Figures & data
Table 1 Characteristics of included studies
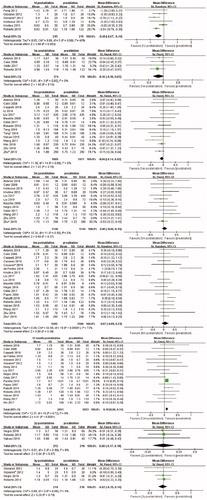
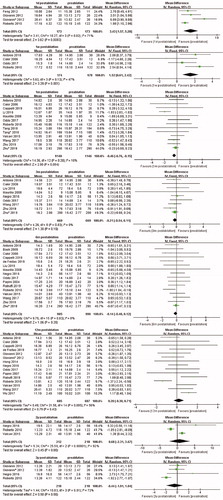
Table 2. New onset of thyroid abnormalities.
Table 3. Sensitivity analysis.
Table 4. Subgroup analysis of TSH level.
Table 5. Subgroup analysis of FT3 level.
Table 6. Subgroup analysis of FT4 level.