Figures & data
Table 1. Baseline characteristic of included studies.
Figure 2. Results of cardiovascular events. (A) Forest plot showing the difference in cardiovascular events between sacubitril/valsartan and control group. (B) Funnel plot of cardiovascular events. Note: Berg et al. defined cardiovascular events as a composite of cardiovascular death or rehospitalization for heart failure [Citation12]; Chen et al. described cardiovascular events as rehospitalization for heart failure and all-cause death [Citation24]; Damman et al. Chang et al. Hsiao et al. Lee et al. and Tsutsui et al. described cardiovascular events as cardiovascular death or heart failure hospitalization [Citation15,Citation19,Citation21–23,Citation26]; Mc Causland et al. defined cardiovascular events as a composite of total (first and recurrent) hospitalizations for heart failure and death from cardiovascular causes; In Sheng et al.’s research, cardiovascular events were regarded as the rehospitalization of patients due to acute myocardial ischemia, HF, thromboembolic or hemorrhagic stroke, arrhythmia, and peripheral vascular disease [Citation20]; Niu et al. regarded cardiovascular events as hospitalization because of cardiovascular diseases [Citation14].
![Figure 2. Results of cardiovascular events. (A) Forest plot showing the difference in cardiovascular events between sacubitril/valsartan and control group. (B) Funnel plot of cardiovascular events. Note: Berg et al. defined cardiovascular events as a composite of cardiovascular death or rehospitalization for heart failure [Citation12]; Chen et al. described cardiovascular events as rehospitalization for heart failure and all-cause death [Citation24]; Damman et al. Chang et al. Hsiao et al. Lee et al. and Tsutsui et al. described cardiovascular events as cardiovascular death or heart failure hospitalization [Citation15,Citation19,Citation21–23,Citation26]; Mc Causland et al. defined cardiovascular events as a composite of total (first and recurrent) hospitalizations for heart failure and death from cardiovascular causes; In Sheng et al.’s research, cardiovascular events were regarded as the rehospitalization of patients due to acute myocardial ischemia, HF, thromboembolic or hemorrhagic stroke, arrhythmia, and peripheral vascular disease [Citation20]; Niu et al. regarded cardiovascular events as hospitalization because of cardiovascular diseases [Citation14].](/cms/asset/a6985d0c-fa5f-4b36-afeb-5fd8e8000f9b/irnf_a_2349135_f0002_c.jpg)
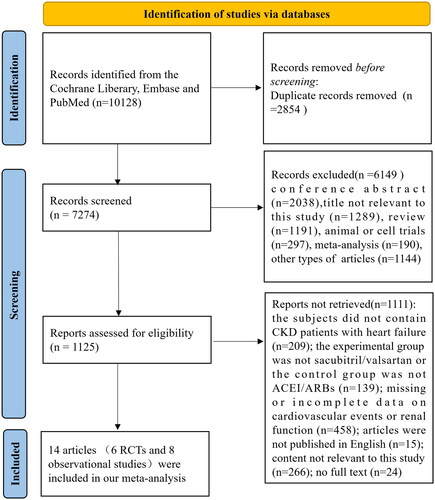
Figure 3. Results about cardiovascular events. (A) Forest plot about changes in Scr. (B) Forest plot regarding changes in eGFR. (C) Meta-analysis of the incidence of ESRD in CKD stages 3–5 patients with heart failure. *Berg et al. defined the change of Scr as an increase in serum creatinine of at least 0.5 mg/dL; **Mc Causland et al. were described the change of Scr as elevated serum creatinine ≥ 2.0 mg/dL; *** Tan et al. described the change of Scr as doubling of serum creatinine; ****Voors et al. defined the change of Scr as >0.3 mg/dL increase in creatinine in combination with an increase of more than 25% in serum creatinine between two time points. †In the Chen’s study, the PARADIGM-HF trial and the PARAGON-HF trial, eGFR level declined >50% from baseline; ††In the Berg et al.’s trial, eGFR level declined >25% from baseline; †††In the Tan’s study, eGFR level declined >30% or more from baseline.
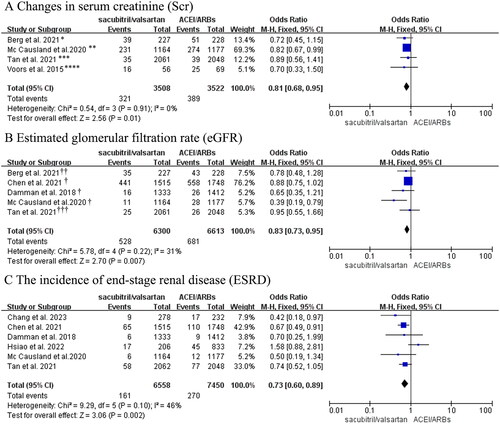
Figure 4. (A) Forest plot of the incidence of hyperkalemia. (B) Meta-analysis of the incidence of hypotension in CKD stages 3-5 patients with heart failure. (C) Forest plots of changes in blood pressure. *Hyperkalemia was defined as potassium > 5.5 mmol/L in these studies; ** Hyperkalemia was defined as potassium > 6mmol/L in Hsiao’s study. †Berg et al. regarded hypotension as symptomatic hypotension; ††Hypotension in the Mc Causland et al.’s trial was regarded as SBP < 100 mmHg.
Supplemental Material
Download PDF (443.8 KB)Data availability statement
All data generated or analyzed during this study are included in this article or Supplementary files.