ABSTRACT
The feasibility of mindful hypnotherapy (MH) intervention for stress reduction was investigated in a randomized trial. Forty-two college-age participants with elevated stress were randomized into MH intervention or wait-list control condition. MH participants completed an 8-week intervention with 1-hour individual sessions and self-hypnosis audio recordings for daily mindfulness. Results indicated excellent feasibility, determined by participant satisfaction, treatment adherence (84% compliance rate), and low rate of adverse events (4.5%). There were significant differences between the MH and control groups postintervention, with the mindful hypnotherapy intervention resulting in significant and large decrease in perceived distress, p < .001, 15.35 (1.54), Hedge’s g = − 1.14, and increase in mindfulness, p < .001, 50.07 (2.04), Hedge’s g = 1.36. This study indicates that MH is a feasible intervention for stress reduction and increasing mindfulness.
Nicholas Olendzki, Gary R. Elkins, Elizabeth Slonena, Julia Hung, und Joshua R. Rhodes
Abstract : Die Machbarkeit von Mindful Hypnotherapy (MH)-Intervention zur Streßreduktion wurde in einem randomisierten Experiment untersucht. 42 Teilnehmer im Collegealter, die erhöhtem Streß ausgesetzt waren, wurden zufällig einer MH-Intervention oder einer Wartelisten-Bedingung zugeordnet. Die MH-Teilnehmer komplettierten eine 8-wöchige Intervention mit einstündigen Einzelsitzungen und Selbsthypnose-Audios für tägliche Achtsamkeitspraxis. Die Ergebnisse deuten exzellente Durchführbarkeit an, die von der Zufriedenheit der Teilnehmer, Behandlungsadhärenz (84 % Compliance-Rate) und einer geringen Rate unerwünschter Ereignisse (4,5 %) bestimmt wird. Nach der Intervention gab es signifikante Unterschiede zwischen den MH.- und den Kontrollgruppen, bei der die Mindful Hypnotherapy-Intervention in signifikanter und großer Abnahme des empfundenen Unwohlseins, p < 0,001, 15,35 (1,54), Hedge’s g = -1,14 und einer Zunahme der Achtsamkeit, p < 0,001, 50,07 (2,04), Hedge’s g = 1,36 resultierte. Diese Studie verweist darauf, daß MH eine geeignete Intervention zur Streßreduktion und einer Achtsamkeitszunahme ist.
Stephanie Riegel, M.D.
Nicholas Olendzki, Gary R. Elkins, Elizabeth Slonena, Julia Hung et Joshua R. Rhodes
Résumé : La faisabilité d’une intervention hypnothérapeutique consciente (IHC) pour réduire le stress a été étudiée dans un essai randomisé. Quarante-deux participants dans la vingtaine souffrant de stress élevé ont été répartis de façon aléatoire dans un groupe avec IHC et un groupe témoin placé sur une liste d’attente. Les participants à l’IHC ont été soumis à une intervention de huit semaines avec séances privées d’une heure et enregistrements audio quotidiens d’auto-hypnose de pleine conscience. Les résultats ont indiqué une excellente faisabilité, déterminée par la satisfaction des participants, l’adhésion du traitement (taux de conformité de 84 %) et le faible taux d’événements indésirables (4,5 %). On a remarqué des différences significatives entre le groupe d’IHC et le groupe témoin aprés l’intervention, celle-ci résultant en une diminution significative et importante de la détresse peréue, p < 0,001, 15,35 (1,54), g de Hedge = -1,14, et en une augmentation de la pleine conscience, p < 0,001, 50,07 (2.04), g de Hedge = 1,36. Cette étude indique que l’IHC est une intervention faisable pour réduire du stress et augmenter la pleine conscience.
Johanne Raynault
C. Tr. (STIBC)
Nicholas Olendzki, Gary R. Elkins, Elizabeth Slonena, Julia Hung, y Joshua R. Rhodes
Resumen: La viabilidad de una intervención de hipnoterapia consciente (HC) para la reducción del estrés se investigó en un ensayo aleatorizado. Cuarenta y dos participantes de edad universitaria con altos niveles de estrés fueron aleatorizados en la intervención HC y el grupo control de lista de espera. Los participantes del grupo HC completaron una intervención de 8 semanas con sesiones individuales de 1 hora, utilizando una audio grabación de autohipnosis para el mindfulness diario. Los resultados indican una viabilidad excelente, determinada por la satisfacción de los participantes, la adherencia al tratamiento (tasa de cumplimiento del 84%), y una baja tasa de eventos adversos (4.5%). Se encontraron diferencias significativas entre los grupos HC y control en la posintervención, con le intervención HC mostrando un decremento grande y significativo en la aflicción percibida, p < .001, 50.07 (2.04), g de Hedge = 1.36. Este estudio indica que la HC es una intervención viable para reducir el estrés e incrementar mindfulness.
Omar Sánchez-Armáss Cappello
Autonomous University of San Luis Potosi, Mexico
Recent epidemiological studies have found that stress and anxiety are extremely common psychological concerns and that there is a need for effective treatment interventions (Bandelow & Michaelis, Citation2015; McLean, Asnaani, Litz, & Hofmann, Citation2011; Stein, Scott, de Jonge, & Kessler, Citation2017). Evidence of several meta-analysis studies support that mindfulness-based therapies such as mindfulness-based stress reduction (MBSR; Kabat-Zinn, Citation1982), mindfulness-based cognitive therapy (MBCT; Teasdale et al., Citation2000), acceptance and commitment therapy (ACT; Hayes & Wilson, Citation1994), and dialectical behavioral therapy (DBT; Linehan, Citation1987) can be efficacious in the reduction of stress and anxiety symptoms (Grossman, Niemann, Schmidt, & Walach, Citation2004; Hofmann, Sawyer, Witt, & Oh, Citation2010; Piet, Würtzen, & Zachariae, Citation2012; Powers, Vörding, & Emmelkamp, Citation2009). A meta-analysis by Powers et al. (Citation2009), which included active-treatment randomized controlled trials (RCTs), found that ACT performed equally to established anxiety treatments such as behavioral and cognitive-behavioral therapy. Furthermore, the literature suggests that these gains tend to be well maintained at long-term follow up (Carlson, Speca, Faris, & Patel, Citation2007; Grossman, Tiefenthaler-Gilmer, Raysz, & Kesper, Citation2007; Miller, Fletcher, & Kabat-Zinn, Citation1995).
Despite indications that mindfulness could be an efficacious intervention for stress and anxiety in a variety of populations, existing mindfulness treatments are time intensive. For example, group mindfulness interventions are typically 2 to 2.5 hours long and include an all-day retreat that may be burdensome on individuals (Miller et al., Citation1995). Additionally, mindfulness-based treatments have not been found to be consistently superior to standard cognitive behavioral therapy in well-controlled empirical studies of stress and anxiety (Forman, Herbert, Moitra, Yeomans, & Geller, Citation2007; Khoury et al., Citation2013; Manicavasgar, Parker, & Perich, Citation2011; Öst, Citation2008). Therefore, if a mindfulness treatment could be developed that obtains results equal to or better than existing treatments but with shorter or fewer sessions, it could have advantages and represent a valuable contribution to treatment options for anxiety and stress reduction.
Integrating Hypnosis into Standard Therapy
Hypnosis and mindfulness have been hypothesized to be “a natural marriage with excellent prospects” (Lynn, Barnes, Deming, & Accardi, Citation2010, p. 217.) due to substantial theoretical compatibility and their phenomenological and physiological overlap (Forte, Brown, & Dysart, Citation1987; Grant, Citation2012; Lynn, Malaktaris, Maxwell, Mellinger, & van der Kloet, Citation2012; Lynn, Surya Das, Hallquist, & Williams, Citation2006; Sabourin, Cutcomb, Crawford, & Pribram, Citation1990; Walrath & Hamilton, Citation1975). Mindfulness is defined as “paying attention in a particular way; on purpose, in the present moment, nonjudgmentally” (Kabat-Zinn, Citation1994, p. 4.), whereas hypnosis is defined as “a state of consciousness involving focused attention and reduced peripheral awareness characterized by an enhanced capacity for response to suggestion” (Elkins, Barabasz, Council, & Spiegel, Citation2015, p. 6). Grover, Jensen, Patterson, Gertz, and Day (Citation2018) state that the targeted therapeutic process may be a fundamental difference between mindfulness-based interventions and hypnosis. More specifically, mindfulness targets a shift in the relationship toward experience, whereas the target of hypnosis is a shift in the experience itself. Rather than a stand-alone treatment, hypnotherapy involves integrating hypnosis into existing treatment modalities (Elkins, Citation2014; Elkins, Fisher, Johnson, Carpenter, & Keith, Citation2013; Schoenberger, Kirsch, Gearan, Montgomery, & Pastyrnak, Citation1998), and there is evidence to suggest that integrating hypnosis into a mindfulness-based treatment (MBT) can address the shortcomings of MBTs discussed above. For example, Kirsch, Montgomery, and Sapirstein (Citation1995) reviewed 18 studies and found that clients receiving cognitive-behavioral therapy enhanced by hypnotherapy showed greater improvement than at least 70% of clients receiving nonhypnotic treatment. Although there is a need for further research on the impact of integrating hypnosis into standard treatment for stress and anxiety disorders specifically (Golden, Citation2012), there is initial evidence that integrating hypnosis into cognitive-behavioral treatment, therapeutic gains are superior to CBT alone. Therefore, it is theorized that third wave cognitive therapies are not only compatible with hypnosis, but treatment gains may even be enhanced by a hypnotic delivery and reinforcement of content.
Mindful Hypnotherapy
The synthesis of mindfulness and hypnosis has been theorized in recent years due to the similarities of the proposed mechanisms of mindfulness and hypnosis for stress reduction (Alladin, Citation2014; Elkins, Roberts, & Simicich, Citation2018; Otani, Citation2016). In both mindfulness and hypnosis, an enhanced mind-body connection is experienced by focusing attention to suggestions and imagery to achieve specified treatment goals (Otani, Citation2016). A unique characteristic of mindfulness is the encouragement of a nonjudgmental, accepting, and flexible relationship to one’s experiences (thoughts, emotions, behaviors, and situations). Thus, mindful hypnotherapy is defined as “an intervention that intentionally uses hypnosis (hypnotic induction and suggestion) to integrate mindfulness for personal and therapeutic benefit” (Elkins & Olendzki, Citation2019).
Many theories posit that a hypnotic induction facilitates internal focus and openness to suggestion with relaxing imagery providing a safe and peaceful mental environment to experience mindfulness throughout the session. Additionally, hypnotic suggestions for mindfulness-based concepts, such as present moment awareness and nonjudgmental acceptance, work synergistically to facilitate an individual’s ability to focus and relax more easily without criticism. Relaxation is continued to be experienced in the present moment, via hypnotic imagery, deepening suggestions, and openness to mindfulness principles. Posthypnotic suggestions are used for continued experience of relaxation, nonjudgement, and present moment awareness after the session is complete. The integration of mindfulness and hypnosis principles (mindful hypnosis) in a single intervention (mindful hypnotherapy) may make the stress-reduction practice time effective, less daunting, and easier to use.
Despite the promise of an integrated mindfulness and hypnosis approach, there have been no studies to date that have been published that integrate mindfulness treatment with hypnosis. In addition, no published trials have demonstrated its feasibility and no manualized interventions exist for such an approach. The present study aims to address these gaps in the empirical literature by investigating a mindful hypnosis intervention for stress reduction using a manualized intervention. The primary outcome of this study was to investigate the feasibility of mindful hypnotherapy. The secondary outcomes were to investigate the impact of mindful hypnotherapy on stress, psychological distress, and mindfulness compared to a waitlist control.
Methods
Participants
Participants were recruited through flyers displayed throughout a university campus and electronic advertising. Participant eligibility requirements included: proficiency in English, at least 18 years of age, self-identify as highly stressed as indicated by a score of 50% or higher on a visual analog scale measuring overall stress, and no diagnostic indicators or a history of borderline personality disorder, psychosis, or schizophrenia due to contraindication with hypnosis. Walker (Citation2016) outlines the need for these exclusions to be utilized, because psychosis involves a distortion of reality and hypnosis blurs the boundaries of the subject’s external reality. People interested in participating (N = 55) were randomly assigned to either the mindful hypnotherapy intervention or assigned to the waitlist control group (WLC). Participants in the WLC were offered the opportunity to complete the intervention after their participation in the study.
Demographics
Participants in this study were all students at Baylor University, and were predominantly undergraduate, white, female, and between the ages of 18 and 21 (mean age = 19.6, 81% female, 65% Caucasian). The intervention and control group were approximately equal in demographic characteristics in most categories. The differences that did exist between groups were generally small and unlikely to have much impact on the interpretation of statistical data.
Instruments
Perceived Stress Scale (PSS)
The PSS is a 10-item self-report questionnaire that measures the respondent’s global levels of perceived stress (Cohen & Williamson, Citation1988). Respondents are asked to rate how often they have experienced various events and feelings during the past month on a scale from 0 (Never) to 4 (Very Often), yielding a total PSS score of 0 to 40. For a college population, the mean score is 23.18 (SD = 7.31), with an alpha reliability of .84 (Roberti, Harrington, & Storch, Citation2006).
Psychological Distress Profile
Psychological distress was measured by the Psychological Distress Profile (PDP), which is a 20-item self-report measure that assesses four constructs of psychological distress: depression, hopelessness, anxiety, and anger (Elkins & Johnson, Citation2015). Respondents are asked to rate how often they feel currently using a 5-point Likert scale ranging from 1 (Strongly Disagree) to 5 (Strongly Agree). The scale demonstrates high internal consistency with alpha coefficients ranging from .87 to .95 across scales and good structure validity on all four constructs with strong correlations with validated measures of depression, hopelessness, anxiety, and anger (Elkins & Johnson, Citation2015).
The Acceptance and Action Questionnaire
The Acceptance and Action Questionnaire (AAQ-II) was used to assess mindfulness domains including acceptance, experiential avoidance, and psychological inflexibility. The AAQ-II is a brief 10-item self-report in which respondents are asked to rate their endorsement of mindful experiences using a 7-point Likert scale ranging from Never True to Always True. The mean alpha coefficient has been measured to be 0.84 (Bond et al., Citation2011).
To measure feasibility and adherence to home practice, participants were given a daily practice log to record how many days they engaged in home practice over the course of the 8-week intervention.
Interventions
Participants randomly assigned to the intervention group participated in eight weekly, 1-hour sessions of mindful hypnotherapy as illustrated in Elkins and Olendzki (Citation2019). All intervention sessions were completed at the Mind-Body Medicine Lab at Baylor University, with the exception of 1 individual whose sessions were conducted off-site to accommodate mobility difficulties. The intervention included an abbreviated psychological intake in session one, and each session included a didactic teaching component and a hypnotic induction tailored to the content of each session. At the end of each session, the participant received a home-practice audio CD based on the content presented that week. Participants were instructed to practice with the audio every day and record their practice in their practice logs. The progression of material for each week was as follows: present-moment awareness, nonjudgmental awareness of the five senses, nonjudgmental awareness of thoughts and feelings, self-hypnosis, compassion for self and others, awareness of personal values and meaning in life, integrated mindfulness, and termination/transition to long-term practice. A more detailed outline of the mindful hypnotherapy intervention can be found in Appendix A. Participants randomly assigned to the waitlist control group did not receive the study intervention during their participation. Waitlist control participants were evaluated at baseline, 4-weeks, and 8-weeks postbaseline.
Procedure
After obtaining written informed consent, participants randomized to either the mindful hypnotherapy (MH) or WLC condition completed a demographic questionnaire and baseline measures. The intervention group consisted of eight weekly, 1-hour sessions of mindful hypnotherapy. Participants randomly assigned to the WLC received no intervention during that time but were offered the opportunity to complete the intervention after their participation in the study. The PDP and AAQ-II were conducted at baseline and at post intervention (8 weeks after baseline, for WLC), and the PSS was administered at baseline, 4 weeks, and 8 weeks. To reduce participant and clinician bias, the participant’s score was not shared with the interventionist or the participant until the conclusion of the study.
Results
Feasibility Results
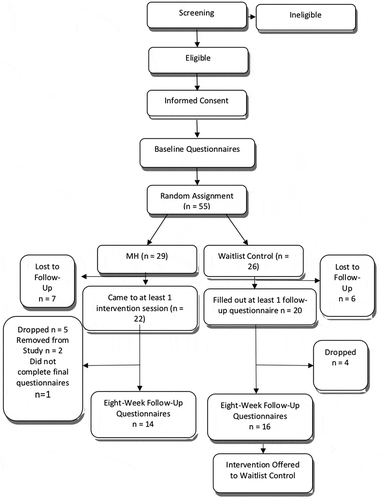
The study initially aimed to randomize 44 participants, however, 42 individuals remained in the study beyond the baseline random assignment (22 in the intervention group, 20 in the control group). Therefore, the attrition statistics are evaluated based on this sample size of 42. Overall, the retention rate resulted in a 68% completion rate in the intervention group. Due to missing data points on follow-up measures, there were a total of 14 members of the intervention group and 16 in the control group whose data could be used in the paired-sample t-tests, repeated-measures ANOVA, and hierarchical linear regression.
Of the 22 individuals randomly assigned to the intervention group, 5 individuals dropped from the study, 2 individuals were removed from the study due to premorbid clinical issues (premorbid depression and a history of PTSD), and 1 individual missed their last session (see ). Furthermore, four individuals from the control group completed their 4-week measures but did not respond to attempts to contact them for the 8-week measures. This resulted in an overall 68% retention rate for the intervention group and 80% retention rate for the waitlist control.
Participant feedback indicates that MH is a highly satisfactory intervention. On a satisfaction rating scale ranging from 0 to 10, with 6 indicating satisfaction, most participants showed a high degree of satisfaction with the number of sessions (mean = 8.5, SD = .26), ease of practice with the home practice hypnosis CDs (mean = 9.15, SD = .32), clarity of session content (mean = 9.46, SD = .18), and overall satisfaction in the intervention (mean = 8.92, SD = .30). The average participant practiced almost every day over the course of the study (mean times practice per week = 5.9, SD = 1.68) and resulted in an 84% compliance rate for home practice. Overall, the MH intervention resulted in a low adverse event rate of 4.5%.
Secondary Outcome Results
Overall, significant results were obtained for the intervention group for most of the constructs measured, and effect sizes were large in the domains of stress, mindfulness, and psychological distress. Changes from pre- to postintervention were not significant in the control group and this is commensurate with expectations. The exceptions where there was significant change in the control group are presented in their respective sections and may be due to natural variations in stress over the course of the semester.
A repeated measures ANOVA was performed for each scale and subscale to determine whether there were differences between the means of the two groups. Overall, significant and large differences were found between groups for perceived stress, all of the subscales for psychological distress, and total mindfulness.
Due to the multitude of t-tests and ANOVA performed in the data analysis, the threshold for rejecting the null hypothesis was systematically controlled using a procedure described by Benjamini, Drai, Elmer, Kafkafi, and Golani (Citation2001). The False Discovery Rate: Benjamini-Hochberg (FDR-BH) procedure used performs well even in the presence of a correlation between the hypothesis tests. The adjustment in the cutoff threshold for statistical significance does not impact the calculation for effect size.
Within groups, there was a large, significant reduction in stress pre- and postintervention measured by the PSS for the intervention group but not for the control group (See ). Regarding between-groups differences, the PSS showed a significant, large effect of group assignment across time points, with the intervention group having a lower mean stress by the end of the study compared to the control group (p < .001, 15.35 (1.54), Hedge’s g = −1.14). Correcting for multiple hypothesis tests did not impact the findings for stress for the PSS scale regarding statistical significance.
Table 1. Descriptive Statistics & Pre-Post t-Test for Stress
Similarly, all findings for psychological distress as measured by the Psychological Distress Profile in the intervention group were large, significant, and in a direction indicating reduced distress from pre- to postintervention (see ). These findings were robust enough that after correcting for multiple t-tests, overall distress and each of its subscales remained significant. All findings for psychological distress for the control group were nonsignificant both before and after correction. There were also large and statistically reliable differences between the intervention and control groups for overall distress and each of its subscales. The direction and effect size of the differences found indicate a significant reduction in distress and its subscale components for the MH group in comparison to controls (see ).
Table 2. Descriptive Statistics & Pre-Post t-Test for Distressed Mood
Table 3. Pre-Post ANOVA for Distressed Mood
The effect size was large and statistically significant for the t-tests of overall mindfulness pre- and postintervention measured by the AAQ-II for the MH intervention (p < .001, 50.07 (2.04), Hedge’s g = 1.36). There was no significant difference in the control group between pre-and postintervention measures of mindfulness. There were statistically significant changes found for mindfulness when comparing the two groups (See ). The findings were statistically significant and large for the AAQ-II. The results suggested that the MH group became more mindful by the end of the study compared to the control group.
Table 4. Pre-Post ANOVA for Mindfulness
Discussion
This study provided the first empirical evaluation of mindful hypnotherapy, a novel intervention which incorporates elements of both mindfulness and hypnosis. The results support the hypothesis that MH is a feasible, highly satisfactory intervention with an acceptable rate of attrition and adverse events. Intervention participants who completed MH reported the intervention to be highly palatable, and their adherence to home practice was exceptional. The drop-out rate for the intervention group was comparable to the drop-out rate for the control group, which suggests that attrition had to do with demographic factors unrelated to the burdensomeness or palatability of the intervention.
Results of the study also suggest that MH coincides with a large, statistically reliable, and clinically significant improvements in perceived stress (p < .01; g = − 1.14), overall mindfulness and psychological flexibility (p < .01; g = 1.11), and psychological distress (p < .01; g = − 1.09). Furthermore, each of the subscales of distress individually decreased by a significant margin, including depression (p < .01; g = − 1.06), hopelessness (p < .01; g = − 1.16), anxiety (p < .01; g = − 0.99), and anger (p < .1; g = − 1.09). The pilot study findings support that MH is a feasible intervention that significantly decreases psychological distress and perceived stress while increasing mindfulness and psychological flexibility.
Limitations for the pilot study include a small sample size, the predominantly female (81%), white (65%), college-student demographics, and a lack of an active control condition. Other future studies may also investigate the applicability of MH to a wider range of presenting concerns, such as depression, chronic pain, or externalizing problems. In addition, it may be possible to adapt MH into a group intervention or briefer audio-recording intervention, which would be a distinct advantage in treatment settings with high demand for services.
In conclusion, mindful hypnotherapy shows promise for being an effective intervention for decreasing stress. Given that the results for mindfulness and psychological flexibility were comparable or superior to mindfulness interventions delivered in a nonhypnotic context, this novel intervention shows potential for being a unique and a valuable contribution to stress reduction interventions. There is a critical need for more effective treatments for stress, and, given the promising findings for MH, future research using this intervention is strongly indicated.
Disclosure Statement
No potential conflict of interest was reported by the authors.
References
- Alladin, A. (2014). Mindfulness-based hypnosis: Blending science, beliefs, and wisdoms to catalyze healing. American Journal of Clinical Hypnosis, 56(3), 285–302. doi:https://doi.org/10.1080/00029157.2013.857290
- Bandelow, B., & Michaelis, S. (2015). Epidemiology of anxiety disorders in the 21st century. Dialogues in Clinical Neuroscience, 17(3), 327.
- Benjamini, Y., Drai, D., Elmer, G., Kafkafi, N., & Golani, I. (2001). Controlling the false discovery rate in behavior genetics research. Behavioural Brain Research, 125(1–2), 279–284. doi:https://doi.org/10.1016/S0166-4328(01)00297-2
- Bond, F. W., Hayes, S. C., Baer, R. A., Carpenter, K. M., Guenole, N., Orcutt, H. K., & Zettle, R. D. (2011). Preliminary psychometric properties of the acceptance and action questionnaire–II: A revised measure of psychological inflexibility and experiential avoidance. Behavior Therapy, 42(4), 676–688. doi:https://doi.org/10.1016/j.beth.2011.03.007
- Carlson, L. E., Speca, M., Faris, P., & Patel, K. D. (2007). One year pre–post intervention follow-up of psychological, immune, endocrine and blood pressure outcomes of mindfulness-based stress reduction (MBSR) in breast and prostate cancer outpatients. Brain, Behavior, and Immunity, 21(8), 1038–1049. doi:https://doi.org/10.1016/j.bbi.2007.04.002
- Cohen, S., & Williamson, G. (1988). Perceived stress in a probability sample of the U.S. In S. Spacapam & S. Oskamp (Eds.), The social psychology of health: Claremont symposium on applied social psychology (pp. 31–67). Newbury Park, CA: Sage.
- Elkins, G. R. (2014). Hypnotic relaxation therapy: Principles and applications. New York, NY: Springer.
- Elkins, G. R., Barabasz, A. F., Council, J. R., & Spiegel, D. (2015). Advancing research and practice: The revised APA Division 30 definition of hypnosis. International Journal of Clinical and Experimental Hypnosis, 63(1), 1–9. doi:https://doi.org/10.1080/00207144.2014.961870
- Elkins, G. R., Fisher, W. I., Johnson, A. K., Carpenter, J. S., & Keith, T. Z. (2013). Clinical hypnosis in the treatment of post-menopausal hot Flashes: A randomized controlled trial. Menopause, 20(3), 291–298. doi:https://doi.org/10.1097/gme.0b013e31826ce3ed
- Elkins, G. R., & Johnson, A. (2015). Psychological distress profile. Menlo Park, CA: Mind Garden, Inc.
- Elkins, G. R., & Olendzki, N. (2019). Mindful hypnotherapy: The basics for clinical practice. New York, NY: Springer Publishing Company, LLC.
- Elkins, G. R., Roberts, R. L., & Simicich, L. (2018). Mindful self-hypnosis for self-care: An integrative model and illustrative case example. American Journal of Clinical Hypnosis, 61(1), 45–56. doi:https://doi.org/10.1080/00029157.2018.1456896
- Forman, E. M., Herbert, J. D., Moitra, E., Yeomans, P. D., & Geller, P. A. (2007). A randomized controlled effectiveness trial of acceptance and commitment therapy and cognitive therapy for anxiety and depression. Behavior Modification, 31(6), 772–799. doi:https://doi.org/10.1177/0145445507302202
- Forte, M., Brown, D., & Dysart, M. (1987). Differences in experience among mindfulness meditators. Imagination, Cognition and Personality, 7(1), 47–60. doi:https://doi.org/10.2190/53EL-UTVW-DN4T-F60D
- Golden, W. L. (2012). Cognitive hypnotherapy for anxiety disorders. American Journal of Clinical Hypnosis, 54(4), 263–274. doi:https://doi.org/10.1080/00029157.2011.650333
- Grant, J. A. (2012). Towards a more meaningful comparison of meditation and hypnosis. Journal of Mind-Body Regulation, 2(1), 71–74.
- Grossman, P., Niemann, L., Schmidt, S., & Walach, H. (2004). Mindfulness-based stress reduction and health benefits: A meta-analysis. Journal of Psychosomatic Research, 57(1), 35–43. doi:https://doi.org/10.1016/S0022-3999(03)00573-7
- Grossman, P., Tiefenthaler-Gilmer, U., Raysz, A., & Kesper, U. (2007). Mindfulness training as an intervention for fibromyalgia: Evidence of postintervention and 3-year follow-up benefits in well-being. Psychotherapy and Psychosomatics, 76(4), 226–233. doi:https://doi.org/10.1159/000101501
- Grover, M. P., Jensen, M. P., Patterson, D. R., Gertz, K. J., & Day, M. A. (2018). The association between mindfulness and hypnotizability: Clinical and theoretical implications. American Journal of Clinical Hypnosis, 61(1), 4–17. doi:https://doi.org/10.1080/00029157.2017.1419458
- Hayes, S. C., & Wilson, K. G. (1994). Acceptance and commitment therapy: Altering the verbal support for experiential avoidance. Behavior Analyst, 17(2), 289–303. doi:https://doi.org/10.1007/BF03392677
- Hofmann, S. G., Sawyer, A. T., Witt, A. A., & Oh, D. (2010). The effect of mindfulness-based therapy on anxiety and depression: A meta-analytic review. Journal of Consulting and Clinical Psychology, 78(2), 169–183. doi:https://doi.org/10.1037/a0018555
- Kabat-Zinn, J. (1982). An outpatient program in behavioral medicine for chronic pain patients based on the practice of mindfulness meditation: Theoretical considerations and preliminary results. General Hospital Psychiatry, 4(1), 33–47. doi:https://doi.org/10.1016/0163-8343(82)90026-3
- Kabat-Zinn, J. (1994). Wherever you go, there you are: Mindfulness meditation in everyday life. New York, NY: Hyperion.
- Khoury, B., Lecomte, T., Fortin, G., Masse, M., Therien, P., Bouchard, V., … Hofmann, S. G. (2013). Mindfulness-based therapy: A comprehensive meta-analysis. Clinical Psychology Review, 33(6), 763–771. doi:https://doi.org/10.1016/j.cpr.2013.05.005
- Kirsch, I., Montgomery, G., & Sapirstein, G. (1995). Hypnosis as an adjunct to cognitive-behavioral psychotherapy: A meta-analysis. Journal of Consulting and Clinical Psychology, 63(2), 214–220. doi:https://doi.org/10.1037/0022-006X.63.2.214
- Linehan, M. M. (1987). Dialectical behavioral therapy: A cognitive behavioral approach to parasuicide. Journal of Personality Disorders, 1(4), 328–333. doi:https://doi.org/10.1521/pedi.1987.1.4.328
- Lynn, S. J., Barnes, S., Deming, A., & Accardi, M. (2010). Hypnosis, rumination, and depression: Catalyzing attention and mindfulness-based treatments. International Journal of Clinical and Experimental Hypnosis, 58(2), 202–221. doi:https://doi.org/10.1080/00207140903523244
- Lynn, S. J., Malaktaris, A., Maxwell, R., Mellinger, D. I., & van der Kloet, D. (2012). Do hypnosis and mindfulness practices inhabit a common domain? Implications for research, clinical practice, and forensic science. Journal of Mind-Body Regulation, 2(1), 12–26.
- Lynn, S. J., Surya Das, L., Hallquist, M. N., & Williams, J. C. (2006). Mindfulness, acceptance, and hypnosis: Cognitive and clinical perspectives. International Journal of Clinical and Experimental Hypnosis, 54(2), 143–166. doi:https://doi.org/10.1080/00207140500528240
- Manicavasgar, V., Parker, G., & Perich, T. (2011). Mindfulness-based cognitive therapy vs cognitive behaviour therapy as a treatment for non-melancholic depression. Journal of Affective Disorders, 130(1–2), 138–144. doi:https://doi.org/10.1016/j.jad.2010.09.027
- McLean, C. P., Asnaani, A., Litz, B. T., & Hofmann, S. G. (2011). Gender differences in anxiety disorders: Prevalence, course of illness, comorbidity and burden of illness. Journal of Psychiatric Research, 45(8), 1027–1035. doi:https://doi.org/10.1016/j.jpsychires.2011.03.006
- Miller, J. J., Fletcher, K., & Kabat-Zinn, J. (1995). Three-year follow-up and clinical implications of a mindfulness meditation-based stress reduction intervention in the treatment of anxiety disorders. General Hospital Psychiatry, 17(3), 192–200. doi:https://doi.org/10.1016/0163-8343(95)00025-M
- Öst, L. G. (2008). Efficacy of the third wave of behavioral therapies: A systematic review and meta-analysis. Behaviour Research and Therapy, 46(3), 296–321. doi:https://doi.org/10.1016/j.brat.2007.12.005
- Otani, A. (2016). Hypnosis and mindfulness: The Twain finally meet. American Journal of Clinical Hypnosis, 58(4), 383–398. doi:https://doi.org/10.1080/00029157.2015.1085364
- Piet, J., Würtzen, H., & Zachariae, R. (2012). The effect of mindfulness-based therapy on symptoms of anxiety and depression in adult cancer patients and survivors: A systematic review and meta-analysis. Journal of Consulting and Clinical Psychology, 80(6), 1007–1020. doi:https://doi.org/10.1037/a0028329
- Powers, M. B., Vörding, M. B., & Emmelkamp, P. M. (2009). Acceptance and commitment therapy: A meta-analytic review. Psychotherapy and Psychosomatics, 78(2), 73–80. doi:https://doi.org/10.1159/000190790
- Roberti, J. W., Harrington, L. N., & Storch, E. A. (2006). Further psychometric support for the 10‐item version of the perceived stress scale. Journal of College Counseling, 9(2), 135–147. doi:https://doi.org/10.1002/(ISSN)2161-1882
- Sabourin, M. E., Cutcomb, S. D., Crawford, H. J., & Pribram, K. (1990). EEG correlates of hypnotic susceptibility and hypnotic trance: Spectral analysis and coherence. International Journal of Psychophysiology, 10(2), 125–142. doi:https://doi.org/10.1016/0167-8760(90)90027-B
- Schoenberger, N. E., Kirsch, I., Gearan, P., Montgomery, G., & Pastyrnak, S. L. (1998). Hypnotic enhancement of a cognitive behavioral treatment for public speaking anxiety. Behavior Therapy, 28(1), 127–140. doi:https://doi.org/10.1016/S0005-7894(97)80038-X
- Stein, D. J., Scott, K. M., de Jonge, P., & Kessler, R. C. (2017). Epidemiology of anxiety disorders: From surveys to nosology and back. Dialogues in Clinical Neuroscience, 19(2), 127–136.
- Teasdale, J. D., Segal, Z. V., Williams, J. M. G., Ridgeway, V. A., Soulsby, J. M., & Lau, M. A. (2000). Prevention of relapse/recurrence in major depression by mindfulness-based cognitive therapy. Journal of Consulting and Clinical Psychology, 68(4), 615–623. doi:https://doi.org/10.1037/0022-006X.68.4.615
- Walker, W. L. (2016). Guidelines for the use of hypnosis: When to use hypnosis and when not to use. Australian Journal of Clinical and Experimental Hypnosis, 41(1), 41–53.
- Walrath, L. C., & Hamilton, D. W. (1975). Autonomic correlates of meditation and hypnosis. American Journal of Clinical Hypnosis, 17(3), 190–197. doi:https://doi.org/10.1080/00029157.1975.10403739
Appendix A
Detailed Summary of the Mindful Hypnotherapy Intervention
Week 1: Intake and Focusing on the Present Moment
Hypnosis was introduced, including misconceptions about hypnosis. Individual information was also collected as necessary for personalizing hypnosis. In the final portion of the didactic part of the session, mindfulness was briefly introduced, with an emphasis on present-moment awareness.
Hypnotic Induction. The hypnotic induction for session one consisted of suggestions for “centering” oneself via present-moment awareness of raw sense-data such as sounds, bodily sensations, and visual stimuli. The hypnotic induction included post-hypnotic suggestions for being able to do this easily in times of stress. At the conclusion of the session, the participant was provided with a home practice CD for session one.
Week 2: Nonjudgmental Awareness of Bodily Sensations
At the beginning of the session home practice was reviewed, and there was a discussion regarding how well material from the previous week had been integrated into the client’s life. New material began with psychoeducation regarding how the body responds to stressors. Next, mindfulness was explained with an emphasis on present-moment awareness of bodily sensations, and the client was encouraged to cultivate an awareness of these sensations without judging them as “good” or “bad”.
Hypnotic Induction. The hypnosis portion of session two focused on present-moment awareness of bodily sensations, without judgment. Post-hypnotic suggestions were given for regular practice and integrating mindful awareness of the body into daily life. At the conclusion of the session, the participant was provided with a home practice CD for session two.
Week 3: Mindfulness of Thoughts and Emotions
In this session, the concept of mindfulness was elaborated upon by building on previous sessions. After reviewing home practice and any questions that have arisen in integrating the previous week’s material, new material was added. Whereas the focus for session two was nonjudgmental awareness of physical sensations (that is, anything perceptible with the five senses), in session three this same attitude was practiced with regard to thoughts and emotions. As with all sessions, these mindfulness skills were applied to the client’s individual stressors and needs.
Hypnotic Induction. The hypnosis portion of session three focused on a guided experience of becoming mindfully aware of thoughts and emotions. In session, participants were asked to become aware of a mild or moderately stressful recent event and were then guided through being mindfully aware of the stress. Post-hypnotic suggestions were given for daily mindfulness of thought and emotion, as well as dealing with stress mindfully on a daily basis. At the conclusion of the session, the participant was provided with a home practice CD for session three, and in the audio for session three participants are encouraged to pay attention to whatever thoughts and feelings arise, without needing to control or respond. This general awareness of emotion takes the place of the suggestion for awareness of stress that occurs during the in-vivo script but is otherwise identical.
Week 4: Integrating Self-Hypnosis into Mindfulness-Based Hypnotherapy
As usual, home practice and any obstacles to practice were discussed, following which the participant was instructed on the principles of self-hypnosis. Where appropriate, self-suggestions can be tailored to the participant’s particular needs. For example, someone who has a preference for using sound to enter a hypnotic trance can use sound, and someone who has a preference for paying attention to the sensations of breathing to enter trance can do that instead.
Hypnotic Induction. Session four included two hypnotic inductions. The first induction included detailed instruction, guiding the participant through each step of hypnosis and naming each step of self-hypnosis as it is performed. The second hypnosis session included the name of each step and minimal guidance, relying upon the subject to guide himself or herself through the experience of hypnosis in their own way. At the conclusion of the session, the participant was provided with a home practice CD for session four.
Week 5: Compassion for Self and Others
In this session, the new material involved exploring examples of how stress can be made worse with self-reprisals, self-hatred, or a lack of self-compassion and introduces self-compassion as a useful attitude. Like the concept of acceptance, this is an attitudinal shift and does not necessarily include a shift in behavior. The clinician explored with the participant any reservations they may have in cultivating greater self-compassion as well as specific areas of their life when self-compassion may be particularly difficult to practice.
Hypnotic Induction. After suggestions for relaxation and deepening trance, the participant was guided to bring to mind someone who has acted with benevolence and love toward them (parent, mentor, God, etc.) and allow natural thoughts and feelings of goodwill and compassion to extend toward this person. Suggestions were then given for experiencing that same compassion toward a neutral party, someone with whom it is difficult to get along, and also toward themselves. Post-hypnotic suggestions were given to enable them to experience this frequently during the week and recall it at will in times of stress. Finally, the participant was provided with a “Mindful Self-Compassion” home practice CD for session five.
Week 6: Hypnotherapy for Acceptance and Awareness of Values
As with previous sessions home practice and any obstacles to practice were reviewed, and the participant was reminded of material from the previous sessions to give context to the new material. The participant’s values and sense of meaning in life were explored, as well as the extent to which the participant has been acting congruently with these values and pursuing a meaningful life. If the participant’s life and values had been congruent, the session focused on how MH can support and deepen this lifestyle while becoming more appreciative of the meaning that is already present in life. If incongruence was found, obstacles to congruence were identified and newly-learned MH skills were brought to bear in overcoming these obstacles.
Hypnotic Induction. Hypnotic suggestions for session six focused on the participant’s individual values and sources of meaning in life. Suggestions were given for an enhanced sense of meaning and dedication to personal values based on the participant’s earlier description, integrating principles of mindfulness as appropriate to support the participant’s congruence with these values and pursuit of personally meaningful life goals.
Week 7: Individualization of Mindfulness-Based Hypnotherapy
Before the session began, home practice and any obstacles to practice were reviewed. Next was a discussion of the client’s progress in integrating mindfulness into daily life (outside of formal practice) and mindfulness concepts that the participant was having trouble understanding or integrating were reinforced with further education and discussion. The bulk of this session was used to individualize MH and focus on areas that have been particularly difficult for the participant to integrate or understand.
Hypnotic Induction. The hypnosis session for session seven was an integrated mindfulness induction focused on the participant’s individual goals and needs. A script for session seven was provided, with the stipulation that individual suggestions should be integrated as needed into this script in order to reinforce the client’s individual goals and address any lingering shortcomings to mindfulness practice. Finally, the participant was provided with the “Integrated Mindfulness-Based Hypnosis” home practice CD.
Week 8: Termination and Transition to Long-Term Practice
Before the session began, home practice and any obstacles to practice were reviewed. This session was devoted to the therapeutic tasks of termination. For example, the participant’s progress over the course of the past eight weeks was reviewed, highlighting reductions in stress or other positive effects (if present) and the changes in perception and attitude that allowed the participant to make these positive life changes. If the participant struggled to make positive changes, the discussion focused on identifying the factors that contributed to the struggle to make changes. The therapist and client then collaborated to outline what steps could be taken to help address these obstacles in the future to enable positive change. Finally, if MH was helpful to the participant, strategies were discussed that would enable the participant to continue MH practice with self-hypnosis in order to maintain positive gains.
Hypnotic Induction. In this termination session, hypnotic suggestions for relaxation and present-moment, nonjudgmental awareness were given. This awareness included an awareness of thoughts, sensations, and emotions without trying to “push” any of these experiences away nor hold on to them. Instead, the participant was guided toward becoming aware of the present moment with equanimity and compassion/self-compassion. Post-hypnotic suggestions were given for the long-term continuation of daily MH practice (including both formal and informal practice) as well as integrating mindfulness as a trait and an easily accessed state of mind.