Figures & data
Figure 1 Example of severely angulated and short neck, which represents a significant limitation for endovascular stent-graft repairs for AAAs.
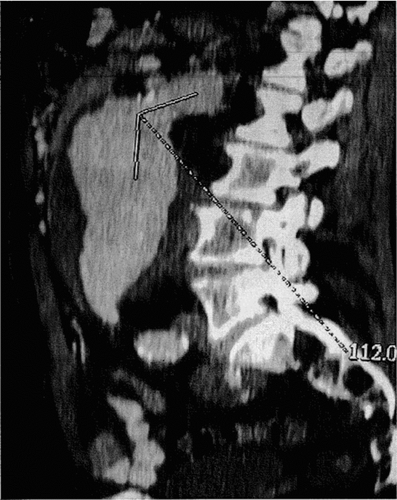
Figure 2 Weft-knitted polyester arterial prosthesis specifically designed to create the aneurysm, holding external gold marks both proximally and distally (arrows) (A) and implanted as substitute of the infra-renal abdominal aorta (B).
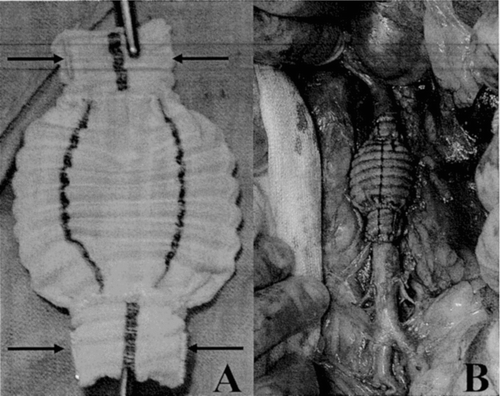
Figure 3 Weft-knitted polyester employed in the construction of the stent-graft, crimped in Module A with a distal suture to create a constriction to firmly hold the distal module (A1) and non crimped in Module B (A2); this polyester knit holds characteristics of dimensionnal adaptability without structural change as evidenced in X-rays (Faxitron) (B).
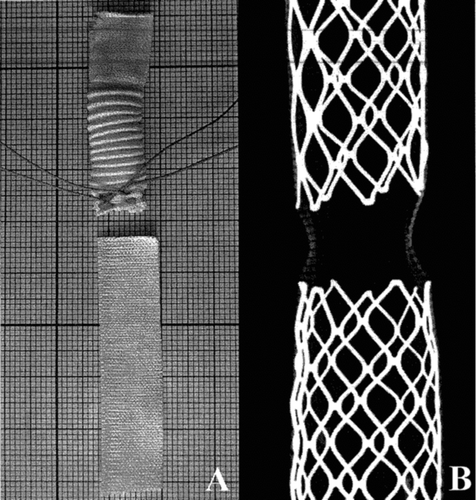
Figure 4 Module A (Seta Rack) still inserted in its cartridge. The proximal half of the Palmaz-type stainless steel is uncovered to permit a safe trans-renal deployment whereas a distal constriction guarantees a safe anchorage to Module B (Seta Rik 2).

Figure 5 Module B (Seta Rik 2) still inserted in its cartridge. This module holds two stents: the proximal one is covered by the polyester textile whereas the distal one is uncovered in its third distal portion.

Figure 6 Ideal morphological measures of the site of operation: diameter of the infra-renal aorta and lengths of the proximal neck, the artificial aneurysm and the distal neck.
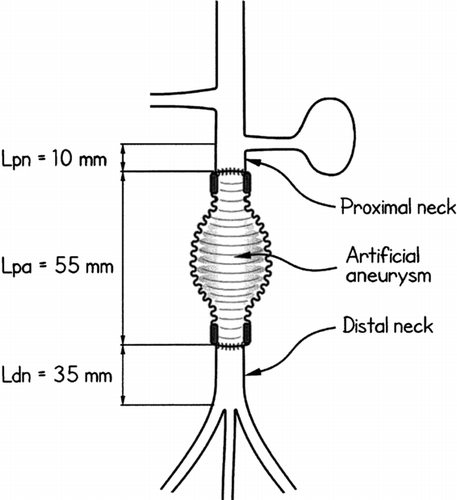
Figure 7 Suprarenal deployment of Module A (Seta Rack): the proximal bare segment of the stent lands vis a vis the orifice of the left renal artery.
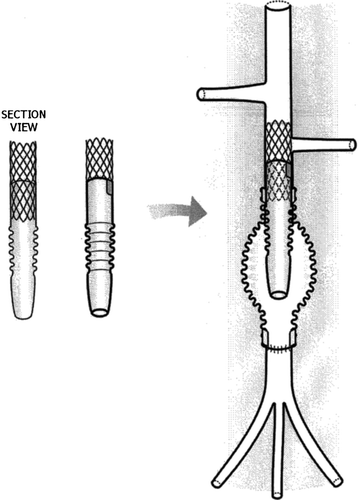
Figure 8 Infrarenal deployment of Module B (Seta Rick 2) to isolate the aneurysm. It is anchored to the Module A by telescoping and securely holds in place thanks to the constriction created with the suture.
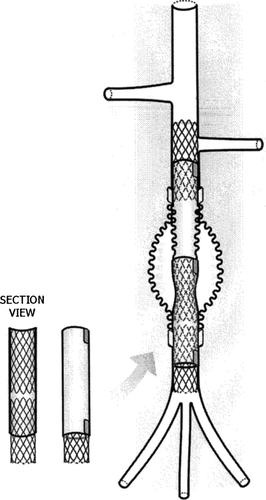
Table 1 Morphological characteristics
Figure 9 Angiographies: before the deployment of the stent-graft to isolate the prosthetic aneurysm (A) and after the deployment of the device (B).
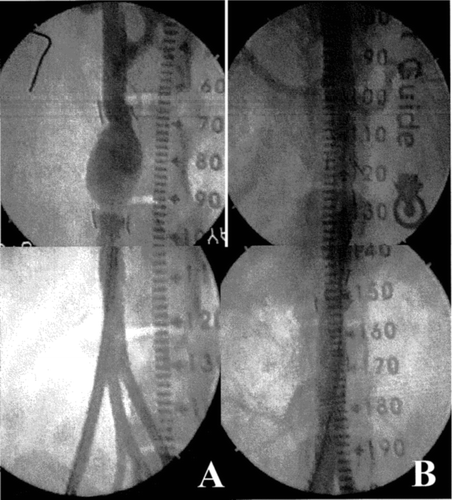
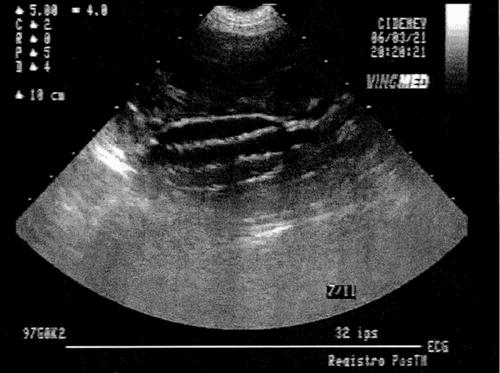
Figure 10 Echodoppler illustrations of observations carried out before (A) and immediately after the deployment of the stent-graft (B) in a dog 113 days after the creation of the aneurysm.
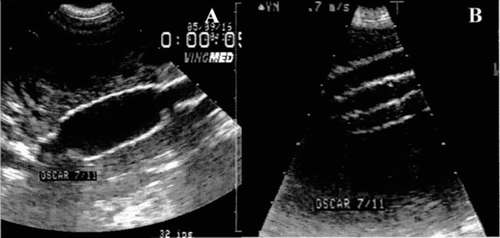
Figure 11 Angiographies recorded before the sacrifice of a dog whose stent-graft was implanted for 6 months, in the absence of contrast agent (A) and in the presence of contrast agent (B).
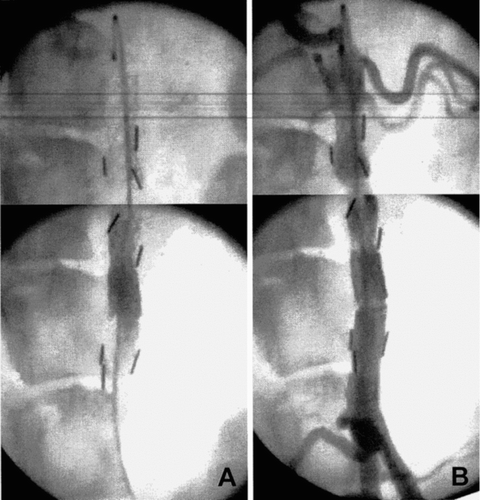
Figure 13 Gross observation of the specimens at the sacrifice of the animals: A) encapsulated prosthetic aneurysm fitted with a stent-graft before explantation; B1, B2) encapsulated prosthetic aneurysm representation of the 19 specimens whose encapsulations was classified as excellent; C1, C2) representative specimen of the 6 devices well encapsulated although the polyester graft of the prosthetic aneurysm was visible through the translucide fibrous tissues; D1, D2) representative specimen of the 4 devices whose external capsule was ulcerated.
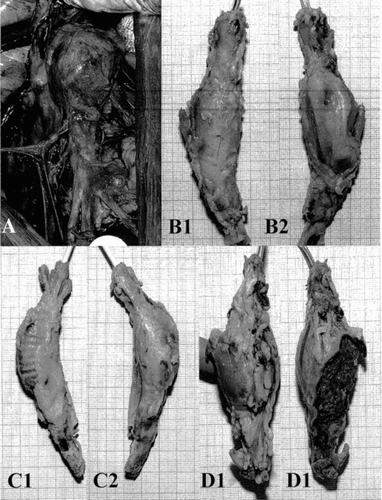
Table 2 Morphology (gross examination)
Figure 14 Different shapes of the stent-grafts after explantation and fixation in formaline; A1, A2) representative specimens of 12 straight devices; B1, B2) representative specimen of 12 slightly bent devices; C1, C2) representative specimen of 4 bent devices; D1, D2) sole misaligned device.
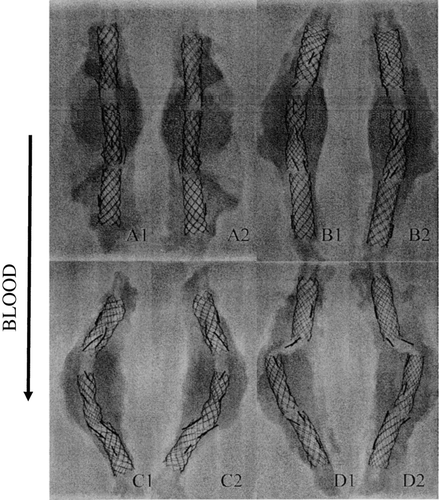
Table 3 X-rays
Figure 15 IVUS illustrations of the lumen and the cross-section of the explanted stent-graft: A1, A2) representative specimen of 18 devices whose capsule was discrete of absent; B1, B2) representative specimen of 7 devices whose thickness of the internal capsule was variable; C1, C2); representative specimen of 4 devices whose luminal surface was scattered with mural thrombi.
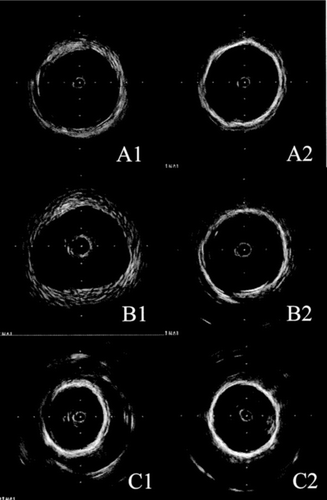
Table 4 IVUS
Figure 16 Illustrations in endoscopy of the luminal surface of the stent-grafts. A) distal end of the transrenal stent constriction in a stent-graft. B) constriction at the anchorage of Module B in Module A with variable levels of thrombotic encroaching in a stent-graft. C1, C2) distal section of the unsupported segment of Module A close to the anchorage of module B. D1, D2) scattered mural thrombi in a stent-graft 97 days after deployment in a 115 days prosthetic aneurysm.
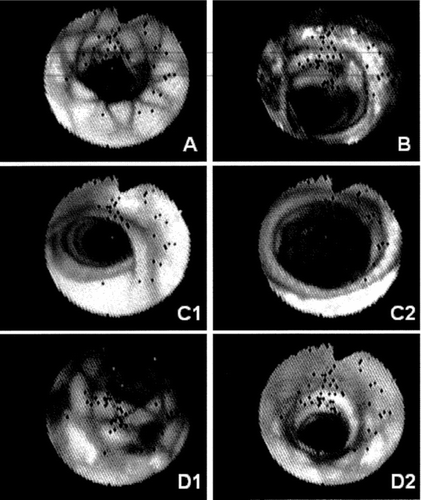
Table 5 Angioscopy