Figures & data
Table 1. Fracture incidence per patient-year in Thailand.
Table 2. Summary of costs.
Table 3. Summary of utility estimates.
Table 4. Treatment efficacy: relative risk of fracture (treatment versus placebo).
Table 5. Treatment persistence estimates.
Table 6. Costs and fracture results for base-case modela.
Table 7. Costs and fracture results for scenario model: total PMO populationa.
Table 8. Incremental cost-effectiveness estimate.
Figure 2. Probabilistic sensitivity analysis: (a) denosumab vs. alendronate and no pharmacologic treatment in high-risk patients: (b) denosumab vs. no pharmacologic treatment in high-risk patients. Abbreviation. WTP: willingness to pay. Postmenopausal women age ≥ 65 years with a femoral neck T-score of ≤−2.5 and history of vertebral fracture.
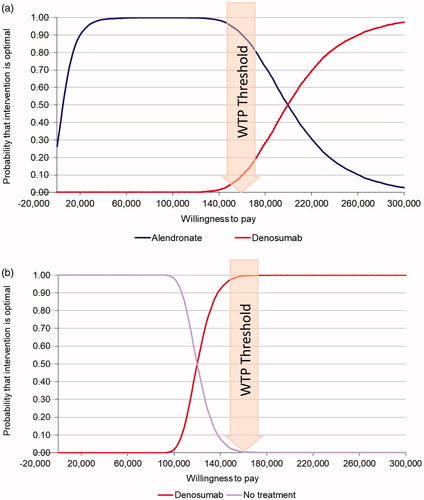
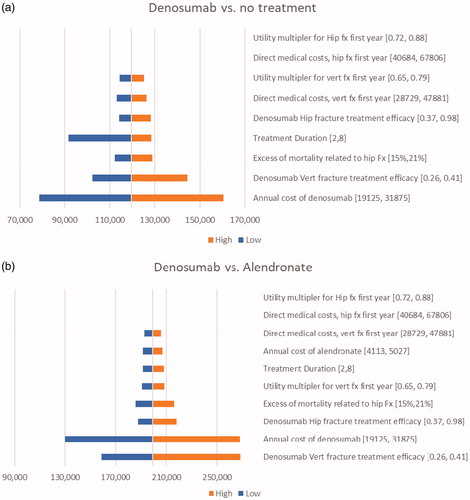
Figure 3. One-way sensitivity analysis: (a) denosumab vs. no pharmacological treatment in high-risk patients: (b) denosumab vs. alendronate in high-risk patients.