Figures & data
Figure 1. Variables associated with survival to discharge in older adults following in-hospital CPR. (A) Percent survival by subgroup. Plots show point estimates and 95% confidence intervals (left margin: group, sample size; right margin: point estimates with 95% confidence intervals). (B) Percent survival versus age. Point estimates are shown with 95% confidence intervals (inset: line plot with least-squares slope). (C) Percent survival in subgroups by age and Charlson Index. (D) Cross-validation prediction accuracy (Charlson Index vs. Age). In each simulation trial, 20,000 randomly sampled admissions were used for model training (50% survivors, 50% non-survivors), and 20,000 randomly sampled admissions were used for model testing (50% survivors, 50% non-survivors). Univariate logistic regression models were estimated in each trial (Charlson Index or age as a predictor). The testing accuracy distribution among all simulations is shown (null expectation: 50% accuracy)
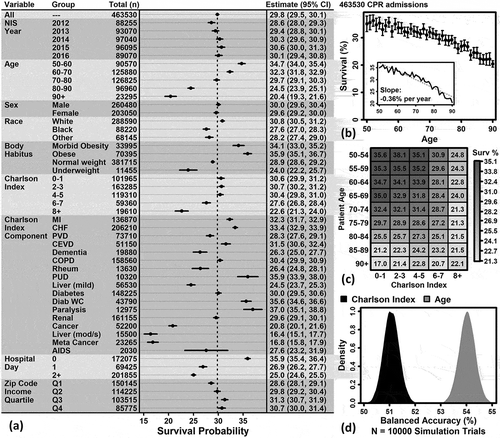
Figure 2. Influence of obesity and morbid obesity on the probability of survival to discharge following in-hospital CPR. (A – C) Percent survival in non-obese and obese patients of varying age, Charlson Index, and chronic condition (D, E) Percent discharge to home among CPR survivors in non-obese and obese patients of varying age and Charlson Index. (F, G) Percent survival in obese or morbidly obese patients with CPR performed at varying times post-admission (H, I) Percent survival in obese and morbidly obese patients with or without diagnosis codes for ventricular tachycardia (V-tach) or ventricular fibrillation (V-fib). In all figures (A – I), an asterisk (*) denotes a significant y-axis percentage difference in the comparison between obese and non-obese patients or between morbidly obese and non-morbidly obese patients (*P < 0.05, general linear model). All such comparisons were made within the subgroups indicated on the horizontal axis
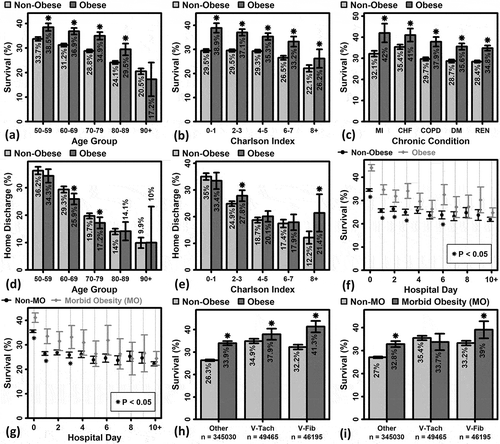
Figure 3. Diagnostic codes enriched among survivors and non-survivors. (A, C) ICD9 and ICD10 diagnostic codes overrepresented among patients that survived to discharge following in-hospital CPR. (B, D) ICD9 and ICD10 diagnostic codes overrepresented among patients that did not survive to discharge following in-hospital CPR. (E) Percent survival by subgroup. Plots show point estimates and 95% confidence intervals (left margin: group, sample size; right margin: point estimates with 95% confidence intervals). (F) Percent survival by potassium level and CKD status (*P < 0.05, non-CKD vs. CKD, general linear model). (G) Percent survival by calcium level and CKD status (*P < 0.05, non-CKD vs. CKD, general linear model)
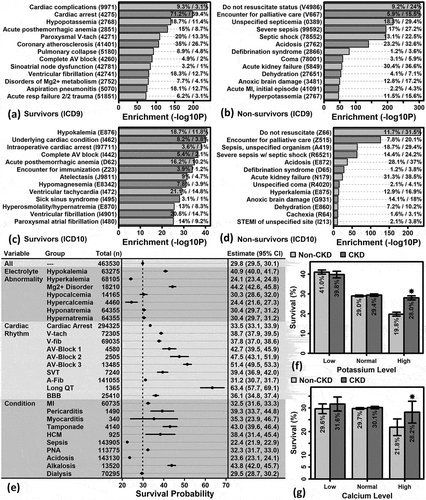
Table 1. Survey-weighted general linear model with ABCD variables. Survival was used as a quasi-binomial response variable (1 if a patient survived to discharge; 0 otherwise). The model was estimated using 463,530 hospital admissions (3 admissions excluded due to a lack of within-strata replication). Age was incorporated as an ordinal variable, whereas obesity, underweight, comorbidity and CPR day were incorporated as categorical predictors (coded as 1 or 0; see footnotes)
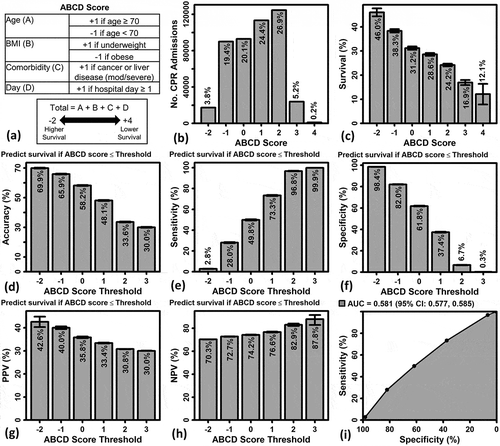
Figure 4. A simple ABCD score to risk-stratify patients with respect to the probability of survival following in-hospital CPR. (A) ABCD score definition. (B) Histogram showing number of CPR admissions relative to ABCD score. (C) Percent survival to discharge versus ABCD score. 95% confidence intervals are shown. (D – H) Accuracy, sensitivity, specificity, positive predictive value (PPV), and negative predictive value (NPV) at different ABCD score thresholds. 95% confidence intervals are shown (not visible for all estimates). (I) ROC curve. The area under the curve (AUC) statistic and confidence interval is shown (top margin)