Abstract
Purpose: To report the diagnosis of a case of recurrent iris fungal granuloma presumed to be an iris tuberculoma in a 10-year-old girl.
Design: Case report
Methods: Retrospective medical chart review including serological and microbiological investigative results
Results: A patient presented with iris mass associated with anterior uveitis. Serological tests were positive for IgM of tuberculosis. Steroids treatment was initiated in conjunction with anti-tuberculosis treatment. The course showed remissions and exacerbation. Fine needle aspiration biopsy (FNAB) of the granuloma proved the etiologic agent to be Aspergillus fumigates.
Conclusion: Fine needle aspiration biopsy should be used in the diagnosis of iris masses associated with recurrent inflammation
Keywords::
CASE REPORT
A 10-year-old girl presented with painless blurring of vision of 2 weeks duration in the left eye. She had no relevant ocular or systemic history.
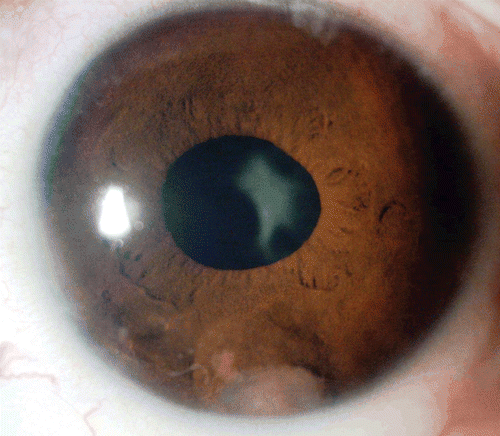
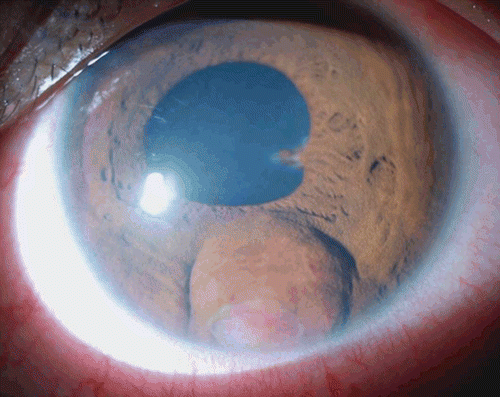
Visual acuity was 6/6 in the right eye and 6/12 in the left. Intraocular pressure was 16 mmHg in both eyes. Slit-lamp examination of the right eye was normal. Left eye showed a spherical bulge at the iris root at 6 o’clock caused by a mass beneath the iris that was visible through an area of overlying iris atrophy. The mass appeared white and vascularized, and adherent to the corneal endothelium. It was associated with keratic precipitates, 2+ aqueous flare and cells, and posterior synaechiae at 3 o’clock (). Posterior subcapsular cataract and vitreous cellular reaction were observed. Bilateral funduscopy was normal.
FIGURE 1 Slit lamp photo shows an iris bulge inferior to the pupil, with an area of iris atrophy showing a white vascularized mass underneath. There is papillary posterior synechia at 3 o’clock meridian.
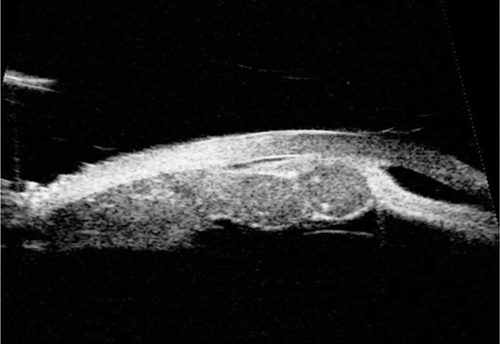
Ultrasound biomicroscopy showed a bilobed moderately echogenic solid lesion, arising from the undersurface of the iris and involves the pars plicata. There were 2 hyperechogenic dots within one lobe. The anterior chamber (AC) appeared narrowed by the bulging iris root and the iris appeared compressed and thinned out by the mass ().
FIGURE 2 Ultrasound Biomicroscopy image shows a bilobed moderately echogenic solid lesion, arising from the undersurface of the iris and involves the pars plicata. There were 2 hyperechogenic dots within one lobe (Arrow). Iris appears thinned out over the mass.
Because of the marked inflammation, a neoplastic origin was unlikely. The findings were suggestive of an inflammatory granuloma. Laboratory investigations for granulomatous uveitis were negative except for a positive IgM for tuberculosis which prompted our physician to start anti-tuberculosis therapy. Treatment also included oral and topical steroids, and cycloplegics.
Two weeks later, vision of left eye improved to 6/9, iris mass regressed, AC reaction reduced. Subsequently, cycloplegics, and steroids were gradually tapered.
The patient was lost to follow-up and presented 8 months later with redness in the same eye. She was still on anti-tuberculosis treatment. Examination demonstrated a residual mass with recurrence of aqueous and vitreous cells. AC aspiration was negative for bacterial and fungal growth. Patient responded again to steroids and cycloplegics.
Four months later, the eye was quiet but there was a residue of the mass. Thus, a fine needle aspiration biopsy of the iris mass was performed. Potassium Hydroxide (KOH) staining showed a few septate fungal filaments with budding diagnostic of Aspergillus fumigatus (). Polymerase Chain Reaction confirmed presence of panfungal genome. Oral voriconazole (150 mg/day) and topical fluconazole were administered. However, vision dropped to 6/60 two weeks later. Thus, intravitreal Voriconazole (50 μg in 0.1 ml) was delivered which improved vision to 6/18. Eventually, inflammation subsided and the mass regressed ().
DISCUSSION
The mass in this patient was initially diagnosed as tuberculoma based on positive serological IgM for tuberculosis and negative aqueous analysis for any bacterial or fungal growth; contrary to previous reports by Agarwal and Jain, in which the anterior chamber fluid tap showed a positive growth of Aspergillus. This made the diagnosis of a fungal granuloma more straightforward.Citation1,Citation2 However, in our case, the diagnostic dilemma was compounded by the positive serological tests for tuberculosis, which led to the erroneous initial diagnosis of iris tuberculoma. The general immune status may influence fungal growth. It is questionable here whether or not steroid treatment has temporarily improved the iritis or unfavorably influenced the local immunity, causing recurrence of inflammation of fungal origin.Citation3,Citation4,Citation5
The patient in previous report by Agarwal et al. was finally diagnosed with Aspergillus terreus, which responded to antibiotic treatment, versus to our case that was diagnosed as Aspergillus fumigatus that required antifungal therapy. The patient in Agarwal’s report had history of ocular trauma that made him stipulate that it could have led to break down of blood-aqueous barrier, and spread of endogenous infection to iris. The patient in Jain’s report did not have history or evidence of tuberculosis, which was the cause of initial misleading diagnosis of our case.Citation1,Citation2
Our paper presents an interesting ultrasound biomicroscopy picture of the lesion, with peculiar echogenic criteria. However, the patient in Agarwal’s report did not undergo the ultrasound biomicroscopy, and the patient in Jain’s underwent an ultrasonography by immersion technique which is much less demonstrative.Citation1,Citation2
The presence of evidence of an associated systemic granulomatous inflammatory diseases, such as tuberculosis or sarcoidosis, may bias the clinician to misdiagnose a coexisting iris granuloma to be of similar etiology. Thus, this case highlights the significance of diagnostic fine needle aspiration biopsy in cases of iris masses, since serological tests and aqueous analysis were initially misleading.
Declaration of interest: No conflicting relationship exists for any author.
REFERENCES
- Agarwal M., Biswas J., Mathur U., Sijwali M.S., Singh AK. Aspergillus iris granuloma in a young male: A case report with review of literature. Indian J Ophthalmol 2007;55,73–74.
- Jain V, Dabir S, Shome D, Dadu T, Natarajan S. Aspergillus iris granuloma: a case report with review of literature. Surv Ophthalmol. 2009;54(2):286–91.
- Whitcup W.S. Bacterial and fungal diseases. In: Nussenblatt R.B, Whitcup W.S. Uveitis Fundamentals and clinical practice. 4th ed. China: Mosby Elsevier, 2010, 137–139.
- Hariprasad S.M., Mieler W.F., Lin T.K., Sponsel W.E., Graybill J.R. Voriconazole in the treatment of fungal eye infections: a review of current literature. Br J Ophthalmol 2008;92:871–878.
- Thompson MJ, Albert DM. Ocular Tuberculosis. Arch Ophthalmol. 2005;123:844–8.