Figures & data
Figure 1 Disruption of the balance in ROS + RNS to antioxidants leads to oxidative stress. Under conditions of oxidative stress, oxygen (O2) is reduced to superoxide (·O2−), hydrogen peroxide (H2O2), or hydroxyl radical (·OH). Hypochlorite (OCl−)is formed through the reaction of H2O2 with chloride ions (Cl−). Nitric oxide (NO) is rapidly oxidized to form nitrite (NO2−) and in the presence of oxyhemoglobin, nitrate (NO3−). Increased production of ROS and RNS causes cell damage through lipid peroxidation, DNA damage, and oxidation of proteins and enzymes. Created with BioRender.com.
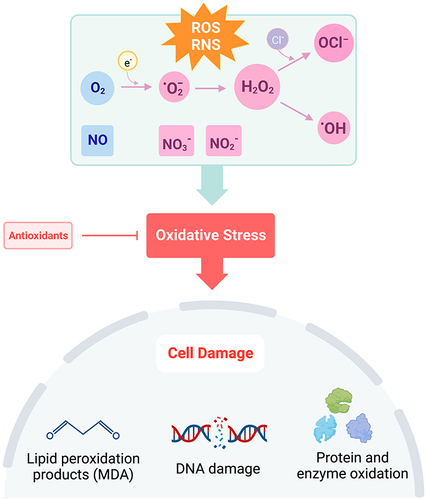
Figure 2 Oxidative stress in patients with asthma and comorbid obesity contributes to persistent immune cell recruitment and inflammation, leading to airway epithelium permeability. Left: The airway epithelium of healthy patients is comprised of several different cell types, including club cells, basal cells, ionocytes, ciliated epithelial cells, goblet cells, tuft cells, and neuroendocrine cells, which are attached to the basement membrane. The pseudostratified epithelium provides a sealed barrier to prevent environmental particles from infiltrating the lung tissue. The submucosal area lies between the basement membrane and blood vessels. Immune cells, such as macrophages, lymphocytes, eosinophils, and basophils are located within both the submucosal area and blood vessels. Right: In the presence of allergenic, viral, or air pollution particles that exacerbate asthma, immune cells are recruited from the blood stream into the submucosal area. These activated immune cells produce ROS in response to these provocative agents. Recurrent exacerbations and oxidative stress cause more inflammation and damage to the epithelial cells, resulting in epithelium permeability. In patients with obesity and asthma, inflamed adipose tissue serves as an additional source of oxidative stress, which may accelerate epithelial damage and barrier permeability. Created with BioRender.com.
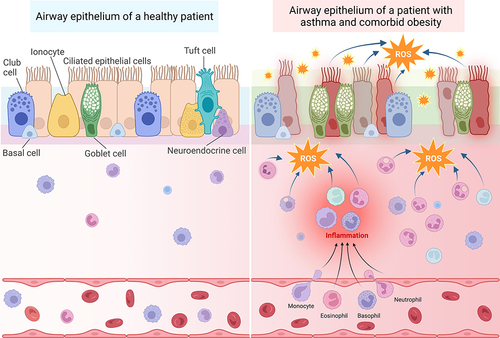
Figure 3 Comparison of postulated apical junctional protein organization in patients with asthma and comorbid obesity versus healthy patients. Airway epithelial cells are kept in close contact with adjacent epithelial cells through an organized arrangement of tight junction (ZO-1, claudin, occludin) and adherens junction proteins. People with asthma and comorbid obesity may have more severe asthma exacerbations caused by allergens, viral and bacterial pathogens, or pollutants, contributing to elevated oxidative stress. This may disrupt the organization expression levels of junction proteins, resulting in airway epithelium permeability. Created with Biorender.com.
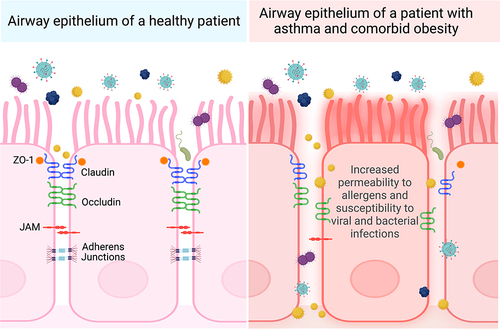
Table 1 Allergens, ROS, RNS, and Cytokines Affecting the Airway Epithelium in Human Cells
Box 1 Future Areas of Study for Clinical and Basic Science Research on Asthma and Obesity
Table 2 Allergens and ROS Affecting the Airway Epithelium in Mouse Models
