Abstract
Background
No study has previously analyzed aggressiveness, homicide, and Lyme disease (LD).
Materials and methods
Retrospective LD chart reviews analyzed aggressiveness, compared 50 homicidal with 50 non-homicidal patients, and analyzed homicides.
Results
Most aggression with LD was impulsive, sometimes provoked by intrusive symptoms, sensory stimulation or frustration and was invariably bizarre and senseless. About 9.6% of LD patients were homicidal with the average diagnosis delay of 9 years. Postinfection findings associated with homicidality that separated from the non-homicidal group within the 95% confidence interval included suicidality, sudden abrupt mood swings, explosive anger, paranoia, anhedonia, hypervigilance, exaggerated startle, disinhibition, nightmares, depersonalization, intrusive aggressive images, dissociative episodes, derealization, intrusive sexual images, marital/family problems, legal problems, substance abuse, depression, panic disorder, memory impairments, neuropathy, cranial nerve symptoms, and decreased libido. Seven LD homicides included predatory aggression, poor impulse control, and psychosis. Some patients have selective hyperacusis to mouth sounds, which I propose may be the result of brain dysfunction causing a disinhibition of a primitive fear of oral predation.
Conclusion
LD and the immune, biochemical, neurotransmitter, and the neural circuit reactions to it can cause impairments associated with violence. Many LD patients have no aggressiveness tendencies or only mild degrees of low frustration tolerance and irritability and pose no danger; however, a lesser number experience explosive anger, a lesser number experience homicidal thoughts and impulses, and much lesser number commit homicides. Since such large numbers are affected by LD, this small percent can be highly significant. Much of the violence associated with LD can be avoided with better prevention, diagnosis, and treatment of LD.
Video abstract
Point your SmartPhone at the code above. If you have a QR code reader the video abstract will appear. Or use:
Plain language summary
This study was performed because a recent study on Lyme disease (LD) and suicide showed 26% of suicidal patients with late stage LD were also homicidal. Violence and homicide rarely have a single cause, instead there are many contributors, deterrents, and acute triggers. Many infections and the immune reactions to them can be associated with violence, including those transmitted by ticks, lice, mosquitos, and so on. The evidence supporting the association between infections and violence is from evolutionary concepts, epidemiology, historical perspectives, case reports, animal studies, brain chemistry, brain immunology, brain circuits, and medical literature review. In this study, inactive charts of Lyme patients were reviewed and analyzed for aggressiveness, homicidality, and homicide. Most aggression in these patients was associated with poor impulse control, sometimes triggered by intrusive images, thoughts and emotions; sound or other stimulation and frustration, and the resulting aggression was invariably bizarre and senseless. In this study of homicidal Lyme patients, it was found that the average patient diagnosis was delayed by 9 years. Lyme infections caused a broad spectrum of clinical findings identified in this study that can collectively be associated with homicidality. A large number of patients with LD have no aggressive tendencies or only mild degrees of low frustration tolerance and irritability, pose no danger to society, and should not be stigmatized. This study can help explain and prevent some previously unexplainable violence and homicide and has broader implications. Understanding the role of Lyme and other infections in causing violence, and prevention, diagnosis, and treatment can help reduce some violence and promote peace.
Introduction
Background
Lyme disease (LD) is the most common tick-borne disease, which is a spirochete, and LD has been compared to syphilis and labeled the New Great Imitator since it may present as many different medical conditions.Citation1,Citation2 The Lyme Borrelia has been found in 15 million-year-old fossilized ticks and in the 5,300-year-old Iceman in the Italian Alps.Citation3,Citation4 LD is transmitted by Ixodes ticks and is the most common tick-borne disease.Citation5 Although Ixodes ticks and Borrelia are present throughout the world, there are regional differences in Borrelia species, tick populations, tick-borne coinfections, and infection rates. In the past 30 years, there has been an expanding awareness of a broad spectrum of neuropsychiatric symptoms that invariably evolve in the later stages of these infections and may include cognitive, emotional, and behavioral symptoms. The diagnosis of LD is often overlooked, and it is increasingly common for psychiatrists to make the initial diagnosis.Citation6–Citation11
LD, or Lyme borreliosis, is a tick-borne infectious disease caused by Borrelia burgdorferi, Borrelia garinii, or Borrelia afzelii while the term Lyme borreliosis/tick-borne diseases recognize that there may also be other tick-borne pathogens and secondary opportunistic infections causing a complex pathophysiological process.
No study has ever before attempted to examine the association between aggressiveness, violence, homicidality, homicide, and LD. A recent article on suicide and Lyme and associated diseases revealed that 68% of LD patients acquired some form of aggressiveness, including 11% who became homicidal after infection, and 26% of the suicidal patients were also homicidal.Citation12 Based upon this finding, a further assessment of aggression and homicidality in LD patients was indicated.
Currently there is a tendency to deal with aggressiveness more through punitive approaches rather than scientific understanding and proactive prevention. Weapon technology is more advanced than our capability to understand and prevent violence, and this limitation is a serious concern when atomic and other weapons of mass destruction may be in the hands of individuals or groups at risk for violent behavior. Therefore, every contributor to violence needs to be better understood and addressed.
Defining aggression and violence
The word aggression may refer to either healthy adaptive emotional effort or more commonly violent maladaptive behavior. Healthy adaptive aggression exists throughout the animal kingdom and is an integral part of human behavior. It includes the pursuit of life, liberty, and happiness and the drives for territoriality, social integration, and reproduction. Social cooperation and respectful competition are an integral part of adaptive aggression and healthy human and societal functioning. A healthy individual in a healthy society values social cooperation and respectful competition over violence as a means of achieving goals.
Anger is an emotion characterized by antagonism toward someone, oneself, or something. Violence can be defined as the use of physical force, power, or threat with the intent to harm or injure another person, oneself, or a group or community, or the destruction of property. Rage is violent, uncontrolled anger. Characteristics of violent acts include self-directed violence (suicidal behavior and self-abuse), interpersonal violence (family – child, partner, elder, or community – acquaintance, and stranger), and collective violence (social, political, and economic). The nature of violent acts can include physical, sexual, psychological, and involving deprivation or neglect.Citation13 Sometimes aggression is used as a synonym for violence. Homicide is the act of one human killing another.
Contributors, deterrents, and triggers of violence
It can rarely be stated that there is only one single cause in any given violent act. Violent behavior is the result of an interaction of multiple contributors, deterrents, acute triggers, and many different sequential events, some of which are both known and unknown ().
Figure 1 The presence or absence of violence is the interactive result of all the multisystem acute and chronic contributors and deterrents to violence.
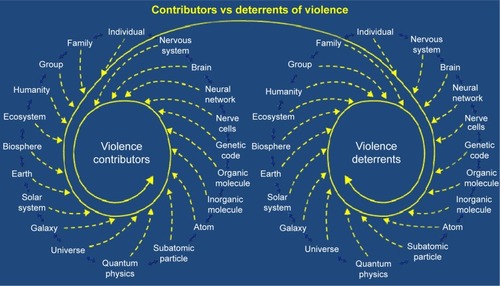
Some of the well-recognized contributors to violence include homelessness, social isolation, being single, living alone, gang membership, low education, unemployment, incarceration, history of violent behavior, fascination with weapons, being a victim of violence, opposing beliefs (religious, political, ethnic, and lifestyle), exposure to violence, exposure to media and computer games with violent themes, younger age, intoxication of potential victim, response of the potential victim, gender, genes (monoamine oxidase A, catechol-O-methyltransferase, serotonin transporter gene, FK506 binding protein s, XYY), threat sensitivity, grudge holding, victim blaming, childhood abuse, child conduct disorder, multiple psychiatric diagnoses (intermittent explosive disorder, narcissistic personality disorder, antisocial personality disorder, psychopathy, bipolar illness, depression, social communication disorder, and other conditions), longer duration of untreated psychosis, cognitive dysfunction, treatment non-adherence, substance abuse, cannabis use, intoxication, head injuries, toxicity, endocrine disorders, limbic encephalitis, Wilson’s disease, brain infections, brain tumors, neurological impairments, and sensory and motor impairments.Citation14–Citation18 One hundred percent of death row inmates had both neurological impairments and a history of abuse.Citation19–Citation21
Deterrents to violence include empathy, frustration tolerance, cognitive abilities, restraint capabilities, higher education, coping skills, supportive relationships, community and other social connections, ethical and religious beliefs, access to social services and psychiatric and medical care, and social structure.Citation22
Triggering events can include acute stress, apperception of threat, jealousy, obsession, psychotic delusions, post-traumatic flashbacks, hopelessness, competition, exposure to violence, traumatic brain injury, unintentional injury, being suicidal, self-harm, impairment from substance use, intoxication, and losing a parent.Citation23,Citation24
While acknowledging the significance of all of these other components to violence, the scope of this article shall specifically focus upon violence and LD.
Epidemiology of violence and infections
Globally, ~1.6 million people die each year because of violence.Citation13,Citation25 Currently violence is not equally distributed throughout the world.Citation26 Peace correlates strongly with education, health, and economic opportunity, and health correlates with a lower prevalence of infectious disease.Citation27 Cognitive impairments contribute to violence, and higher cognitive functioning is a deterrent to violence. There is a strong correlation between national intelligence quotient and lower parasite stress. As countries overcome infectious diseases, the intelligence of their citizens increases; this helps explain the Flynn Effect.Citation28 One study sampled 20 European nations and demonstrated that the prevalence of the brain parasite Toxoplasma gondii was positively associated with national homicide rates.Citation29,Citation30
Violence and infections: historical perspective
Violence is a significant part of history. Death due to violence was much more common in prehistoric societies, in which it was estimated that 10% died because of homicide. Throughout history, violence has decreased as civilization has advanced with increases in literacy, education, democratic governments, and health.Citation31 Different parts of the world at different times in history had different rates of violence in individuals and groups. Poor hygiene correlates with a higher rate of infectious diseases, which in turn correlates with a greater prevalence of violence. The greater prevalence of violence in a critical mass of individuals and influential individuals may contribute to collective violence and wars at different times in history.Citation32
Influential leaders considered to have mental symptoms from syphilis impacting their behavior include Joseph Stalin, Adolf Hitler, Ivan the Terrible, Idi Amin Dada, Benito Mussolini, Henry VIII, Al Capone, Napoleon Bonaparte, Vladimir Lenin, Pope Alexander VI, Charles VIII of France, Peter the Great, and Catherine the Great.Citation33–Citation36
Types of violence
Two basic types of violence are individual violence and collective or group violence. Individual violence involves one person directing violence against others. Collective or group violence is acts committed by normal people and includes situational collective violence which is unplanned and spontaneous, organized collective violence that is unofficial and lacking government approval, and institutional collective violence which is directed by legally constituted officials.
Individual violence can be categorized into three major types – impulsive (or affective), psychotic, and predatory (or psychopathic). Some individual violent acts may be a combination of more than one of these categories. Impulsive violence, also called disorders of impulse control or affective violence is reactive, emotional, rapid and unplanned in response to a real or perceived perception of threat with intense autonomic arousal without regard for long-term consequences. Psychotic violence is motivated by a persecution belief, and there may be an attack against imagined enemies. Paranoia, paranoid schizophrenia, and drug-induced paranoid states are included in this category. Predatory violence is planned, purposeful, and emotionless without autonomic arousal. Impaired functioning contributes to violence in all the three categories, which include impairments of cognition, threat perception, autonomic arousal, impulse control, empathy, and reality testing.Citation14,Citation37
The characteristics of violent acts include self-directed violence and interpersonal violence. Self-directed violence can include suicidal behavior and self-abuse. Interpersonal violence can include family and intimate partner violence (child, partner, and elder), community violence (acquaintance and stranger), and collective violence (social, political, and economic). The nature of violent acts includes physical, sexual, psychological, and/or involving deprivation or neglect.Citation13,Citation38
Impaired and violent individuals or groups of impaired and violent individuals may also contribute to causing collective violence on others who are normal healthy individuals if these impaired individuals are in positions of leadership or influence upon other normal healthy individuals. Leaders or influential individuals prone to predatory violence are particularly dangerous which may result in genocide.Citation32
Neural circuitry of violence
Although a detailed review of all the known neural circuits and transmitters involved in violence is beyond the scope of this article, some general concepts deserve attention. In a state of health, higher level cortical and limbic functioning has sufficient control over more primitive limbic and hypothalamic functioning. Higher level brain functioning integrates many feedforward and feedback pathways that are both stimulatory and inhibitory. Injury to a higher center can result in a dysfunction or a loss of a function leading to a decline in adaptive abilities. Injury to an inhibiting pathway will cause a decline or an inability to inhibit that function. In individuals prone to violence, higher level neural circuits associated with civilized behavior have insufficient control over more primitive mammalian and reptilian neural circuits.Citation39
The right ventromedial prefrontal cortex integrates cognition and affect which contributes to mediating the empathic response.Citation40 The orbital frontal cortex contributes to constraining impulsive outbursts, while the anterior cingulate cortex recruits other brain regions in the response to conflict. Parts of the amygdala are involved in the production of a fear response and other negative emotions. Other parts of the amygdala recognize fear, social emotions, and multiple other emotions in facial expressions as demonstrated by impaired recognition of emotions of social significance following amygdala damage.Citation41,Citation42
In impulsive violence, cortical functioning generally has insufficient control over lower level functioning. This failure of the prefrontal cortex to modulate aggressive acts triggered by anger-provoking stimuli combined with a hyper-responsive amygdala and other limbic regions that are part of affective reactivity contributes to impulsive violence.Citation43 Brain activity in the orbital and anterior regions (impulse control) were blunted or entirely absent in many violent offenders, while the amygdala (fear) showed normal or heightened activity. The inability of the two brain regions to effectively balance the response of the amygdala may help explain how threatening situations can become explosive in some people.Citation44 Brain imaging in murderers supports this model and demonstrates reduced activity in the prefrontal cortex as well as the superior parietal cortex, left angular gyrus, and corpus callosum.Citation45
In psychotic aggression, there is also a hypoactive prefrontal cortex but in contrast to impulsive violence there is invariably normal limbic drive and striatal hyperactivity.Citation14,Citation46 In predatory aggression, there is also a hypoactive prefrontal cortex, but instead a hypoactive limbic system and amygdala.Citation14,Citation46
Particularly violence is correlated with intrusive symptoms, which is relevant to impulsive, predatory, and psychotic aggression. The neural circuit relevant to these symptoms are associated with the activation of basolateral amygdala and ventral hippocampus.Citation47–Citation50 Activation of this circuit also seems to be associated with chronic inflammation with elevated inflammatory markers (tumor necrosis factor-alpha, interleuken-6, interleukin-1β, and C-reactive protein).Citation51–Citation53 LD is associated with chronic inflammation and activation of this circuit.Citation54
Neurochemistry of violence
The neurotransmitters serotonin, dopamine, norepinephrine, acetylcholine, glutamate, and gamma-aminobutyric acid are thought to be involved in violent behavior.Citation14 Particularly serotonin is significant.Citation55–Citation57 Impulsively violent individuals have decreased serotonin activity as demonstrated by significantly lower concentrations of the major metabolite of serotonin, 5-hydroxyindoleacetic acid, in their cerebrospinal fluid.Citation58 Serotonin serves an important inhibitory function in the amygdala, anterior cingulate cortex, dorsolateral prefrontal cortex, and orbitofrontal cortex.Citation59
Inflammatory markers are elevated in individuals with intermittent explosive disorder. Elevations of both plasma C-reactive protein and interleukin-6 levels were significantly elevated in individuals with intermittent explosive disorder compared with psychiatric or normal controls. In addition, these inflammatory markers were directly correlated with a composite measure of aggression and with measures reflecting history of actual aggressive behavior in all individuals.Citation60
Persistence of inflammation is associated with persistent elevations of proinflammatory cytokines, which results in the dysregulation of tryptophan metabolism, that increases quinolinic acid, which is a N-methyl-D-aspartate receptor agonist and this can result in glutamate dysfunction and violent behavior.Citation12
Violence and infections
Violent behavior has been associated with a number of infectious diseases including Spanish flu, encephalitis lethargica, Western equine encephalitis, viral encephalitis, herpes simplex encephalitis, neurosyphilis, cerebral malaria, sepsis, and toxoplasmosis.Citation61–Citation76 In a review of 108 cases of acute viral encephalitis, 23% experienced violence or aggression.Citation77 Criminal behavior as a result of neurological injury has been documented in both acute and chronic infections including neurosyphilis, encephalitis lethargica, herpes simplex encephalitis, AIDS dementia complex, infections causing dementia, and various other viral encephalitides.Citation78–Citation81
T. gondii seropositive individuals have higher aggression and impulsivity scores, which suggests T. gondii changes brain chemistry in a fashion that increases the risk of aggressive behavior. The personality of men infected with T. gondii showed higher apprehension compared to uninfected controls, lower superego strength, and higher vigilance, they were more likely to disregard rules, and were more expedient, suspicious, jealous, and dogmatic. Possible mechanisms by which T. gondii may affect human behavior include its effect on dopamine and on testosterone.Citation82
Parasitic infections have adverse effects throughout life, but are particularly traumatic to the young. Newborn children need 87% of their metabolic energy for brain functioning, while the brains of 5-year-old children consume 87% of their metabolic energy and an adult brain requires approximately a quarter of the body’s energy. In addition to the pathogenic effects of parasites, they also compete for energy which can harm brain development and functioning, which can in turn contribute to violent behavior.Citation28
Violence and infectious diseases in animals
Parasites sometimes manipulate the behavior of hosts in a manner that facilitates their survival and reproduction.Citation83 Sometimes this manipulation includes fostering aggressive behavior.Citation84,Citation85 Historically, rabies has been the main model for infections causing violence in animals.Citation86 In addition, aggression associated with tick-borne infections in animals has been documented with Babesia microti in mice,Citation87 Babesia gibsoni in dogs,Citation88 B. burgdorferi in dogs,Citation89,Citation90 Bartonella henselae in dogs,Citation91 B. henselae in horses,Citation92 and B. burgdorferi in chimpanzees.Citation93,Citation94
In order to study the neuroendocrine effects, work has been done with prairie voles and dogs to understand aggressiveness in animals with selective aggression versus affiliation and bonding in the context of arginine-vasopressin versus oxytocin.Citation95–Citation97 Both the neuropeptides are significant in social behavior, but oxytocin is more associated with affiliation while arginine-vasopressin is more associated with aggression and male behavior.Citation98 In sheep, increased oxytocin results in maternal acceptance while lower levels may result in violent rejection and indifference toward a newborn.Citation99 In humans, low oxytocin levels are associated with alexithymia and anorexia nervosa.Citation100 Arginine-vasopressin and oxytocin are released from the posterior pituitary gland, a part of the brain lacking a blood–brain barrier and more vulnerable to penetration by B. burgdorferi which has been demonstrated in the vasculature in a murine model.Citation101–Citation104
Murine and primate models demonstrated infection of the trigeminal nerve is a transneuronal entry route for brain infections involving temporal lobe and limbic structures.Citation22,Citation105
Violence and LD
More serious cases often involve a complex interactive infection with Lyme borreliosis and other tick-borne coinfections and sometimes the activation of opportunistic viruses and other pathogens. A survey of over 3,000 chronic LD patients demonstrated that over 50% had laboratory-confirmed coinfections and 30% had two or more coinfections, including Babesia (32%), Bartonella (28%), Ehrlichia (15%), Mycoplasma (15%), Rickettsia rickettsia (6%), Anaplasma (5%), and Francisella tularemia (1%). A very similar study of chronic Lyme patients in Canada demonstrated similar coinfection rates.Citation106,Citation107 Although some tick studies show that coinfection rates are relatively low, these findings can be explained since chronically ill patients often report exposure to multiple tick bites.
The first human reference to aggressiveness with tick-borne diseases that could be located was a 1990 study by Logigian et al demonstrating that 26% of chronic Lyme patients had extreme irritability.Citation108 In 1991, Harvey et al described a patient who became aggressive and combative following a Bartonella infection.Citation109 The first reference to homicide associated with LD was a meatpacker who killed his supervisor at a meat-packing plant in Michigan in 1992 and used LD as part of the defense. His identical twin who did not have LD had no neurological deficits or history of violence.Citation110 In 1992, Fallon et al described a man acutely sensitive to sound who was so intensely bothered by the noise of his 3-year-old son that he picked him up and shook him in a sudden and unprecedented fit of violence.Citation111 Sherr described LD patients having sudden personality changes, in people of known character after acquiring LD, including outbursts of anger, breaking doors, cursing at other drivers, and road rage.Citation112 In a publication, a LD patient described an incident where someone else pulled into a parking space that he wanted; he responded by jumping out of his car and knocking the other driver unconscious. Another LD patient was described lunging out of his car after a motorist beeped the horn and he began pounding on the windshield of their car, then suddenly stopped in bewilderment because he did not recall or understand why he was behaving in this manner. Another LD patient was arrested for shoplifting during a state of confusion, and another patient was accused of pedophilia.Citation113
Other media reports include: a LD patient who stalked, threatened to rape, and made repeated threats against multiple political candidates;Citation114 a LD patient committed sexual acts with his 9-year-old son;Citation115 a LD patient shot at police after a 911 call;Citation116 a LD patient was charged with assault associated with marital conflicts;Citation117 and there have been multiple additional references to aggressiveness, violence, homicidality, and homicide associated with LD.Citation6,Citation9,Citation54,Citation113,Citation118–Citation136
In one presentation, 26 different individuals with LD committing multiple violent acts including multiple assaults on police officers and 11 homicides were described.Citation137 Violent behavior seen with LD included homicide; suicide; combined homicide and suicide; assaults with a gun, knife, sword, axe, hammer, rocks, and darts; assaulting a sibling’s head with a rock; pedophilia; stalking; child abuse; assault toward teachers and other students; assaults at summer camp; self-inflicted injuries; road rage incidents; domestic violence; torturing household pets; killing pets; armed robbery; fire setting; shoplifting; destroying property with total amnesia of the event afterwards; breaking and attempting to break automobile windshields; and various forms of public lewdness.Citation137
Antibiotic treatment has on occasion provoked aggressive behavior as a result of the Jarisch–Herxheimer reaction.Citation111,Citation138 There were a number of homicides associated with LD in the press. A LD patient strangled his fiancé with a dog leash. He was considered psychotic at the time of the homicide by the examining forensic psychiatrist.Citation139,Citation140 A LD patient bludgeoned his mother to death while she was sleeping.Citation141 There was a murder, suicide of a couple with advanced LD who also killed the pet dog.Citation142 There was a LD homicide in a Shelter Island in which a Lyme patient killed a longtime friend. The news release states, “Norstrom stated ‘in my own research in the past dozen years we’ve seen a lot of this.’”Citation143–Citation145
In a further communication with Norstrom, he gave consent to publish the following information. He has worked with a very large number of LD patients; he described a significant number of patients with aggressive behavior, such as women who had told him they wanted to hurt their children and did not know why; an easygoing man is arrested for a brawl who had no history of abuse; a teenager who became involved in physical altercations with peers, parents, and teachers; people who never said hell or damn going into a rage; children breaking the bones of their sibling, throwing a TV set through a window, destroying their bedroom, picking fights with classmates; and a teenager who went to a neighbor’s house and attacked him with a hammer because he thought the neighbor was going into his house. He stated he could list hundreds of other similar examples. Noise was magnified and certain pitches, a whiney voice, a squeak in a gate hinge, a barking dog, a crowd of people’s voices seem to bring on irrational behavior (Nostrom SJ, founder and director of Lyme borrelia Out-Reach Foundation, personal communication, August, 2008).
There were indications the shooter at the Sandy Hook Elementary School massacre, Adam Lanza, may have had LD, however the medical examiner failed to pursue LD assessment.Citation146–Citation148 LD has been a valid defense in the legal system.Citation149 LD has been used as a defense in assaults, such as detonating a fertilizer bomb and an axe attack.Citation150,Citation151
When discussing homicide associated with LD, it is more common to think of a LD patient with a mental impairment who kills another person; however, there are other homicides associated with LD. In one case, the wife of a debilitated LD patient assisted in the planning and implementation of his suicide and pleaded guilty to felony murder.Citation152 In reviewing other legal cases involving fatalities, LD patients who were inadequately diagnosed and treated earlier in their illness became debilitated with chronic pain, developed opioid dependence and abuse, and died from opioid overdoses.Citation153
In a prior study analyzing the prevalence of findings, patients who were both homicidal and suicidal demonstrated low frustration tolerance (100%), cognitive symptoms (100%), sudden mood swings (93%), generalized anxiety (90%), explosive anger (83%), disinhibition (80%), panic disorder (80%), paranoia (76%), depersonalization (76%), hypervigilance (72%), anhedonia (72%), intrusive images (48%), obsessive compulsive disorder (48%), hallucinations (45%), substance abuse (28%), posttraumatic stress disorder (PTSD) (24%), and dissociative episodes (18%).Citation12 In another presentation evaluating children with LD, 53% had anger/irritability, 25% had rages/explosive behavior, 54% had panic attacks, and 50% had mood swings.Citation154
Neural circuitry of violence and infections
Infections and the associated immune provocation can sometimes alter the functioning of cortical, limbic, and brainstem functioning. Brain regions and associated circuits particularly significant to aggressive potential include the amygdala, the right ventromedial prefrontal cortex, the orbitofrontal cortex, the anterior cingulate, and the ventral hippocampus.Citation53,Citation155,Citation156 The amygdala is involved in fear responsiveness and other negative emotions, the right ventromedial prefrontal cortex mediates empathic responsiveness, and the orbital frontal cortex plays a crucial role in constraining impulsive outbursts, while the anterior cingulate cortex recruits other brain regions in response to conflict, and the basolateral amygdala and ventral hippocampus are significant with traumatic memory.
Infectious encephalopathies are most commonly associated with impulse control disorders and predominately white matter encephalopathies with dysfunction of the prefrontal cortex and limbic structures. LD is commonly associated with white matter dysfunction, and many patients have explosive anger. Intermittent explosive disorder is associated with lower white matter integrity of the superior longitudinal fasciculus and density and lower white matter integrity in long-range connections between the frontal and temporoparietal regions.Citation157
A certain type of temporal lobe and amygdala damage is strongly associated with predatory aggression in which there is impaired recognition of social emotions. This type of aggression has many similarities to Kluver–Bucy syndrome, which is a rare condition associated with temporal lobe injury and dysfunction. It includes visual agnosia, excessive oral tendencies, hypermetamorphosis, placidity, altered sexual behavior, and changes in dietary habits.Citation158 Psychopathic and serial killers display visual agnosia and consistently lack normal empathetic human interpersonal recognition, and humans are not human to them.Citation159 Kluver–Bucy syndrome is caused by a number of conditions including head injuries and a number of infections that injure the temporal lobes. These infections include Mycoplasma pneumoniae, tubercular meningitis, herpes simplex encephalitis, herpes meningoencephalitis, tick-borne infections, Epstein–Barr virus, and neurocysticercosis.Citation160–Citation170
Infections and aggression: psychoimmunology and neurochemistry
From an evolutionary medicine perspective, zoonotic parasites that manipulate the aggressive and social behavior of hosts achieve this by altering the actions of serotonin, dopamine, and norepinephrine, but in particular serotonin.Citation171 Persistent infections and the immune reactions to them are associated with chronic inflammation and sometime autoimmune reactions.
Persistent inflammation is associated with increased interleukin-6 and interleukin-1 beta, reduced serotonin as demonstrated by reduced 5 hydroxy-indoleacetic acid, and increased quinolinic acid which is a N-methyl-D-aspartate receptor agonist that contributes to glutamate dysregulation and can result in both aggressive and self-destructive behavior (the death formula).Citation12,Citation172,Citation173 These immune and associated biochemical findings have been seen in a number of infections associated with violence, including LD, cerebral malaria, and HIV.Citation53,Citation54,Citation174 Other evidence supporting the association between inflammation and aggression includes hepatitis C treatment with interferon alpha, which can be associated with irritability, impulsiveness, hostility, aggression, anger, emotional lability, and relapse of substance abuse.Citation175–Citation177
Autoimmune reactions are also associated with aggression, and they have been seen in cases of pediatric autoimmune diseases associated with Streptococcal infections, M. pneumoniae and human herpesvirus 7 encephalitis, limbic encephalitis, and anti-N-methyl-D-aspartate receptor encephalitis.Citation178–Citation182
Materials and methods
The author specializes in treating treatment-resistant psychiatric illnesses and some of the patient charts include patients with LD. A total of 1,000 inactive charts of patients with LD from the author’s practice were retrospectively reviewed. Three groups of charts were reviewed, and aggregate data were collected – of those involving LD and aggressiveness, 50 homicidal LD subjects were compared with 50 who were not homicidal, and charts involving homicide were analyzed in more detail.
In the first part of the study, the charts of patients who had aggressive thoughts, impulses, and/or behaviors were selected and reviewed. These charts were reviewed for documentation or statements giving insight into the pathophysiology. All but two were from the United States.
In the second part of the study, the charts were screened until 50 charts of LD patients with homicidality with completed neuropsychiatric assessments were identified. Fifty randomly selected charts of LD patients who were not homicidal were selected as a control group. None of these control charts were used in the previous study on suicidality, and all were from the United States.Citation12 These patients were evaluated with a comprehensive assessment including premorbid assessment, history of tick exposure, history of the presence of erythema migrans rash, early tick-borne disease symptoms, symptoms in the course of illness, current status with a comprehensive neuropsychiatric and general medical assessment, review of systems using the 280-item Neuropsychiatric Lyme Assessment with pattern recognition, and a review of laboratory assessment, which may include enzyme-linked immunosorbent assay, immunofluorescent assay, Western blot, DNA-based testing, coinfection testing, single-photon emission tomography, magnetic resonance imaging, or other diagnostic testing to determine the diagnosis in compliance with the Institute of Medicine–recognized guidelines.Citation183–Citation187 In addition to diagnostic criteria, the patients who met Center for Disease and Prevention surveillance criteria were noted, which is more stringent criteria and captureŝ10% of LD cases.Citation188
Only testing from laboratories validated by the Clinical Laboratory Improvement Amendments of the US Department of Health and Human Services Centers for Medicare and Medicaid Services was considered valid. This is sometimes confused with the US FDA clearance for mass marketed test kits which does not validate the fundamental accuracy of the test but instead demonstrates it is comparable to other similar tests that may or may not have been properly validated in the first place. Charts in which the diagnosis of LD was unclear were excluded from the study. Names were converted to an identifier before entering the findings into a database of individual participant data. The charts were then reviewed with their identity protected to extract aggregate data, including findings relevant to homicidality and aggression, and were analyzed. The baseline health status of each of these two groups before infection was compared with the postinfection findings and the clinical findings of the subjects who were homicidal were compared with the subjects who were not homicidal. Symptoms associated with risk were ranked by comparing the prevalence of different findings among the two different groups.
Data collection included age, sex, diagnosed by comprehensive criteria, Center for Disease Control and Prevention surveillance criteria, years before diagnosis and antibiotic treatment, coinfections, comorbid conditions, pre-existing symptoms before infection, misdiagnoses, number of homicides, attention deficits, auditory hyperacusis, other sensory hyperacusis, memory impairments, processing impairments, dyslexia symptoms, facial memory, depersonalization, derealization, intrusive aggressive images, intrusive sexual images, nightmares, hallucinations, executive functioning impairments, decreased frustration tolerance, sudden abrupt mood swings, hypervigilance, paranoia, disinhibition, exaggerated startle reflex, explosive anger, suicidal tendencies, homicidal tendencies, decline in social relationships, decline in school or work productivity, marital and/or family problems, substance abuse, legal problems, dissociative episodes, depression, rapid cycling bipolar disorder episodes, panic disorder, obsessive compulsive disorder, social anxiety disorder, generalized anxiety disorder, PTSD, sleep disorders, anhedonia, cranial nerve symptoms, seizures, neuropathy, incontinence, decreased libido, irritable bladder, genital pain, chronic pain, and intolerance to alcohol.
The data of the impairments were charted and calculated to the 95% confidence interval (CI). The total impairments of all the 100 patients analyzed was charted preinfection and postinfection, and the 95% CI was calculated for each impairment. The incidence of each psychiatric symptom was calculated for the homicidal versus the non-homicidal groups.
In addition, homicides involving LD were reviewed in greater detail and categorized in regard to the type of homicide (impulsive, psychotic, or predatorial), and additional information was extracted. All the patients were from the United States.
The data were then abstracted to assess the association between aggression, violence, and homicide and LD to create a model for aggressiveness, violence, and homicidality in LD patients to possibly explain and ultimately prevent such an association, if it is found.
Ethical considerations
The Meridian Health Institutional Review Board, Neptune, NJ, USA, approved this study (IRB # 201704192J). Patient consent to review their medical records was not required by the Institutional Review Board as there was minimal risk to subjects, no subject identifiers or links to identifiers were used or collected, and it was a retrospective chart review of already existing data.
Results
Retrospective chart review: aggressiveness
A total of 1000 charts of LD patients were screened to identify charts documenting aggression. All but two were from the US. These charts were then reviewed to identify patterns of aggressiveness. This part of the study was not a statistical analysis of frequency, dominance, or general occurrence of the behaviors discussed.
The most commonly reported aggression with LD was impulsive, sometimes provoked by intrusive symptoms, sensory stimulation or frustration and was invariably bizarre and senseless. Aggression occurred both in homes and in public settings. Some of the aggressive patients had temporal lobe dysfunction, sometimes accompanied with partial seizures. Acute episodes of rage, sometimes referred to as “Lyme rage,” were reported and were witnessed on multiple occasions. The anger during these episodes had a very abrupt onset and was extremely intense and often with minimal cognitive control.
Patients described horrific intrusive symptoms. At night, they would take the form of vivid nightmares. During the day, these intrusive symptoms could be intrusive images, thoughts, and/or impulses. A typical description is that these intrusive symptoms include descriptions of frightening, stabbing, horrific images, usually of death, dying, or pain and suffering. They could be gory and unreal as in a horror story with faces with blood or terror exaggerated, awful expressions. They are described as people in the worse possible situation, perhaps close to death. These images can then evolve into visions of stabbing or killing, most commonly of people close or familiar to the person. A number of patients have described intrusive thoughts of killing multiple family members and themselves. Representative cases include a young adolescent with seizures who had repeated urges to kill their younger sibling. Another patient who had frequent temporal lobe seizures had intrusive thoughts of killing with an axe or knife any female he had a relationship with and described a mechanism in their head that would say kill her, kill her. These thoughts were invariably ego dystonic. The same patient also had thoughts of killing infant and adult female family members. In some cases, the aggression can be particularly toward women. Some patients described intrusive bizarre sexual and pedophilic thoughts and impulses. Others also described sudden and unprovoked urges to harm family members, and sometimes these episodes would be preceded by feeling a sense of derealization. Patients also describe intrusive and unprovoked episodes of anger with an urge to destroy. One patient described sudden urges to rip the room apart and kill everyone and every animal in the house. The intrusive episodes are often described as being episodic and not continuous. The images do not seem to necessarily be associated with a particular trigger, and one patient described them as invading the privacy of their mind.
Patients described fear of their suicidal and homicidal rage. It is described as rage that comes out of nowhere and takes over their whole body, with no control over it. In some, it is worse when they are driving. Some patients are scared for the people who come in contact with them and are afraid the thoughts will become even worse. Patients have described episodes of anger that would occur suddenly and totally unprovoked. A patient described looking at someone and feeling anger for no reason whatsoever, for example, looking at someone in a restaurant and having an urge to hurt the person. A patient described road rage out of nowhere and fantasies of beating and killing people. Patients have also described obsessions where they wished they had an excuse to go after someone. Another patient had an intrusive urge to throw a baby off of a balcony. He was particularly frightened when he had these urges in the presence of children and considered suicide to prevent himself from killing anyone.
One patient described that his pain was so bad, and he wanted to take it out on everyone else. Another patient who developed an impairment of empathy and was highly sensitive to perceived injury expressed, “if someone hurts me, I want to hurt them back. I want to make them cry. I want them to feel my pain.” Others responded to the intrusive homicidal and harmful impulses by becoming suicidal or self-destructive in an effort to prevent themselves from harming others. One patient accused his family members of being imposters.
Frequently, the thoughts or impulses to harm are preceded by being overstimulated, often by sound. For example, a normally passive individual who is an animal lover has hyperacusis and has intrusive hostile imagery of killing the dog by bludgeoning, suffocation, stabbing, or poisoning when it howled. Another patient responded to the neighbor’s dog barking by opening the window and screaming death threats to the dog. After acting in that manner, the patient began crying uncontrollably and wanted to die. Another patient described intrusive, overpowering very violent thoughts which sometimes would be triggered by stimulation; such as a dog barking, a bird chirping, a strobe light, or the presence of other people. Another patient described that the noise of her neighbors playing sports was unbearable. She had an urge to go to the neighbors and start screaming wildly. Sound is not the only trigger. A patient described sitting at a table with guests and her father behind her. When the father called for the dog, the patient became startled, punched her father and screamed at him with a total lack of control.
Not all aggressiveness is described as being provoked by stimulation. Some LD patients are intolerant to alcohol and/or react strongly to low doses of psychotropics or have idiosyncratic reactions to them. Some episodes are associated with the combination of the effects of LD and exposure to a number of medications and/or alcohol. A number of legal cases have involved bizarre and aggressive behavior while under the effects of alcohol and/or medications.
A few patients who had acquired LD as a congenital infection or were infected at a very young age had significantly impaired recognition of emotions of social significance and had difficulty processing interpersonal cues. They would sometimes take offense when normal limits were set on them. This occasionally resulted in a perceived injury, a rapid escalation of agitation, and because of their impaired capacity for empathy, it would sometimes result in assaultive behavior. Violent behavior seemed more problematic when the illness began in young children who have no memory to serve as a reference point for healthy functioning. There were a number of cases involving children infected at a young age that were quite severe. In these cases, psychopathic traits are evident, and the patients may repeatedly assault their family members, damage their house, knock over furniture, and kick and punch holes through walls and doors. Frequent police intervention was needed with these patients. In these cases, there is often a lack of empathy and a lack of remorse for their behavior. With antibiotic and psychotropic treatment, the impulse control disorder can improve, but sometimes lack of empathy and lack of remorse can persist.
The oldest legal case that could be found involving LD was in 1993, in which the patient was treated and the legal charges were dismissed. A number of cases were managed in a similar manner over a span of years. There were a number of shoplifting cases, mostly involving females. There were a few cases involving fire setting. In one case, the patient burned down his house as a result of a paranoid delusion. Some individuals with psychotic symptoms acted bizarrely and were repeatedly drawing the attention of the legal system and occasionally SWAT (special weapons attack team) teams. A few patients attacked multiple police officers in a bizarre and senseless manner.
Retrospective chart review: homicidality
Inactive charts were reviewed until 50 LD subjects with homicidal tendencies were identified, that is, 520 charts were screened until 50 cases could be identified (9.6%). A few of these charts had a few incomplete data points. There were 98% (N=49) of the subjects who were also suicidal. In this group of 50 homicidal patients, there were five homicides. The subjects who committed homicides were incarcerated and evaluated in forensic settings. Forty nine of the 50 homicidal patients were not homicidal before being infected with LD. It is possible one patient may have been homicidal before being infected with LD. The average age was 35 years (youngest 11 years and oldest 63 years). The average age of onset of illness was 26 years. There were 52% male and 48% female subjects, and 10% were diagnosed immediately after infection, but had inadequate initial treatment. The average subject experienced a delay of 9 years before diagnosis and treatment. There were 22% of subjects that were diagnosed in ≤2 years. The longest length of time before diagnosis was 40 years. There were 66% that met Center for Disease and Prevention Surveillance Criteria for Lyme disease. All who committed homicides met the Surveillance Criteria. There were 84% of subjects misdiagnosed at some point, and the misdiagnoses included “all in your head,” “just nuts,” “laziness,” “nervousness,” “hyper,” “a witch in another life,” “psychiatric,” “everything,” bipolar depression, depression, major depression, panic disorder, anxiety attacks, alcoholism, attention deficit disorder, pervasive developmental disorder, PTSD, anxiety, intermittent explosive disorder, adjustment reaction, obsessive compulsive disorder, oppositional defiant disorder, multiple sclerosis, brain tumor, Alzheimer’s disease, visual labyrinthitis, headaches, sensory motor dysfunction syndrome, migraine syndrome, sciatica, bulging disc, dysautonomia, orthostatic intolerance, seizure disorder, amyotrophic lateral sclerosis, vertigo, Meniere’s disease, chronic fatigue/immune deficiency syndrome, fibro-myalgia, lupus, arthritis, rheumatoid arthritis, mononucleosis, bronchitis, asthma, fever of unknown origin, erythromelalgia, systemic candidiasis, food allergies, and flu.
Coinfections in this group in order of frequency included Babesia, Anaplasma, Bartonella, Ehrlichia chaffeensis, Epstein–Barr virus, cytomegalovirus, mycoplasma, Rickettsia rickettsii, and Hepatitis C.
An additional 50 charts of LD patients who were not homicidal were randomly selected, and the prevalence of symptoms was compared with the prevalence of the same symptoms in LD patients who were homicidal. In this group, the average age was 42 years (youngest 8 years and oldest 67 years). There were 44% of male and 56% of female subjects. About 10% were diagnosed immediately after infection, but had inadequate initial treatment. The average subject experienced a delay of 8.1 years before diagnosis and treatment. There were 32% who were diagnosed in ≤2 years. The greatest length of time before diagnosis was 39 years. There were 74% meeting Center for Disease and Prevention Surveillance Criteria. Misdiagnosis had occurred in 92% of these subjects.
Both the groups of patients in this study were generally quite healthy compared with the general population, preinfection; however, postinfection, both the groups developed significant cognitive symptoms, emotional symptoms, vegetative symptoms, behavioral symptoms, neurological symptoms, musculoskeletal symptoms, cardiovascular symptoms, gastrointestinal symptoms, urogenital symptoms, and other symptoms. Coinfections in this group in order of frequency included Babesia, Bartonella, E. chaffeensis, Anaplasma, mycoplasma, R. rickettsii, Epstein–Barr virus, Chlamydia pneumoniae, and Coxiella burnetii.
Comparing the two groups, it was found that there were significant differences in the prevalence of psychiatric symptoms, behavioral symptoms, psychiatric syndromes, cognitive symptoms, neurological symptoms, and urogenital symptoms. Not all symptoms that were studied showed a statistically significant separation between the two groups that might explain homicidality or appeared relevant to violence. These symptoms included attention deficits, auditory hyperacusis, other sensory hyperacusis, facial memory impairments, executive functioning impairments, decreased frustration tolerance, fatigue, sleep disorder, decline in social relationships, decline in school or work productivity and chronic pain. A number of signs, symptoms and syndromes associated with violent risk were increased in the homicidal group and these findings were further analyzed. The 95% CI was calculated for each data point ().
Table 1 The homicidal group had more impairments postinfection
Both the homicidal and non-homicidal groups showed an increase of all the impairments studied preinfection versus postinfection (95% CI) ().
Table 2 All impairments were increased postinfection
The homicidal group had a greater incidence of all the psychiatric symptoms studied when compared to the non-homicidal group. The mean of the psychiatric symptoms was 71% in the homicidal versus 41% in the non-homicidal group ().
Retrospective chart review: homicide
In reviewing the LD charts involving both LD and homicide, 10 homicides were identified. None of these homicides were cases discussed when reviewing media reports in the “Background” section. Three of the 10 homicides involved suspected LD that was not confirmed, and these cases were not included in the study. The other seven homicides were associated with well-confirmed cases of LD. All seven victims had a prior personal relationship with the perpetrators, either real or imagined by the perpetrator. Two of these cases did not have completed neuropsychiatric assessments and were included in the retrospective chart review of homicides but were not included in the retrospective data analysis of homicidal LD patients.
Of the seven homicides, one was a combined homicide, dog killing, and suicide, which seemed to have been related to impulsivity. Also there were other homicide, dog killing, and suicide cases which occurred that were not evaluated by the author.Citation189,Citation190 Another homicide was associated with psychosis, and the other five had predatory features. In a predatory case, the Lyme enzyme-linked immunoassay was 6.83 (positive ≥ 1.10). Whenever these cases involving homicide were tested for coinfections, there was positive reactivity to coinfections, which included Bartonella, Babesia, mycoplasma, Anaplasma phagocytophilum, E. chaffeensis, and viral coinfections. All cases involving predatory aggression also included a history of reported abuse. Findings also included head injuries, social communication impairments, an impaired capacity to bond and empathize with others, social isolation, a fascination with knives, less than a normal amount of anxiety, fire setting, and torturing animals prior to the homicides. In all of the LD cases involving homicide, there were obstacles preventing both adequate antibiotic and psychiatric treatments.
Discussion
Upon reviewing the existing literature and the retrospective chart reviews, LD patients postinfection may acquire a number of impairments that are collectively associated with an increased risk of violence and homicidality, but some acquired impairments are more likely to increase risk than others. In spite of having impairments, the majority of LD patients are able to compensate and may only demonstrate low frustration tolerance and irritability. Some, however, demonstrate more severe symptoms. To better understand why many LD patients are not aggressive, while others can be highly aggressive, it is necessary to look at the different symptoms seen in these two groups.
For organizational purposes, the data are presented as cognitive impairments, emotional impairments, behavioral symptoms, psychiatric syndromes (multiple brain regions), neurological impairments, and somatic impairments.
Individuals with cognitive impairments have less coping skills and in general can have increased risk for violence. Among the homicidal subjects in this study, 98% had impaired capacity for sustained and/or selective attention; 88% had auditory hyperacusis (misophonia); 86% had sensory hyperacusis to light, touch, and/or smell; 98% had memory impairments (most commonly working memory and short-term memory); 94% had processing impairments; 78% had dyslexia symptoms; and 98% had executive functioning memory impairments. Sensory hyperacusis is associated with an impaired capacity to filter incoming stimulation, resulting in a sensory overload, and contributes to making a patient more reclusive and socially isolated and also contributes to them being more emotionally reactive to stimulation that average people can easily tolerate. Some patients have selective hyperacusis to mouth sounds, which I propose may possibly be the result of a disinhibition of a primitive fear of oral predation from brain dysfunction. Facial memory impairments were similar in both the homicidal and non-homicidal groups and seems to be non-contributory. However, patients with more violent potential had an impairment of emotional recognition when they saw a familiar person, and this impairment would sometimes result in their accusations that family and friends were imposters (Capgras’ syndrome).Citation191
Individuals with certain emotional impairments can have greater risk for aggressiveness. Among the homicidal subjects in this study, 71% had depersonalization, 37% had derealization, 62% had intrusive aggressive images, 26% had intrusive sexual images, 82% had vivid nightmares, 47% had hallucinations, 98% had decreased frustration tolerance, 94% had sudden abrupt mood swings, 84% had hypervigilance, 88% had paranoia, 84% had disinhibition, 84% had exaggerated startle reactions, 91% had explosive anger, 38% had dissociative episodes, and 86% had anhedonia.
Individuals with certain behavioral symptoms can have greater risk for aggressiveness. Among the homicidal subjects in this study, 98% were suicidal, 91% had a decline in social functioning, 90% had a decline in school or work productivity, 80% had marital and/or family problems, 33% had substance abuse, and 42% had legal problems.
Individuals with certain psychiatric syndromes can have greater risk for aggressiveness. Among the homicidal subjects in this study, 98% had depression, 28% had rapid cycling bipolar illness, 82% had panic disorder, 51% had obsessive compulsive disorder, 66% had social anxiety disorder, 86% had generalized anxiety disorder, and 36% had PTSD.
Individuals with certain urological symptoms, particularly urinary incontinence (along with torturing animals and fire setting), are considered by some to be at greater risk for predatory aggression. Among the homicidal subjects in this study, 38% had urinary incontinence, 56% had irritable bladder, and 32% had genital pain.
Among the homicidal subjects in this study, 44% had intolerance to alcohol with a more exaggerated response to alcohol consumption. Alcohol intoxication is a well recognized risk for violence and homicide.Citation192
Among the homicidal subjects in this study, other symptoms that were present but may or may not correlate with homicidal risk included 96% with sleep disorders, 38% with decreased libido, 92% with cranial nerve symptoms, 92% with neuropathy, 20% with seizures (mostly complex partial), 48% with chronic pain, and 92% with fatigue.
Violent behavior was more problematic when the illness began in young children who had no memory to serve as a reference point for healthy functioning.
Although data are limited in two of the homicide cases, it seems in the cases involving homicides that there were other contributors to violence; however, it also seems that these homicides would not have occurred if the perpetrators had not had neurological deterioration as a result of LD.
Multiple patients described intrusive thoughts, images, and impulses to kill everything, including themselves. These descriptions have similarities to the episodes in which the individuals attempt to kill everyone and everything, including house pets and themselves. The pathophysiology behind this process may be the result of the previously described death formula (persistent infection→persistent proinflammatory cytokines→dysregulation of tryptophan metabolism→quinolinic acid→N-methyl-D-aspartate receptor agonism→glutamate dysregulation→neural circuit dysfunction→psychiatric dysfunction→suicidal and/or homicidal tendencies) which may be a pathophysiological explanation of the death drive (Thantos) concept that was first proposed by Spielrein and further advanced by Freud.Citation12,Citation193 It is unclear why a few LD patients develop the collective risk contributors for violence, but most do not. Possible explanations include the following – there is a genetic vulnerability that is triggered in only some who become infected, some other pathogen or pathogens other than Borrelia (either tick-borne or opportunistic within the host microbiome) may be responsible for causing the aggressiveness or it may be more the immune reaction to the infection rather than the infection itself that is causative, and this immune reaction may have multiple other causes. In this study, there was no clear difference in the coinfections in the homicidal versus the non-homicidal group.
In synthesizing these findings, the following model for violence and LD can be constructed ( and ).
Figure 3 Violence results from the interactive effects of contributors, failed deterrents, and acute triggers.
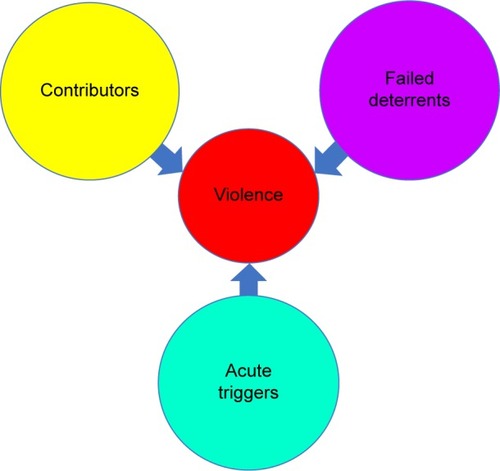
Figure 4 Violence is more likely to occur in Lyme disease patients when there is a greater number and severity of the contributors to violence combined with compromised deterrents and acute triggers.
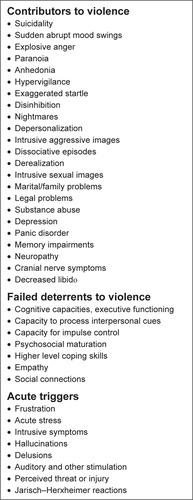
There are multiple mechanisms through which infection may contribute to violence, and many seem to be immune mediated. Impairments associated with infectious disease that can contribute to violent behavior include decreased frustration tolerance; decreased impulse control; cognitive impairments; sensory hyperacusis; hypervigilance; paranoia; increased startle reflex, particularly increased acoustic startle; sudden abrupt mood swings; impairment in the ability to regulate emotional arousal levels; social anxiety disorder when contributing to social isolation; obsessive compulsive disorder combined with intrusive thoughts, images, and compulsions that are of aggressive nature and/or sexually aggressive nature; hyposexuality and hypersexuality, both of which cause increased interpersonal frustration; suicidal and homicidal preoccupations, intrusive images, and urges; decreased bonding capacity; decreased empathy; decreased emotional insight; depersonalization; derealization; dissociative states; illusions; delusions; hallucinations and decreased tolerance to the effects of drugs and alcohol.
Conclusion
Violent behavior is the result of a complex interaction of many contributors, failures of deterrents, and acute triggering events. From evolutionary, geographical, epidemiological, and historical perspectives, multiple studies, case reports, and animal studies, some infections can be associated with violence. These infections have psychoimmune and pathophysiological implications through multiple mechanisms that include proinflammatory and autoimmune mechanisms that can cause multiple impairments impacting brain neurochemistry and neural circuit functioning which can cause different types of violence. LD can be one of the many infectious contributors associated with aggressiveness, violence, homicidality, and homicide. There is support for this from journal citations, presentations, animal studies, psychoimmunology, neurochemistry, neural circuity, reports, and observations. Delays in diagnosing and treating LD may result in an increased risk of aggressiveness that can result in impulsive, psychotic, and/or predatory aggression. Most violence seen with LD seems to be impulsive, bizarre, and senseless.
The most common case is a young male with impairments during development who lacks a reference point of mature healthy functioning before the onset of impairment who may be at greater risk for violence if he was infected at a younger age and has impaired recognition of emotions of social significance and difficulty processing interpersonal cues.
LD causes a number of impairments that collectively increase the risk of homicidality. Postinfection findings associated with homicidality that separated from the non-homicidal group within the 95% CI included suicidality, sudden abrupt mood swings, explosive anger, paranoia, anhedonia, hypervigilance, exaggerated startle, disinhibition, nightmares, depersonalization, intrusive aggressive images, dissociative episodes, derealization, intrusive sexual images, marital/family problems, legal problems, substance abuse, depression, panic disorder, memory impairments, neuropathy, cranial nerve symptoms, and decreased libido. Although predatory aggression with LD seems to be an uncommon presentation, it accounts for the greatest number of homicides. A patient who acquires LD and is inadequately diagnosed and treated may be at risk for committing homicide if they have a history of reported abuse, head injuries, social communication impairments, an impaired capacity to bond and empathize with others, social isolation, a fascination with knives, less than a normal amount of anxiety, fire setting, torturing animals, and obstacles preventing adequate antibiotic and psychiatric treatment.
Some patients have selective hyperacusis to mouth sounds, which I propose may possibly be the result of brain dysfunction causing a disinhibition of a primitive fear of oral predation.
As with the vast majority of patients with mental illness, many patients with LD have no aggressive tendencies or only mild degrees of low frustration tolerance and irritability and pose no danger to society. A lesser number experience marital and family conflicts, a lesser number experience explosive anger, a lesser number experience homicidal thoughts and impulses, and a much lesser number commit homicides. Since such a large number of individuals are affected by LD, this small percent of LD cases can be significant and is a cause for concern.
Many of the patients who became aggressive and homicidal responded to effective treatment, and much of the violence associated with LD can be avoided with better prevention, diagnosis, and treatment of LD. Although this article focused upon violence associated with LD, violence associated with other infectious diseases are also significant, and greater research into the association between infections and violence is strongly recommended. Human history is also a history of violence. Understanding violence and recognizing the role of microbes and psychoimmunology opens new opportunities to prevent violent behavior, suffering, crime, war, and social discord and protect peace. We need a multidisciplinary mobilization of our scientific community to better understand all the facets of violence to prevent future tragedies similar to the approach used to understand and prevent airplane crashes.
Acknowledgments
Thanks to Michael J Cook for statistical assistance and Rhiannon Woolwich-Holzman, VMD; Ed Breitschwerdt, DVM, DACVIM; Barbara Rosenthal; Courtney Bransfield; Douglas Bransfield; Phillis Chrampanis and Willison Reed for assistance.
Disclosure
The author has treated, evaluated, and been an expert witness in cases involving homicide and other violent behaviors over a span of 45 years. The author has worked in correctional systems. The author has worked with patients with LD over a span of 30 years and has been an expert witness in cases involving LD and in cases involving LD and homicide, multiple homicides, violent behavior, and other legal cases. The author reports no conflicts of interest in this work.
References
- DupuisMJMultiple neurologic manifestations of Borrelia burgdorferi infectionRev Neurol (Paris)198814412765775 French3070690
- PachnerARBorrelia burgdorferi in the nervous system: the new “great imitator”Ann N Y Acad Sci198853956643190104
- GannonMAncient Lyme Disease Bacteria Found in 15-Million-Year-Old Tick FossilsLive Science2014 Available from: https://www.livescience.com/46007-lyme-disease-ancient-amber-tick.htmlAccessed Jan 6, 2018
- KeanWFTocchioSKeanMRainsfordKDThe musculoskeletal abnormalities of the Similaun Iceman (“ÖTZI”): clues to chronic pain and possible treatmentsInflammopharmacology2013211112023096483
- Lyme diseaseCenter for Disease Control and Prevention Available from: https://www.cdc.gov/lyme/index.htmlAccessed Jan 6, 2018
- FallonBANieldsJALyme disease: a neuropsychiatric illnessAm J Psychiatry199415111157115837943444
- FallonBAKochevarJMGaitoANieldsJAThe underdiagnosis of neuropsychiatric Lyme disease in children and adultsPsychiatr Clin North Am1998213693703viii9774805
- TagerFAFallonBAKeilpJRissenbergMJonesCRLiebowitzMRA controlled study of cognitive deficits in children with chronic Lyme diseaseJ Neuropsychiatry Clin Neurosci200113450050711748319
- GreenbergRThe role of infection and immune responsiveness in a case of treatment-resistant pediatric bipolar disorderFront Psychiatry201787828588506
- HájekTPaskováBJanovskáDHigher prevalence of antibodies to Borrelia burgdorferi in psychiatric patients than in healthy subjectsAm J Psychiatry2002159229730111823274
- BanerjeeRLiuJJMinhasHMLyme neuroborreliosis presenting with alexithymia and suicide attemptsJ Clin Psychiatry2013741098124229748
- BransfieldRCSuicide and Lyme and associated diseasesNeuropsychiatr Dis Treat2017131575158728670127
- KrugEGMercyJADahlbergLLZwiABThe world report on violence and healthLancet200236093391083108812384003
- StahlSMMorrissetteDAMunterNStahl’s Illustrated ViolenceCambridge UKCambridge University Press2014
- LidzCWMulveyEPGardnerWThe accuracy of predictions of violence to othersJAMA19932698100710118429581
- BeckJCWhiteKAGageBEmergency psychiatric assessment of violenceAm J Psychiatry199114811156215651928473
- TardiffKUnusual diagnoses among violent patientsPsychiatr Clin North Am19982135675769774796
- DugréJRDellazizzoLGiguèreCÉPotvinSDumaisAPersistency of cannabis use predicts violence following acute psychiatric dischargeFront Psychiatry2017817628983261
- LewisDOPincusJHFeldmanMJacksonLBardBPsychiatric, neurological, and psychoeducational characteristics of 15 death row inmates in the United StatesAm J Psychiatry198614378388453717422
- FeldmanMMallouhKLewisDOFilicidal abuse in the histories of 15 condemned murderersBull Am Acad Psychiatry Law19861443453523801685
- FreedmanDHemenwayDPrecursors of lethal violence: a death row sampleSoc Sci Med200050121757177010798330
- BransfieldRCWhy Violence?1999 Available from: http://www.mentalhealthandillness.com/may1999.htmAccessed October 20, 2017
- SariaslanALichtensteinPLarssonHFazelSTriggers for violent criminality in patients with psychotic disordersJAMA Psychiatry201673879680327410165
- VolavkaJTriggering violence in psychosisJAMA Psychiatry201673876977027409516
- MathersCThe Global Burden of Disease, 2004 UpdateGeneva, SwitzerlandWorld Health Organization2008
- Homicide-world.pngWikimedia Commons2009 [updated June 8, 2014]. Available from: https://en.wikipedia.org/wiki/File:Homicide-world.pngAccessed October 16, 2017
- US Peace Index Available from: http://peacealliance.org/cms/assets/uploads/2013/05/U.S.-Peace-Index-Overview.pdfAccessed October 16, 2017
- EppigCFincherCLThornhillRParasite prevalence and the worldwide distribution of cognitive abilityProc Biol Sci201027717013801380820591860
- LesterDToxoplasma gondii and homicidePsychol Rep2012111119619723045862
- ThornhillRFincherCLParasite stress promotes homicide and child maltreatmentPhilos Trans R Soc Lond B Biol Sci201136615833466347722042922
- RoserMThe Visual History of Decreasing War and Violence – Our World in Data2011 Available from: https://ourworldindata.org/slides/war-and-violence/Accessed October 16, 2017
- BransfieldRCCould a Pandemic Causing Mental Dysfunction Contribute to Global Instability?Paper presented at: International Lyme and Associated Diseases 7th European ConferenceMay 19, 2017Paris, France
- RetiefFPWesselsADid Adolf Hitler have syphilis?S Afr Med J2005951075075275475616341329
- SacksOAwakeningsNew YorkHarper Perennial1973
- MortonRSDid Catherine the Great have syphilis?Genitourin Med1991674985021774056
- NevinsMMeanderings in Medical History. Book FourBloomington, INiUniverse2016
- DietzPEMentally disordered offenders. Patterns in the relationship between mental disorder and crimePsychiatr Clin North Am19921535395511409020
- GómezJMVerdúMGonzález-MegíasAMéndezMThe phylogenetic roots of human lethal violenceNature2016538762423323727680701
- BransfieldRAre There Psychoimmune and Infectious Contributors to Violence?Paper presented at: New Jersey Psychiatric Association MeetingSeptember 21, 2016Princeton, NJ Available from: https://www.researchgate.net/publication/308549616_Are_There_Psychoimmune_and_Infectious_Contributors_to_ViolenceAccessed Oct 1, 2017
- Shamay-TsoorySGTomerRBergerBDAharon-PeretzJCharacterization of empathy deficits following prefrontal brain damage: the role of the right ventromedial prefrontal cortexJ Cogn Neurosci200315332433712729486
- AdolphsRTranelDDamasioHDamasioAImpaired recognition of emotion in facial expressions following bilateral damage to the human amygdalaNature199437265076696727990957
- AdolphsRBaron-CohenSTranelDImpaired recognition of social emotions following amygdala damageJ Cogn Neurosci20021481264127412495531
- SieverLJNeurobiology of aggression and violenceAm J Psychiatry2008165442944218346997
- DavidsonRJPutnamKMLarsonCLDysfunction in the neural circuitry of emotion regulation – a possible prelude to violenceScience2000289547959159410915615
- RaineABuchsbaumMLaCasseLBrain abnormalities in murderers indicated by positron emission tomographyBiol Psychiatry19974264955089285085
- StahlSMDeconstructing violence as a medical syndrome: mapping psychotic, impulsive, and predatory subtypes to malfunctioning brain circuitsCNS Spectr201419535736525296964
- RitovGArdiZRichter-LevinGDifferential activation of amygdala, dorsal and ventral hippocampus following an exposure to a reminder of underwater traumaFront Behav Neurosci201481824523683
- HeathNMChesneySAGerhartJIInterpersonal violence, PTSD, and inflammation: potential psychogenic pathways to higher C-reactive protein levelsCytokine201363217217823701836
- EralySANievergeltCMMaihoferAXMarine Resiliency Study TeamAssessment of plasma C-reactive protein as a biomarker of posttraumatic stress disorder riskJAMA Psychiatry201471442343124576974
- ZimmermanGShaltielGBarbashSPost-traumatic anxiety associates with failure of the innate immune receptor TLR9 to evade the pro-inflammatory NFκB pathwayTransl Psychiatry20122e7822832815
- CopelandWEWolkeDLereyaSTShanahanLWorthmanCCostelloEJChildhood bullying involvement predicts low-grade systemic inflammation into adulthoodProc Natl Acad Sci U S A2014111217570757524821813
- BobPRabochJMaesMDepression, traumatic stress and interleukin-6J Affect Disord20101201–323123419359044
- BransfieldRCIntrusive symptoms and infectious encephalopathiesNeurol Psychiatry Brain Res20162234
- BransfieldRCThe psychoimmunology of Lyme/tick-borne diseases and its association with neuropsychiatric symptomsOpen Neurol J20126889323091569
- RosellDRSieverLJThe neurobiology of aggression and violenceCNS Spectr201520325427925936249
- LidbergLBelfrageHBertilssonLEvendenMMAsbergMSuicide attempts and impulse control disorder are related to low cerebrospinal fluid 5-HIAA in mentally disordered violent offendersActa Psychiatr Scand2000101539540210823300
- PucilowskiOKostowskiWAggressive behaviour and the central serotonergic systemsBehav Brain Res19839133486309192
- VirkkunenMGoldmanDNielsenDALinnoilaMLow brain serotonin turnover rate (low CSF 5-HIAA) and impulsive violenceJ Psychiatry Neurosci19952042712757544158
- de BoerSFCaramaschiDNatarajanDKoolhaasJMThe vicious cycle towards violence: focus on the negative feedback mechanisms of brain serotonin neurotransmissionFront Behav Neurosci200935219949469
- CoccaroEFLeeRCoussons-ReadMElevated plasma inflammatory markers in individuals with intermittent explosive disorder and correlation with aggression in humansJAMA Psychiatry201471215816524352431
- HallAEpidemic Encephalitis. (Encephalitis Lethargica)Bristol, UKJohn Wright and Sons1924
- CheyetteSRCummingsJLEncephalitis lethargica: lessons for contemporary neuropsychiatryJ Neuropsychiatry Clin Neurosci1995721251347626955
- MulderDParrottMThalerMSequelae of western equine encephalitisNeurology1951131832714853039
- McMillanTMPapadopoulosHCornallCGreenwoodRJModification of severe behaviour problems following herpes simplex encephalitisBrain Inj1990443994062252971
- AhokasARimonRKoskiniemiMVaheriAJulkunenISarnaSViral antibodies and interferon in acute psychiatric disordersJ Clin Psychiatry19874851941962437102
- AnstettREWoodLThe patient exhibiting episodic violent behaviorJ Fam Pract19831636056096827236
- GamacheFWJrDuckerTBAlterations in neurological function in head-injured patients experiencing major episodes of sepsisNeurosurgery19821044684727099394
- RayelMGLandWBGutheilTGDementia as a risk factor for homicideJ Forensic Sci199944356556710408111
- HoffmanBFReversible neurosyphilis presenting as chronic maniaJ Clin Psychiatry19824383383397096276
- VarneyNRRobertsRJSpringerJAConnellSKWoodPSNeuropsychiatric sequelae of cerebral malaria in Vietnam veteransJ Nerv Ment Dis1997185116957039368547
- SowunmiASPsychosis after cerebral malaria in childrenJ Natl Med Assoc19938596956968120932
- BransfieldRCDid Infections Caused by World War I Contribute to Causing World War II?Contagion Live152018 Available from: http://www.contagionlive.com/news/did-infections-caused-by-world-war-i-contribute-to-causing-world-war-iiAccessed January 6, 2018
- SobinAOzerMMental disorders in acute encephalitisJ Mt Sinai Hosp1966337382
- FlegrJHrdyIInfluence of chronic toxoplasmosis on some human personality factorsFolia Parasitol (Praha)1994422122126
- FlegrJZitkovaSKodymPFryntaDInduction of changes in human behaviour by the parasitic protozoan Toxoplasma gondiiParasitology1996113Pt 149548710414
- PiekarskiGBehavioral alterations caused by parasitic infection in case of latent toxoplasma infectionZentralbl Bakteriol Mikrobiol Hgy [A]19812503403406
- CaroffSMannSGliattoMSullivanKCampbellEPsychiatric manifestations of acute viral encephalitisPsychiatr Ann200131193204
- SchlesingerLBSexual Murder: Catathymic and Compulsive HomicidesBoca Raton, FLCRC Press2004
- TselisABoossJBehavioral consequences of infections of the central nervous system: with emphasis on viral infectionsJ Am Acad Psychiatry Law200331328929814584527
- RayelMGLandWBGutheilTGDementia as a risk factor for homicideJ Forensic Sci199944356556710408111
- BachetMThe concept of encephaloses criminogenic (criminogenic encephalosis)Am J Orthopsychiatry19512179479914885387
- CoccaroEFLeeRGroerMWCanACoussons-ReadMPostolacheTTToxoplasma gondii infection: relationship with aggression in psychiatric subjectsJ Clin Psychiatry201677333434127046307
- ZimmerCParasite Rex: Inside the Bizarre World of Nature’s Most Dangerous Creatures New Ed EditionNew York, NYAtria Publishing Group2000
- SergievVPChange of host’s behavior including man under the influence of parasitesZh Mikrobiol Epidemiol Immunobiol2010310811420734729
- WhitfieldJWorm turns fish antisocialNature200079 Available from: http://www.nature.com/news/1998/020708/full/news020708-3.htmlAccessed October 21, 2017
- WinklerWGSchneiderNJJenningsWLExperimental rabies infection in wild rodentsJ Wildl Dis197281991035007906
- BarnardCJBehnkeJMSewellJEnvironmental enrichment, immunocompetence, and resistance to Babesia microti in male micePhysiol Behav1996605122312318916175
- BirkenheuerAJCorreaMTLevyMGBreitschwerdtEBGeographic distribution of babesiosis among dogs in the United States and association with dog bites: 150 cases (2000–2003)J Am Vet Med Assoc2005227694294716190594
- MitchellCDog aggression link-deer tick Lyme disease: dogs that are too aggressive to peopleLeerburg Webboard2007 Available from: http://leerburg.com/webboard/thread.php?topic_id=20140Accessed October 16, 2017
- GoswaniNTour of Duty Ends for DogBennington Banner20061128 Available from: http://www.benningtonbanner.com/stories/tour-of-duty-ends-for-dog,257240Accessed October 16, 2017
- BradleyJMMascarelliPETrullCLMaggiRGBreitschwerdtEBBartonella henselae infections in an owner and two Papillon dogs exposed to tropical rat mites (Ornithonyssus bacoti)Vector Borne Zoonotic Dis2014141070370925325313
- BishopBLCherryNAHegartyBCBreitschwerdtEBEnrichment blood culture isolation of Bartonella henselae from horses with chronic circulatory, musculoskeletal and/or neurologic deficitsAdv Biotech Micro201745
- CBSNews CBS/APChimp Shot Dead After Attacking Woman2009217 Available from: www.cbsnews.com/news/chimp-shot-dead-after-attacking-womanAccessed October 16, 2017
- ChristoffersenJEaston RobbPHuge chimp shot dead after mauling woman in ConnAssociated Press2172007 Available from: https://www.nhregister.com/news/article/Huge-chimp-shot-dead-after-mauling-woman-11635518.phpAccessed October 16, 2017
- WinslowJTHastingsNCarterCSHarbaughCRInselTRA role for central vasopressin in pair bonding in monogamous prairie volesNature199336564465455488413608
- TabbaaMPaedaeBLiuYWangZNeuropeptide regulation of social attachment: the prairie vole modelCompr Physiol2016718110428135000
- MacLeanELGesquiereLRGruenMEShermanBLMartinWLCarterCSEndogenous oxytocin, vasopressin, and aggression in domestic dogsFront Psychol20178161327
- HeinrichsMDomesGNeuropeptides and social behaviour: effects of oxytocin and vasopressin in humansProg Brain Res200817033735018655894
- KeverneEBKendrickKMMaternal behaviour in sheep and its neuroendocrine regulationActa Paediatr Suppl199439747567981474
- SchmelkinCPlessowFThomasJJLow oxytocin levels are related to alexithymia in anorexia nervosaInt J Eat Disord201750111332133829044580
- NormanMUMoriartyTJDresserARMillenBKubesPChaconasGMolecular mechanisms involved in vascular interactions of the Lyme disease pathogen in a living hostPLoS Pathog2008410e100016918833295
- MoriartyTJNormanMUColarussoPBankheadTKubesPChaconasGReal-time high resolution 3D imaging of the Lyme disease spirochete adhering to and escaping from the vasculature of a living hostPLoS Pathog200846e100009018566656
- KandelERSchwartzJHJessellTMPrinciples of Neural Science4th edNew YorkMcGraw-Hill Health Professions Division2000
- RheeHCameronDJLyme disease and pediatric autoimmune neuropsychiatric disorders associated with streptococcal infections (PANDAS): an overviewIn J Gen Med20125163174
- BarnettEMJacobsenGEvansGCassellMPerlmanSHerpes simplex encephalitis in the temporal cortex and limbic system after trigeminal nerve inoculationJ Infect Dis199416947827868133092
- JohnsonLWilcoxSMankoffJStrickerRBSeverity of chronic Lyme disease compared to other chronic conditions: a quality of life surveyPeerJ20142e32224749006
- SperlingJMiddelveenMKleinDSperlingFEvolving perspectives on Lyme borreliosis in CanadaOpen Neurol J201269410323091570
- LogigianELKaplanRFSteereACChronic neurologic manifestations of Lyme diseaseN Engl J Med199032321143814442172819
- HarveyRMisselbeckWUpholdRCat-scratch disease: an unusual cause of combative behaviorAm J Emerg Med1991952531985652
- DeeJEAx attacker using Lyme disease as defense case intensifies debate over ailment’s effects on brainCourant1999117
- FallonBANieldsJABurrascanoJJLiegnerKDelBeneDLiebowitzMRThe neuropsychiatric manifestations of Lyme borreliosisPsychiatr Q1992631951171438607
- SherrVTLetter to EditorSpotlight on LymeLyme Alliance Inc61998Concord, MI, USA
- BransfieldRCAggression and Lyme diseaseSpotlight19986 Available from: http://www.thedogplace.org/health/aggression-lyme-disease-1608-bansfield-md.aspAccessed October 21, 2017
- Staff“I fear for my friends’ and for my family’s safety”: Palin wins restraining order against teenage stalker (and his dad)Daily Mail20121212 Available from: http://www.dailymail.co.uk/news/article-1385553/Sarah-Palin-wins-restraining-order-teenage-stalker-Shawn-Christy-dad.html#ixzz4wAYLzGSTAccessed October 21, 2017
- HowellTDepraved’ mom gets five yearsNew Jersey Herald2009416 Available from: http://www.njherald.com/article/20090416/ARTICLE/304169997#Accessed October 21, 2017
- CutroniLTusten resident surrenders after shooting at policeThe River Reporter200622 Available from: http://www.riverreporter.com/issues/06-02-02/news-tusten.htmlAccessed October 21, 2017
- GreensteinTDown for the countChicago Tribune2000213 Available from: http://articles.chicagotribune.com/2000-02-13/sports/0002130275_1_casino-industry-art-collection-afterglow/2Accessed October 21, 2017
- FallonBDSchwartzenbergMBransfieldRLate stage neuropsychiatric Lyme borreliosisPsychosomatics19953632953007638317
- BransfieldRCThe Many Faces of Lyme: Neuropsychiatric Lyme Disease Case PresentationsPaper presented at: Neuropsychiatric Lyme Disease Symposium, 149th Annual MeetingAmerican Psychiatric AssociationMay 9, 1996New York, NY
- BransfieldRCDiagnosis, treatment, and prevention of Lyme diseaseJAMA1998280121049 Author reply 1051
- BransfieldRCFallonBARaxlenBDSheplerLTSherrVTA modest proposalPsychiatric News199833:181816
- BransfieldRCFallonBAMicrobes and Mental Illness, Neuropsychiatric Features of Lyme DiseasePapers presented at: Microbes and Mental Illness Symposium, American Psychiatric Association Institute on Psychiatric Services MeetingOctober 25, 2000Philadelphia, PA
- BransfieldRLyme neuroborreliosis and aggressionPaper presented at: 14th International Scientific Conference on Lyme Disease and Other Tick-Borne DisorderApril 22; 2001Hartford, CT Available from: https://sites.google.com/site/marylandlyme/symptoms-information/mental-health-issues/lyme-neuroborreliosis-agression-dr-bransfieldAccessed October 21, 2017
- BransfieldRCPosttraumatic stress disorder and infectious encephalopathiesSpotlight2001Nov-Dec Available from: http://www.mentalhealthandillness.com/Articles/PosttraumaticStressDisorder.htmAccessed October 21, 2017
- BärKJJochumTHägerFMeissnerWSauerHPainful hallucinations and somatic delusions in a patient with the possible diagnosis of neuroborreliosisClin J Pain200521436236315951656
- SchallerJLBurklandGALanghoffPJDo bartonella infections cause agitation, panic disorder, and treatment-resistant depression?MedGenMed20079354
- BransfieldRCan infections and immune reactions to them cause violent behavior?Paper presented at: International Lyme and Associated Diseases Society Neurological/Psychiatric Lyme Disease ConferenceOctober 29, 2011Toronto, Canada Available from: https://www.youtube.com/watch?v=UI3Yap1KgmoAccessed October 19, 2017
- BransfieldRCCan infections and immune reactions to them cause violent behavior?Neurol Psychiatry Brain Res201218342
- BransfieldRCThe role of brain mechanisms in intrusive symptoms and post-traumatic stress disordersPaper presented at: International Lyme and Associated Diseases Annual ConferenceOctober 10, 2014Washington, DC
- BransfieldRCChronic infections as aetiological factors in psychiatric disordersPaper presented at: 21st Annual International Integrative Medicine ConferenceJuly 19, 2015Melbourne, Australia
- BreitschwerdtEBMascarelliPESchweickertLAHallucinations, sensory neuropathy, and peripheral visual deficits in a young woman infected with Bartonella koehleraeJ Clin Microbiol20114993415341721734026
- MunirAAadilMRehan KhanASuicidal and homicidal tendencies after Lyme disease: an ignored problemNeuropsychiatr Dis Treat2017132069207128814875
- BransfieldRCResponse to Letter to Editor Suicidal and homicidal tendencies after Lyme disease: an ignored problemNeuropsychiatr Dis Treat2017132071
- FinkPJAnother great imposterPhiladelphia Medicine19996
- FinkPJAnother great imposterClinical Psychiatry News19993
- LanghoffPJRecognizing the face of rage in tick-borne illnessPublic Health Alert20072849 Available from: http://www.betterhealthguy.com/images/stories/PDF/PHA/2007_08.pdfAccessed October 20, 2017
- BransfieldRCan infections and immune reactions to them cause violent behavior?Paper presented at: International Lyme and Associated Diseases Society Neurological/Psychiatric Lyme Disease ConferenceOctober 29, 2011Toronto, Canada Available from: https://www.youtube.com/watch?v=UI3Yap1KgmoAccessed October 19, 2017
- BransfieldRCAntimicrobials in psychiatryPsychiatric Times19997
- SingleyPLawyer: Southbury strangling sparked by Lyme disease or drugsRepublican-American200629 Available from: http://www.lymeblog.com/modules.php?name=News&file=article&sid=390Accessed October 20, 2017
- Appellate Court of ConnecticutGregg Madigosky v. Commissioner of Correction (AC 38962) Decided: 2017 April 11 Available from: http://caselaw.findlaw.com/ct-court-of-appeals/1855564.htmlAccessed October 20, 2017
- WeirRLibrarian savagely beaten while sleeping in her West Islip home. Son held in slay of MomNew York Daily News20061010 Available from: http://www.nydailynews.com/archives/boroughs/librarian-savagely-beaten-sleeping-west-islip-home-son-held-slay-mom-article-1.645217Accessed October 20, 2017
- MillerALTwo dead in murder-suicide had advanced Lyme diseaseOcala Star Banner2010710 Available from: http://www.ocala.com/article/LK/20100710/News/604190440/OS/Accessed October 20, 2017
- McQuistonJTMan Pleads Not Guilty in Slaying on Shelter IThe New York Times200857 Available from: http://www.nytimes.com/1998/05/07/nyregion/man-pleads-not-guilty-in-slaying-on-shelter-i.html?mcubz=3Accessed October 20, 2017
- McQuistonJTFear, Not Anger, Led to Shelter Island Slaying, Defense SaysThe New York Times2000523 Available from: http://www.nytimes.com/2000/05/23/nyregion/fear-not-anger-led-to-shelter-island-slaying-defense-says.html?mcubz=3Accessed October 20, 2017
- WackerTLyme made him do it? Lyme psychosis eyed as defense in S.I. ShootingThe Suffolk Times1998514
- BernsteinJDid Adam Lanza have Lyme disease?Counterpunch2013111 Available from: https://www.counterpunch.org/2013/01/11/did-adam-lanza-have-lyme-disease/Accessed October 20, 2017
- Abrahams WilsonAUnder Our Skin 2: Emergence Available from: http://underourskin.com/emergence/Accessed October 20, 2017
- AltimariDFull Report Confirms No Drugs, Alcohol in Lanza’s SystemThe Hartford Courant10292013 Available from: http://articles.courant.com/2013-10-29/news/hc-sandy-hook-lanza-toxicology-20131029_1_peter-lanza-adam-lanza-toxicology-reportAccessed October 20, 2017
- StaffThe tick defenseNew Jersey Law Journal1999155NJLJ13313
- FritzMForeboding at Ground Zero of Lyme DiseaseLA Times199867 Available from: http://articles.latimes.com/1998/jun/07/news/mn-57486/2Accessed October 21, 2017
- VivianoJDefense blames Lyme disease in ax attackRegister2001126 Available from: https://groups.google.com/forum/#!topic/sci.med.diseases.lyme/9Q3813YOx70Accessed October 20, 2017
- StaffWoman pleads guilty to fatal fireTimes Free Press20101211 Available from: http://www.timesfreepress.com/news/news/story/2010/dec/11/woman-pleads-guilty-to-fatal-fire/36780/Accessed October 20, 2017
- StaffNY follow-up letter, Dr. Bransfield connects Lyme to opioid crisis 2017 Sept 6LymeDisease.org Available from: https://www.lymedisease.org/bransfield-lyme-opioid-crisis/?utm_source=sept+9-sleeper&utm_campaign=sept+5-sleeper+cells&utm_medium=emailAccessed October 20, 2017
- SheaLJThe Neuropsychology of Lyme DiseasePaper presented at: Challenges and Controversy in Lyme Disease and Tick-Borne Illness Care SymposiumNovember 9, 2013Boston, MA
- BlairRJThe amygdala and ventromedial prefrontal cortex: functional contributions and dysfunction in psychopathyPhilos Trans R Soc Lond B Biol Sci200836315032557256518434283
- BlairRJThe Neurobiology of Impulsive AggressionJ Child Adolesc Psychopharmacol20162614926465707
- LeeRArfanakisKEviaAMFanningJKeedySCoccaroEFWhite matter integrity reductions in intermittent explosive disorderNeuropsychopharmacology201641112697270327206265
- ShrabergDWeisbergLThe Klüver-Bucy syndrome in manJ Nerv Ment Dis19781662130134627885
- MoranaHCStoneMHAbdalla-FilhoETranstornos de person-alidade, psicopatia e serial killers. [Personality disorders, psychopathy and serial killers]Rev Bras Psiquiatr20062827479 Portuguese
- JhaKKSinghSKKumarPAroraCDPartial Kluver-Bucy syndrome secondary to tubercular meningitisBMJ Case Rep2016162016
- OumerzoukJMouhadiKKHssainiYKlüver-Bucy syndrome complicating herpes meningoencephalitis in a pregnant womanPresse Med2014437–887187424703732
- EikmeierGForquignonIHonigHKlüver-Bucy syndrome after herpes simplex encephalitisPsychiatr Prax201340739239323846508
- BransfieldRCWulfmanJSHarveyWTUsmanAIThe association between tick-borne infections, Lyme borreliosis and autism spectrum disordersMed Hypotheses200870596797417980971
- DaxboeckFMycoplasma pneumoniae central nervous system infectionsCurr Opin Neurol200619437437816914976
- AuvichayapatNAuvichayapatPWatanatornJThamarojJJitpimolmardSKluver-Bucy syndrome after mycoplasmal bronchitisEpilepsy Behav20068132032216356778
- PatelRJhaSYadavRKPleomorphism of the clinical manifestations of neurocysticercosisTrans R Soc Trop Med Hyg2006100213414116214195
- De TiègeXDe LaetCMazoinNPostinfectious immune-mediated encephalitis after pediatric herpes simplex encephalitisBrain Dev200527430430715862196
- LocatelliCVergineGCiambraRKluver Bucy syndrome and central diabetes insipidus: two uncommon complications of herpes simplex encephalitisPediatr Med Chir200325644244615279370
- ManciniJChabrolBLivetMOPinsardNRésultat de l’encéphalite herpétique. À propos de 10 cas. [Outcome of herpetic encephalitis. Apropos of 10 cases]Ann Pediatr (Paris)1991383143149 French1710096
- HartRPKwentusJAFrazierRBHormelTLNatural history of Klüver-Bucy syndrome after treated herpes encephalitisSouth Med J19867911137613783022394
- WebsterJLambertonPHDonnellyCTorreyEParasites as causative agents of human affective disorders? The impact of anti-psychotic, mood-stabilizer and anti-parasite medication on Toxoplasma gondii’s ability to alter host behaviourProc Roy Soc B Biol Sc2006273158910231030
- CarrollJELowCAPratherAANegative affective responses to a speech task predict changes in interleukin (IL)-6Brain Behav Immun20112523223820888901
- WestlingSAhrénBTräskman-BendzLBrundinLIncreased IL-1β reactivity upon a glucose challenge in patients with deliberate self-harmActa Psychiatr Scand2011124430130621762115
- SergievVPChange of host’s behavior including man under the influence of parasitesZh Mikrobiol Epidemiol Immunobiol20103108114 Russian20734729
- ConstantACasteraLDantzerRMood alterations during interferon-alfa therapy in patients with chronic hepatitis C: evidence for an overlap between manic/hypomanic and depressive symptomsJ Clin Psychiatry20056681050105716086622
- LotrichFESearsBMcNamaraRKAnger induced by interferon-alpha is moderated by ratio of arachidonic acid to omega-3 fatty acidsJ Psychosom Res201375547548324182638
- Chantal HenryCLaurent CastéraLDemotes-MainardJHepatitis C and interferon: Watch for hostility, impulsivityCurr Psychiatr2006587177
- KleinsasserBJMisraLKBhataraVSSanchezJDRisperidone in the treatment of choreiform movements and aggressiveness in a child with “PANDAS”S D J Med199952934534710522469
- TillmanJARaffGJParaneoplastic limbic encephalitis cured with resection of an adnexal massJSLS2009133433435
- KhanNWieserHGLimbic encephalitis: a case reportEpilepsy Res19941721751818194513
- VenâncioPBritoMJPereiraGVieiraJPAnti-N-methyl-D-aspartate receptor encephalitis with positive serum antithyroid antibodies, IgM antibodies against mycoplasma pneumoniae and human herpesvirus 7 PCR in the CSFPediatr Infect Dis J201433888288325222311
- FrohmanEMFrohmanTCMoreaultAMAcquired sexual paraphilia in patients with multiple sclerosisArch Neurol20025961006101012056938
- BransfieldRCA structured clinical interview when neuropsychiatric Lyme disease is a possibilityPaper presented at: LDF’s 10th Annual International Scientific Conference on Lyme Borrelosis and Other Tick-borne DisordersApril 28, 1997Bethesda, MD
- CiteraMFreemanPRHorowitzRIEmpirical validation of the Horowitz Multiple Systemic Infectious Disease Syndrome Questionnaire for suspected Lyme diseaseInt J Gen Med20171024927328919803
- AHRQNational Guideline Clearinghouse2016 Available from: https://www.guideline.govAccessed April 30, 2017
- CameronDJJohnsonLBMaloneyELEvidence assessments and guideline recommendations in Lyme disease: the clinical management of known tick bites, erythema migrans rashes and persistent diseaseExpert Rev Anti Infect Ther20141291103113525077519
- The American Psychiatric Association practice guidelines for the psychiatric evaluation of adultsThird edition2016 Available from: http://psychiatryonline.org/doi/pdf/10.1176/appi.books.9780890426760Accessed March 3, 2017
- U.S. Centers for Disease Control and PreventionHow many people get Lyme disease?2015 Available from: https://www.cdc.gov/lyme/stats/humancases.htmlAccessed October 20, 2017
- GlistaKMoranDMurder-suicide of Durham couple shakes communityHartford Courant2015 Available from: http://www.courant.com/breaking-news/hc-durham-murder-suicide-0319-20150318-story.htmlAccessed October 20, 2017
- EnchassiNJTribune Media Wire and CNN Wire. DA: Pennsylvania dad of heart-transplant toddler killed family, self2016 Available from http://kfor.com/2016/08/15/pennsylvania-dad-of-heart-transplant-toddler-killed-family-self-da/Accessed October 21, 2017
- SalvatorePBhuvaneswarCTohenMKhalsaHMMagginiCBaldessariniRJCapgras’ syndrome in first-episode psychotic disordersPsychopathology201447426126924516070
- GoodmanRAMercyJALoyaFAlcohol use and interpersonal violence: alcohol detected in homicide victimsAm J Public Health19867621441493946695
- FrankCOn the reception of the concept of the death drive in Germany: expressing and resisting an ‘evil principle’?Int J Psychoanal201596242544425220224