Abstract
Purpose
The prescribing of oral chemotherapy agents has introduced the new challenge of ensuring patients’ adherence to therapy. Aspects of a close patient–doctor relationship are reported to be correlated with adherence to oral anticancer drugs, but data on capecitabine are scarce.
Patients and methods
Sixty-four outpatients with a diagnosis of cancer and prescribed capecitabine were recruited from a German Comprehensive Cancer Center. We used the Patient–Doctor Relationship Questionnaire (PDRQ-9), the Medical Adherence Rating Scale (MARS), the Beliefs about Medicines Questionnaire (BMQ), and the Satisfaction with Information about Medicines Scale (SIMS) to assess patients’ perceptions and behavior. Medical data were extracted from the charts.
Results
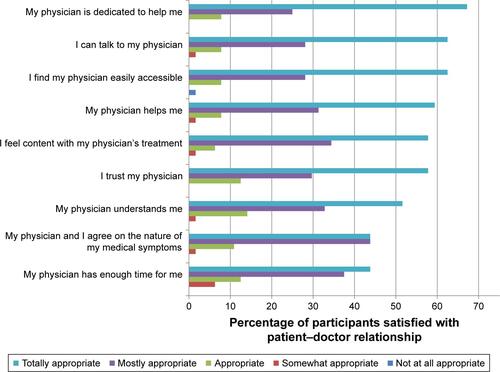
Non-adherence was reported by 20% of the 64 participants. The perceived quality of the patient–doctor relationship was high in general, but it did not emerge as a predictor of adherence in our survey (odds ratio [OR]=0.915, P=0.162, 95% CI=0.808–1.036). However, beliefs about medicine (OR=1.268, P<0.002; 95% CI=1.090–1.475) as well as satisfaction with information about medicine (OR=1.252, P<0.040, 95% CI=1.010–1.551) were predictors of adherence and the quality of the patient–doctor relationship was correlated with both variables (r=0.373, P=0.002 for SIMS sum score; r=0.263, P=0.036 for BMQ necessity/concern difference). Overall, adherence to capecitabine was high with a conviction that the therapy is necessary. However, concerns were expressed regarding the long-term effect of capecitabine use. Patients have unmet information needs regarding interactions of capecitabine with other medicines and the impairment of their intimate life.
Conclusions
In order to ensure adherence to capecitabine, our results seem to encourage the default use of modern and perhaps more impersonal means of information brokerage (eg, email, internet). However, the contents of some of patients’ informational needs as well as the associations of patients’ beliefs and satisfaction about the information received suggest a benefit from a trustful patient–doctor relationship.
Supplementary materials
Figure S2 Participant reported necessities of capecitabine therapy (Beliefs about Medicines Questionnaire – Necessity Scale, n=64).
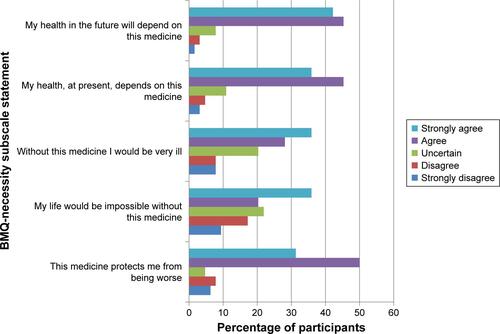
Figure S3 Participant reported concerns of capecitabine therapy (Beliefs about Medicines Questionnaire – Concerns Scale, n=64).
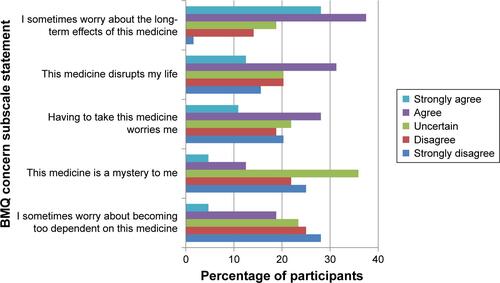
Table S1 Single items of the Patient–Doctor Relationship Questionnaire (PDRQ-9, n=64)
Table S2 Self-reported adherence to capecitabine (n=64)
Acknowledgments
E Göbel, J Haas, E Hupp, B Schoettker, and H Reinel provided and cared for study patients. This publication was funded by the German Research Foundation (DFG) and the University of Wuerzburg in the funding programme Open Access Publishing.
Author contributions
All authors contributed toward data analysis, drafting and critically revising the paper and agree to be accountable for all aspects of the work.
Disclosure
The authors report no conflicts of interest in this work.