Figures & data
Table II. Clinico-pathological characteristics of prostate cancer patients undergoing radical prostatectomy: ethnic group comparison.
Table I. Clinico-pathological characteristics of the 341 prostate cancer patients undergoing radical prostatectomy.
Figure 1. Overall PSA-free survival and life tables analyses. With mean and median follow-up of 39.1 months and 31.0 months (range 5–120 months), 127 men (37.2%) had PSA recurrence. Majority of the PSA recurrence 117 (92.1%) developed in the first 3-year period (83 PSA recurrence events in the first one year, 12 PSA recurrence events in the second year and 22 PSA recurrence events in the third year). Subset analysis of cT1–cT2 cases showed similar trend. Eighty-eight men (31.2%) had PSA recurrence. Majority of the PSA recurrence 78 (88.6%) developed in the first 3-year period.
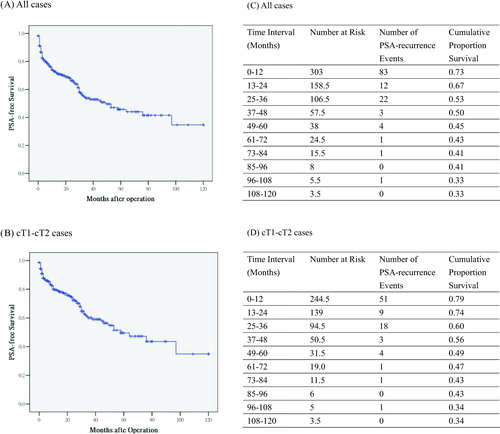
Figure 2. PSA-free survival analyses according to clinico-pathological characteristics. The PSA recurrence free probability was not significant different between the young age group (<67-years old) and old age group (≥67-year old) (Figure 2a). The PSA-free survival probabilities were significant different between the per-operative PSA level (<10 ng/mL vs., 10–20 ng/mL vs. > 20 ng/mL), biopsy Gleason Score and pathological Gleason Score (2–6 vs. 7 vs. 8–10), clinical stages, pathological stages, surgical margin and lymph node metastasis. The log-rank tests comparing these variables were all statistically significant (all p < 0.001) (Figure 2b–h).
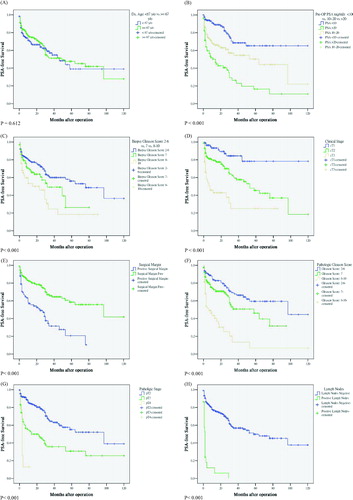
Figure 3. PSA-free survival stratified according to D'Amico risk classification. The log-rank test across three strata (low risk group vs. intermediate risk group vs. high risk group) was statistically different (p < 0.001).
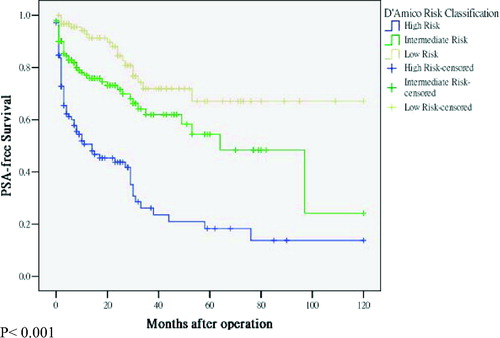
Table III. Univariate and multivariate Cox proportional hazards analyses of clinico-pathological factors predicting PSA recurrence after radical prostatectomy.