ABSTRACT
Widely circulating anti-vaccine misinformation online has been constituting a large obstacle for the success of COVID-19 vaccination campaigns and for the well-being of people during the pandemic. In this paper we discuss strategies to mitigate negative effects of online anti-vaccine contents on public health and to prevent hesitant individuals from falling prey of the traps set by anti-vaccine disinformation spreaders. Here we discuss the importance of filling information voids and understanding trends and concerns that shape the vaccine debate, and we highlight the relevance of building resilience to vaccine misinformation by strengthening public health and digital literacy.
Introduction
Vaccinations are the greatest achievement for public health in the 20th century, as they allowed for a drastic decrease in mortality due to vaccine-preventable diseases. Despite this, an anti-vaccine sentiment is widespread.Citation1 The recent growth of the anti-vaccine movement has mostly been caused by increasing concerns about the safety of vaccines which find their root in a famous and yet disproven study linking MMR vaccine (for measles, mumps and rubella) to autism.Citation2,Citation3 Then, the invention and rapid growth of social media allowed fake news and misinformation to spread faster than ever.Citation4 This unwittingly provided a platform for anti-vaccine supporters to spread their beliefs, and the ongoing COVID-19 pandemic has been providing a fertile ground for the circulation of myths and conspiracy theories about vaccines.Citation5 As WHO’s Director-General Tedros Adhanom Ghebreyesus recognized last year, we are living through an “infodemic,” as the issue of digital misinformation have become a large obstacle to overcoming the COVID-19 pandemic.Citation6 In this paper we describe different strategies to halt the circulation of vaccine misinformation online, embedded in an ethical framework to ensure these interventions are not abused for other scopes than to curb misinformation, increase access to accurate information and save lives.
Different positions, different strategies
Vaccine hesitancy and vaccine refusal: The landscape of anti-vaccine sentiment online
Vaccine hesitancy has been defined by WHO as “the reluctance or refusal to vaccinate despite the availability of vaccines.”Citation7 Despite this reluctance, hesitant individuals often do not develop a strong or dichotomic position about vaccines, but might oppose vaccines when exposed to misinformation and conspiracy theories.Citation8,Citation9 As of 2021, COVID-19 vaccine acceptance was estimated to be very low in the US (56.9%), France (58.9%) and Italy (53.7%), among others.Citation10 An online survey estimated vaccine hesitancy in Italy to account for 18.1%,Citation11 an exploratory study during 2020 showed an acceptance rate of 65.7% in the US,Citation12 and another study showed a higher vaccine acceptance rate of 71.8% in France.Citation13 Another report, pre-pandemic, reported that vaccine hesitancy among Italian parents accounted for 15.6% of the population, and an additional 0.7% of parents were holding strong anti-vaccine positions.Citation14 Vaccine hesitancy estimates vary depending on the sample, report, and time of the analysis, but considering the aforementioned studies, it is 30% in Western countries; this estimate may work well for different regions of the world, as the phenomenon of vaccine hesitancy is equally concerning in the Middle East, Europe and Central Asia, as well as Western and Central Africa.Citation15 However, as of June 2022, the share of people with a complete or partial initial COVID-19 vaccination protocol has been higher than earlier vaccine hesitancy estimates would suggest, with a 99% vaccination rate in the United Arab Emirates, 84.1% in Italy, 80.7% in France, and 77.8% in the US.Citation16 This indicates that a large fraction of previously hesitant individuals opted for vaccination at some point during the ongoing pandemic, supporting the idea that vaccine hesitancy is a reversible phenomenon.
Also online, where misinformation is generated and spreads, different degrees of anti-vaccine opposition exist, which can be classified in vaccine hesitancy and vaccine refusal/opposition, despite these two categories form a continuum.Citation17 These two categories form what superficially appears to be a cohesive anti-vaccine movement online, which produces and shares vaccine misinformation and more or less engages with anti-vaccine discussions on social media. Vaccine hesitancy is an addressable problem, whereas vaccine opposition is a bigger challenge to counter, although anti-vaccine opposition is less common than vaccine hesitancy, as COVID-19 vaccination rates proved, and as previously estimated.Citation14,Citation16 The core of the anti-vaccine movement online is constituted by active individuals engaged in discussion online who often share misinformation or disinformation (Box 1) about vaccines, including myths and conspiracy theories.
Box 1. Disinformation and misinformation – what’s the difference?
Both misinformation and disinformation consist in the spread of false information. Disinformation implies the perpetrator has intentionally spread false claims, myths or conspiracy theories, for subversive purposes or for monetary interests. Instead, misinformation does not imply the person or institution spreading misinformation has been intentionally and purposefully misleading others. Individuals spreading misinformation believe in the truthfulness of the contents they share, and think sharing such contents will help others.
The anti-vaccine community on Twitter is split in two groups: a small fraction of influencers with many followers and a large group of profiles with a small number of followers. The latter group functions as an echo chamber for the contents generated by the small fraction of influential profiles. This community dynamic helps anti-vaccine messages to spread widely and reinforce anti-vaccine beliefs within the group.Citation18,Citation19 The great majority of people, which are marginally active within the anti-vaccine community, are generally vaccine-hesitant individuals, which believe the truthfulness of contents generated by anti-vaccine influencers, and may further share it with their audiences.
Besides anti-vaccine supporters, also individuals and organizations that support the use of vaccines engage in discussion on social media. Those with many followers can be defined as “vaccine influencers” and are often active communicators online. Despite their important role in counteracting anti-vaccine discourse online and providing valuable information, the pro-vaccine community is less engaged in discussion on Twitter, and profiles within this community are not well connected with each other when compared with profiles belonging to the anti-vaccine community, thus dampening the efficacy of pro-vaccine discourse on social media.Citation18
For each of the above-mentioned contexts (i.e., anti-vaccine influencers/vaccine opposition, vaccine hesitancy, and pro-vaccine influencers) different strategies should be put forward to increase vaccine acceptance and increase vaccination rates.Citation20
Censorship
To deal with anti-vaccine supporters who developed strong positions, one option may be to act on the flow of misinformation and conspiracy theories they produce and share (i.e., censorship). Limiting their potential to influence other people can be achieved through various strategies: 1) banning their profiles on social media if they infringe misinformation policies; 2) shadow banning their profiles to limit their outreach; 3) flagging their posts or tweets for potential misinformation using disclaimers. Some of these steps have been taken by social media to reduce misinformation on their platforms, but these processes are far from being efficient; for instance, Facebook has been collaborating with dozens of independent fact-checking organizations,Citation21 but the decision on banning contents is laborious as it involves real people taking decisions for each reported post.
Influencers
The damaging actions taken by anti-vaccine supporters can be counteracted with pro-vaccine influencers. It is important for information providers, such as WHO, to design strategies that support pro-vaccine influencers and enhance their communication skills. Pro-vaccine influencers, including health organizations, adopt a sterile language when communicating online, whereas anti-vaccine supporters use emotional and people-centered communication – often highlighting individual stories of struggles and sufferance to convey a particular information or take-home message.Citation18,Citation22,Citation23 Health organizations could provide guidance and work with trusted amplifiers, globally and within specific communities of people sharing values, religious beliefs, or hobbies.Citation24 Such organizations could provide guidance on 1) how to communicate more efficiently; for instance, people-centered and emotional messages may be more efficient ways to communicate evidence-based information about vaccinesCitation25 – in fact, these two aspects are not mutually exclusive; 2) how to make the most efficient use of social media, to increase outreach;Citation26 3) create a network of influencers able to help each other against haters and bots.Citation27 Cross-commenting and sharing each other’s contents is needed to spread pro-vaccine messages wider and further. Ultimately, a stronger community of science and vaccine communicators could also help building trust in the guiding principles provided by health organizations and in their activities.
Social listening
These strategies are not sufficient: in fact, blocking misinformation through censorship has been proposed to be very effective in the short-term, but may undermine public trust in the organizations providing public health guidance in the long run, thus creating a favorable environment for the circulation of inaccurate information and conspiracy theories;Citation28 providing accurate information is also not enough. In fact, overarching strategies that do not consider the root causes and the contingent factors that sustain vaccine hesitancy are set to failure.Citation29 Hesitant individuals do not have a pre-defined view about vaccinations, but they may be skeptical or insecure, causing a delay in acceptance or refusal of vaccines.Citation8 First and foremost, it is imperative to understand the nature of their doubts – what concerns they have and why, including whether they are aware of how vaccines work, the side effects, etc.Citation30 Gathering information through a process of social listening helps gathering evidence and understanding of the public which can then be used to fill information voids and provide accurate information through appropriate channels, at the time when such information is needed the most.Citation31 Finally, a longer-term strategy needs to consider the causes of vaccine hesitancy, through a precise dissection of the processes of belief formation and reinforcement,Citation32,Citation33 as well as the understanding of relevant factors (such as education, cultural background, critical thinking skills, etc.) that play a role in determining the success or failure of a disinformation campaign.Citation8–36 This will help to design intervention tools that increase public resilience to misinformation.
Filling information voids to prevent misinformation
Increasing presence online
A few aspects determine the success of failure of information campaigns ().
Figure 1. How to fill information voids to prevent misinformation (scheme). The success of information campaigns can be promoted by (a) increasing presence online; (b) understanding real-time trends and concerns (social listening); (c) reaching out to as many people as possible; (d) designing comprehensible and efficient communication strategies.
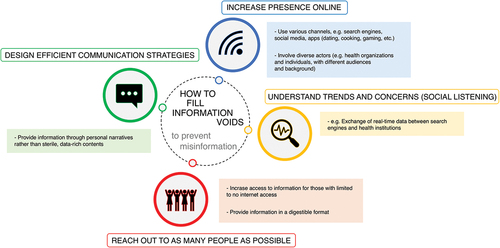
We propose that online presence needs to be increased; various channels of communication online need to be used, including search engines, social media, and other platforms, such as dating, cooking, or gaming apps. Further, we suggest that various actors need to be involved – from WHO to local organizations and influencers. The plurality of actors is important: the more people are involved in creating various type of contents, the more people will be able to access accurate information about vaccines. Similarly, we propose that the more diverse is the pool of active organizations and influencers, in terms of cultural background, political orientation or engagement in local communities, the more people will be reached out by accurate and helpful health messages.
Analyzing online searches
Increasing presence online is necessary but not sufficient to tackle vaccine hesitancy. Besides the number and the origin of the information produced or shared, understanding trends and concerns through real-time analysis of data is crucial. Efforts would be in vain if information cannot answer open questions or cannot clear people’s doubts about vaccines. Partnerships between health organizations and search engines or social media could allow for an exchange of relevant data to determine, almost in real-time, global and local search trends. This would prevent misinformation from filling information voids and would help respond quickly and effectively when misinformation is already circulating (thus correcting it). The 2019 Samoan measles epidemic serves as an example: Following the death of two children in 2018 due to inappropriate inoculation of the MMR vaccine by hospital personnel,Citation37 anti-vaccine misinformation started to spread, and search queries related to vaccines spiked in Samoa in 2019.Citation38 As a consequence and prior to the measles outbreak, vaccination rates in Samoa dropped by 34% in 2018 and 31% in 2019.Citation39 Analyzing search trends and topics discussed online allows health organizations and professionals to understand when, where and what type of information is needed to prevent misinformation or to respond to it quickly and effectively.
Adopting understandable communication strategies
The contents generated need to be comprehensible and should circulate widely. This is particularly challenging as it has been proven that misinformation circulates faster than accurate information does.Citation40 Since reliance on emotions has been shown to promote belief in fake news,Citation41 disinformation is often designed to produce emotional and instinctive reactions, rather than to trigger cognitive responses. We therefore suggest that successful information campaigns learn from disinformation campaigns – by understanding the reasons of their success and implementing communication strategies that allow for the most efficient transmission of information from the provider to the user. Scientific communication is data-driven and based on evidence. Despite this is a fundamental and necessary feature of proper scientific communication – the use of statistics, data, graphs or references in tweets, news features, or Facebook posts is not necessary, and possibly limits outreach,Citation18,Citation42,Citation43 There is a difference between a strategy which focuses on providing evidence for claims, and a strategy that focuses on communicating a desired evidence-based message (providing versus communicating evidence). When institutional trust is not an issue, health organizations and professionals shouldn’t constantly prove they have expertise, but should focus on the message they want to convey. Instead of claiming vaccines are safe and support these assertions with data from clinical trials, the ideal communication strategy could illustrate a happy child after vaccination; or, alternatively, the image of a child suffering from a vaccine-preventable disease with an overlaid text claiming “This is what happens when parents refuse to vaccinate their children.”
A case for risk/benefit communication
Emotional content is very important and should be a primary communication strategy, but data can still be used if their communication is useful and effective, and if their understanding is simple. For example, another way to confront anti-vaccine sentiment is to present a simple and effective risk-benefit analysis, in which the known risks of vaccines are presented alongside the known benefits. Presenting a clear picture of vaccine adverse events would enhance public trust in institutions, would compete with and thus reduce the circulation of misinformed risk-benefit estimates and analyses, and would likely reduce vaccine hesitancy. Communicating risk-benefit analyses should refer to relatable and understandable real-life examples, such as driving a car: for those needing to move in the absence of alternative effective means of transport, the risk/benefit profile of driving a car is heavily in favor of the benefits, even though riding cars is a leading cause of injury and death. Comparing different profiles, such as the risk/benefit profile of driving a car with the risk/benefit profile of vaccines could be powerful and instrumental to explain the value of vaccines without hiding their potential adverse events from the public.
Building resilience to anti-vaccine misinformation
The role of education in building information literacy has been widely discussed, but so far, it can be considered marginal. Several studies hypothesized that literacy in various fields could indirectly provide students with a set of critical thinking skills, which could serve as tools to rationally evaluate information in various contexts. It emerged that proficiency in specific literacies (including scientific literacy, programming, learning to play a music instrument) is not associated with better scores in critical thinking, despite a partial improvement was observed due to overlap of these activities with core skills necessary to develop critical thinking.Citation44,Citation45,Citation46 Enhancing critical thinking could be a viable strategy to fight misinformation, but there is no clear consensus on the definition of critical thinking and no systematic measure of which skills are inherently important to train it, even more so if we consider critical thinking in the context of information literacy. Studies describe critical thinking skills as the ability to a) question the validity of arguments, b) reject conclusions which are not supported by substantiated reasons, c) detect logic pitfalls and assumptions,Citation47 as well as to d) evaluate the credibility of sources, e) understand the concepts of bias, sample size and randomization, f) experimental controls or g) graphical representation of data.Citation48 Despite these efforts, to date no study has tried to quantitatively measure and characterize a minimum set of critical thinking skills necessary to navigate through the multitude of scientific information online, including those related to vaccines. Based on the existing literature and the need to identify long-term, resilience-building anti-misinformation strategies, we suggest identifying, categorizing, and validating a minimum set of skills that underpin critical thinking in the context of scientific and vaccine misinformation. This could allow the design of simple and effective public health strategies and tools that could have a positive impact on reducing the effects of misinformation globally. Local authorities may consider adding critical thinking to science curricula at school starting from a young age, specifically to build scientific and digital literacy.Citation49 Social media, search engines and public health organizations could collaborate to create intervention tools that teach people critical thinking skills while they navigate online. As an example, Facebook could occasionally show users interactive posts while they read posts from their friends and colleagues, asking them or highlighting which element of the post could indicate its lack of accuracy. People could potentially absorb this knowledge and learn while they go about their daily activities online. The success or failure of such interventions would also be easily quantifiable, thus providing useful learning experiences for researchers and experts involved in designing strategies to fight misinformation.
Disinformation is often designed with the objective of producing strong emotional responses, often negative in nature, such as anger or fear. In fact, news contents or images generating strong emotions are more likely to be shared, and those stimulating negative emotions are particularly prone to become viral.Citation50 The tendency to respond to negative stimuli with negative behaviors can be mitigated with mindfulness approaches.Citation51 Training mindfulness has been proposed to help people recognize emotional cues and regulate their own emotional responses,Citation52,Citation53 and people practicing meditation have been suggested to be less susceptible to believe fake news, and it has been shown that they need less time to assess the same information and recognize its credibility.Citation54 Research also shows that meditation techniques focusing on attention activate brain regions associated with information assessment and attentiveness.Citation55 Given these observations, mindfulness has been proposed to be relevant in times of crises and to be instrumental to clear vaccine hesitancy, as it allows for a critical assessment of information.Citation56,Citation57 The practice of mindfulness and the ability to critically assess information are not unrelated; mindfulness has been shown to have a positive impact on training critical thinking skills.Citation58 Mindfulness could therefore provide a state of mind, a predisposition that enables individuals to be more attentive toward information and their own emotional sphere, thus allowing critical thinking skills to assist with information assessment in the least emotionally biased way possible.
Ethical considerations
Dealing with vaccine misinformation raises a first important ethical question: Should we inform the public or should we influence their decisions? Increasing access to information, filling information voids and providing accurate information are not ethically concerning per se. Investigating communication strategies that effectively work is instead problematic, as these can influence emotions and personal engagement with information. However, resilience to misinformation can be built by providing tools to enhance information literacy, rather than by convincing people that vaccines are safe and effective. Critical thinking skills can be seen as tools to assess information, and do not undermine freedom to have personal opinions about any given topic. Rather, critical thinking skills help people build their opinions around available evidence and through logical considerations. The same applies to mindfulness: This approach does not influence nor alter a person’s emotional status, but rather provides tools to self-control emotional responses, allowing critical assessment of information. Control is a key aspect: tools (e.g., critical thinking or mindfulness) allow a person to be in control (internal control); instead, instruments that are meant to deceive and/or influence others are generally designed to control their behaviors (external control).
Vaccine misinformation has been recognized as a threat to global health by WHO.Citation59 Since it can be described as a disease, one relevant question is: should it be cured or should it be prevented? Or both? The ongoing infodemic calls for acute interventions to “cure the disease:” as we have discussed in previous sections, this can be achieved with strategies that censor, or silence, the sources of misinformation and interrupt the flow of information between users. The issue is that censorship may be arbitrary and may have undesired consequences. Tech industry and social media, as private enterprises, operate in their best interests, and their interests may or may not be in line with the public good and the best practices for global and public health. Despite social media have designed their policies to meet WHO guidance, the enforcement of their policies remains subject to personal interpretation and is potentially prone to abuses,Citation60 something that could potentially lead to silencing of political opposition. That said, during crises and especially when the public is not resilient to (or “vaccinated” for) misinformation, it may be necessary to act immediately and effectively through acute interventions – in this case it is important to prevent abuses by allowing actions to be coordinated between individuals, private and public institutions or corporations with independent interests. Specifically, banning vaccine misinformation and profiles of anti-vaccine supporters should be considered with the condition that policies are well-defined and there is no space for personal interpretation. This has practical implications. For example, the tweet “Vaccines kill and are a tool of population control” is incorrect and should be removed. Instead, the tweet “Vaccinations should not be compulsory” does not contain misinformation and should not be removed. Examples of what is allowed and what is not, which thresholds have been defined and why, should constitute the foundations of properly designed social media policies. A second undesired issue with censorship is the consequent decline in public trust;Citation61 for example, when the public is prone to believe conspiracy theories, the removal of conspiratorial tweets or posts from social media may reduce the number of people reached by the message, but likely reinforces and strengthens the anti-establishment, conspiratorial beliefs of those users previously exposed and convinced by the message. In the long term censorship may further exacerbate the problem and, in the context of vaccines, decrease vaccine hesitancy in favor of vaccine refusal and stark opposition.
These ethical issues can be overcome with the design of long-term approaches which aim to build the public’s resilience to misinformation. These approaches help preventing, rather than curing, the “misinformation disease,” and are thus less ethically challenging. Long-term, prevention strategies should be preferred whenever possible.
Disclosure statement
No potential conflict of interest was reported by the author(s).
Additional information
Funding
References
- Haelle T. This is the moment the anti-vaccine movement has been waiting for. The New York Times; 2021. https://www.nytimes.com/2021/08/31/opinion/anti-vaccine-movement.html .
- Chen W, Landau S, Sham P, Fombonne E. No evidence for links between autism, MMR and measles virus. Psychol Med. 2004;34(3):1–6. doi:10.1017/S0033291703001259.
- DeStefano F. Vaccines and autism: evidence does not support a causal association. Clin Pharmacol Ther. 2007;82(6):756–759. doi:10.1038/sj.clpt.6100407.
- Center for Information Technology and Society at UC Santa Barbara. A brief history of fake news. https://www.cits.ucsb.edu/fake-news/brief-history .
- Sturm T, Albrecht T. Constituent covid-19 apocalypses: contagious conspiracism, 5G, and viral vaccinations. Anthropol Med. 2021;28(1):122–139. doi:10.1080/13648470.2020.1833684.
- Tedros AG. For the world health organization. Munich Security Conference; 2020. https://www.who.int/director-general/speeches/detail/munich-security-conference .
- World Health Organization . Ten Threats to global health in 2019. 2022 [accessed 2022 June 3. https://www.who.int/news-room/spotlight/ten-threats-to-global-health-in-2019 .
- MacDonald NE, SAGE Working Group on Vaccine Hesitancy. Vaccine hesitancy: definition, scope and determinants. Vaccine. 2015;33(34):4161–4164. doi:10.1016/j.vaccine.2015.04.036.
- Puri N, Coomes EA, Haghbayan H, Gunaratne K. Social media and vaccine hesitancy: new updates for the era of COVID-19 and globalized infectious diseases. .Hum Vaccin Immunother. 2020;16(11): 2586–2593. doi:10.1080/21645515.2020.1780846.
- Sallam M. COVID-19 vaccine hesitancy worldwide: a concise systematic review of vaccine acceptance rates. Vaccines. 2021;9(2):160. doi:10.3390/vaccines9020160.
- Del Riccio M, Boccalini S, Rigon L, Biamonte MA, Albora G, Giorgetti D, Bonanni P, Bechini A. Factors influencing SARS-CoV-2 vaccine acceptance and hesitancy in a population-based sample in Italy. Vaccines. 2021;9(6):633. doi:10.3390/vaccines9060633.
- de Figueiredo A, Larson HJ. Exploratory study of the global intent to accept COVID-19 vaccinations. Commun Med. 2021;1(1):30. doi:10.1038/s43856-021-00027-x.
- Schwarzinger M, Watson V, Arwidson P, Alla F, Luchini S. COVID-19 vaccine hesitancy in a representative working-age population in France: a survey experiment based on vaccine characteristics. Lancet Public Health. 2021;6(4):e210–e222. doi:10.1016/S2468-2667(21)00012-8.
- Giambi C, Fabiani M, D’Ancona F, Ferrara L, Fiacchini D, Gallo T, Martinelli D, Pascucci MG, Prato R, Filia A, et al. Parental vaccine hesitancy in Italy – results from a national survey. Vaccine. 2018;36(6):779–787. doi:10.1016/j.vaccine.2017.12.074.
- Sallam M, Al-Sanafi M, Sallam M. A global map of COVID-19 vaccine acceptance rates per country: an updated concise narrative review. J Multidiscip Healthc. 2022;15:21–45. doi:10.2147/JMDH.S347669.
- Our World in Data. Share of people vaccinated against COVID-19. 2022 June 2 [accessed 2022 June 3]. https://ourworldindata.org/covid-vaccinations .
- McIntosh EDG, Janda J, Ehrich JHH, Pettoello-Mantovani M, Somekh E. Vaccine hesitancy and refusal. J Pediatr. 2016;175:248–249.E1. doi:10.1016/j.jpeds.2016.06.006.
- Germani F, Biller-Andorno N, Lavorgna L. The anti-vaccination infodemic on social media: a behavioral analysis. PLoS One. 2021;16(3):e0247642. doi:10.1371/journal.pone.0247642.
- Motta M, Callaghan T, Sylvester S, Lunz-Trujillo K. Identifying the prevalence, correlates, and policy consequences of anti-vaccine social identity. Politics Groups Identities. 2021;1–15. doi:10.1080/21565503.2021.1932528.
- Burgess RA, Osborne RH, Yongabi KA, Greenhalgh T, Gurdasani D, Kang G, Falade AG, Odone A, Busse R, Martin-Moreno JM, et al. The COVID-19 vaccine rush: participatory community engagement matters more than ever. The Lancet. 2021;397(10268):8–10. doi:10.1016/S0140-6736(20)32642-8.
- Mosseri AFF. Working to stop misinformation and false news. 2017. https://www.facebook.com/formedia/blog/working-to-stop-misinformation-and-false-news .
- Ball P. Anti-vaccine movement could undermine efforts to end coronavirus pandemic, researchers warn. Nature; 2020. https://www.nature.com/articles/d41586-020-01423-4 .
- Scannell D, Desens L, Guadagno M, Tra Y, Acker E, Sheridan K, Rosner M, Mathieu J, Fulk M. COVID-19 vaccine discourse on twitter: a content analysis of persuasion techniques, sentiment and mis/disinformation. J Health Commun. 2021;26(7):443–459. doi:10.1080/10810730.2021.1955050.
- Steffens MS, Dunn AG, Wiley KE, et al. How organisations promoting vaccination respond to misinformation on social media: a qualitative investigation. 2019.BMC Public Health. 19:1348. doi:10.1186/s12889-019-7659-3.
- Shelby A, Ernst K. Story and science: How providers and parents can utilize storytelling to combat anti-vaccine misinformation. Hum Vaccin Immunother. 2013;9(8):1795–1801. doi:10.4161/hv.24828 .
- World Health Organization. WHO strategic communications framework for effective communications. 2017. https://cdn.who.int/media/docs/default-source/documents/communication-framework.pdf?sfvrsn=93aa6138_0 .
- Lorenz T. To fight vaccine lies, authorities recruit an ‘Influencer Army’. The New York Times; 2021. https://www.nytimes.com/2021/08/01/technology/vaccine-lies-influencer-army.html .
- Spitale G, Germani F, Biller-Andorno N. The PHERCC matrix. An ethical framework for planning, governing, and evaluating risk and crisis communication in the context of public health emergencies. Zenodo (Preprint). 2022.
- The Lancet Child Adolescent Health. Vaccine hesitancy: a generation at risk. Lancet Child Adolesc Health. 2019;3(5):281. doi:10.1016/S2352-4642(19)30092-6.
- Larson HJ. Negotiating vaccine acceptance in an era of reluctance. Hum Vaccin Immunother. 2013;9(8):1779–1781. doi:10.4161/hv.25932.
- World Health Organization. Infodemic. https://www.who.int/health-topics/infodemic#tab=tab_1 .
- Xiao X, Wong RM. Vaccine hesitancy and perceived behavioral control: a meta-analysis. Vaccine. 2020;38(33):5131–5138. doi:10.1016/j.vaccine.2020.04.076.
- Mercer J. Emotional beliefs. International Organization; 2010.
- Bertoncello C, Ferro A, Fonzo M, Zanovello S, Napoletano G, Russo F, Baldo V, Cocchio S. Socioeconomic determinants in vaccine hesitancy and vaccine refusal in Italy. Vaccines. 2020;8(2):276. doi:10.3390/vaccines8020276.
- Guay M, Gosselin V, Petit G, Baron G, Gagneur A. Determinants of vaccine hesitancy in Quebec: a large population-based survey. Hum Vaccin Immunother. 2019:15(11):2527–2533. doi:10.1080/21645515.2019.1603563.
- Xiao X. Follow the heart or the mind? Examining cognitive and affective attitude on HPV vaccination intention. Atl J Commun. 2021;29(2):93–105. doi:10.1080/15456870.2019.1708743 .
- Samoan nurses jailed over deaths of two babies who were given incorrectly mixed vaccines. Pacific Beat; 2019. https://www.abc.net.au/news/2019-08-02/samoa-nurses-sentenced-manslaughter-infant-vaccination-deaths/11378494 .
- Google trends. “Vaccine (topic)” in Samoa. https://trends.google.com/trends/explore?date=today%205-y&geo=WS&q=%2Fm%2F07__7 .
- Hooper V. Misinformation in the 2019 Samoan measles epidemic: the role of the influencer. ECSM 2020 8th European Conference on Social Media; 2020. https://books.google.ch/books?hl=en&lr=&id=FCAEEAAAQBAJ&oi=fnd&pg=PA112&dq=hooper+misinformation+in+the+2019+samoan&ots=UhP5wlnvCf&sig=t6CaTuclYZVvph9KSZ3m9M5SvSM&redir_esc=y#v=onepage&q=hooper%20misinformation%20in%20the%202019%20samoan&f=false .
- Vosoughi S, Roy D, Aral S. The spread of true and false news online. Science. 2018;359(6380):1146–1151. doi:10.1126/science.aap9559.
- Martel C, Pennycook G, Rand DG. Reliance on emotion promotes belief in fake news. Cogn Res. 2020;5:47. doi:10.1186/s41235-020-00252-3.
- Jones D, Anderson Crow D. How can we use the ‘science of stories’ to produce persuasive scientific stories? Palgrave Commun. 2017;3:53. doi:10.1057/s41599-017-0047-7.
- Corless V. The role of narrative in science. Advanced Science News. 2019. https://www.advancedsciencenews.com/the-role-of-narrative-in-science/ .
- Sala G, Gobet F. Do the benefits of chess instruction transfer to academic and cognitive skills? a meta-analysis. Educ Res Rev. 2016;18:46–57. doi:10.1016/j.edurev.2016.02.002.
- Scherer R, Siddiq F, Sánchez Viveros B. The cognitive benefits of learning computer programming: a meta-analysis of transfer effects. J Educ Psychol. 2019;111(5):764–792. doi:10.1037/edu0000314.
- Willingham DT. Ask the cognitive scientist: how can educators teach critical thinking? Am Educ. 2020;44(3):41.
- Vieira RM, Tenreiro-Vieira C, Martins IP. Critical thinking: conceptual clarification and its importance in science education. Sci Educ Int. 2011;22(1):43–54.
- Gormally C, Brickman P, Lutz M. Developing a Test of Scientific Literacy Skills (TOSLS): measuring undergraduates’ evaluation of Scientific information and arguments. CBE—Life Sci Edu. 2017;11(4):364–377.
- Santos LF. 2017. The role of critical thinking in science education. Online Submission 2017;8(20):160–173.
- Sebastiao LV. The effects of mindfulness and meditation on fake news credibility [ dissertation]. 2019. https://www.lume.ufrgs.br/bitstream/handle/10183/197895/001098894.pdf?sequence=1&isAllowed=y .
- Jones K, Libert K, Tynski K. The emotional combinations that make stories go viral. Harvard Business Review; 2016. https://hbr.org/2016/05/research-the-link-between-feeling-in-control-and-viral-content .
- Arch JJ, Craske MG. Mechanisms of mindfulness: emotion regulation following a focused breathing induction. Behav Res Ther. 2006;44(12):1849–1858. doi:10.1016/j.brat.2005.12.007.
- Sivek SC. Both facts and feelings: emotion and news literacy. J Media Lit Educ. 2018;10(2):123–138.
- Teper R, Segal ZV, Inzlicht M. Inside the mindful mind: how mindfulness enhances emotion regulation through improvements in executive control. Curr Dir Psychol Sci. 2013;22(6):449–454. doi:10.1177/0963721413495869.
- Lutz A, Brefczynski-Lewis J, Johnstone T, Davidson RJ. Regulation of the neural circuitry of emotion by compassion meditation: effects of meditative expertise. PLoS One. 2008;3(3):e1897. doi:10.1371/journal.pone.0001897.
- Capulong HGM. Mindfulness as key in easing COVID-19 vaccine hesitancy. J Public Health (Bangkok). 2021;43(2):e338–e339. doi:10.1093/pubmed/fdab050.
- Aguas JJ. Critical thinking in this time of global pandemic. Philos: Int J Phil. 2020;21:285–290.
- Noone C, Bunting B, Hogan MJ. Does mindfulness enhance critical thinking? evidence for the mediating effects of executive functioning in the relationship between mindfulness and critical thinking. Front Psychol. 2016;6. doi:10.3389/fpsyg.2015.02043.
- World Health Organization. Vaccine misinformation: statement by WHO director-general on Facebook and instagram. 2019. https://www.who.int/news/item/04-09-2019-vaccine-misinformation-statement-by-who-director-general-on-facebook-and-instagram .
- Eidelman V, et al. Time and again, social media giants get content moderation wrong: silencing speech about al-aqsa mosque is just the latest example. ACLU; 2021. https://www.aclu.org/news/free-speech/time-and-again-social-media-giants-get-content-moderation-wrong-silencing-speech-about-al-aqsa-mosque-is-just-the-latest-example/ .
- Armitage R. Online ‘anti-vax’ campaigns and COVID-19: censorship is not the solution. Public Health. 2021;190:e29–e30. doi:10.1016/j.puhe.2020.12.005.
