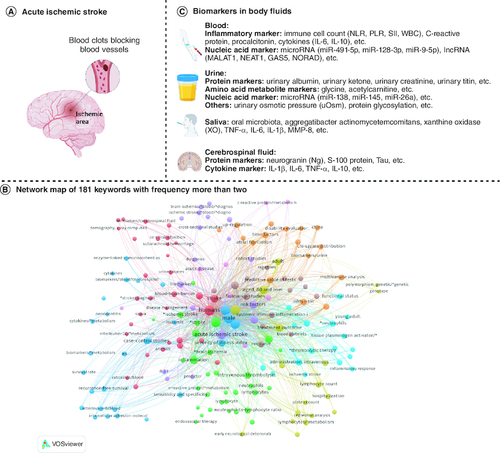
Figures & data
Table 1. Prognostic biomarkers of AIS associated with inflammatory and their prognostic value.
Table 2. Nucleic acid-related prognostic markers of AIS in blood.
Table 3. Prognostic biomarkers in urine, saliva, and CSF.