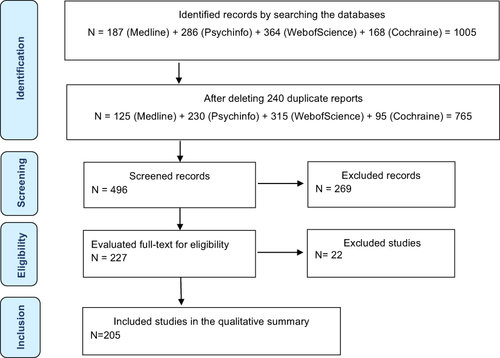
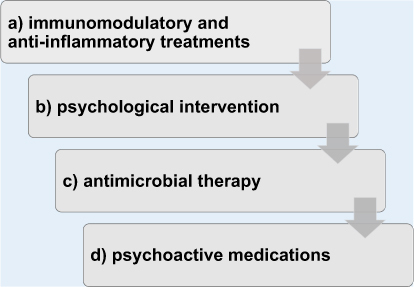
Figures & data
Box 1 PANS working criteria
Table 1 Laboratory-based Biomarkers
Table 2 Main behavioral/neuropsychological evaluation instruments
Table 3 Immunomodulatory/anti-inflammatory and antimicrobial treatment options