Figures & data
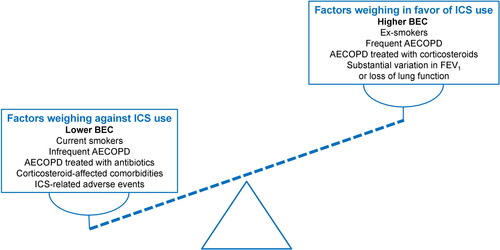
Figure 1. PubMed publications on blood eosinophils in COPD between 1991 and 2021 (accessed on July 20, 2021).
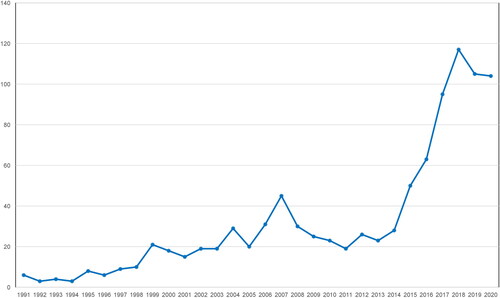
Figure 2. Pathogenetic mechanisms including the role of eosinophils in airways inflammation in COPD.
TSLP: Thymic stromal lymphopoietin; IL: Interleukin; ILC2: Type 2 innate lymphoid cell; ILC3: Type 3 innate lymphoid cell; TNFa: Tumor Necrosis Factor a; Tc1: Cytotoxic T cell; Th: T helper cell.
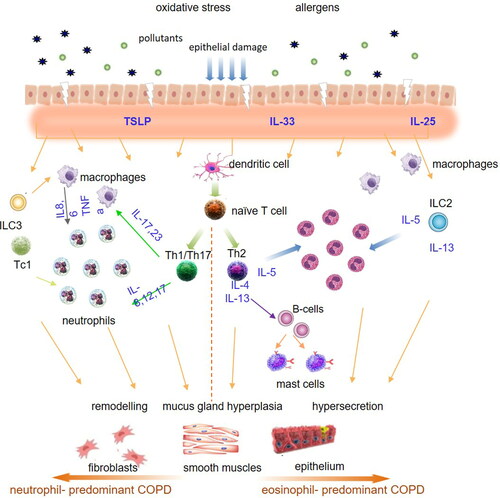
Figure 3. Factors affecting the decision for the use of ICS in stable COPD, focusing on the role of blood eosinophil counts. Dashed line represents schematically blood eosinophils as a continuous variable.
AECOPD: acute exacerbations of COPD; BEC: blood eosinophil counts; FEV1: forced expiratory volume in 1 second.