Figures & data
Figure 1. The role of platelets after vascular injury.[Citation13–Citation16] After plaque rupture, TF is released from endothelial cells and platelets are activated by collagen and vWF. TF is converted to thrombin, which activates platelets and facilitates formation of a fibrin meshwork. Activated platelets produce ADP and TXA2, which in turn augment platelet activation and recruit additional platelets to the area. Activated platelets also produce inflammatory signals that recruit leukocytes to the area. The leukocytes amplify platelet activation signals and cross-link to fibrin, facilitating clot formation. ADP: adenosine diphosphate; TF: tissue factor; TXA2: thromboxane A2; vWF: von Willebrand factor.
![Figure 1. The role of platelets after vascular injury.[Citation13–Citation16] After plaque rupture, TF is released from endothelial cells and platelets are activated by collagen and vWF. TF is converted to thrombin, which activates platelets and facilitates formation of a fibrin meshwork. Activated platelets produce ADP and TXA2, which in turn augment platelet activation and recruit additional platelets to the area. Activated platelets also produce inflammatory signals that recruit leukocytes to the area. The leukocytes amplify platelet activation signals and cross-link to fibrin, facilitating clot formation. ADP: adenosine diphosphate; TF: tissue factor; TXA2: thromboxane A2; vWF: von Willebrand factor.](/cms/asset/ec9c22d6-5b0b-4093-b215-bf476a6740e0/ipgm_a_1131106_f0001_b.gif)
Figure 2. Mechanism of action of aspirin. Aspirin inhibits production of TXA2 by preventing the conversion of arachidonic acid to PGH2 by COX-1 and COX-2. COX, cyclooxygenase; PG, prostaglandin; TXA2, thromboxane A2.
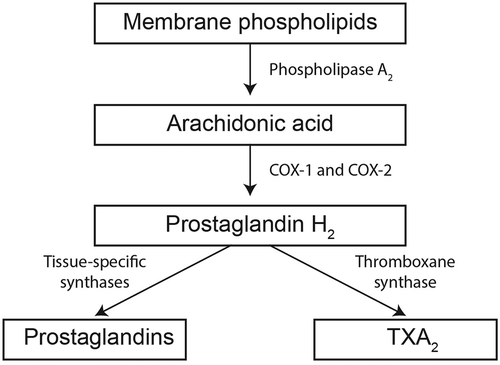
Figure 3. Antiplatelet effect of IR aspirin in healthy individuals.[Citation20,Citation29] Healthy male volunteers (n = 10) received a single dose of IR aspirin 20 mg orally (A). Vertical line represents time of aspirin administration. Serum TXB2 concentration (a surrogate marker of TXA2 production) in healthy volunteers (n = 50) who received non-enteric-coated aspirin 75 mg for 7 days (B). Serum TXB2 levels tended to increase 24 h after aspirin dosing, although this difference did not reach statistical significance. ASA: aspirin; IR: immediate release; TXA2: thromboxane A2; TXB2: thromboxane B2.
![Figure 3. Antiplatelet effect of IR aspirin in healthy individuals.[Citation20,Citation29] Healthy male volunteers (n = 10) received a single dose of IR aspirin 20 mg orally (A). Vertical line represents time of aspirin administration. Serum TXB2 concentration (a surrogate marker of TXA2 production) in healthy volunteers (n = 50) who received non-enteric-coated aspirin 75 mg for 7 days (B). Serum TXB2 levels tended to increase 24 h after aspirin dosing, although this difference did not reach statistical significance. ASA: aspirin; IR: immediate release; TXA2: thromboxane A2; TXB2: thromboxane B2.](/cms/asset/b3b941ab-eccb-4959-8239-73b732b9c550/ipgm_a_1131106_f0003_b.gif)
Figure 4. Risk of adverse cardiovascular outcomes in patients with diabetes who were receiving low-dose aspirin.[Citation34,Citation43–Citation50] Relative risk and 95% confidence interval with aspirin versus controls is provided for all studies except Stavrakis et al. [Citation45], for which the odds ratio versus controls is presented. CV: cardiovascular; MI: myocardial infarction.
![Figure 4. Risk of adverse cardiovascular outcomes in patients with diabetes who were receiving low-dose aspirin.[Citation34,Citation43–Citation50] Relative risk and 95% confidence interval with aspirin versus controls is provided for all studies except Stavrakis et al. [Citation45], for which the odds ratio versus controls is presented. CV: cardiovascular; MI: myocardial infarction.](/cms/asset/a5079d5c-be01-4382-a011-0b7888034608/ipgm_a_1131106_f0004_b.gif)
Figure 5. Relative risk of CV endpoints in patients with diabetes with and without comorbid CHD who received preventative aspirin therapy.[Citation46] Data from a meta-analysis of randomized controlled trials (n = 1 to 13 trials) that enrolled patients with diabetes alone or with diabetes and CHD who received aspirin (50–1300 mg/day) for prevention of CV events. CHD: coronary heart disease; CV: cardiovascular; MI: myocardial infarction.
![Figure 5. Relative risk of CV endpoints in patients with diabetes with and without comorbid CHD who received preventative aspirin therapy.[Citation46] Data from a meta-analysis of randomized controlled trials (n = 1 to 13 trials) that enrolled patients with diabetes alone or with diabetes and CHD who received aspirin (50–1300 mg/day) for prevention of CV events. CHD: coronary heart disease; CV: cardiovascular; MI: myocardial infarction.](/cms/asset/ce7c8ea7-117a-4b59-a60e-da9e7d0e7108/ipgm_a_1131106_f0005_b.gif)
Figure 6. Mechanisms underlying increased clot formation in patients with diabetes.[Citation17] Altered glucose metabolism and insulin signaling increase platelet activation, inflammation and vasoconstriction, all of which increase clot formation. PG: prostaglandin; VSMC: vascular smooth muscle cell.
![Figure 6. Mechanisms underlying increased clot formation in patients with diabetes.[Citation17] Altered glucose metabolism and insulin signaling increase platelet activation, inflammation and vasoconstriction, all of which increase clot formation. PG: prostaglandin; VSMC: vascular smooth muscle cell.](/cms/asset/d37bcebc-4d76-4ee0-865f-ba02d83d7f85/ipgm_a_1131106_f0006_b.gif)
