ABSTRACT
Importance
Severe traumatic brain injury (sTBI) is a critical health problem in regions of limited resources (RLRs). Younger populations are among the most impacted. The objective of this review is to analyze recent consensus-based algorithms, protocols and guidelines proposed for the care of patients with TBI in RLRs.
Observations
The principal mechanisms for sTBI in RLRs are road traffic injuries (RTIs) and violence. Limitations of care include suboptimal or non-existent pre-hospital care, overburdened emergency services, lack of trained human resources, and surgical and intensive care. Low-cost neuromonitoring systems are currently in testing, and formal neurotrauma registries are forming to evaluate both long-term outcomes and best practices at every level of care from hospital transport to the emergency department (ED), to the operating room and intensive care unit (ICU).
Conclusions and Relevance
The burden of sTBI is highest in RLRs. As working-age adults are the predominantly affected age-group, an increase in disability-adjusted life years (DALYs) generates a loss of economic growth in regions where economic growth is needed most. Four multi-institutional collaborations between high-income countries (HICs) and LMICs have developed evidence and consensus-based documents focused on capacity building for sTBI care as a means of addressing this substantial burden of disease.
Introduction
Regions with limited resources (RLRs) generally have high unemployment rates, social inequality and unfair distribution of wealth, low educational level and weak health-care systems. Many of these conditions lead to poor health infrastructure and poor compliance with existing laws, and they help explain why the prevalence of severe traumatic brain injury (sTBI) continues to increase in low- and middle-income countries (LMICs), where RLRs remain more common than their high-income country (HIC) counterparts (Citation1,Citation2). According to a recent analysis of global neurosurgery academic groups, more than two-thirds of the world’s population has gaps in the provision of appropriate surgical and anesthetic care(Citation3). There are an estimated 13.8 million potential neurosurgical cases every year worldwide, with more than 80% occurring in LMICs(Citation4). It has also been calculated that nearly 45% of the total neurosurgical cases are related to traumatic brain injury (TBI) care, including burr holes, craniotomies, and craniectomies(Citation4).
The Global Burden of Disease Study 2019 reports that road injuries remain the leading cause of death in the 10–24 and 25–49 age groups(Citation5), especially in countries with a low socio-demographic index (SDI), measured by a combination of personal income, educational attainment, and total fertility rate and considered a strong indicator of a country’s development and poverty level(Citation6). Recent modeling suggests that nearly 69 million people sustain a TBI each year, of which the highest incidences map to RLRs in Africa, Latin America, and South-East Asia(Citation3). While HICs have nearly 18 million cases, LMICs have around 50 million cases, a nearly 3-fold increase in both cases and mortality (Citation4,Citation7).
This data matters because in RLRs, pre-hospital care of sTBI is highly variable, and in some cases, inexistent. Resources vary substantially across hospitals, with limited or no CT imaging capacity, neurosurgery services or intensive care units (ICU). With the disproportionately high burden of neurotrauma disease in LMICs, neurotrauma is a highly technical and complex subspecialty in these geographic areas where it is most needed. It is not uncommon to see formal fellowship training programs in endovascular or spine neurosurgery in LMICs, with an absence of neurotrauma specific training (Citation8,Citation9). In these countries, the national burden of neurotrauma has an incidence of 800 to 939 cases for every 100,000 people. This, in contrast to the incidence of aneurysms and cervical stenosis in these countries as 3.4 to 6.9 cases for every 100,000 and 2.3 to 3.4 cases for every 100,000, respectively (Citation3,Citation10,Citation11).
The objective of this review was to review recent algorithms, protocols, and guidelines for improving the care of patients with sTBI in specific RLR contexts.
Methods
We carried out a systematic search using specific search terms in PubMed, EMBASE, ProQuest, and LILACS as described in the supplementary file. We also performed free-text searches for keywords like, “traumatic brain injury” AND “consensus” OR “guidelines” OR “protocols” AND “low-and middle-income countries” in Google Scholar. We also used these search terms to scan international websites of groups working in this discipline, like the Global Health Research Group in Neurotrauma at the University of Cambridge (NIHR-UK), the Benchmark Evidence from South American Trials at the University of Washington (NIH-USA), the Program in Global Surgery and Social Change in the Department of Global Health and Social Medicine at Harvard Medical School (USA) and others. Finally, we reviewed the references of articles selected through our search strategy to identify additional pertinent citations. In this review, we included all relevant articles describing the development of algorithms, protocols, or guidelines for the management of patients with sTBI designed for application in RLRs.
Inclusion criteria: algorithms, protocols, or guidelines for the management of sTBI in RLRs developed by inter-institutional and interdisciplinary teams in addition to collaborations between HIC and LMIC practitioners.
Results
The search identified 1903 publications, of which six fulfilled the inclusion criteria (Citation12–17). Three additional publications were found, which did not fulfill all inclusion criteria, but were found to be useful, of which one focused on neuromonitoring in emerging economies (not specific for patients with sTBI)(Citation18), another with a definite recommendation for performing a decompressive craniectomy in patients with sTBI in low-resource settings(Citation19), and lastly, one which provided comprehensive policy recommendations for head and spine injury care in LMICs(Citation20).
A comparative analysis of the six publications which met all inclusion criteria is presented in , including the scope, developing team and algorithms, and protocols or guideline recommendations.
Table 1. Comparative analysis between the 5 publications presenting algorithms, protocols or guidelines for the management of sTBI patients in the context of RLRs. CT (computed tomography), ICU (intensive care unit, TBI (Traumatic Brain Injury), AGREE (appraisal of guidelines for research & evaluation instrument), PICO (population, intervention, comparison, outcome scheme for developing evidence based questions)
Overall, these six documents present the evolution of recommendations for the management of sTBI in RLRs. The Neurosurgical Australasian Society developed the first of these recommendations(Citation12). The guidelines were initially published in 1992 and updated in 2000 and most recently in 2009 for the management of acute neurotrauma in rural and remote locations in the Pacific island region. The society developed the guidelines using data from clinical and surgical case series performed in the 80s and early 90s when neurosurgeons’ access to essential neurosurgical equipment was limited to instruments like the Hudson brace to perform burr-holes to facilitate necessary decompression in rural settings. The guidelines relied upon possibilities of communication by the primary health-care facility and the remote neurosurgery service in order to define additional measures like hyperventilation or hyperosmolar therapy with mannitol (standard therapies at that time). The guidelines present useful schemes for anatomical localization of neurosurgical procedures, including specific protocols for medical interventions and recommendations for pediatric and spine trauma cases.
In 2014, two guidelines were developed for LMICs. One was a multi-institutional collaboration between several medical associations from India and the United States(Citation13). This consensus-based document offers a public health system perspective, presenting recommendations for prevention, facilities, infrastructure, and pre-hospital, in-hospital and rehabilitation care. General recommendations for airway management, ventilation, blood pressure management, CT scanning and ICP monitoring are presented, describing specific medical therapies and providing general algorithms.
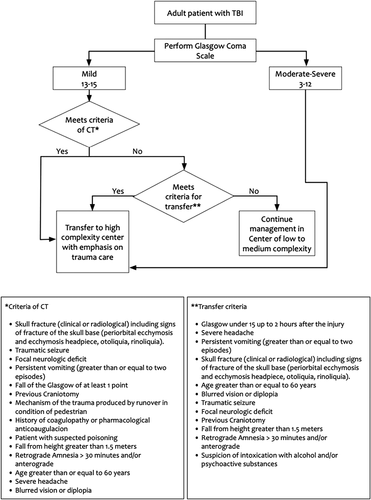
In the same year, the Colombian Clinical Practice Guidelines for the Management of Severe Traumatic Brain Injury in Adult Patients was published as a technical document by the Colombian Ministry of Health(Citation15). This was a multi-institutional, evidence-based, and consensus-based exercise supported by international methodological advisors like the Cochrane Collaboration. Following a strict GRADE (Grading of Recommendations Assessment, Development and Evaluation) methodology, ten structured PICO (population, intervention, comparison, and outcome) type questions were answered using different clinical studies with low to a high quality of evidence. The questions designed to evaluate heterogeneity of practice among different TBI care providers are shown in . Recommendations were developed for each question, along with specific algorithms to offer guidance specific to RLRs. An example of the algorithm for referral of patients with TBI from low resources facilities to high resources facilities is presented in .
Table 2. List of questions for answering with GRADE methodology in the Clinical Practice Guidelines exercise of the Colombian Ministry of Health
In 2020, the updated version of the 2012 Benchmark Evidence from South American Trials: BEST-TRIP study protocol, for the management of patients with sTBI without ICP monitoring and based on clinical examination and CT imaging was published with a new acronym called “Protocol for the Treatment of Severe Traumatic Brain Injury Based on Imaging and Clinical Examination for Use When Intracranial Pressure Monitoring Is Not Employed (CREVICE)”(Citation10). The protocol, based on an expert consensus approach, includes three levels of interventions and additional recommendations for patient monitoring, general measures, goals for cerebral perfusion and oxygenation treatment and for escalation or tapering therapies. This protocol also includes heat maps for withdrawing sedation therapy in ICU for patients with sTBI in the first 24 to 72 or more hours of hospital stay. The major and minor criteria for defining high ICP in the absence of ICP monitoring of the CREVICE protocol are presented in .
An innovative approach for protocol development for the management of patients with sTBI in different levels of resource contexts was also published in 2020. This stratified process was named “Beyond One Option for Treatment of Traumatic Brain Injury: A Stratified Protocol (BOOTStraP).”(Citation14) BOOTStraP offers ten protocols to facilitate interactions from shallow resource scenarios to high-resource scenarios. The users of the protocols can choose the preferred treatment option according to the level of resources available and then move to another treatment option if resources increase or decrease. This is a common situation in daily practice for many RLR practitioners. The protocols specifically include recommendations for basic or advanced emergency transportation (pre-hospital level); low-, middle-, or high-resourced emergency rooms, defined by the availability of CT scanning capabilities; recommendations for managing patients in centers without neurosurgical services or with neurosurgical services but without ICU availability; and recommendations for centers with low-resource, intermediate postoperative units or centers with full ICU capabilities. All ten protocols are available open-access at https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7055642/bin/10-1055-s-0040-1701370_00284_s1.pdf
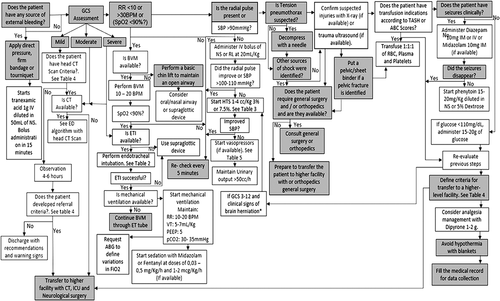
An example of an algorithm for the management of sTBI in emergency settings with a low level of resources is presented in .
A group of Latin American critical care physicians and neurosurgeons, most of whom were involved in the development of the CREVICE protocol, developed another consensus guideline document in 2020, which focused on general care measures for patients with sTBI. The document provides updated recommendations on general UICU measures like head positioning, use of cervical collars, mouth hygiene, eye protection and management of artificial airways. Additional recommendations were generated for fluid resuscitation, blood pressure optimization, management of body temperature, and thresholds for hemoglobin, glycemia, sodium, and sedation levels(Citation17).
There is a pressing need to define protocols and guidelines tailored regions with different degrees of resource limitations (Citation21–24). Integrating the recommendations from these six documents opens a unique set of possibilities for developing a structured sTBI care pathway in RLRs.
Additional recommendations have been proposed from the public policy perspective. A document from the Program in Global Surgery and Social Change of the Harvard Medical School includes a six-component approach for building technical strategies in LMICs where neurotrauma is poorly organized as part of the healthcare system. The first component is related to recommendations for infrastructure (surgical facilities, facility readiness, and blood supply and referral systems) (Citation20,Citation25). The second set of recommendations is oriented toward workforce (surgical, anesthesia and obstetric providers, including other allied health providers). The third set is focused on service delivery (including aspects related to surgical volume, system coordination and quality and safety). The fourth set of recommendations is related to financing aspects (health financing and accounting, including budget allocation). The fifth and sixth sets of recommendations are related to information management (information systems, data streams and local research agendas), and governance (policy and political architecture to improve visibility and accountability). These aspects have been considered pivotal in order to establish organized neurotrauma care systems, especially in RLRs.
Protocols for the management of sTBI in RLRs can be refined using lessons learned from military protocols applied to civilian settings (Citation26,Citation27). Reliance on serial physical examinations (including basic neurological exams), optimizing the use of portable devices for intracranial bleeding detection(Citation28), evaluation of intracranial hypertension with noninvasive portable devices (Citation29,Citation30), and early aggressive surgical management with specific decision-making ethics-based algorithms are good examples (Citation31–33). Furthermore, neurotrauma registries have recently been developed to advance research in sTBI across RLRs (Citation34–42). Analysis of data from these registries will be invaluable when evaluating the impact of future protocol modifications on the outcome of patients with sTBI.
Conclusion
The burden of sTBI is highest in RLRs, where it remains a significant cause of death, severe disability, and productivity loss. Several collaborations between HICs and LMICs have developed tailored algorithms, protocols and guidelines to improve the quality of sTBI care in RLRs. Neurotrauma registries in RLRs provide new valuable sources of information to study the impact of applying specific care protocols to practice. Innovation on portable and noninvasive technology for diagnosis and monitoring of sTBI promises to offer new possibilities to reduce the enormous personal and societal losses from sTBI in RLRs.
Disclosure Statement
All authors contributed equally to the development and writing of this manuscript
Dr. Jibaja, Dr. Godoy, Dr. Rubiano, Mr. Griswold and Dr. Rabinstein declare no conflict of interest. None have received financial support or any fees to write this manuscript.
Dr. Rubiano is supported by the Global Health Research Group in Neurotrauma of the University of Cambridge. Grant of the National Institute of Health Research using Official Development Assistance (ODA) funding. Mr Griswold is supported by the Gates Cambridge Trust. The views expressed in this publication are those of the author(s) and not necessarily those of the NHS, National Institute for Health Research or the Department of Health.
All authors have completed the ICMJE uniform disclosure form and declare: no support from any organisation for the submitted work; no financial relationships with any organisations that might have an interest in the submitted work in the previous three years, no other relationships or activities that could appear to have influenced the submitted work. The lead author affirms that this manuscript is an honest, accurate, and transparent account of the study being reported; that no important aspects of the study have been omitted; and that any discrepancies from the study as planned (and, if relevant, registered) have been explained.
Additional information
Funding
References
- Acharya KP, Pathak S Applied Research in Low-Income Countries: why and How? Frontiers Res Metrics Anal 2019;4:3. https://doi.org/10.3389/frma.2019.00003.
- James SL, Theadom A, Ellenbogen RG, GBD 2016 Traumatic Brain Injury and Spinal Cord Injury Collaborators. Global, regional, and national burden of traumatic brain injury and spinal cord injury, 1990–2016: a systematic analysis for the Global Burden of Disease Study 2016. Lancet Neurology. 2019;18(1):56–87. doi:https://doi.org/10.1016/s1474-4422(18)30415-0.
- Dewan MC, Rattani A, Fieggen G, Arraez MA, Servadei F, Boop FA, Johnson WD, Ward BC, Park KB. Global neurosurgery: the current capacity and deficit in the provision of essential neurosurgical care. Executive Summary of the Global Neurosurgery Initiative at the Program in Global Surgery and Social Change. J Neurosurg. 2019;130(4):1055–64. doi:https://doi.org/10.3171/2017.11.jns171500.
- Dewan MC, Rattani A, Gupta S, Baticulon RE, Hung YC, Punchak M, Agrawal A, Adeleye AO, Shrime MG, Rubiano AM. et al. Estimating the global incidence of traumatic brain injury. J Neurosurg. 2019;130(4):1080–97. doi:https://doi.org/10.3171/2017.10.jns17352.
- Collaborators G. Global burden of 369 diseases and injuries in 204 countries and territories, 1990–2019: a systematic analysis for the Global Burden of Disease Study 2019. Lancet. 2019;396(10258):1204–22. D and I, Vos T, Lim SS, et al. 2020. doi:https://doi.org/10.1016/s0140-6736(20)30925-9.
- Collaborators G. Global age-sex-specific fertility, mortality, healthy life expectancy (HALE), and population estimates in 204 countries and territories, 1950–2019: a comprehensive demographic analysis for the Global Burden of Disease Study 2019. Lancet. 2019;396(10258):1160–203. D Wang H, Abbas KM, et al. 2020. doi:https://doi.org/10.1016/s0140-6736(20)30977-6.
- Iaccarino C, Carretta A, Nicolosi F, Morselli C 2018. Epidemiology of severe traumatic brain injury. J Neurosurg Sci. 62(5):535–41. doi:https://doi.org/10.23736/s0390-5616.18.04532-0
- Africa Ao. AOspine South African Long-Term Fellowship—Guidelines.; 2016. https://www.headandnecktrauma.org/wp-content/uploads/2016/06/NEW_Fellowship20guidelines20ZA.pdf
- Medicasur: Curso de Alta Especialidad En Enfermedad Vascular Cerebral, 2018 https://Www.Medicasur.Com.Mx/Es_mx/Ms/Curso-Alta-Especialidad-Enfermedad-Vascular-Cerebral [Accessed October 19, 2019].; n.d.
- Ravindra VM, Senglaub SS, Rattani A, Dewan MC, Härtl R, Bisson E, Park KB, Shrime MG. Degenerative Lumbar Spine Disease: estimating Global Incidence and Worldwide Volume. Global Spine J. 2018;8(8):784–94. doi:https://doi.org/10.1177/2192568218770769.
- Hughes JD, Bond KM, Mekary RA, Dewan MC, Rattani A, Baticulon R, Kato Y, Azevedo-Filho H, Morcos JJ, Park KB. Estimating the global incidence of aneurysmal subarachnoid hemorrhage: a systematic review for central nervous system vascular lesions and meta-analysis of ruptured aneurysms. World Neurosurg. 2018;115:430–447.e7.
- Inc NS of A. The Management of Acute Neurotrauma in Rural and Remote Locations A Set of Guidelines for the Care of Head and Spinal Injuries.; 2009:30. https://dstc.com.au/wp-content/uploads/2017/02/The-Management-of-Acute-Neurotrauma-in-Rural-and-Remote-Locations.pdf
- Origin 8. American Association of South Asian Neurosurgeons/American Association of Physicians of Indian. Traumatic Brain Injury, Multi Organizational Consensus Recommendations for India. 1st Edition. ed. Bangalore, India: American Association of South Asian Neurosurgeons (AASAN); 2016.
- Rubiano AM, Vera DS, Montenegro JH, Carney N, Clavijo A, Carreño JN, Gutierrez O, Mejia J, Ciro JD, Barrios ND, et al. Recommendations of the Colombian Consensus Committee for the Management of Traumatic Brain Injury in Prehospital, Emergency Department, Surgery, and Intensive Care (Beyond One Option for Treatment of Traumatic Brain Injury: a Stratified Protocol [BOOTStraP]). J Neurosci Rural Pract. 2020;11(1):7–22. doi:https://doi.org/10.1055/s-0040-1701370.
- Health CM of. Diagnosis and Treatment of Adult Patients with Severe Traumatic Brain Injury.; 2014. http://gpc.minsalud.gov.co/gpc_sites/Repositorio/Conv_563/GPC_trauma_craneo/CPG_TBI_professionals.pdf
- Chesnut RM, Temkin N, Videtta W, Petroni G, Lujan S, Pridgeon J, Dikmen S, Chaddock K, Barber J, Machamer J, et al. Consensus-Based Management Protocol (CREVICE Protocol) for the Treatment of Severe Traumatic Brain Injury Based on Imaging and Clinical Examination for Use When Intracranial Pressure Monitoring Is Not Employed. J Neurotraum. 2020;37(11):1291–99. doi:https://doi.org/10.1089/neu.2017.5599.
- Godoy DA, Videtta W, Cruz RS, Silva X, Aguilera-Rodríguez S, Carreño-Rodríguez JN, Ciccioli F, Piñero G, Ciro JD, Re-Gutiérrez S da, et al. General care in the management of severe traumatic brain injury: latin American consensus. Med Intensiva;2020. Published online. doi: https://doi.org/10.1016/j.medin.2020.01.014.
- Monitoring TP in the IMCC on M, Figaji A, Puppo C. Multimodality Monitoring Consensus Statement: monitoring in Emerging Economies. Neurocrit Care. 2014;21(2)):239–69. doi:https://doi.org/10.1007/s12028-014-0019-3.
- Hutchinson PJ, Kolias AG, Tajsic T, Adeleye A, Aklilu AT, Apriawan T, Bajamal AH, Barthélemy EJ, Devi BI, Bhat D, et al. Consensus statement from the International Consensus Meeting on the Role of Decompressive Craniectomy in the Management of Traumatic Brain Injury: consensus statement. Acta Neurochir. 2019;161(7):1261–74. doi:https://doi.org/10.1007/s00701-019-03936-y.
- Corley J, Barthèlemy EJ, Lepard J, Alves JL, Ashby J, Khan T, Park KB. Comprehensive Policy Recommendations for Head and Spine Injury Care in Low- and Middle-Income Countries. World Neurosurg. 2019;132:434–36.
- Customizing SD 2020. Guidelines for Management of Traumatic Brain Injury. J Neurosci Rural Pract. 11(1):002–002. doi:https://doi.org/10.1055/s-0040-1701539
- Interprofessional Research PR 2020. Team Approach Is the Key to Traumatic Brain Injury Intervention. J Neurosci Rural Pract. 11(1):003–004. doi:https://doi.org/10.1055/s-0040-1701540
- Khan T, Paradigm Shift: KM 2020. From Standard-Driven Protocols to Resource-Driven Guidelines for Neurotrauma Management in Low- and Middle-Income Countries. J Neurosci Rural Pract. 11(1):5–6. doi:https://doi.org/10.1055/s-0040-1701558
- Pen AD 2020. Is Mightier than the Sword: columbia Shows the Way in Formulating Neurotrauma Guidelines. J Neurosci Rural Pract. 11(1):001–001. doi:https://doi.org/10.1055/s-0040-1701777
- School. P in GS and SChangeHM.Comprehensive Policy Recommendations for Head and Spine Injury Care in LMICs.1st Edition. Peshawar, Pakistan; 2019. https://bit.ly/3kRGzHV
- Bridges EJ, McNeill MM 2015. Trauma resuscitation and monitoring: military lessons learned. Crit Care Nurs Clin. 27(2):199–211. doi:https://doi.org/10.1016/j.cnc.2015.02.003
- JM G, PE L, Prins M, DWV W, RR M, DW M 2020. The Prehospital Evaluation and Care of Moderate/Severe TBI in the Austere Environment. Mil Med 185(1):148–53. doi:https://doi.org/10.1093/milmed/usz361
- Kontojannis V, Hostettler I, Brogan RJ, Raza M, Harper-Payne A, Kareem H, Boutelle M, Wilson M. Detection of intracranial hematomas in the emergency department using near infrared spectroscopy. Brain Injury. 2019;33(7):875–83. doi:https://doi.org/10.1080/02699052.2019.1610796.
- Jahns F-P, Miroz JP, Messerer M, Daniel RT, Taccone FS, Eckert P, Oddo M. Quantitative pupillometry for the monitoring of intracranial hypertension in patients with severe traumatic brain injury. Critical Care Lond Engl. 2019;23(1):155. doi:https://doi.org/10.1186/s13054-019-2436-3.
- Aduayi OS, Asaleye CM, Adetiloye VA, Komolafe EO, Aduayi VA 2015. Optic nerve sonography: a noninvasive means of detecting raised intracranial pressure in a resource-limited setting. J Neurosci Rural Pract. 6(4):563–67. doi:https://doi.org/10.4103/0976-3147.165347
- Rubiano AM, Maldonado M, Montenegro J, Restrepo CM, Khan AA, Monteiro R, Faleiro RM, Carreño JN, Amorim R, Paiva W, et al. The Evolving Concept of Damage Control in Neurotrauma: application of Military Protocols in Civilian Settings with Limited Resources. World Neurosurg. 2019;125:e82–e93.
- Charry JD, Rubiano AM, Puyana JC, Carney N, Adelson PD 2015. Damage control of civilian penetrating brain injuries in environments of low neuro-monitoring resources. Brit J Neurosurg. 30(2):235–39. doi:https://doi.org/10.3109/02688697.2015.1096905
- Clavijo A, Khan AA, Mendoza J, Montenegro JH, Johnson ED, Adeleye AO, Rubiano AM. . The Role of Decompressive Craniectomy in Limited Resource Environments. Front Neurol. 2019;10:112.
- Servadei F, Rossini Z, Nicolosi F, Morselli C, Park KB The Role of Neurosurgery in Countries with Limited Facilities: facts and Challenges. World Neurosurg. 2018;112:315–21. https://doi.org/10.1016/j.wneu.2018.01.047.
- Rosenfeld JV 2015. Who will perform emergency neurosurgery in remote locations? Anz J Surg 85(9):600–600. doi:https://doi.org/10.1111/ans.13207
- Kolias AG, Rubiano AM, Figaji A, Servadei F, Hutchinson PJ 2019. Traumatic brain injury: global collaboration for a global challenge. Lancet Neurology. 18(2):136–37. doi:https://doi.org/10.1016/s1474-4422(18)30494-0
- Rubiano AM, Carney N, Chesnut R, Puyana JC 2015. Global neurotrauma research challenges and opportunities. Nature. 527(7578):S193–7. doi:https://doi.org/10.1038/nature16035
- Gupta S, Khajanchi M, Kumar V, Raykar NP, Alkire BC, Roy N, Park KB. Third delay in traumatic brain injury: time to management as a predictor of mortality. J Neurosurg. 2020;132(1):289–95. doi:https://doi.org/10.3171/2018.8.jns182182.
- Punchak M, Mukhopadhyay S, Sachdev S, Hung Y-C, Peeters S, Rattani A, Dewan M, Johnson WD, Park KB. Neurosurgical Care: availability and Access in Low-Income and Middle-Income Countries. World Neurosurg. 2018;112:e240–e254.
- Johnson WD, Griswold DP 2017. Traumatic brain injury: a global challenge. Lancet Neurology. 16(12):949–50. doi:https://doi.org/10.1016/s1474-4422(17)30362-9
- Corley J, Lepard J, Barthélemy E, Ashby JL, Park KB Essential Neurosurgical Workforce Needed to Address Neurotrauma in Low- and Middle-Income Countries. World Neurosurg. 2019;123:295–99. https://doi.org/10.1016/j.wneu.2018.12.042.
- Mansouri A, Ku JC, Khu KJ, Mahmud MR, Sedney C, Ammar A, Godoy BL, Abbasian A, Bernstein M. Exploratory Analysis into Reasonable Timeframes for the Provision of Neurosurgical Care in Low- and Middle-Income Countries. World Neurosurg. 2018;117:e679–e691.