Abstract
A case of renal oncocytoma associated with focal segmental necrotizing glomerulonephritis is described. The patient showed haematuria, mild proteinuria and arterial hypertension; the diagnosis was made after right nephrectomy performed because of the presence of a renal mass. A severe re-activation of the glomerulonephritis was observed 15 months after the nephrectomy and a steroid and immunosuppressive therapy was started. Our case is the first reported in which the removal of renal oncocytoma is not followed by the disappearance of renal symptoms, as currently reported in literature, suggesting that the two diseases are not always related.
INTRODUCTION
The occurrence of glomerulonephritis in patients with neoplasia is commonly reported, and tumoral antigens have been indicated to explain immune response and renal deposition of immunoglobulins and/or complement.Citation[1] Several different histologic findings have been described quite extensively with different tumors in patients with malignancy and glomerulonephritis.Citation[2–4]
However, the association between renal oncocytoma and nephritis is a rare event. Few cases have been reported in literatureCitation[5–7], and in all of them, the removal of oncocytoma was followed by recovery from clinical and laboratory signs of nephritis.
We report a case in which the diagnosis of focal necrotizing glomerulonephritis was made after a nephrectomy performed because of a renal oncocytoma, and it was not followed by a nephrologic clinical course as benign as those of other reported oncocytomas.Citation[5–7]
CASE REPORT
A 58-year-old male was admitted to the hospital because of a renal ultrasound that had shown a right intrarenal mass. Five months before the admission, an episode of macrohematuria and fever occurred, and he was treated with antibiotic with success.
At admission, physical examination was negative, arterial blood pressure was 140/90 mmHg, and a chest radiograph was negative. Serum creatinine was 1.3 mg/dL. Urinalysis showed microhematuria (10 rbc × hpf) and mild proteinuria (100–300 mg/24 h). A computed tomography (CT) scan of the kidneys confirmed a solid enhancing mass arising from the right kidney, and a right nephrectomy was performed.
Histologic examination of the removed kidney showed that the renal mass was composed of cells with eosinophilic granular cytoplasm, and a diagnosis of oncocytoma was made (). In addition, the remaining parenchyma displayed focal necrotizing glomerulonephritis, involving about 30% of the glomeruli. Of these, 10% showed segmental necrosis of the tuft, sometimes associated with cellular or fibrocellular crescents (), while the remaining 20% displayed segmental sclerosis and/or adhesions to Bowman's capsule. Significant increase of mesangial cells and/or mesangial matrix was not evident. Arteries showed atherosclerotic lesions. There were also areas of interstitial scarring with atrophic tubules. Standard immunofluorescence and electron microscopy failed to reveal deposits.
Figure 1. Light microscopy: the renal mass was composed of cells with eosinophilic granular cytoplasm. E&E 400×.
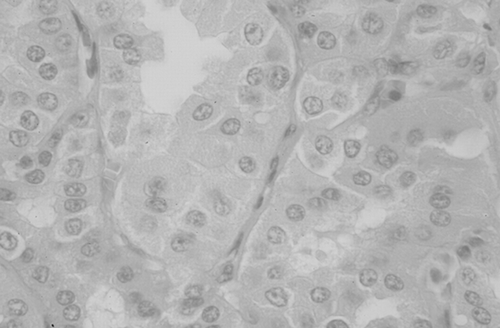
Figure 2. Light microscopy: a focal segmental necrotizing glomerulonephritis with a fibrocellular crescent was present in the renal parenchyma. PAS 200×.
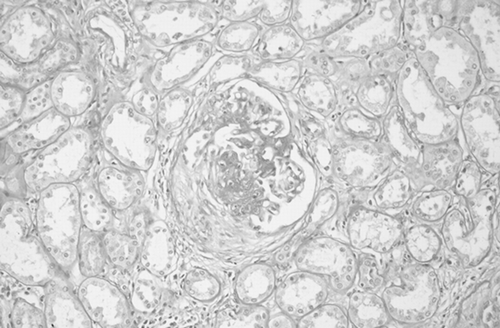
After the nephrectomy, his serum creatinine was increased to 2.1 to 2.2 mg/dL, Cystatin C 2.3 to 2.5 mg/L. Proteinuria was about 600 to 800 mg/24 h; urinalysis confirmed microhematuria but without any kind of casts. Erythrocytes sedimentation rate (ESR) was 45 mm/h.
Testing for antineutrophil cytoplasmatic antibody (ANCA) was repeatedly negative, either with indirect immunofluorescence or with enzyme-linked immunosorbent assay (ELISA).
On the basis of clinical and laboratory data and histologic findings, and being concerned by the possibility of side effects of steroids and immunosuppressive drugs, treatment of the patient was limited to ACE-inhibitor 10 mg, AT1 receptor blocker 50 mg, and dietary control.
Serum creatinine and Cystatin C remained stable for about 15 months (2–2.3 mg/dL and 2.5 mg/L, respectively); subsequently, serum creatinine went up to 4.4 mg/dL in less than a month. Urinalysis disclosed 10 to 20 red blood cells and 2 granular casts/hpf, proteinuria/24 h was 1.4 g, and immunofluorescent test for ANCA was positive for P-ANCA, whereas the ELISA test was negative.
Treatment with intravenous high doses of steroid (methylprednisolone 1 g/3 days, followed by 0.5 mg/kg/die) and cyclophosphamide (2 mg/kg/os/die) was started.
After a few weeks of therapy, serum creatinine was reduced to 3 mg/dL, and 24/h proteinuria was reduced to 1 g. After 6 months, cyclophosphamide was substituted by azathioprine; in the following weeks, an episode of cutaneous herpes zoster occurred and treatment was discontinued. During the last year, the renal function of the patient has remained stable, and his serum creatinine is still around 3 mg/dL.
DISCUSSION
In this report, a patient affected by a renal oncocytoma and by a focal necrotizing glomerulonephritis is described. The interest of this case lies mainly in the unusual association between oncocytoma and necrotizing glomerulonephritis, and in its nephrologic clinical course. Renal oncocytoma is a capsulated tumour, which originates from tubular cells and is discovered accidentally, being usually asymptomatic; in the vast majority of cases, it bears a benign course.Citation[8],Citation[9] To the best of our knowledge, only three cases of an association between renal oncocytoma and glomerulonephritis have been reported: an elderly man with vasculitis,Citation[5] a man with minimal change nephropathy,Citation[6] and a membranous nephropathy in a renal transplant. Citation[7] In these reports, the removal of oncocytoma was followed by complete recovery of the clinical picture. Although a clear relationship between oncocytoma and glomerulonephritis is not evident, the authors suggest a possible link referring to an immunologic stimulus (antigen/s) coming from the neoplastic cells.Citation[5–7]
In our case, the whole clinical picture was probably due to necrotizing vasculitis.
We had also evidence that oncocytoma and glomerulonephritis were not related. The presence of ANCA in the serum of patients with paraneoplastic vasculitis has been well described;Citation[10–13] however, in our patient, ANCA were positive only in an immunofluorescence test performed 15 months after nephrectomy, whereas they were repeatedly negative immediately after the diagnosis of vasculitis was made. A positive ANCA test with immunofluorescence associated with a negative ELISA test, in the same sample, has been already reported and could suggest that other antigens besides antiproteinase 3 could be involved.Citation[14–16] In addition, a severe reactivation of the vasculitis was observed 15 months after nephrectomy, whereas in the cases previously reportedCitation[5–7] the removal of oncocytoma was followed by an improvement of glomerulonephritis.
The decision not to treat the patient with steroid and immunosuppressive drugs, which allowed us to observe the spontaneous trend of glomerulonephritis after the nephrectomy, was based mainly on clinical and laboratory grounds. In addition, spontaneous remissions of necrotizing glomerulonephritis have been reported in literature,Citation[17] and 50% of glomerular involvement is considered the cut-off for a more aggressive treatment.Citation[18] Having evaluated the whole kidney, we had the evidence that active glomerular involvement was about 10%.
In conclusion, we report the second case of renal oncocytoma associated with vasculitis (the fourth with glomerulonephritis) in which, however, such an association seems to be coincidental. We therefore suggest that renal oncocytoma and glomerulonephritis occurred either in close clinical connection, as previously described, but also independently, as in our experience.
REFERENCES
- Fauci AS, Haynes BF, Katz P. The spectrum of vasculitis. Clinical, pathologic, immunologic and therapeutic considerations. Ann Intern Med 1978; 89(5 pt 1)660–676, [PUBMED], [INFOTRIEVE]
- Burstein DM, Korbet SM, Schwartz MM. Membranous glomerulonephritis and malignancy. Am J Kidney Dis 1993; 22(1)5–10, [PUBMED], [INFOTRIEVE]
- Nakaya I, Iwata Y, Abe T, Yokoyama H, Oda Y, Nomura O. Malignant gastrointestinal stromal tumor originating the lesser omentum, complicated by rapidly progressive glomerulonephritis and gastric carcinoma. Intern Med 2004; 43(2)102–105, [PUBMED], [INFOTRIEVE], [CROSSREF]
- Norris SH. Paraneoplastic glomerulopathies. Semin Nephrol 1993; 13(3)258–272, [PUBMED], [INFOTRIEVE]
- Susman BR, Levin FC, Barland P, Fromowitz F. Vasculitis: associated with renal carcinoma. N Y State J Med 1981; 81: 1501–1503, [PUBMED], [INFOTRIEVE]
- Forland M, Bannayan GA. Minimal-change lesion nephritic syndrome with renal oncocytoma. Am J Med 1983; 75(4)715–720, [PUBMED], [INFOTRIEVE], [CROSSREF]
- Lian M, Mulley W, Kan K, MacGregor D, Tosolini A, Ierino F. Nephrotic range proteinuria associated with oncocytoma of the native kidney. Nephrol Dial Transplant 2004; 19(2)482–485, [PUBMED], [INFOTRIEVE], [CROSSREF]
- Klein MJ, Valensi QJ. Proximal tubular adenoma of kidney with so-called oncocytic features. A clinicopathologic study of 13 cases of a rarely reported neoplasm. Cancer 1976; 38(2)906–914, [PUBMED], [INFOTRIEVE]
- Lieber MM, Tsukamoto T. Renal oncocytoma. Tumors of the Kidney, JB de Kernion, M Pavone-Macaluso. Williams & Wilkins, Baltimore, MD 1986; 306–319
- Edgar JD, Rooney DP, McNamee P, McNeill TA. An association between ANCA-positive renal disease and malignancy. Clin Nephrol 1993; 40(1)22–25, [PUBMED], [INFOTRIEVE]
- Hruby Z, Bronowicz A, Rabczyncki J, Kopec W, Szewczyk Z. A case of severe anti-neutrophil cytoplasmatic antibody (ANCA)-positive crescentic glomerulonephritis and asymptomatic gastric cancer. Int Urol Nephrol 1994; 26(5)579–586, [PUBMED], [INFOTRIEVE]
- Hoag G. Renal cell carcinoma and vasculitis: report of two cases. J Surg Oncol 1987; 35(1)35–38, [PUBMED], [INFOTRIEVE]
- Biava CG, Gonwa TA, Naughton JL, Hopper J. Crescentic glomerulonephritis associated with nonrenal malignancies. Am J Nephrol 1984; 4(4)208–214, [PUBMED], [INFOTRIEVE]
- Schonermarc U, Lamprecht P, Csernok E, Gross WL. Prevalence and spectrum of rheumatic disease associated proteinase-3 anti-neutrophil cytoplasm antibodies (ANCA) and Myeloperoxidase ANCA. Rheumatology 2001; 40(2)178–184, [CROSSREF]
- Lai KN, Jayne DR, Brownlee A, Lockwood CM. The specificity of anti-neutrophil cytoplasm antibodies in systemic vacsulitis. Clin Exp Immunol 1990; 82(2)233–237, [PUBMED], [INFOTRIEVE]
- Bashund B, Segermark M, Wiik A, Szpirf W, Petersen J, Wieslander J. Screening for anti-neutrophil cytoplasmic antibodies (ANCA): is immunofluorescence the method of choice?. Clin Exp Immunol 1995; 99(3)350–357
- Plaisance M, Goldsmith D. Spontaneous and protracted partial remission of microscopic polyangiitis. Am J Kidney Dis 2002; 39(5)1113–1117, [PUBMED], [INFOTRIEVE], [CROSSREF]
- Heaf JG, Jorgensen F, Nielsen LP. Treatment and prognosis of extracapillary glomerulonephritis. Nephron 1983; 35(4)217–224, [PUBMED], [INFOTRIEVE]