Images in cardiovascular revascularization medicine
A 72-year-old man presented for evaluation of recurrent exertional angina. There was a preceding history of hypertension and cigarette smoking. Thallium-201 scintigraphy showed inducible ischemia of the anterior wall.
Coronary angiography displayed a severe stenosis of the proximal left anterior descending coronary artery after the first septal branch (LAD; ). A diagonal branch trifurcated into minor vessels with significant lesions. The left circumflex artery was atheromatic with no severe obstruction. Right coronary angiogram revealed an atheromatic, dominant right coronary artery with a 60% stenosis in the posterior descending artery.
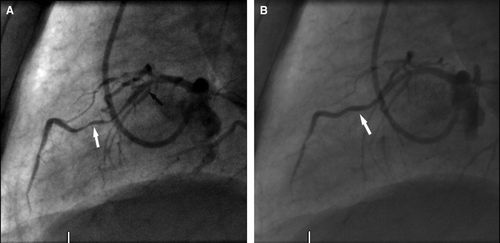
Figure 1. (A) Left coronary angiogram in lateral projection showing a proximal severe stenosis in LAD with TIMI flow score of 2 (white arrow). (B) Right coronary angiogram in left anterior oblique view showing an atheromatic right coronary artery with a significant stenosis in the posterior descending artery.
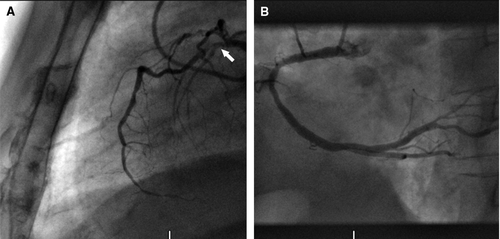
The LAD was successfully dilated and stented with a 2.5×12 mm Taxus stent, which was inflated at high pressure (16 Atm with final stent diameter of 2.85 mm). Immediately after stent implantation and nitroglycerin intracoronary administration, a significant systolic compression consistent with a myocardial bridge became then visible (); this compression had not been apparent before angioplasty was performed. Myocardial bridging of the coronary segment was not seen before intervention, presumably because of the severe fixed proximal stenosis, which limited coronary flow at the distal vessel, masking systolic compression. Improved myocardial contractility post revascularization of the LAD could have resulted in increased intramyocardial pressure which might have unmasked bridging. Intracoronary nitroglycerin administration may also have enhanced systolic compression by altering ventricular loading conditions. During the six-month follow-up period, the patient remained asymptomatic with no evidence of ischemia on exercise testing.