Figures & data
Table I. Demographic and clinical characteristics of the study population.
Table II. Obstetrical and neonatal outcomes of the study population.
Table III. Demographic and clinical characteristics of uncomplicated pregnant women whose samples were used to construct the reference range (n = 180)
Figure 1. Plasma concentration of sVEGFR-1 in Multiple of Median (MoM) unit. The mean MoM plasma concentration of sVEGFR-1 was significantly higher in patients with mild preeclampsia who subsequently developed severe preeclampsia than those who remained stable until term (p = 0.002). Comparisons among groups were performed after logarithmic transformation.
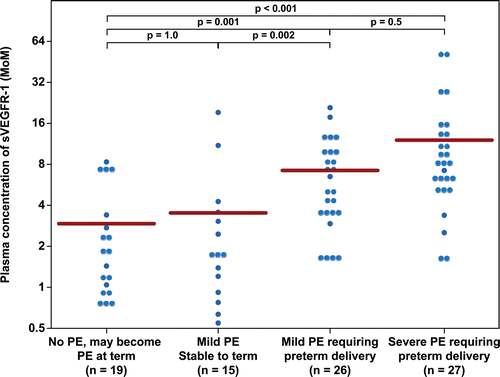
Figure 2. Plasma concentration of sEng in Multiple of Median (MoM) unit. The mean MoM plasma concentration of sEng was significantly higher in patients with mild preeclampsia who subsequently developed severe preeclampsia than those who remained stable until term (p = 0.008). Comparisons among groups were performed after logarithmic transformation.
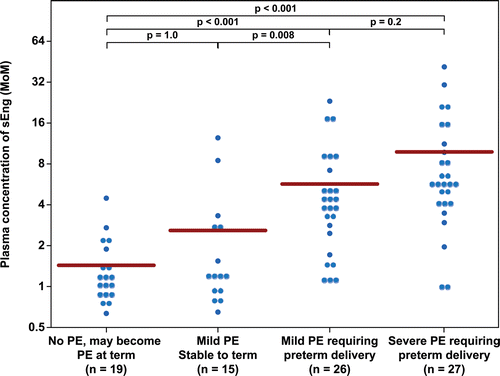
Figure 3. Plasma concentration of PlGF in Multiple of Median (MoM) unit. The mean MoM plasma concentration of PlGF was significantly lower in patients with mild preeclampsia who subsequently developed severe preeclampsia than those who remained stable until term (p = 0.005). Comparisons among groups were performed after logarithmic transformation.
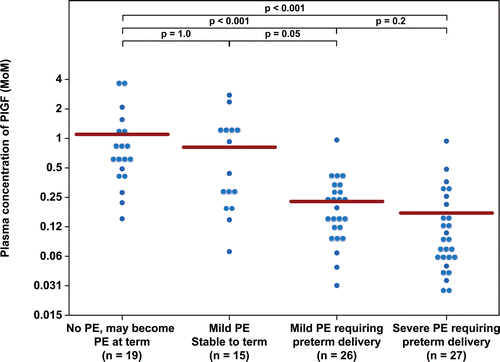
Figure 4. Plasma concentration of sVEGFR-2 in Multiple of Median (MoM) unit. The mean MoM plasma concentration of sVEGFR-2 was significantly lower in patients with mild preeclampsia who subsequently developed severe preeclampsia than those who remained stable until term (p = 0.001). Comparisons among groups were performed after logarithmic transformation.
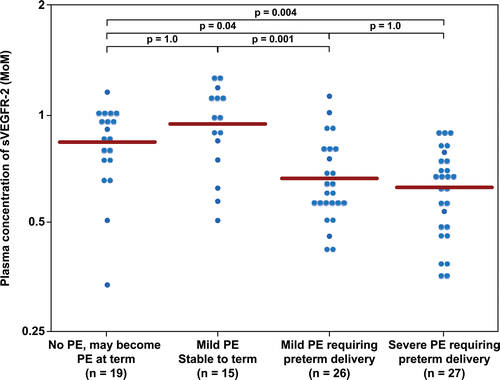
Figure 5. Plasma concentration of PlGF/sVEGFR-1 ratio in Multiple of Median (MoM) unit. The mean MoM plasma concentration of PlGF/sVEGFR-1 ratio was significantly lower in patients with mild preeclampsia who subsequently developed severe preeclampsia than those who remained stable until term (p < 0.001). Comparisons among groups were performed after logarithmic transformation.
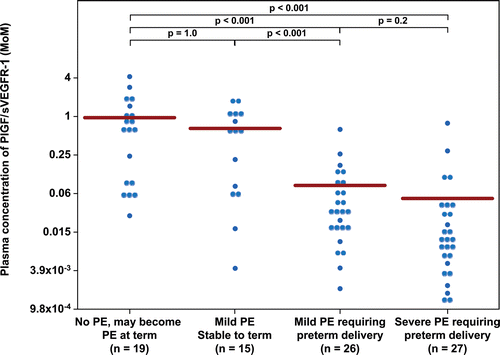
Figure 6. Plasma concentration of PlGF/sEng ratio in Multiple of Median (MoM) unit. The mean MoM plasma concentration of PlGF/sEng ratio was significantly lower in patients with mild preeclampsia who subsequently developed severe preeclampsia than those who remained stable until term (p = 0.002). Comparisons among groups were performed after logarithmic transformation.
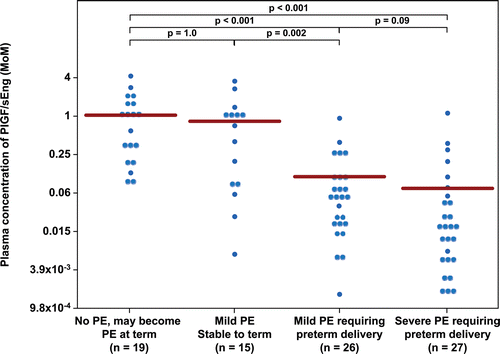
Table IV. Diagnostic performance of plasma concentrations of angiogenic/anti-angiogenic factors for the identification of patients who subsequently develop severe preeclampsia (Group III and IV).
Figure 7. Plasma concentrations of sVEGFR-1 (ng/ml) in patients from each study group plotted against a reference range (2.5th, 5th, 50th, 95th, and 97.5th percentile) derived from quantile regression of 1046 samples obtained from 180 uncomplicated pregnant women.
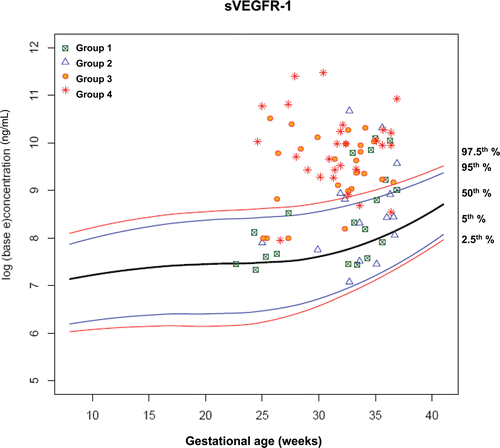
Figure 8. Plasma concentrations of sEng (ng/ml) in patients from each study group plotted against a reference range (2.5th, 5th, 50th, 95th, and 97.5th percentile) derived from quantile regression of 1046 samples obtained from 180 uncomplicated pregnant women.
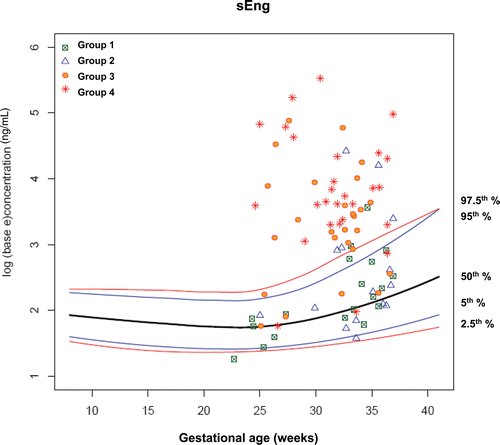
Figure 9. Plasma concentrations of PlGF (ng/ml) in patients from each study group plotted against a reference range (2.5th, 5th, 50th, 95th, and 97.5th percentile) derived from quantile regression of 1046 samples obtained from 180 uncomplicated pregnant women.
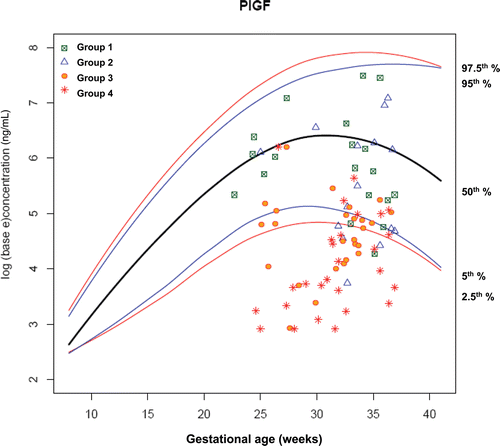
Figure 10. Plasma concentrations of sVEGFR-2 (ng/ml) in patients from each study group plotted against a reference range (2.5th, 5th, 50th, 95th, and 97.5th percentile) derived from quantile regression of 1046 samples obtained from 180 uncomplicated pregnant women.
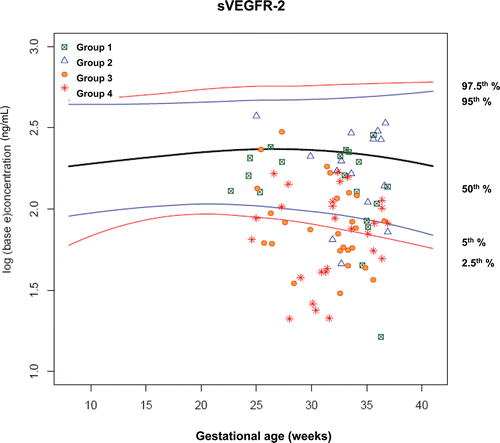
Figure 11. Plasma concentrations of PIGF/sVEGFR-1 ratio in patients from each study group plotted against a reference range (2.5th, 5th, 50th, 95th, and 97.5th percentile) derived from quantile regression of 1046 samples obtained from 180 uncomplicated pregnant women.
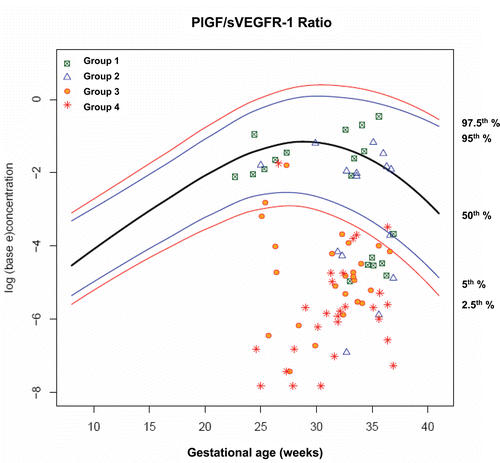
Figure 12. Plasma concentrations of PlGF/sEng ratio in patients from each study group plotted against a reference range (2.5th, 5th, 50th, 95th, and 97.5th percentile) derived from quantile regression of 1046 samples obtained from 180 uncomplicated pregnant women.
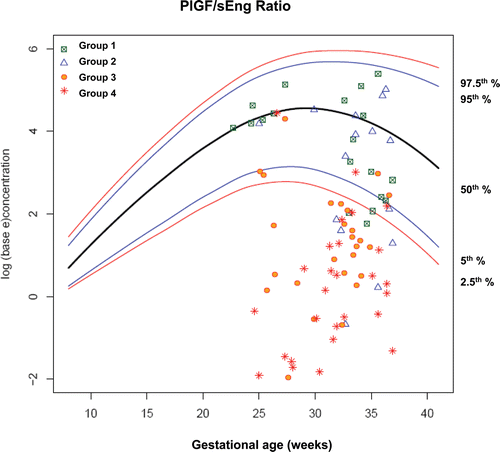
Table V. Diagnostic performance of plasma concentrations of angiogenic/anti-angiogenic factors in patients who presented at <34 weeks for the identification of those who subsequently delivered within 14 days due to preeclampsia.
Figure 13. Survival curve of patients who had plasma concentration of PlGF/sVEGFR-1 ratio ≤ 0.033 MoM and >0.033 MoM. This cut-off was associated with a shorter interval-to-delivery due to preeclampsia [PlGF/sVEGFR-1 > 0.033 MoM: n = 27, censored 5; median survival 41 days, interquartile range (IQR) 22–85 days vs. PlGF/sVEGFR-1 ≤ 0.033 MoM: n = 32, censored 3, median survival 6 days, IQR 3-10 days; p < 0.001; hazard ratio = 6 (95% CI 2.5–14.6)].
![Figure 13. Survival curve of patients who had plasma concentration of PlGF/sVEGFR-1 ratio ≤ 0.033 MoM and >0.033 MoM. This cut-off was associated with a shorter interval-to-delivery due to preeclampsia [PlGF/sVEGFR-1 > 0.033 MoM: n = 27, censored 5; median survival 41 days, interquartile range (IQR) 22–85 days vs. PlGF/sVEGFR-1 ≤ 0.033 MoM: n = 32, censored 3, median survival 6 days, IQR 3-10 days; p < 0.001; hazard ratio = 6 (95% CI 2.5–14.6)].](/cms/asset/5fd0f620-828f-4e7b-a21a-0250bc523c92/ijmf_a_589932_f0013_b.gif)
Figure 14. Plasma concentrations of PIGF/sVEGFR-1 ratio in patients from each study group plotted against a reference range (2.5th, 5th, 50th, 95th, and 97.5th percentile) and the cut-offs (dash line) according to the 3-zone classification.
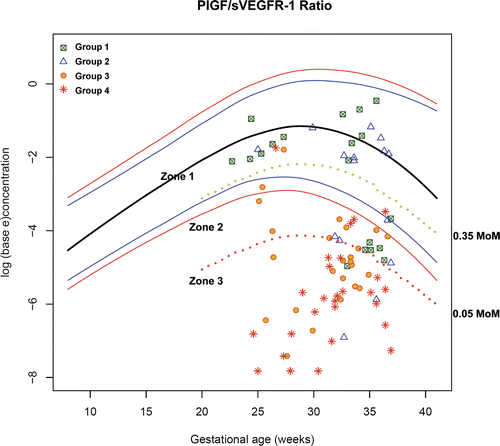
Figure 15. Plasma concentrations of PlGF/sEng ratio in patients from each study group plotted against a reference range (2.5th, 5th, 50th, 95th, and 97.5th percentile) and the cut-offs (dash line) according to the 3-zone classification.
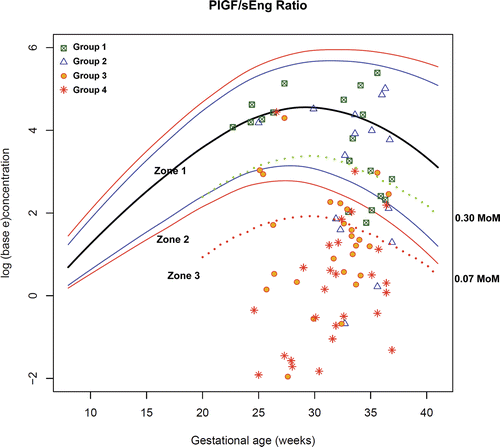
Table VI. Rate of preterm delivery in patients presenting to the obstetrical triage area at <34 weeks with a diagnosis of “suspected preeclampsia” according to the 3-zone classification of plasma angiogenic/anti-angiogenic factor concentrations.
Table VII. Disposition of patients with “suspected preeclampsia” before 34 weeks of gestation from the triage area according to the 3-zone classification of plasma angiogenic/anti-angiogenic factor concentrations.
Table VIII. Obstetrical characteristics and plasma concentrations of PlGF/sVEGFR-1 and PlGF/sEng ratio in patients with severe maternal complications.