Figures & data
Table 1 Recent Milestones in the Study of Skin Ultrasound, Analysed by Skin High-Frequency Ultrasound in Systemic Sclerosis
Table 2 The Main Characteristics of the Studies Using Ultrasound for the Study of Localized Scleroderma
Table 3 The Main Characteristics of the Studies Using Ultrasound Elastography
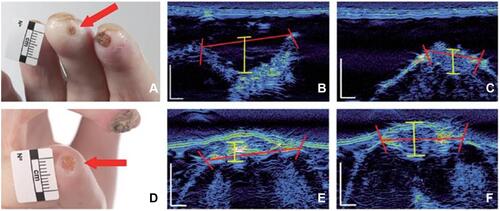
Table 4 Recent Milestones in the Study of Cutaneous Ulcers Analysed by Ultrasound in Systemic Sclerosis