Figures & data
Table 1. Minimum inhibitory concentrations (MICs) or minimum effective concentrations (MECs) of different antifungal agents against Pleurostoma species.Table Footnotea
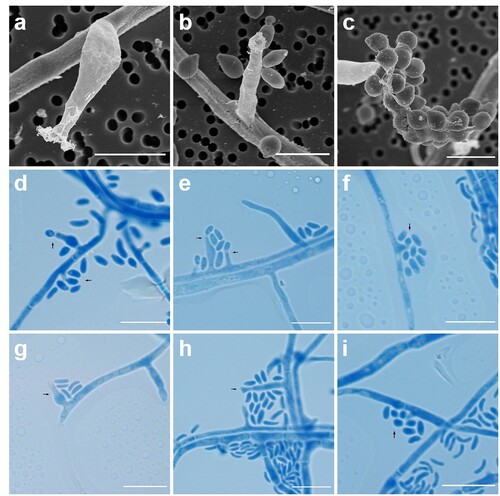
Table 2. Microscopic features of different Pleurostoma species during asexual life cycles.
Table 3. Infections caused by Pleurostoma species.