Figures & data
Table 1. Oligonucleotide primer sequences used in identification of APEC.
Table 2. Prevalence of histologically confirmed BCO in necropsied birds.
Table 3. Prevalence of histologically confirmed BCO at different ages in necropsied birds from longitudinally sampled flocks.
Table 4. Total bacteria isolated from all sites.
Table 5. Distribution of the virulence genes among the APEC isolates in the proximal end of the femur or tibia of the birds.
Table 6. Age distribution of bacterial isolates and histological detection inflammation in the proximal end of the femur or tibia of the birds.
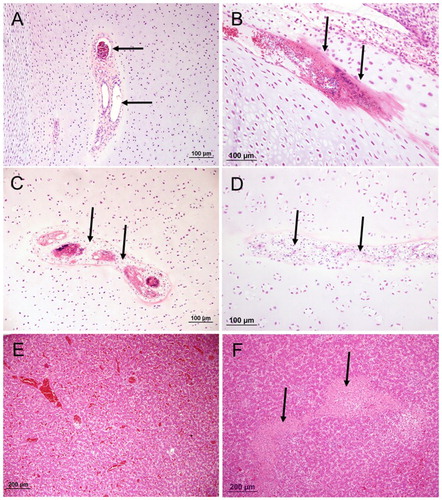
Figure 1. The proximal end of femur or tibiotarsus (haematoxylin and eosin) with different lesions. (A) an example of a typical healthy growth plate; (B), an example of a typical BCO inflammation within the epiphyseal growth plate (arrow); (C), non-artefactual separation at the hypertrophic zone of the growth plate. Note evidence of remodelling at the margins of the cleft (eosinophilic matrix, arrow) and cellular debris within the cleft (arrowheads); (D), large plug of retained cartilage extending down the diaphysis; (E), an example of a typical healthy thin synovium and (F), an example of fibrinoheterophilic synovitis with exudate in joint (arrow) and thickened synovium.
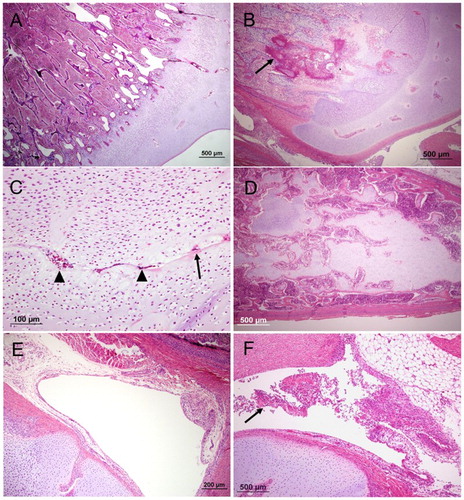
Figure 2. The proximal end and diaphysis of femur or tibiotarsus (haematoxylin and eosin) with different lesions; (A), normal vascular channel containing patent blood vessels (arrows); (B), early-stage vascular regression, cartilage channel displaying fibrin accumulation containing pyknotic nuclear debris (arrows); (C), mid-stage vascular regression; chondrocytic metaplasia of mesenchymal cells (arrows) surrounding degenerate vessels; (D), late-stage vascular regression. Effacement of channel by cartilage matrix; (E), normal liver tissue and (F), typical coalescing regions of parenchymal necrosis in a case of hepatitis (arrow).