation type, tumor size, and combined resection, were found to be closely associated with the prognosis of gastric cancer.Citation28–30
However, this study had some limitations. First, it was a single center retrospective study which limits the reliability of the research conclusions. Therefore, multi-center and prospective studies should be conducted to further verify our results. Second, although the prediction formula used to obtain BMR was convenient and practical, the inability to prospectively obtain the actual metabolic status of patients is still a shortcoming of this study, which needs to be supplemented in subsequent studies.
Conclusions
This study has revealed that LBMR on admission is associated with the occurrence of postoperative complications in patients with gastric cancer, and this population has a poor long-term prognosis. Therefore, we recommend incorporating BMR into one of the routine evaluations, and more attention should be paid to the perioperative management of patients with this risk factor before surgery.
Ethical Approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Author Contributions
Yun-Shi Huang: project development, data acquisition, telephone interview, statistical analysis, manuscript writing/editing; Wei-Sheng Chen: data acquisition, telephone interview, statistical analysis, manuscript writing; Xiu-Ya Zeng and Wen-Tao Cai: project development, data acquisition, statistical analysis, manuscript writing/editing. All authors made final approval of the version to be published and agree that for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved.
Acknowledgements
Thanks to all the authors who contributed to this article. No funding source was involved in the study.
Disclosure Statement
No potential conflict of interest was reported by the author(s).
References
- Sung H, Ferlay J, Siegel RL, et al. Global cancer statistics 2020: Globocan estimates of incidence and mortality worldwide for 36 cancers in 185 countries. CA Cancer J Clin. 2021;71(3):1–10. doi:10.3322/caac.21660.
- Kanda M. Preoperative predictors of postoperative complications after gastric cancer resection. Surg Today. 2020;50(1):3–11. doi:10.1007/s00595-019-01877-8.
- Pan T, Chen X-L, Liu K, et al. Nomogram to predict intensive care following gastrectomy for gastric cancer: a useful clinical tool to guide the decision-making of intensive care unit admission. Front Oncol. 2021;11:641124. doi:10.3389/fonc.2021.641124.
- Rinninella E, Cintoni M, Raoul P, et al. Effects of nutritional interventions on nutritional status in patients with gastric cancer: a systematic review and meta-analysis of randomized controlled trials. Clin Nutr ESPEN. 2020;38:28–42. doi:10.1016/j.clnesp.2020.05.007.
- Kuwada K, Kuroda S, Kikuchi S, et al. Clinical impact of sarcopenia on gastric cancer. Anticancer Res. 2019;39(5):2241–2249. doi:10.21873/anticanres.13340.
- Bosaeus I, Daneryd P, Lundholm K. Dietary intake, resting energy expenditure, weight loss and survival in cancer patients. J Nutr. 2002;132(11 Suppl):3465S–3466S. doi:10.1093/jn/132.11.3465S.
- Vazeille C, Jouinot A, Durand J-P, et al. Relation between hypermetabolism, cachexia, and survival in cancer patients: a prospective study in 390 cancer patients before initiation of anticancer therapy. Am J Clin Nutr. 2017;105(5):1139–1147. doi:10.3945/ajcn.116.140434.
- Japanese Gastric Cancer Association. Japanese gastric cancer treatment guidelines 2014 (ver. 4). Gastric Cancer. 2017;20(1):1–19. doi:10.1007/s10120-016-0622-4.
- Kang HW, Seo SP, Lee HY, et al. A high basal metabolic rate is an independent predictor of stone recurrence in obese patients. Investig Clin Urol. 2021;62(2):195–200. doi:10.4111/icu.20200438.
- Clavien PA, Barkun J, de Oliveira ML, et al. The Clavien-Dindo classification of surgical complications: five-year experience. Ann Surg. 2009;250(2):187–196. doi:10.1097/SLA.0b013e3181b13ca2.
- Kliemann N, Murphy N, Viallon V, et al. Predicted basal metabolic rate and cancer risk in the European prospective investigation into cancer and nutrition. Int J Cancer. 2020;147(3):648–661. doi:10.1002/ijc.32753.
- Ng JCM, Schooling CM. Effect of basal metabolic rate on cancer: a Mendelian randomization study. Front Genet. 2021;12:735541. doi:10.3389/fgene.2021.735541.
- Sabounchi NS, Rahmandad H, Ammerman A. Best-fitting prediction equations for basal metabolic rate: informing obesity interventions in diverse populations. Int J Obes. 2013;37(10):1364–1370. doi:10.1038/ijo.2012.218.
- Stojcev Z, Matysiak K, Duszewski M, Banasiewicz T. The role of dietary nutrition in stomach cancer. Contemp Oncol. 2013;17(4):343–345. doi:10.5114/wo.2013.37213.
- Fearon K, Strasser F, Anker SD, et al. Definition and classification of cancer cachexia: an international consensus. Lancet Oncol. 2011;12(5):489–495. doi:10.1016/s1470-2045(10)70218-7.
- Oh S-K, Son D-H, Kwon Y-J, Lee HS, Lee J-W. Association between basal metabolic rate and handgrip strength in older Koreans. Int J Environ Res Public Health. 2019;16(22):4377. doi:10.3390/ijerph16224377.
- Iliakis D, Kressig RW. The relationship between malnutrition and immune. Ther Umsch. 2014;71(1):55–61. doi:10.1024/0040-5930/a000481.
- Sasahara M, Kanda M, Ito S, et al. The preoperative prognostic nutritional index predicts short-term and long-term outcomes of patients with stage II/III gastric cancer: analysis of a multi-institution dataset. Dig Surg. 2020;37(2):135–144. doi:10.1159/000497454.
- Li J, Xu R, Hu DM, Zhang Y, Gong TP, Wu XL. Prognostic nutritional index predicts outcomes of patients after gastrectomy for cancer: a systematic review and meta-analysis of nonrandomized studies. Nutr Cancer. 2019;71(4):557–568. doi:10.1080/01635581.2019.1577986.
- Yang FZ, Wang H, Wang DS, et al. The effect of perioperative Eras pathway management on short-and long-term outcomes of gastric cancer patients. Zhonghua yi Xue za Zhi. 2020;100(12):922–927. doi:10.3760/cma.j.cn112137-20190711-01325.
- Tian Y, Li Q, Pan Y. Prospective study of the effect of Eras on postoperative recovery and complications in patients with gastric cancer. Cancer Biol Med. 2021;19(8):1274–1281. doi:10.20892/j.issn.2095-3941.2021.0108.
- Xu L-B, Shi M-M, Huang Z-X, et al. Impact of malnutrition diagnosed using global leadership initiative on malnutrition criteria on clinical outcomes of patients with gastric cancer. JPEN J Parenter Enteral Nutr. 2022;46(2):385–394 doi:10.1002/jpen.2127.
- Yang Y, Gao P, Song Y, et al. The prognostic nutritional index is a predictive indicator of prognosis and postoperative complications in gastric cancer: a meta-analysis. Eur J Surg Oncol. 2016;42(8):1176–1182. doi:10.1016/j.ejso.2016.05.029.
- Molife R, Lorigan P, MacNeil S. Gender and survival in malignant tumours. Cancer Treat Rev. 2001;27(4):201–209. doi:10.1053/ctrv.2001.0220.
- Ramos MFKP, Pereira MA, Dias AR, Ribeiro U, JrZilberstein B, Nahas SC. Laparoscopic gastrectomy for early and advanced gastric cancer in a Western Center: A propensity score-matched analysis. Updates Surg. 2021;73(5):1867–1877. doi:10.1007/s13304-021-01097-1.
- Honda M, Kumamaru H, Etoh T, et al. Surgical risk and benefits of laparoscopic surgery for elderly patients with gastric cancer: a multicenter prospective cohort study. Gastric Cancer. 2019;22(4):845–852. doi:10.1007/s10120-018-0898-7.
- Kanda M, Ito S, Mochizuki Y, et al. Multi-institutional analysis of the prognostic significance of postoperative complications after curative resection for gastric cancer. Cancer Med. 2019;8(11):5194–5201. doi:10.1002/cam4.2439.
- Dittmar Y, Rauchfuss F, Dondorf F, Ardelt M, Scheuerlein H, Settmacher U. Extended pathohistological criteria for assessment of the long-term prognosis of gastric cancer. Zentralbl Chir. 2016;141(4):433–441. doi:10.1055/s-0034-1383080.
- Liao F, Guo X, Lu X, Dong W. A validated survival nomogram for early-onset diffuse gastric cancer. Aging. 2020;12(13):13160–13171. doi:10.18632/aging.103406.
- Ozer I, Bostanci EB, Orug T, et al. Surgical outcomes and survival after multiorgan resection for locally advanced gastric cancer. Am J Surg. 2009;198(1):25–30. doi:10.1016/j.amjsurg.2008.06.031.