ABSTRACT
COVID-19 has taken a terrible toll on the nursing home population. Yet, there are five times the number of seniors living in the community who are also extremely vulnerable because they suffer from respiratory illnesses. Using the 2018 wave of the Health and Retirement Study we analyze this group of roughly 7 million seniors living in the community and find that they have multiple risk factors that make them particularly exposed. We also show how current strategies for protecting this population may be exacerbating risks and suggest concrete steps for better protecting this group.
Much has been written about the terrible toll – current and projected – of the COVID-19 pandemic on the older adult population, and in particular, those living in nursing homes. Currently, there are roughly 1.3 million nursing facility residents (Kaiser Family Foundation, Citation2019), most of whom are older adults. This group is at very great risk for contracting the disease and is already paying a heavy price in the pandemic (Mosk et al., Citation2020). For many reasons, mortality rates are highest in homes where one or more residents have become infected. Some have estimated that upwards of 20% of nursing home residents will die from the illness (Syre, Citation2020). Moreover, more than three million older adults are living in close communal contact in independent living, assisted living, and senior housing facilities, thus placing them at high risk as well (Weisman, Citation2020).
The focus on this extremely vulnerable population is certainly warranted. However, even as nursing homes have been identified as a top priority for COVID-19 testing, it is important to note that there are five times the number of elders living in the community who would also be classified as extremely vulnerable, in large part because they currently suffer from respiratory illnesses (Condon & Herschaft, Citation2020). These include diseases such as asthma, Chronic Obstructive Pulmonary Disease (COPD), emphysema, and other conditions. In fact, our analysis of the 2018 wave of the Health and Retirement Study indicates that 12.6% of the roughly 55 million adults age 65 and over, or about 6.9 million elders, suffer from such respiratory ailments (AARP, Citationn.d.; Institute for Social Research, Citation2020). This high prevalence among seniors explains, in part, why COVID-19 is particularly lethal among this age group (Begley, Citation2020). For instance, an estimated 13.4% of patients 80 and older have an infection fatality ratio, compared to 1.25% of those in their 50s, and 0.3% of those in their 40s (Verity et al., Citation2020).
In this perspective we characterize the community-dwelling senior population (including those residing in assisted living and other senior housing outside of nursing home facilities) with respiratory illnesses in terms of the socio-economic and health characteristics that put them at heightened risk in the context of the pandemic. We then briefly summarize how certain current approaches to the pandemic may be exposing them to additional risk and conclude by putting forward concrete actions to be taken to better protect them.
A highly vulnerable sub-population
Part of what makes the population living at home with respiratory illness so vulnerable is that they have multiple additional risk factors in addition to their respiratory problems. Our analysis (), which compares some of the key health and socio-demographic characteristics between groups with and without respiratory illnesses, shows that older adults living in non-institutional settings with respiratory illnesses are more likely to be unmarried and living alone and are 1.3 times more likely to be living below the poverty line.
Figure 1. Individuals age 65 and over with and without respiratory issues by selected socio-demographic characteristics.
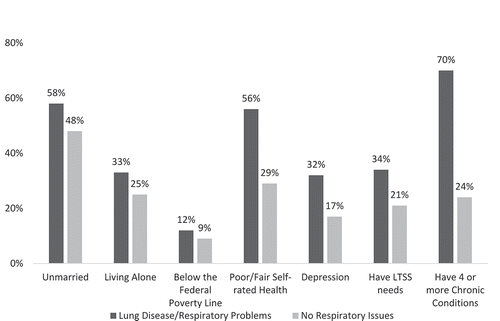
Not surprisingly, older adults with chronic respiratory issues living on their own in the community also suffer from additional health issues that place them at high risk. They are about twice as likely to report that their health is fair or poor, twice as likely to report depression, 1.6 times as likely to need long-term services and supports (LTSS) in their homes, and 2.9 times more likely to have four or more chronic conditions (inclusive of, and often medically related to, their respiratory conditions) than are those without respiratory issues. This pattern of heightened risk is not surprising given that they tend to be somewhat older on average – age 77 versus age 74.
Given the profile of these individuals, the current strategy for dealing with the virus – social distancing – may be exacerbating other problems that already exist: namely, the problem of social isolation (Blumenthal et al., Citation2020). Specifically, 33% of individuals with respiratory illnesses live alone and we know from other research that many do not have Internet connections (Anderson & Perrin, Citation2017). There is a large body of literature documenting the negative health effects of social isolation (Holt-Lunstad et al., Citation2015). These effects have been considered more detrimental to health than smoking 15 cigarettes a day (Tate, Citation2018). Thus, while socially distancing or isolating individuals may be an appropriate short-term strategy to aid our health care system, over the long-term, it will likely lead to additional health-related issues for this population. As well, during the current pandemic non-urgent doctors’ visits and chronic illness checkups are being significantly delayed or canceled. This means that even without contracting COVID-19, this population is facing increased health risks from reduced management of their existing respiratory disease (LTSS Center, Citation2020). Furthermore, for those with LTSS needs – roughly 34% of those with respiratory illnesses or 2.4 million people – there is an added risk: they are being cared for by front line home care workers who lack essential protective equipment amid national shortages, even basics such as hand sanitizers and gloves (Leland, Citation2020).
What can be done?
The coronavirus pandemic poses an elemental challenge to our society: How diligently will we respond to prioritize the safety and care of all groups who are at heightened risk, especially those older adults living at home with respiratory illnesses? We can meet this challenge in several ways, including the provision of additional testing, assessment, social support, and a focus on basic needs, as well as protection of the home care workers who care for them. Clearly, taking the actions we put forward below is not without challenges. There are continued shortages of tests, the front-line work force is already stretched caring for those who currently have symptoms of the illness, and not all care workers have personal protective equipment. Nevertheless, in order to minimize the potential harm for this group, taking these steps, at the earliest time possible, is both a public health and moral imperative.
Increasing testing
It is critically important that we prioritize older adults with known respiratory issues for coronavirus testing, wherever they live. Screening will save lives, as it will be possible to target resources to individuals who may be at the early stages of symptoms and illness onset, thus affording more potential for early intervention treatment options. Some states such as Massachusetts and Florida have targeted communities with higher populations of older adults and other at-risk individuals for random coronavirus testing among even among those who are asymptomatic as a way to track the virus and limit its spread. Screening those with known respiratory issues should fall under this same umbrella of targeted community testing efforts.
Conducting assessments
Healthcare providers such as physicians and hospital staff should proactively assess older adults’ underlying medical and social conditions that pose a higher risk of death, should they contract COVID-19. This means proactively flagging all chronic conditions, particularly known respiratory issues, for all their patients’ providers in order to encourage proper vigilance and early treatment.
Providing social support
Supportive services providers must reach out to this population using telehealth approaches in order to combat isolation and loneliness. A schedule of “check-ins” with isolated older adults is vital to provide social connection and meaningful interactions, either by way of telephone calls or, if the person has access, through video technologies that facilitate face-to-face interactions (e.g., Zoom, Facetime, Facebook Messenger video chat, Skype, etc.).
Meeting basic needs
Essential food and medicine must be delivered to these older adults in their homes so that they avoid potential exposure to the virus by going out, for the duration of time physical distancing needs to be practiced. This may be in the form of expanding already existing Meals on Wheels programs as well as coordinated efforts on the part of senior centers and/or food banks to reconfigure services to provide food delivery.
Protecting home care workers
Amid the national crisis of shortages of personal protective equipment (PPE), frontline workers providing LTSS to older adults in their homes lack essential protective equipment (Leland, Citation2020). These workers, and the people they dedicatedly care for, must be protected by prioritizing allocation of PPE to them (Beckman et al., Citation2020). In addition, this work force needs other protections: financial protections similar to those that were provided to 9/11 emergency responders; the ability to self-isolate and not come to work when sick; regular testing; and compensated respite days.
Conclusion
Even amidst the mounting reports of catastrophic transmission and fatality clusters within institutional settings, we must be proactive in monitoring and caring for the millions of older adults with preexisting respiratory disease living on their own in the community. Further, it is not only the pandemic-related illness that should be of concern to us. This group suffers a variety of health and social challenges that must be tended to even in the midst of this pandemic. There are already reports of individuals not using hospitals and emergency rooms when they should be doing so, due to fears about catching the virus, concerns about over-burdening front-line health workers, or a lack of transportation (Hearst Television, Inc., Citation2020). The multi-prong approach that we are advocating here should help to ameliorate these concerns and mitigate further risk. It is incumbent on us to work together with urgency to keep these vulnerable seniors safe.
Key points
Seniors living in the community with respiratory illnesses are particularly vulnerable to COVID-19.
This population suffers from multiple health and social risks and if exposed to the virus, are likely to face very high mortality rates.
Current approaches for protecting this population are inadequate and may exacerbate the risks faced.
What is needed is a focus on improved testing, better assessment, increased social supports, assurance that basic needs are being met, and protection for home care workers.
Disclosure statement
No potential conflict of interest was reported by the authors.
Additional information
Funding
References
- AARP. (n.d.). Baby boomer facts on 50+ livable communities and aging in place. AARP Livable Communities. Retrieved April 27, 2020, from http://www.aarp.org/livable-communities/info-2014/livable-communities-facts-and-figures.html
- Anderson, M., & Perrin, A. (2017, May 17). Technology use among seniors. Pew Research Center: Internet, Science & Tech. https://www.pewresearch.org/internet/2017/05/17/technology-use-among-seniors/
- Beckman, A. L., Gondi, S., & Forman, H. P. (2020, March 18). How to stand behind frontline health care workers fighting coronavirus. Health Affairs. https://www.healthaffairs.org/do/10.1377/hblog20200316.393860/full/
- Begley, S. (2020, March 30). What explains Covid-19’s lethality for the elderly? STAT Health. https://www.statnews.com/2020/03/30/what-explains-coronavirus-lethality-for-elderly/
- Blumenthal, D., Jacobson, G., & Shah, T. (2020, April 3). The gaps in our social safety net. The Hill. Opinion. https://thehill.com/opinion/healthcare/491007-the-gaps-in-our-social-safety-net
- Condon, B., & Herschaft, R. (2020, April 13). Nursing home deaths soar past 3,600 in alarming surge. The Idaho News. https://idahonews.com/news/coronavirus/nursing-home-deaths-soar-past-3600-in-alarming-surge
- Hearst Television, Inc. (2020, April 23). Gov. Baker urges people who need non-COVID-19 emergency care to seek it [Video]. https://www.wcvb.com/article/gov-charlie-baker-urges-people-who-need-non-covid-19-emergency-care-to-seek-it/32255040
- Holt-Lunstad, J., Smith, T. B., Baker, M., Harris, T., & Stephenson, D. (2015). Loneliness and social isolation as risk factors for mortality: A meta-analytic review. Perspectives on Psychological Science, 10(2), 227–237. https://doi.org/10.1177/1745691614568352
- Institute for Social Research. (2020). Health and retirement study. Health and Retirement Study. https://hrs.isr.umich.edu/
- Kaiser Family Foundation. (2019, June 3). Total number of residents in certified nursing facilities. The Henry J. Kaiser Family Foundation: State Health Facts. https://www.kff.org/other/state-indicator/number-of-nursing-facility-residents/
- Leland, J. (2020, March 22). She had to choose: Her Epileptic patient or her 7-year-old daughter. The New York Times. https://www.nytimes.com/2020/03/22/nyregion/coronavirus-caregivers-nyc.html
- LTSS Center. (2020, March 23). COVID-19 is disrupting services for older adults living in community. The LeadingAge LTSS Center @UMass Boston. https://www.ltsscenter.org/covid-19-is-disrupting-services-for-older-adults-living-in-community/
- Mosk, M., Romero, L., Pecorin, A., & Freger, H. (2020, April 19). Inside nursing homes, coronavirus brings isolation and 7,300 deaths; Outside, families yearn for news. ABC News. https://abcnews.go.com/Health/inside-nursing-homes-coronavirus-brings-isolation-7300-deaths/story?id=70225836
- Syre, S. (2020, April 6). Institute talk: A conversation with Hospice Physician Joanne Lynn about nursing homes dealing with COVID-19. University of Massachusetts Boston: The Gerontology Institute Blog. http://blogs.umb.edu/gerontologyinstitute/2020/04/06/institute-talk-a-conversation-with-hospice-physician-joanne-lynn-about-nursing-homes-dealing-with-covid-19/
- Tate, N. (2018, May 4). Loneliness rivals obesity, smoking as health risk. WebMD. https://www.webmd.com/balance/news/20180504/loneliness-rivals-obesity-smoking-as-health-risk
- Verity, R., Okell, L. C., Dorigatti, I., Winskill, P., Whittaker, C., Imai, N., Cuomo-Dannenburg, G., Thompson, H., Walker, P. G. T., Fu, H., Dighe, A., Griffin, J. T., Baguelin, M., Bhatia, S., Boonyasiri, A., Cori, A., Cucunubá, Z., FitzJohn, R., Gaythorpe, K., Hamlet, A., … Ferguson, N. M. (2020). Estimates of the severity of coronavirus disease 2019: A model-based analysis. The Lancet Infectious Diseases. https://doi.org/10.1016/S1473-3099(20)30243-7
- Weisman, R. (2020, April 26). Assisted-living sites struggle with coronavirus in shadow of nursing home crisis—The Boston Globe. The Boston Globe. https://www.bostonglobe.com/2020/04/26/metro/assisted-living-sites-struggle-with-covid-19-shadow-nursing-home-crisis/
