Figures & data
Table 1 Characteristics of Included Studies
Table 2 Scoring of Study Quality Based on Modified Versions of the Newcastle–Ottawa Scale for Cross-Sectional and Longitudinal Studies
Table 3 Measurement Methods and Scores of Physical Activity and Sedentary Behavior
Table 4 Assessment, Scores, and Breakdown of Activities in Tool Used for the Assessment of Activities of Daily Living
Table 5 Assessment, Scores, and Breakdown of Activities in Tool Used for the Assessment of Instrumental Activities of Daily Living
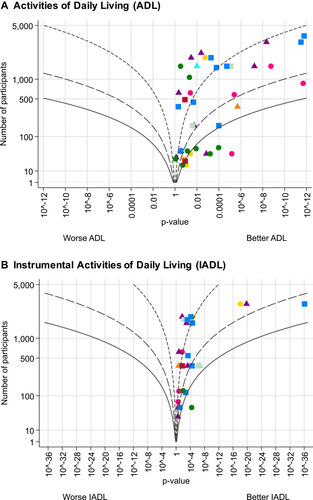
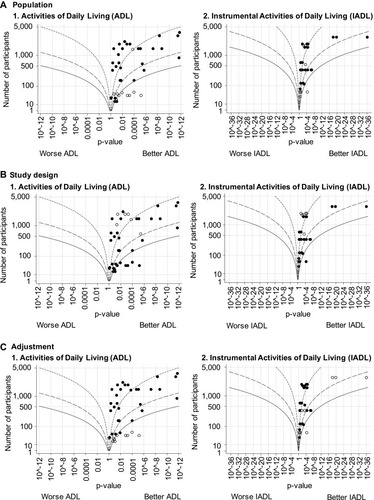
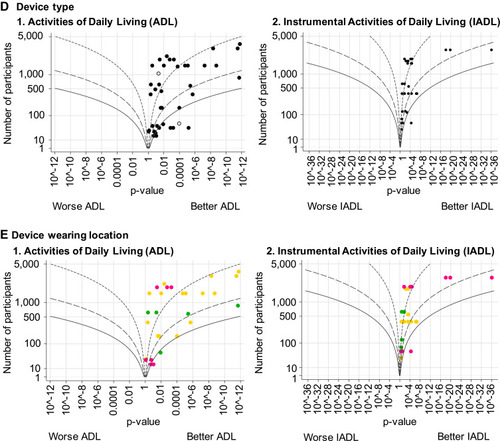
Table 6 Associations of Objectively Measured Physical Activity and Sedentary Behavior with Activities of Daily Living and Instrumental Activities of Daily Living in Community-Dwelling Older Adults, Stratified by Domain