ABSTRACT
There is evidence that advice from Healthcare Professionals (HCPs) plays an important role in patients’ decision to get vaccinated, but the extent to which patients perceive this impact is unclear. The aim of this study was to assess the perceived impact of a discussion with a HCP on participants’ decision to be vaccinated against COVID-19. A cross-sectional survey was conducted among adults who consulted a general practitioner (GP) or a pharmacist in Ile-de-France, France, after COVID-19 vaccines became available (October-November 2021 period). A total of 344 participants were included, 65.2% of whom reported having had a discussion about COVID-19 vaccines with a HCP. Overall, 55% of participants were advised to be vaccinated by their HCP. Most of the discussions took place with a GP (n = 203, 48.9%). According to 52.5% of participants, the discussion had a positive impact, i.e. it was perceived as encouraging vaccination. The latter reported that, among HCPs, GPs had the greatest number of discussions with a positive impact on the decision to be vaccinated against COVID-19 (93.1%). In the study population, the COVID-19 vaccine hesitancy rate, according to the WHO definition, was high (38.1%), although the COVID-19 vaccine coverage rate was 87.1%. Vaccine hesitant participants were more likely to report a discussion that had a perceived negative impact on their decision to get vaccinated (20.0%) than non-hesitant participants (5.8%, p = .004).
Introduction
Vaccination is a safe and cost-effective way to prevent harmful diseases.Citation1 It has been estimated that in the first year of the COVID-19 vaccination roll-out, 55.9% of the global population received at least one dose of COVID-19 vaccine, and that COVID-19 vaccines prevented up to 14 million deaths worldwide.Citation2 However, some people consider COVID-19 vaccines with suspicion, doubts, reluctance and hesitancy.Citation3–7
Vaccine hesitancy predates COVID-19 vaccines. It is defined as the “delay in acceptance or refusal of vaccination despite availability of vaccination services. Vaccine hesitancy is complex and context specific, varying across time, place and vaccines”.Citation8 Vaccine hesitancy is a complex phenomenon, with many different determinants. A number of psychological determinants and/or factors that exist prior to the vaccination decision and that influence the vaccination decision process have now been identified.Citation9 The “7 Cs” model, which includes Confidence, Complacency, Convenience, benefit-risk Calculation, Collective responsibility, social Conformism and Conspiracy, is the best developed in the light of recent studies.Citation10 The role of healthcare professionals (HCPs) has been identified as a relevant category of determinants of vaccine hesitancy,Citation11 as HCPs can provide their patients with tailored vaccine-related information and recommendations, and have a positive impact on vaccination uptake. It has been shown that the fact that a HCP recommends the vaccine is associated with an increase in vaccination coverage for the HPV,Citation12 influenzaCitation13 and H1N1 vaccines.Citation14 There is emerging evidence of effective ways of influencing the cognitive process of vaccination decisions. For example, awareness that influenza is a serious illness (ruling out complacency) and the desire not to transmit influenza to family members and friends (promoting collective responsibility) seem to facilitate adherence.Citation15 While discussing the risk/benefit ratio of a vaccine can be counter-productive,Citation16 an intervention based on motivational interviewing increases mothers’ intention to vaccinate their child at the age of 2 months.Citation17
In the specific context of COVID-19 vaccines, patients value their HCPs’ opinion of COVID-19 vaccines when making their vaccination decision.Citation18–22 Trust in physicians has been positively associated with COVID-19 vaccine uptake,Citation23 and greater physicians’ communication skills have been associated with a less negative patients’ opinion of the side effects of the COVID-19 vaccines.Citation24
Attitude and beliefs of HCPs toward COVID-19 vaccination have been well studied in FranceCitation25–27 but little is known about their role on their patients’ decision-making regarding COVID-19 vaccination. The rate of vaccine hesitancy is high in France: an estimated 45.8% of the French population showed some form of vaccine hesitancy in 2018,Citation28 and in 2016, France was the country where the perception of vaccine safety in the general population was the lowest in a survey conducted in 67 countries.Citation29 At the start of the COVID-19 vaccination campaign in France in December of 2021, vaccine intention rates were less than 50%,Citation30 and a national study has estimated the final COVID-19 vaccination rate in France to be low, with estimates ranging between 38.4% and 43.6%.Citation3 However, the actual COVID-19 vaccination coverage in France is surprisingly high, with 89.3% of the eligible French population vaccinated by December 2021.Citation31 This high coverage is partly due to the implementation of a mandatory vaccination pass by the French government during the summer of 2021,Citation4 which made access to public places and some professional venues conditional on vaccination. The promotion of COVID-19 vaccines by HCPs may also have helped to reduce vaccine hesitancy and increase vaccination rates in France, given that HCPs have positive opinions on COVID-19 vaccinesCitation25–27 and are considered trustworthy sources of information regarding COVID-19 vaccines.Citation32
The aim of this study was to assess the perceived impact of a discussion with a HCP on participants’ decision to be vaccinated against COVID-19, in the Paris region, in France.
Materials and methods
Study design
A cross-sectional descriptive study was conducted in adults consulting a general practitioner (GP) or a pharmacist in the Ile-de-France region.
Recruitment procedure
Recruitment took place from October 25 to November 22, 2021.
Participants were included from 15 GP practices and 5 community pharmacies. Recruitment sites were all located in the Ile-de-France region, which is an urban densely populated administrative French region including the city of Paris.
The GPs were recruited from a network of GPs used to participating in studies, ensuring a distribution of GPs across various geographic locations in the region. The community pharmacies were recruited based on their locations to diversify the origin of participants within the region.
In each of the 20 sites, inclusions took place within a maximum of 2 days and were stopped once 20 participants had agreed to participate. Each site kept a count of the refusals to participate. Inclusions from GP practices were performed by the GPs themselves. Each GP invited all patients in their consultation list who met the inclusion criteria to participate, consecutively and without selection. Inclusions in pharmacies were performed by a study investigator. All pharmacy customers meeting the inclusion criteria were invited to participate, consecutively and without selection. The number of participants per site was limited to 20 to reduce the site effect in our sample, and a duration of 2 days was considered sufficient to achieve the inclusion objective (all eligible participants were included consecutively without selection).
Inclusion criteria were:
aged 18 and over
able to understand and complete the study form
not subject to any legal protection measure.
Data collection
A survey form was created for this study and was based on preexisting literature.Citation33–35 The structured form consisted of 25 questions (24 closed-end questions and 1 open-ended question).It was tested during its development for comprehension and completion time (estimated at 5–10 minutes). Printed copies of the survey form were provided to participants. Participants completed and returned their form on site.
The following data were collected as part of the surveyCitation1: sociodemographic data,Citation2 COVID-19-related data (history of COVID-19 infection, medical condition associated with an increased risk of COVID-19 severity, need for a mandatory vaccination pass or vaccination certificate in the workplace),Citation3 vaccine-related data (COVID-19 vaccination status, COVID-19 vaccine hesitancy status, main reason for vaccination/non-vaccination, general opinion of vaccines), andCitation4 data on COVID-19 vaccine-related discussions with a HCP (whether the participant had had such a discussion and, if so, what was the HCP’s advice regarding the participant’s COVID-19 vaccination, what was the perceived impact of this discussion on the participant’s decision-making regarding COVID-19 vaccination, what was the type of HCP, and whether the HCP was a relative of the participant). The survey form is presented in the appendix.
To maintain data confidentiality, the form was anonymous, completed in the absence of the recruiting GP/pharmacist and the investigator, and returned by the participants themselves in a sealed return box.
Variables
The COVID-19 vaccine hesitancy status was characterized using the following SAGE WG definition: “delay in acceptance or refusal of vaccination despite availability of vaccination services.” In France, COVID-19 vaccines were available without shortage at the time of the survey. According to French vaccination guidelines, all adults were eligible for vaccination in France at the time of the study, except for those who had developed the COVID-19 within the last 4–6 months. Participants were considered vaccinated with COVID-19 if they had received at least one dose of vaccine. Thus, the participants who were not vaccinated at the time of the survey were considered vaccine hesitant, except for participants who reported a recent COVID-19 infection as the reason for not having been vaccinated. Vaccinees were considered vaccine hesitant if they reported that they had voluntarily delayed vaccination, or that they had not intended to be vaccinated and felt compelled to do so.
The participants’ perceived impact of the discussion regarding their decision to be vaccinated against COVID-19 was assessed using the following question: “What was the impact of this (these) discussion(s) with your HCP(s) on your decision to be vaccinated or not?”. Possible answers were presented on a 4-point Likert scale, ranging from “strong impact in favor of vaccination” to “strong impact against vaccination”. The vaccination recommendation by the HCP was assessed using a 4-point Likert scale ranging from “strongly advised vaccination” to “strongly advised against vaccination”. Discussions with several HCPs could be selected in the form, and the perceived impact and advice provided by the HCP were assessed individually for each discussion. The nature of the relationship between the participant and the HCP was assessed by asking whether the HCP was a relative. Separate questions on the type of HCP, advice, and impact of these specific discussions were asked using the same methodology.
Data analysis
Data were analyzed using R 4.2.1 and Microsoft Excel. Descriptive data analysis is presented as a frequency distribution with numbers and percentages for qualitative data, and as a mean and standard deviation (SD) for quantitative data. The perceived impact of the discussion with a HCP was assessed on a 4-point Likert scale and divided into two categories (“favorable” and “unfavorable”) for analysis. The quantitative analysis was performed using Fisher’s exact test, and the significance threshold was set at a p-value of < 0.05.
Ethics
Participants’ oral informed consent was obtained before inclusion, either by GPs in their practices or by a study investigator in pharmacies. An information letter was given to all participants, as well as to GPs and pharmacists involved in recruitment, to inform them of their right to withdraw consent and to access their personal data. This study was approved by the Collège National des Généralistes Enseignants (CNGE) ethics committee (authorization no. 308 on September 7, 2021).
Results
Participation
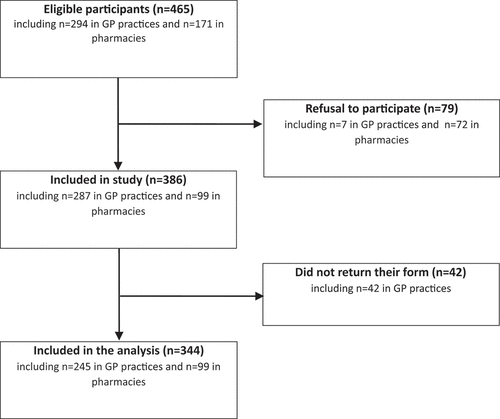
A total of 465 eligible participants were invited to participate in this survey. Among them, 79 refused to participate (72 in a pharmacy and 5 in a GP practice), and 42 agreed to participate but did not return their form. Thus, 344 completed forms were included in the analysis, corresponding to 99 (28.8%) participants recruited in a pharmacy and 245 (71.2%) participants recruited in a GP practice. The overall participation rate was 74.0% (83.3% in GP practices and 57.9% in pharmacies). The participation is presented in .
Participants’ characteristics, COVID-19 vaccine coverage and hesitancy rates
The mean age of the participants was 48.2 ± 19.9 years. Women were overrepresented in the sample (n = 233, 67.7%). The perception of vaccination in general was favorable, with 271 participants (78.8% of the sample) having a positive opinion of vaccines. Participants’ characteristics are detailed in .
Table 1. Characteristics of participants included in the study, COVID-19 and health-related data (N = 344).
The COVID-19 vaccination rate was estimated at 87.1% (n = 296) in the sample for which data were available for analysis, while the COVID-19 vaccine hesitancy rate was estimated at 38.1% (n = 131). Most of the participants who were reluctant to be vaccinated against COVID-19 (n = 93, 71.0%) were vaccinated against COVID-19.
For the 296 vaccinated participants, the types of COVID-19 vaccines administered were as follows:
- mRNA vaccines for 271 (91.6%) participants (Comirnaty Biontech-Pfizer©, Spikevax Moderna©)
- non-replicating viral vector vaccines for 21 (7.1%) participants (Vaxzevria AstraZeneca©, COVID-19 vaccine Janssen©, Spoutnik V©)
- data not available for 4 (1.3%) participants.
Frequency and features of the discussions with HCPs about COVID-19 vaccination
Of the data available (n = 322), 210 participants (65.2%) had had a discussion about COVID-19 vaccines with a HCP. Many participants reported having had several discussions with different HCPs, totaling 415 different discussions. A total of 203 discussions took place with a GP, which was the most frequent situation (48.9% of all discussions). Other HCPs frequently consulted were nurses (n = 59, 14.2%), specialist physicians (n = 49, 11.8%) and pharmacists (n = 43, 10.4%). In most cases, the HCPs who discussed with the participants were not family members (n = 243, 58.6% of discussions).
Recommendation in favor of vaccination by HCPs and perceived impact of the discussion on participants’ decision regarding the COVID-19 vaccine
According to the participants, 91.3% of discussions with a HCP resulted in a recommendation in favor of COVID-19 vaccination (n = 355 discussions). In only 6.4% of discussions (n = 25), HCPs did not recommend vaccination. The perceived impact of the discussion with a HCP on participants’ decision to vaccinate against COVID-19 was assessed as favorable (strongly favorable, somewhat favorable) to vaccination in 84.1% (n = 317) of discussions (). Half of the participants (175 participants, 52.5% of the sample) reported having had a discussion with a HCP that had a positive impact on their decision to be vaccinated against COVID-19. Discussions considered to have a negative impact on participants’ decision to vaccinate against COVID-19 accounted for 6.5% of all discussions (n = 27) and were reported by 6.1% of participants (n = 21). Participants defined as vaccine hesitant more often reported having had a discussion that had an impact against vaccination (n = 14, 20.0% of hesitant-to-vaccinate participants) than non-hesitant participants (n = 7, 5.8%) (p = .004).
Table 2. Description of the perceived impact of the discussion depending on the type of HCPs and their relationship with the participants.
Influence of the type of HCPs and their relationship with the participants on the perceived impact of the discussion
GPs and specialist physicians were the two types of HCPs that most frequently had a positive reported impact on participants’ decision to vaccinate against COVID-19 (respectively 93.1%, n = 176 and 88.9%, n = 40 of discussions assessed). The impact of nurses on vaccination was statistically different from that of GPs (p < .001), as 24.1% (n = 13) of the discussions assessed were perceived to have had a negative impact on COVID-19 vaccination by participants (versus 2.6% of discussions with a GP, n = 5). The relationship between the HCP and the participant had no effect on vaccine recommendation or perceived impact.
Reasons to get vaccinated against COVID-19
Among the participants, the main reasons for getting vaccinated against COVID-19 were “to protect myself against COVID-19” (n = 69, 29.1% of vaccinated participants), “to live a normal life” (n = 45, 19.0%), “to protect others against COVID-19” (n = 36, 15.2%) and “to be able to access public places that require a vaccine pass” (n = 33, 13.9%).
Participants who were both vaccine hesitant and vaccinated against COVID-19 (n = 93) reported different reasons for their vaccination. The reason most frequently reported by hesitant participants was “to be able to access public places that require a vaccine pass” (n = 21, 26.9% of hesitant participants). Medical reasons for getting vaccinated (i.e., to protect themselves or others against COVID-19, or because they usually vaccinate against diseases) were reported by 30.8% (n = 24) of hesitant participant and 63.2% (n = 98) of non-hesitant participants (p < .001).
Discussion
HCPs are trusted sources of information regarding COVID-19 vaccines.Citation32 We observed that most participants (52.5% of the sample) felt that their discussion with their HCP had had a positive impact on their decision to be vaccinated against COVID-19, and that vaccination had very often been recommended by the HCP during this discussion (91.3%). Our results suggest that people value the opinion and advice of their HCP regarding COVID-19 vaccines, and that HCPs have the ability to promote COVID-19 vaccines to their patients. Previous studies have shown that before COVID-19 vaccine became available, people felt that their HCP’s advice would play an important role in their future decision to be vaccinated or not.Citation18–22 Our study confirmed these results with regard to vaccination decision-making after the COVID-19 vaccines became available. Unlike other vaccination campaigns, and in order to maximize the benefits of vaccination, the French COVID-19 vaccination campaign did not focus on primary HCPs in the community. Nevertheless, discussions about vaccination with HCPs were frequent and the participants reported that they had an impact.
These findings add to the results of a large study by Nguyen et al.Citation37 which has shown that the recommendation of COVID-19 vaccines by HCPs had an impact on patients’ perception of the efficacy and safety of COVID-19 vaccines. Nguyen et al. have also found that a recommendation by a HCP had an objective impact on vaccination uptake. These results indicate that patients can be influenced by their discussions with HCPs.
This study also suggests that COVID-19 vaccine hesitancy is common in Ile-de-France, since 38.1% of our sample could be classified as vaccine hesitant according to the SAGE definition of vaccine hesitancy. Vaccine coverage did not seem to have been affected by the high prevalence of vaccine hesitancy since 87.1% of the sample was vaccinated, this vaccination coverage is close to the vaccination coverage of the adult population in Ile-de-France at the time of the study (88.9%).Citation38
The majority (71.0%) of hesitant participants were vaccinated against COVID-19 despite their reluctance. We found that hesitant participants most often reported a non-medical reason for vaccination (i.e., vaccine pass, occupational obligation, travel, etc.). These findings suggest that participants who were hesitant to be vaccinated against COVID-19 were vaccinated for different reasons than non-hesitant. This could help to identify potential motivations for vaccination as part of a patient-centered vaccination decision-making, and could help HCPs to promote COVID-19 vaccination to vaccine hesitant patients by highlighting the non-medical benefits of vaccination. These findings are in line with the conclusions of Ward et al. that COVID-19 vaccine hesitant subjects in France could have been vaccinated against COVID-19 despite their doubts and/or negative feelings about COVID-19 vaccination, and that the enforcement of a national vaccine pass could have had a significant influence on their decision to be vaccinated.Citation4,Citation39
Our study has several limitations. Participants were included from GP practices and pharmacies. Consequently, the prevalence of discussions with a HCP about COVID-19 vaccines, which was 61.0% (n = 210) in this study, is probably overestimated. This recruitment setting could also have biased the characteristics of the participants compared to those of the general population. Indeed, the male/female ratio was unbalanced (67.7% of women), participants were older, and were more likely to report having a disease exposing them to a higher risk of COVID-19 than the general population.Citation40 This recruitment setting was chosen to increase the likelihood that participants would have had a recent discussion with a HCP, and because patients regard GPs and pharmacists as their preferred and most reliable source of health and medical information.Citation41
Recruitment took place only in densely populated and urban areas. This is a limitation because the COVID-19 vaccine coverage and attitudes in rural areas could have been different from those in urban areas at the time of the study.Citation42
Discussions between the participants and their HCPs could have taken place weeks or months before the start of this study. Therefore, the assessment of our primary endpoint could be affected by a memory bias. The data collection period was planned to reduce this bias and data were collected when vaccination rates among French adults had recently reached a plateau.
GPs proved to be a frequent and influential contact for COVID-19. Most participants were recruited from GP practices, and this recruitment setting probably led to an overestimation of the prevalence of discussions with GPs. This setting could also have led to a desirability bias, as participants recruited from GP practices could have overestimated the impact of their GP on their vaccine decision.
This study focused on how participants subjectively perceived the impact of a discussion with a HCP. The perceived impact (positive or negative) was presented regardless of participants’ actual vaccine uptake. Unlike other authors,Citation37 we did not assess whether these discussions had an objective impact on vaccine uptake, as this was not our objective.
Recent changes in the vaccination strategy in France have increased the involvement of pharmacists and nurses in the vaccination process to facilitate access to vaccines.Citation43 Our results suggest that assessing the impact of these specific types of HCPs on vaccination promotion could be an interesting research prospect.
In conclusion, the study participants valued their HCP’s opinion of COVID-19 vaccination. The perceived impact of HCPs was generally favorable to vaccination, with variations ranging from 60.0% to 93.1% depending on the type of HCP with whom participants discussed. GPs and specialist physicians were the two types of HCPs with the greatest impact.
Author contributions
Conceptualization, A.C., A.F. and J.P.; methodology, A.C., A.F. and J.P.; software, A.C.; validation, A.C., A.F., J.P., H.P., M.E. and P.J.; formal analysis, A.C., A.F. and J.P.; investigation, A.C.; data curation, A.C.; writing – original draft preparation, A.C.; writing – review and editing, A.C., A.F., J.P., H.P., M.E. and P.J.; supervision, A.F., J.P., H.P., M.E. and P.J. All authors have read and agreed to the published version of the manuscript.
Institutional review board statement
The study was conducted in accordance with the Declaration of Helsinki, and approved by the Ethics Committee of Collège National des Généralistes Enseignants (CNGE) (authorization no. 308 on September 7, 2021)
Informed consent statement
Informed consent was obtained from all participants who participated in the study.
Appendix 1 Survey form.docx
Download MS Word (55.4 KB)Disclosure statement
No potential conflict of interest was reported by the author(s).
Data availability statement
The data presented in this study are available on request from the corresponding author. The data are not publicly available due to privacy.
Supplementary material
Supplemental data for this article can be accessed on the publisher’s website at https://doi.org/10.1080/21645515.2024.2307735
Additional information
Funding
References
- Ten Great Public Health Achievements—Worldwide, 2001–2010. JAMA. 2011 Aug 3;3065:484–8.
- Watson OJ, Barnsley G, Toor J, Hogan AB, Winskill P, Ghani AC. Global impact of the first year of COVID-19 vaccination: a mathematical modelling study. Lancet Infect Dis. 2022 Jun;22(9):1293–302. 10.1016/S1473-3099(22)00320-6.
- Velardo F, Watson V, Arwidson P, Alla F, Luchini S, Schwarzinger M. et al. 2021 Nov 20. Regional differences in COVID-19 vaccine hesitancy in December 2020: a natural experiment in the French working-age population. Vaccines. 9(11):1364. doi: 10.3390/vaccines9111364.
- Ward JK, Gauna F, Gagneux-Brunon A, Botelho-Nevers E, Cracowski JL, Khouri C, Launay, O, Verger, P, Peretti-Watel, P, et al The French health pass holds lessons for mandatory COVID-19 vaccination. Nat Med. 2022 Feb;28(2):232–5. doi:10.1038/s41591-021-01661-7.
- Ward JK, Alleaume C, Peretti-Watel P, Group COCONEL. The French public’s attitudes to a future COVID-19 vaccine: the politicization of a public health issue. Soc Sci Med 1982. 2020 Nov;265:113414. doi:10.1016/j.socscimed.2020.113414.
- Chaney D, Lee MS. COVID-19 vaccines and anti-consumption: understanding anti-vaxxers hesitancy. Psychol Mark. 2022 Apr;39(4):741–54. doi:10.1002/mar.21617.
- Bajos N, Spire A, Silberzan L. EPICOV study group. The social specificities of hostility toward vaccination against covid-19 in France. PLoS ONE. 2022;17(1):e0262192. doi:10.1371/journal.pone.0262192.
- MacDonald NE. Vaccine hesitancy: Definition, scope and determinants. Vaccine. 2015 Aug;33(34):4161–4. doi:10.1016/j.vaccine.2015.04.036.
- Bussink-Voorend D, Hautvast JLA, Vandeberg L, Visser O, MEJL H. A systematic literature review to clarify the concept of vaccine hesitancy. Nat Hum Behav. 2022 Dec;6(12):1634–48. doi:10.1038/s41562-022-01431-6.
- Geiger M, Rees F, Lilleholt L, Santana AP, Zettler I, Wilhelm O, Betsch C, Böhm R. Measuring the 7Cs of vaccination readiness. Eur J Psychol Assess. 2022 Jul;38(4):261–9. doi:10.1027/1015-5759/a000663.
- Larson HJ, Jarrett C, Eckersberger E, Smith DMD, Paterson P. Understanding vaccine hesitancy around vaccines and vaccination from a global perspective: a systematic review of published literature, 2007–2012. Vaccine. 2014 Apr;32(19):2150–9. doi:10.1016/j.vaccine.2014.01.081.
- Oh NL, Biddell CB, Rhodes BE, Brewer NT. Provider communication and HPV vaccine uptake: a meta-analysis and systematic review. Prev Med. 2021 Jul;148:106554. doi:10.1016/j.ypmed.2021.106554.
- Lu PJ, Srivastav A, Amaya A, Dever JA, Roycroft J, Kurtz MS, O’Halloran A, Williams WW. Association of provider recommendation and offer and influenza vaccination among adults aged ≥18 years – United States. Vaccine. 2018 Feb;36(6):890–8. doi:10.1016/j.vaccine.2017.12.016.
- Zhao AR, Bishai DM. Public health spending, primary care, and perceived risk promoted vaccination against H1N1. Vaccine. 2022 Jan;40(2):325–33.
- European Centre for Disease Prevention and Control. Review of the scientific literature on drivers and barriers of seasonal influenza vaccination coverage in the EU/EEA. [Internet]. LU: Publications Office; 2013 [accessed 2024 Jan 3]. https://data.europa.eu/doi/10.2900/89599.
- Chyderiotis S, Sicsic J, Thilly N, Consortium P, Mueller JE. Vaccine eagerness: a new framework to analyse preferences in single profile discrete choice experiments. Application to HPV vaccination decisions among French adolescents. SSM - Popul Health. 2022 Mar;17:101058. doi:10.1016/j.ssmph.2022.101058.
- Gagneur A, Battista MC, Boucher FD, Tapiero B, Quach C, De Wals P, Lemaitre T, Farrands A, Boulianne N, Sauvageau C. et al. Promoting vaccination in maternity wards ─ motivational interview technique reduces hesitancy and enhances intention to vaccinate, results from a multicentre non-controlled pre- and post-intervention RCT-nested study, Quebec, March 2014 to February 2015. Euro Surveill Bull Eur Sur Mal Transm Eur Commun Dis Bull. 2019 Sep;24(36):1800641. doi:10.2807/1560-7917.ES.2019.24.36.1800641.
- Wang J, Jing R, Lai X, Zhang H, Lyu Y, Knoll MD, Fang H. Acceptance of COVID-19 vaccination during the COVID-19 pandemic in China. Vaccines. 2020 Aug 27;8(3):482. doi:10.3390/vaccines8030482.
- Reiter PL, Pennell ML, Katz ML. Acceptability of a COVID-19 vaccine among adults in the United States: how many people would get vaccinated? Vaccine. 2020 Sep;38(42):6500–7. doi:10.1016/j.vaccine.2020.08.043.
- Wong MCS, Wong ELY, Huang J, Cheung AWL, Law K, Chong MKC, Ng RWY, Lai CKC, Boon SS, Lau JTF. et al. Acceptance of the COVID-19 vaccine based on the health belief model: a population-based survey in Hong Kong. Vaccine. 2021 Feb;39(7):1148–56. doi:10.1016/j.vaccine.2020.12.083.
- King I, Heidler P, Marzo RR. The long and winding road: uptake, acceptability, and potential influencing factors of COVID-19 vaccination in Austria. Vaccines. 2021 Jul 15;9(7):790. doi:10.3390/vaccines9070790.
- Cordina M, Lauri MA, Lauri J. Attitudes towards COVID-19 vaccination, vaccine hesitancy and intention to take the vaccine. Pharm Pract (Granada). 2021 Mar 21;19(1):2317. doi:10.18549/PharmPract.2021.1.2317.
- Viskupič F, Wiltse DL, Meyer BA. Trust in physicians and trust in government predict COVID-19 vaccine uptake. Soc Sci Q. 2022;103(3):509–20. doi:10.1111/ssqu.13147.
- Zheng H, Jiang S, Wu Q. Factors influencing COVID-19 vaccination intention: the roles of vaccine knowledge, vaccine risk perception, and doctor-patient communication. Patient Educ Couns. 2022 Feb;105(2):277–83. doi:10.1016/j.pec.2021.09.023.
- Verger P, Scronias D, Dauby N, Adedzi KA, Gobert C, Bergeat M, Gagneur, A, Dubé, E et al. Attitudes of healthcare workers towards COVID-19 vaccination: a survey in France and French-speaking parts of Belgium and Canada, 2020. Eurosurveillance. Internet. 2021 Jan21; 263: [accessed 2022 Mar 8]. https://www.eurosurveillance.org/content/10.2807/1560-7917.ES.2021.26.3.2002047.
- Janssen C, Maillard A, Bodelet C, Claudel AL, Gaillat J, Delory T. Hesitancy towards COVID-19 vaccination among healthcare workers: a multi-centric survey in France. Vaccines. 2021 May 22;9(6):547. doi:10.3390/vaccines9060547.
- Gagneux-Brunon A, Detoc M, Bruel S, Tardy B, Rozaire O, Frappe P, Botelho-Nevers E. Intention to get vaccinations against COVID-19 in French healthcare workers during the first pandemic wave: a cross-sectional survey. J Hosp Infect. 2021 Feb 1;108:168–73. doi:10.1016/j.jhin.2020.11.020.
- Bocquier A, Fressard L, Cortaredona S, Zaytseva A, Ward J, Gautier A, Peretti-Watel P, Verger P. Social differentiation of vaccine hesitancy among French parents and the mediating role of trust and commitment to health: a nationwide cross-sectional study. Vaccine. 2018 Nov;36(50):7666–73. doi:10.1016/j.vaccine.2018.10.085.
- Larson HJ, de Figueiredo A, Xiahong Z, Schulz WS, Verger P, Johnston IG, Cook AR, Jones NS. The state of vaccine confidence 2016: global insights through a 67-country survey. EBioMedicine. 2016 Oct;12:295–301. doi:10.1016/j.ebiom.2016.08.042.
- Stojanovic J, Boucher VG, Gagne M, Gupta S, Joyal-Desmarais K, Paduano S, Aburub AS, Sheinfeld Gorin SN, Kassianos AP, Ribeiro PAB. et al. 2021 Jun 17. Global trends and correlates of COVID-19 vaccination hesitancy: findings from the iCARE study. Vaccines (Basel). 9(6):661. doi: 10.3390/vaccines9060661.
- SPF. COVID-19 : point épidémiologique du 23 décembre 2021 [Internet]. [accessed 2023 May 19]. https://www.santepubliquefrance.fr/maladies-et-traumatismes/maladies-et-infections-respiratoires/infection-a-coronavirus/documents/bulletin-national/covid-19-point-epidemiologique-du-23-decembre-2021.
- Ipsos European Public Affairs. Flash eurobarometer 494 attitudes on vaccination against COVID-19. 2021.
- Schwarzinger M, Flicoteaux R, Cortarenoda S, Obadia Y, Moatti JP. Low acceptability of A/H1N1 pandemic vaccination in French adult population: did public health policy fuel public dissonance? PLoS One. 2010 Apr 16;5(4):e10199. 10.1371/journal.pone.0010199. Li W, editor.
- Rosenthal SL, Weiss TW, Zimet GD, Ma L, Good MB, Vichnin MD. Predictors of HPV vaccine uptake among women aged 19-26: importance of a physician’s recommendation. Vaccine. 2011 Jan 29;29(5):890–5. doi:10.1016/j.vaccine.2009.12.063.
- CEVIPOF. Baromètre de la confiance politique : Une embellie sanitaire qui n’endigue ni la défiance ni la crise sociale (vague 12 bis) [Internet]. 2021. https://www.sciencespo.fr/cevipof/sites/sciencespo.fr.cevipof/files/Barome%cc%80tre%20Vague%2012%20bis%20-%20VERSION%20FINALE%20(pour%20mise%20sur%20le%20site%20CEVIPOF).pdf.
- Coronavirus SARS-CoV-2 : personnes à risque de formes sévères [Internet]. [accessed 2023 Jun 10]. https://www.hcsp.fr/Explore.cgi/AvisRapportsDomaine?clefr=904.
- Nguyen KH, Yankey D, Jun LP, Kriss JL, Brewer NT, Razzaghi H, Meghani M, Manns BJ, Lee JT, Singleton JA. et al. 2021 Dec 17. Report of health care provider recommendation for COVID-19 vaccination among adults, by recipient COVID-19 vaccination status and attitudes — United States, April–September 2021. MMWR Morb Mortal Wkly Rep. 70(50):1723–30. doi: 10.15585/mmwr.mm7050a1.
- Santé Publique France. Données relatives aux personnes vaccinées contre la Covid-19. 2023 July 13. https://www.data.gouv.fr/fr/datasets/donnees-relatives-aux-personnes-vaccinees-contre-la-covid-19-1/
- PACA ORS. J Ward Enquête SLAVACO Vague 2 : passe sanitaire, obligation vaccinale et rappels. 2021.
- Semenzato L, Botton J, Drouin J, Cuenot F, Weill A, Zureik M. Maladies chroniques, états de santé et risque d’hospitalisation et de décès hospitalier pour COVID-19 : analyse comparative de données des deux vagues épidémiques de 2020 en France à partir d’une cohorte de 67 millions de personnes. EPI-PHARE (CNAM - ANSM); 2021 July 21. https://ansm.sante.fr/uploads/2021/07/23/20210723-rapport-epiphare-covid-19-hospitalisation-deces.pdf.
- Bouder F, Way D, Löfstedt R, Evensen D. Transparency in Europe: a quantitative study: transparency in Europe. Risk Anal. 2015 Jul;35(7):1210–29. doi:10.1111/risa.12386.
- ORS, Firdion L, Féron V, Mangeney C, Saunal A. Vaccination contre la COVID-19 en Île-de-France : évolution dans le temps et l’espace au cours de l’année 2021. [Internet]. 2022. https://www.ors-idf.org/fileadmin/DataStorageKit/ORS/Etudes/2022/Vaccination_Covid/ORS_FOCUS_vaccination_covid.pdf.
- Haute Autorité de Santé (HAS). Élargissement des compétences en matière de vaccination des infirmiers, des pharmaciens et des sages-femmes chez les adolescents de plus de 16 ans et les adultes [Internet]. Saint-Denis La Plaine; 2022. https://www.has-sante.fr/jcms/p_3312462/fr/elargissement-des-competences-en-matiere-de-vaccination-des-infirmiers-des-pharmaciens-et-des-sages-femmes-chez-les-adolescents-de-plus-de-16-ans-et-les-adultes.