Figures & data
Table I. Demographic and clinical characteristics of patients in the mid-trimester and those at term with and without spontaneous labour.
Table II. Demographic and clinical characteristics of patients presenting with spontaneous preterm labour with intact membranes.
Table III. Demographic and clinical characteristics of patients presenting with preterm prelabour rupture of membranes.
Figure 1. AF concentrations of resistin in normal pregnancies at mid-trimester and in those at term with and without labour. The median AF concentration of resistin was significantly higher in pregnancies at term not in labour than in those in the mid-trimester (23.6 ng/mL, IQR 16.3–31.1 vs. 10 ng/mL, IQR 6.2–15.3; p < 0.001). In contrast, no significant differences were observed in the median AF resistin concentration between women with spontaneous labour at term and those at term not in labour (28.7 ng/mL, IQR 19.3–39.4 vs. 23.6 ng/mL, IQR 16.3–31.1; p = 0.07).
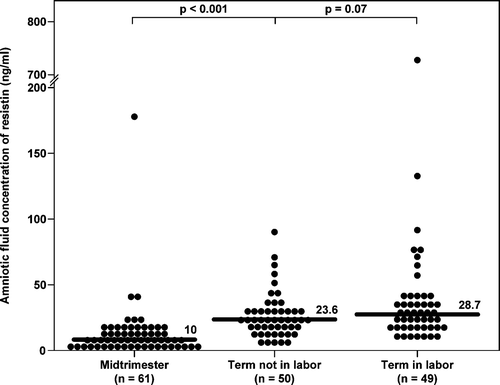
Figure 2. AF concentrations of resistin among women with spontaneous PTL and intact membranes. (a) The median AF concentration of resistin was significantly higher in patients with intra-amniotic infection/inflammation (IAI) than in women without IAI (144.9 ng/mL, IQR 44.6–623.2 vs. 18.7 ng/mL, IQR 12.1–25.8; p < 0.001) as well as in those who delivered at term (144.9 ng/mL, IQR 44.6–623.2 vs. 16.3 ng/mL, IQR 12.5–22.3; p < 0.001). There was no significant difference in the median AF concentration of resistin between those who delivered preterm and those who delivered at term. (b) Patients with spontaneous PTL without IAI delivered within 48 h from the amniocentesis had a significantly higher median AF concentration of resistin than those who delivered at term (23.2 ng/mL, IQR 18.4–28.3 vs. 16.3 ng/mL, IQR 12.5–22.3; p = 0.02).
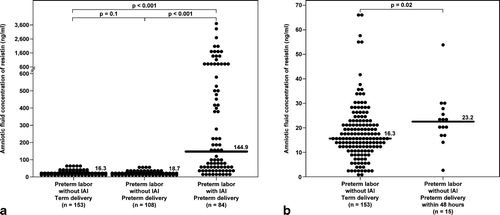
Figure 3. AF concentrations of resistin in women with preterm prelabour rupture of the membranes (PPROM). (a) The median AF concentration of resistin was significantly higher in patients with IAI than in those without IAI (132.6 ng/mL, IQR 32.3–869.7 vs. 13 ng/mL, IQR 6.9–19.4; p < 0.001). (b) In the absence of IAI, patients with PTL who deliver preterm had a significantly higher median AF resistin concentration than those with PPROM (18.7 ng/mL, IQR 12.1–25.8 vs. 13 ng/mL, IQR 6.9–19.4; p = 0.003).
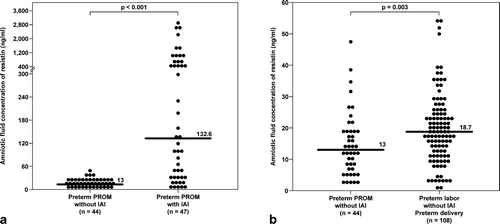
Figure 4. AF concentrations of resistin in patients with clinical chorioamnionitis at term. The median AF concentration of resistin was significantly higher in patients with microbial invasion of the amniotic cavity (MIAC) than in those without MIAC (110.5 ng/mL, IQR 52.4–243.4 vs. 40.3 ng/mL, IQR 26.2–85.9; p = 0.008).
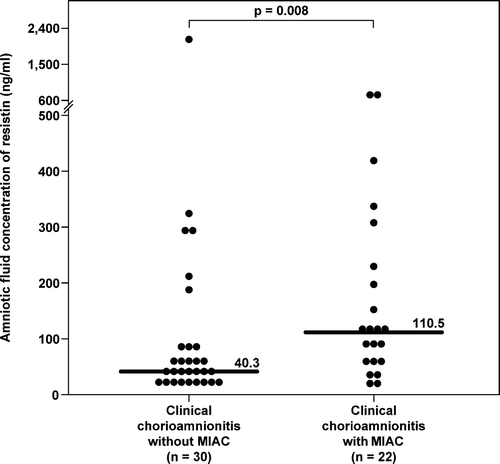
Figure 5. AF concentrations of resistin in patients with spontaneous PTL with and without histologic chorioamnionitis who delivered within 72 h from amniocentesis. Patients with histologic chorioamnionitis and/or funisitis had a significantly higher median resistin concentration in AF than those without histologic inflammation (495.1 ng/mL, IQR 15.7–3554.1 vs. 29.1 ng/mL, IQR 3–846.4, respectively; p < 0.001).
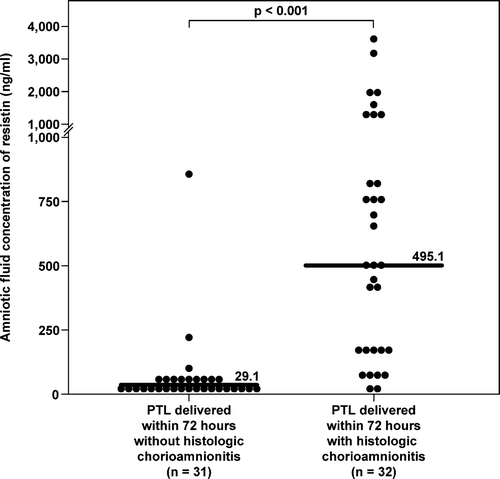
Figure 6. ROC curves of AF resistin concentration in patients with spontaneous PTL and intact membranes. (a) ROC curve for the identification of positive AF culture for microorganisms [area under the curve (AUC) for AF resistin: 0.932; p < 0.001]. (b) ROC curve for the identification of intra-amniotic inflammation, defined as AF IL-6 concentration ≥2.6 ng/mL (AUC for AF resistin: 0.933; p < 0.001).
![Figure 6. ROC curves of AF resistin concentration in patients with spontaneous PTL and intact membranes. (a) ROC curve for the identification of positive AF culture for microorganisms [area under the curve (AUC) for AF resistin: 0.932; p < 0.001]. (b) ROC curve for the identification of intra-amniotic inflammation, defined as AF IL-6 concentration ≥2.6 ng/mL (AUC for AF resistin: 0.933; p < 0.001).](/cms/asset/220119fd-fb90-4cec-9063-d32968af0b44/ijmf_a_332202_f0006_b.gif)
Figure 7. Survival analysis of the amniocentesis-to-delivery interval (days) according to AF resistin concentration cutoff ≥37 ng/mL in patients with spontaneous PTL and intact membranes. Patients with an AF resistin concentration ≥37 ng/mL (dotted line) had a shorter median amniocentesis-to-delivery interval than those with an AF resistin concentration <37 ng/mL (solid line) (3 days, 95% CI 2–4 vs. 43 days, 95% CI 39–47, respectively; p < 0.001, log rank test).
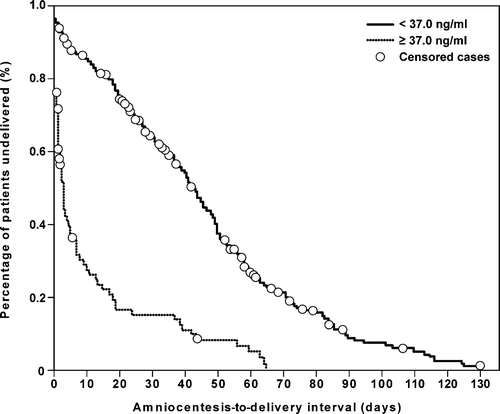
Table IV. Diagnostic indices and likelihood ratios of amniotic fluid resistin concentration for the detection of intra-amniotic infection and intra-amniotic inflammation in patients presenting with spontaneous preterm labour with intact membranes.
Table V. Diagnostic indices and likelihood ratios of amniotic fluid resistin concentration ≥37 ng/mL for the identification of patients with spontaneous preterm delivery within 48 h, 7days, 14 days and at <32 and <34 weeks of gestation