Figures & data
Table 1 MDT Members’ Characteristics (n = 24)
Table 2 MDT Case Discussion Characteristics
Table 3 Overview of Needs for Patient-Centeredness
Table 4 Overview of Strategies to Improve Patient-Centeredness
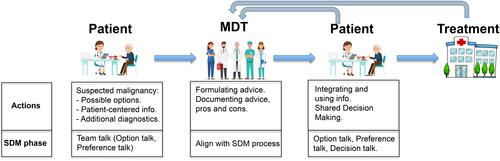
Figure 1 Cancer-related decision-making process. At suspicion of malignancy the physician discusses the possible diagnosis and treatment options with the patient (team talk and, if possible, option talk). Patient-centered information is acquired (preference talk) and additional diagnostics are ordered. The treating physician discusses the patient case in the MDT meeting, where an advice is formulated and well-documented. The team aims to align MDT decision-making with Shared Decision-Making with the patient. Then, the physician translates the MDT advice to the patient and integrates this with the patient towards a personalized treatment plan. Options are explained with pros and cons (option talk) and preferences are discussed (preference talk). The treatment is applied. During decision-making or treatment, the MDT may be consulted again, when necessary.