Figures & data
Table 1 In vitro susceptibilities (evaluated based on the criteria of the Clinical and Laboratory Standards Institute 2018 and European Committee on Antimicrobial Susceptibility Testing 2018Table Footnotea) of bloodstream isolates of Escherichia coli, Klebsiella pneumoniae, and other Gram-negative bacteria, including isolates of non-typhoid Salmonella species from any site, fecal Shigella species, and Neisseria gonorrhoeae from the genitourinary system, collected from patients treated at 16 major teaching hospitals across Taiwan in 2017 to key antimicrobial agents tested
Figure 1 Comparison of (A) in vitro non-susceptibility to important antibiotics among overall, hospital-acquired, and community-acquired bloodstream Escherichia coli isolates, (B) Klebsiella pneumoniae isolates collected from 16 major teaching hospitals across Taiwan in 2017, and (C) in vitro non-susceptibility to important antibiotics between bloodstream Escherichia coli (n=148) and K. pneumoniae isolates (n=92) exhibiting the phenotype of extended-spectrum β-lactamase (unrelated to carbapenemase) production (ie, MDR phenotype).
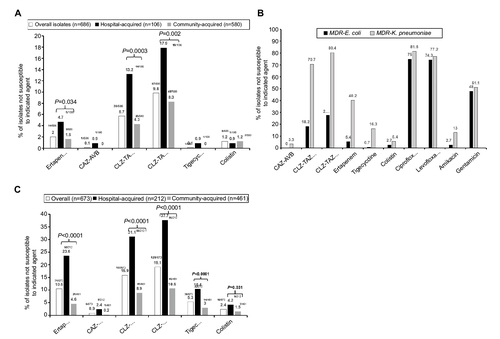
Table 2 MIC values of some key antibiotics against isolates of mcr-1-harboring Escherichia coli (n=5) and Klebsiella pneumoniae (n=4) collected from 16 major teaching hospitals throughout Taiwan in 2017
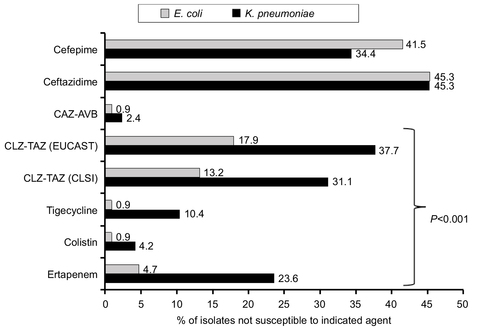
Figure 2 Comparison of in vitro non-susceptibility to important antibiotics of hospital-acquired Escherichia coli (n=106) and Klebsiella pneumoniae bloodstream isolates (n=212) collected from 16 major teaching hospitals across Taiwan in 2017.