ABSTRACT
We examined perceptions of vaccines and changes during the coronavirus disease 2019 (COVID-19) pandemic. From 2019 to 2021, a national sample of young gay, bisexual, and other men who have sex with men completed an open-ended survey item about vaccine perceptions. Analyses identified themes and polarity (negative, neutral, or positive) within responses and determined temporal changes across phases of the pandemic (“pre-pandemic,” “pandemic,” “initial vaccine availability,” or “widespread vaccine availability”). Themes included health benefits of vaccines (53.9%), fear of shots (23.7%), COVID-19 (10.3%), vaccines being safe (5.6%), and vaccine hesitancy/misinformation (5.5%). Temporal changes existed for multiple themes (p < .05). Overall, 53.0% of responses were positive, 31.2% were negative, and 15.8% were neutral. Compared to the pre-pandemic phase, polarity was less positive for the widespread vaccine availability phase (odds ratio = 0.64, 95% confidence interval: 0.42–0.96). The findings provide insight into how vaccine perceptions change in concert with a public health emergency.
Introduction
Vaccination is one of the greatest public health achievements of the 20th century,Citation1 yet many people in the United States (US) still do not receive their recommended doses.Citation2,Citation3 Several vaccines have been surrounded by controversy (e.g., measles, mumps, and rubella [MMR] vaccineCitation4; human papillomavirus [HPV] vaccine,Citation5,Citation6 which has contributed to a growing vaccine hesitancy movement in the US.Citation7 Indeed, nonmedical exemptions for vaccination have increased meaningfully over the last decade, and there are nearly 500 websites that feature content against vaccination.Citation8,Citation9 This public health concern has likely been exacerbated by the coronavirus disease 2019 (COVID-19) pandemic, as COVID-19 vaccination has been met with a great deal of misinformation, controversy, and opposition.Citation10
Given the evolving vaccine landscape in the US, it is important to continue to examine people’s thoughts and cognitions about vaccination, as these are key correlates of vaccine acceptability and hesitancy.Citation11 We sought to examine perceptions of vaccines among a national sample of young adult gay, bisexual, and other men who have sex with men (YGBMSM) and temporal patterns in these perceptions during the COVID-19 pandemic. YGBMSM often face challenges in accessing and receiving preventive healthcare, so the results will provide key insight into this public health issue.Citation12,Citation13 This information can then help inform future interventions and communication efforts about vaccination.
Methods
Participants
Data were collected as part of a randomized controlled trial of an HPV vaccination intervention for YGBMSM. Details about this trial have been described previously.Citation14 Briefly, we recruited a convenience sample of YGBMSM in the US through advertisements on social media sites, existing research panels, and university-based health organizations. Interested individuals were directed to a mobile-friendly project website to complete an eligibility screener.
Eligibility criteria included: (a) cisgender male; (b) 18–25 years of age; (c) either self-identifying as gay, bisexual, or queer; reporting ever having oral or anal sex with a male; or reporting being sexually attracted to males; (d) living in the US; (e) no doses of HPV vaccine received; and (f) no previous participation in the study. After providing informed consent, participants completed a baseline survey prior to receiving any content about HPV vaccination. Participants received $40 for completing baseline activities. The Institutional Review Board at The Ohio State University approved this study.
Measures
Data for the current analysis are from the baseline survey of participants who enrolled in the study between December 2019 and June 2021 and answered an open-ended question about vaccine perceptions: “What is the first thing you think about when you hear the word ‘vaccine’?” (n = 1,069). Two research team members first independently reviewed a subset of responses to inductively identify initial qualitative codes and met to compare codes and develop a coding scheme. The coders then applied the scheme to all responses for this survey item, after which they compared codes, resolved any discrepancies, made any needed adaptations, and identified themes. For each theme, each participant’s response was categorized as having the theme (given a value of “1”) or not having the theme (given a value of “0”). A response could be categorized as having multiple themes.
We also examined the polarity of responses and its timing in relation to the COVID-19 pandemic. For polarity, we categorized each response as being either negative (contained language not supportive of vaccination), neutral (contained language that was conflicting about or ambiguous toward vaccination), or positive (contained language supportive of vaccination). For timing, we used a participant’s date of enrollment into the study to categorize their response as having occurred during one of four phases of the COVID-19 pandemic.Citation15
The phases represent important pandemic-related events that occurred in the US and included: “pre-pandemic” for participants who enrolled prior to March 11, 2020 (the day the World Health Organization designated COVID-19 a pandemic)Citation16; “pandemic” for those who enrolled between March 11, 2020 and December 13, 2020, during which time period no COVID-19 vaccines were available in the US outside of clinical trials; “initial vaccine availability” for participants who enrolled between December 14, 2020 (the day the COVID-19 vaccine was first given outside of a clinical trial in the US) and April 18, 2021Citation17; and “widespread vaccine availability” for participants who enrolled on or after April 19, 2021 (the first day the vaccine was available to all individuals ages 16 and older in all 50 states and the District of Columbia).Citation18
Data analysis
For quantitative data analysis, we first described participant characteristics, themes, and polarity. We then used logistic regression to assess differences in the prevalence of each theme across the four phases of the COVID-19 pandemic and used ordinal logistic regression to determine temporal changes in polarity of responses. The ordinal logistic regression model dinal logistic regression model met the assumption of proportional odds according to the Brant test.Citation19 Regression models produced odds ratios (ORs) and 95% confidence intervals (CIs). All statistical tests were two-tailed with a critical alpha of 0.05. Data were analyzed with R version 4.2.1 (R Foundation for Statistical Computing, Vienna, Austria) and Stata version 15.0 (Statacorp, College Station, TX).
Results
Most participants were ages 22–25 (64.5%), were single and having sex or casually dating (65.4%), had at least some college education (67.4%), and self-identified as gay (64.8%) (). Just over half of participants indicated a minoritized racial/ethnic identity (54.1%). Overall, 119 (11.1%) participants were recruited during the pre-pandemic phase, 154 (14.4%) during the pandemic phase, 507 (47.4%) during the initial vaccine availability phase, and 289 (27.0%) during the widespread vaccine availability.
Table 1. Demographic and health-related characteristics of participants (n = 1,069).
Themes
shows the nine themes about vaccines that were identified, along with example terms/responses that demonstrate each theme. The most common themes were the health benefits of vaccines (53.9%), fear of shots (23.7%), COVID-19 (10.3%), vaccines being safe (5.6%), and vaccine hesitancy/misinformation (5.5%). The remaining themes were present in less than 5% of responses and included vaccine side effects (4.3%), other (non-COVID-19) diseases (3.7%), vaccine enthusiasm (2.0%), and other barriers to vaccination (i.e., not involving a fear of shots or vaccine side effects) (1.7%).
Table 2. Themes about vaccination across the phases of the COVID-19 pandemic (n = 1,069).
Responses from the widespread vaccine availability phase were less likely to mention the health benefits of vaccines compared to the pre-pandemic phase (46.7% vs. 59.7%; OR = 0.59, 95% CI: 0.38–0.91). Compared to the pandemic phase, responses from the initial vaccine availability phase (13.4% vs. 3.2%; OR = 4.62, 95% CI: 1.83–11.66) and widespread vaccine availability phase (12.8% vs. 3.2%; OR = 4.38, 95% CI: 1.68–11.38) were more likely to mention COVID-19. Pandemic phase served as the referent group for the COVID-19 theme. Compared to the pre-pandemic phase, responses from the initial vaccine availability phase (3.4% vs. 7.6%; OR = 0.42, 95% CI: 0.18–0.98) and widespread vaccine availability phase (2.4% vs. 7.6%; OR = 0.30, 95% CI: 0.11–0.83) were less likely to mention other (non-COVID-19) diseases. There were no other temporal changes in themes (all other p > .05).
Polarity
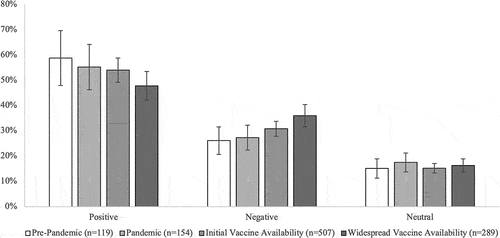
Overall, about half (53.0%) of responses were categorized as positive with fewer being negative or neutral (31.2%, and 15.8%, respectively). Compared to the pre-pandemic phase, responses from the widespread vaccine availability phase were less positive in polarity (OR = 0.64, 95% CI: 0.42–0.96). This reflects that positive polarity decreased from 58.8% during the pre-pandemic phase to 47.8% during the widespread vaccine availability phase, while the negative polarity increased from 26.1% during the pre-pandemic phase to 36.0% during the widespread vaccine availability phase (). The polarity of responses during the pandemic phase and the initial vaccine availability phase did not differ from the pre-pandemic phase (both p > .05).
Discussion
Vaccine hesitancy is an increasing public health concern in the US.Citation8,Citation9 The current study offered a unique opportunity to examine sentiments toward vaccines among a national sample of YGBMSM and identify potential temporal changes in these sentiments. The most prevalent themes identified in this study (health benefits of vaccines, fear of shots, vaccines being safe, vaccine hesitancy/misinformation) are consistent with past research qualitatively examining vaccine perceptions.Citation20,Citation21 However, one notable difference is that these past studies also identified autonomy as a common theme.Citation20,Citation21 This difference could be due to these studies focusing on parents and healthcare providers, whereas our study included only young adults (who may perceive autonomy as a less salient issue).Citation20,Citation21 For polarity, over half of the responses in our study were positive, which also aligns with past research on people’s thoughts about vaccines.Citation22
We also found temporal changes in both themes and polarity. The increase in responses related to COVID-19 over time likely reflects the large increase in media coverage and attention around COVID-19 vaccination that occurred during our study.Citation23,Citation24 The decrease in responses related to the health benefits of vaccines may be attributable to evolving concerns about the efficacy of COVID-19 vaccines that occurred during this time. For example, there may have been concerns about vaccine efficacy against different COVID-19 variants or that two of the original COVID-19 vaccine series were the first messenger ribonucleic acid (mRNA) vaccines to be approved by the Food and Drug Administration.Citation25 Future efforts should explore how people’s perceptions of vaccines may be affected by the emergence of new types of vaccines. Interestingly, we did not find temporal changes in the prevalence of comments related to vaccine misinformation and hesitancy, despite its presence on social media and other avenues.Citation26,Citation27 This suggests that the observed decrease in positive polarity and increase in negative polarity over time was not driven by increases in vaccine misinformation and hesitancy, but rather other vaccine-related concerns (e.g., vaccine efficacy) or potentially recent negative experiences with vaccination (e.g., experiencing an adverse event after COVID-19 vaccination or another vaccination).
Future implications
The results of our study have implications for future vaccine communication efforts for young adults. The identified themes represent topics that are likely salient to young adults concerning vaccination and should therefore be highlighted in future communication efforts for these ages. Further, our results concerning temporal patterns in themes and polarity show how views on vaccines change in concert with a public health emergency. People’s cognitions change during such crises,Citation28 and our results provide novel insight into how vaccine perceptions changed during the COVID-19 pandemic. Such information can help future efforts promoting vaccination anticipate such temporal changes and be prepared to provide timely content.
Limitations
Study limitations include assessing participants’ perceptions about vaccines with a single open-ended survey item, though participants could provide as much information as they wanted to for this item. Data collection for the baseline survey concluded in June 2021, and it is likely that perceptions about vaccines have continued to evolve in response to vaccine-related developments since then (e.g., the availability of additional COVID-19 doses.Citation29 Related, the survey item was only included on a baseline survey, so we were not able to measure within-person changes over time. Participants were a convenience sample of YGBMSM that were participating in an HPV vaccination intervention and who were recruited via online avenues, which may limit the generalizability of our findings. However, participants were from throughout the US, where most young adults use the internet (about 99%)Citation30 and social media (over 80%)Citation31; and past research has shown that vaccine-related attitudes of YGBMSM are similar to those of other young men.Citation32 Lastly, we were not able to examine how temporal changes in our outcomes may have differed by participants’ characteristics due to small sample sizes. Future research is needed to examine such subgroup differences.
Conclusion
We examined perceptions of vaccines among a national sample of YGBMSM in the US. Most participants had positive views about vaccines (i.e., polarity), and we identified several key themes within their responses. Importantly, we also determined that how themes and polarity changed in concert with the COVID-19 pandemic. Results can help guide future interventions and communication efforts about vaccination by informing the content and timeliness of such efforts.
Author’s contributions
Conception and Design: Daniel Marshall, Annie-Laurie McRee, Amy L. Gower, and Paul L. Reiter
Analysis and Interpretation of the Data: Daniel Marshall and Paul Reiter
Manuscript Drafting: Daniel Marshall, Annie-Laurie McRee, Amy L. Gower, and Paul L. Reiter
Critical Revision: Daniel Marshall, Annie-Laurie McRee, Amy L. Gower, and Paul L. Reiter
All authors approve the final version to be published and agree to be accountable for all aspects of the work.
Disclosure statement
No potential conflict of interest was reported by the author(s).
Additional information
Funding
References
- Centers for Disease Control and Prevention. Ten great public health achievements — United States, 2001–2010. Updated 2011 [accessed 2023 Jan 30]. https://www.cdc.gov/mmwr/preview/mmwrhtml/mm6019a5.htm.
- Seither R, Calhoun K, Yusuf OB, Dramann D, Mugerwa-Kasujja A, Knighton CL, Black CL. Vaccination coverage with selected vaccines and exemption rates among children in kindergarten — United States, 2021–22 school year. MMWR Morb Mortal Wkly Rep. 2023;72(2):26–5. doi:10.15585/mmwr.mm7202a2.
- Lu P, Hung M, Srivastav A, Grohskopf LA, Kobayashi M, Harris AM, Dooling KL, Markowitz LE, Rodriguez-Lainz A, Williams WW. Surveillance of vaccination coverage among adult populations —United States, 2018. MMWR Surveill Summ. 2021 [accessed 2023 Feb 1];70(3):1–26. https://pubmed.ncbi.nlm.nih.gov/33983910/.
- Chatterjee A, O Keefe C. Current controversies in the USA regarding vaccine safety. Expert Rev Vaccines. 2010;9(5):497–502. doi:10.1586/erv.10.36.
- Bednarczyk RA. Addressing HPV vaccine myths: practical information for healthcare providers. Hum Vaccin Immunother. 2019;15(7–8):1628–38. doi:10.1080/21645515.2019.1565267.
- Zimet GD, Rosberger Z, Fisher WA, Perez S, Stupiansky NW. Beliefs, behaviors and HPV vaccine: correcting the myths and the misinformation. Prev Med. 2013;57(5):414–8. doi:10.1016/j.ypmed.2013.05.013.
- Larson HJ, Gakidou E, Murray CJL, Longo DL. The vaccine-hesitant moment. N Engl J Med. 2022;387(1):58–65. doi:10.1056/NEJMra2106441.
- Moran MB, Lucas M, Everhart K, Morgan A, Prickett E. What makes anti-vaccine websites persuasive? A content analysis of techniques used by anti-vaccine websites to engender anti-vaccine sentiment. J Commun Healthcare. 2016;9(3):151–63. doi:10.1080/17538068.2016.1235531.
- Olive JK, Hotez PJ, Damania A, Nolan MS. The state of the antivaccine movement in the united states: a focused examination of nonmedical exemptions in states and counties. PLoS Med. 2018;15(6):e1002578. doi:10.1371/journal.pmed.1002578.
- Yasmin F, Najeeb H, Moeed A, Naeem U, Asghar MS, Chughtai NU, Yousaf Z, Seboka BT, Ullah I, Lin C-Y, et al. COVID-19 vaccine hesitancy in the United States: a systematic review. Front Public Health. 2021;9:770985. doi:10.3389/fpubh.2021.770985.
- Dubé E, Laberge C, Guay M, Bramadat P, Roy R, Bettinger JA. Vaccine hesitancy. Hum Vaccin Immunother. 2013;9(8):1763–73. doi:10.4161/hv.24657.
- Halkitis PN, Maiolatesi AJ, Krause KD. The health challenges of emerging adult gay men: effecting change in health care. Pediatr Clin North Am. 2020;67(2):293–308. doi: 10.1016/j.pcl.2019.12.003.
- Knight DA, Jarrett D. Preventive health care for men who have sex with men. Am Fam Physician. 2015 [accessed 2023 May 18];91(12):844–51. https://pubmed.ncbi.nlm.nih.gov/26131944/.
- Reiter PL, Gower AL, Kiss DE, Malone MA, Katz ML, Bauermeister JA, Shoben AB, Paskett ED, McRee A-L. A web-based human papillomavirus vaccination intervention for young gay, bisexual, and other men who have sex with men: protocol for a randomized controlled trial. JMIR Res Protoc. 2020;9(2):e16294. doi:10.2196/16294.
- McRee A, Gower AL, Kiss DE, Reiter PL. Has the COVID-19 pandemic affected general vaccination hesitancy? Findings from a national study. J Behav Med. 2022:1–6. doi:10.1007/s10865-022-00298-2.
- Ghebreyesus TA. WHO director-general’s opening remarks at the media briefing on COVID-19 - Updated 2020 11 March 2020. https://www.who.int/director-general/speeches/detail/who-director-general-s-opening-remarks-at-the-media-briefing-on-covid-19—11-march-2020.
- Guarino B, Cha AE, Wood J, Witte G ‘The weapon that will end the war’: first coronavirus vaccine shots given outside trials in U.S. The Washington Post. 2020 Dec 14 [accessed 2023 Jan 30]. https://www.washingtonpost.com/nation/2020/12/14/first-covid-vaccines-new-york/.
- Schumaker E All US adults now eligible for COVID-19 vaccines. ABC News Web site; Updated 2021 [accessed 2023 Jan 30]. https://abcnews.go.com/Health/adults-now-eligible-covid-19-vaccines/story?id=77163212.
- Brant R. Assessing proportionality in the proportional odds model for ordinal logistic regression. Biometrics. 1990;46(4):1171–8. doi:10.2307/2532457.
- Akande A, Ahmad M, Majid U. A qualitative meta-synthesis on how autonomy promotes vaccine rejection or delay among health care providers. Health Promot Int. 2022;37(1). doi:10.1093/heapro/daab099.
- Majid U, Ahmad M. The factors that promote vaccine hesitancy, rejection, or delay in parents. Qual Health Res. 2020;30(11):1762–76. doi:10.1177/1049732320933863.
- Lyu JC, Han EL, Luli GK. COVID-19 vaccine–related discussion on twitter: topic modeling and sentiment analysis. J Med Internet Res. 2021;23(6):e24435. doi:10.2196/24435.
- Sousa-Pinto B, Anto A, Czarlewski W, Anto JM, Fonseca JA, Bousquet J. Assessment of the impact of media coverage on COVID-19–related google trends data: infodemiology study. J Med Internet Res. 2020;22(8):e19611. doi:10.2196/19611.
- Ming W, Huang F, Chen Q, Liang B, Jiao A, Liu T, Wu H, Akinwunmi B, Li J, Liu G, et al. Understanding health communication through google trends and news coverage for COVID-19: multinational study in eight countries. MIR Public Health Surveill. 2021;7(12):e26644. doi:10.2196/26644.
- National Center for Immunization and Respiratory Diseases (NCIRD). Division of viral diseases. Overview of COVID-19 vaccines. Centers for disease control and prevention web site; Updated 2023 [accessed 2023 Oct 17]. https://www.cdc.gov/coronavirus/2019-ncov/vaccines/different-vaccines/overview-COVID-19-vaccines.html.
- To QG, To KG, Huynh VN, Nguyen NT, Ngo DT, Alley S, Tran AN, Tran AN, Pham NT, Bui TX, et al. Anti-vaccination attitude trends during the COVID-19 pandemic: a machine learning-based analysis of tweets. Digital Health. 2023;9:20552076231158033. doi:10.1177/20552076231158033.
- Romer D, Jamieson KH. Patterns of media use, strength of belief in COVID-19 conspiracy theories, and the prevention of COVID-19 from march to july 2020 in the united states: survey study. J Med Internet Res. 2021;23(4):e25215. doi:10.2196/25215.
- Veil S, Reynolds B, Sellnow TL, Seeger MW. CERC as a theoretical framework for research and practice. Health Promot Pract. 2008;9(4):26S–34S. doi:10.1177/1524839908322113.
- FDA authorizes booster dose of pfizer-BioNTech COVID-19 vaccine for certain populations. FDA Web site; Updated 2021 [accessed 2023 Mar 23]. https://www.fda.gov/news-events/press-announcements/fda-authorizes-booster-dose-pfizer-biontech-covid-19-vaccine-certain-populations.
- Internet/Broadband fact sheet. Pew research center web site. Updated 2021 [accessed 2023 Mar 22]. https://www.pewresearch.org/internet/fact-sheet/internet-broadband/.
- Social media fact sheet. Pew research center web site. Updated 2022 [accessed 2023 Mar 22]. https://www.pewresearch.org/internet/fact-sheet/social-media/.
- Gutierrez B, Leung A, Jones KT, Smith P, Silverman R, Frank I, Leader AE. Acceptability of the human papillomavirus vaccine among urban adolescent males. Am J Mens Health. 2013 [accessed 2023 Oct 17];7(1):27–36. doi:10.1177/1557988312456697.