In modern society, researchers and clinicians have focused on the significance of disturbed sleep regarding the health, psychosocial and safety-related consequences. There has been a high incidence of sleep-related breathing disorders (SRBD), which include central sleep apnea, obstructive sleep apnea (OSA), sleep related hypoventilation syndromes, and other SRBDs. Epidemiologically, adult OSA is estimated to affect 24% of men and 9% of women between 30 and 60 years of age.[Citation1]
The treatment of OSA remains an area of intense debate. Fundamentally, positive airway pressure (PAP) therapy remains the gold standard medical management for the treatment of OSA; however, other therapies (weight loss, positional therapy, myofunctional therapy,[Citation2] sleep surgery,[Citation3] and oral appliances) may improve compliance and outcomes in cases when PAP therapy is poorly tolerated, unavailable, or undesirable.
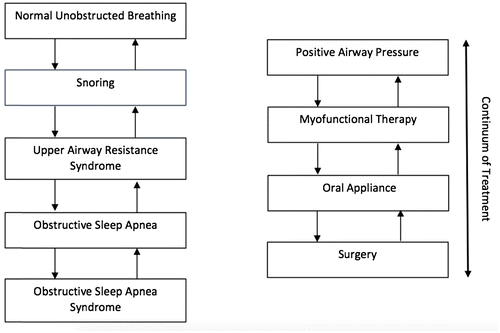
A misconception in daily practice is that surgical and non-surgical options are opposing treatments. In the academic literature, the concept of continuum of disease is used frequently as an explanation for the evolution of OSA. In this short communication, we introduce the concept of continuum of treatment. OSA treatment can be viewed as a continuum from continuous positive airway pressure (CPAP), oral appliances, and surgical treatment, based on disease severity or patient preference (Figure ). Treatments should not be excluded contingent on previous treatments, and the continuum of treatment adapts to the disease severity.
Parameters such as age, weight loss, compliance to treatment, and efficacy coupled with the increasing desire to have individualized, ‘patient-centered’ care and outcomes in chronic diseases such as OSA, can shift therapy up or down this treatment continuum. Treatment of OSA requires long-term monitoring by professionals from the multiple specialties involved. For example, in cases of nasal obstruction, nasal surgery may complement and yield improved compliance to PAP therapy [Citation4] and oral appliances. Moreover, conservative measures including weight reduction, optimizing sleep hygiene, positional therapy, and pharmacotherapy can work synergistically with more invasive therapies.[Citation5]
In summary, the continuum of treatment has never been established in the academic literature despite being empirically applied to OSA treatment. Thus, constant monitoring and re-evaluation of patients diagnosed with OSA is critical in designing an improved treatment paradigm, one that considers the concept of a treatment spectrum: the best therapeutic approach may vary over time with the disease severity.
Disclaimer
The views expressed in this manuscript are those of the authors and do not reflect the official policy or position of the Department of the Army, Department of Defense, or the US Government.
Department of Otorhinolaryngology/Sleep Medicine Centre – Hospital CUF Porto & CHEDV, Portugal; CINTESIS – Center for Research in Health Technologies and Information Systems, University of Porto, Porto, Portugal
Macario Camacho, MD
Sungjin A. Song, MD
Division of Sleep Surgery and Medicine, Department of Otolaryngology-Head and Neck Surgery, Tripler Army Medical Center, Honolulu, HI, USA
[email protected]
Robson Capasso, MD
Sleep Surgery Division, Department of Otolaryngology-Head & Neck Surgery, Stanford University School of Medicine, Stanford, CA, USA
References
- Young T, Palta M, Dempsey J, et al. The occurrence of sleep-disordered breathing among middle-aged adults. N Engl J Med. 1993;328:1230–1235.10.1056/NEJM199304293281704
- Camacho M, Certal V, Abdullatif J, et al. Myofunctional therapy to treat obstructive sleep apnea: a systematic review and meta-analysis. Sleep. 2015;38:669–675.
- Certal V, Nishino N, Camacho M, et al. Reviewing the systematic reviews in OSA surgery. Otolaryngol Head Neck Surg. 2013;149:817–829.10.1177/0194599813509959
- Camacho M, Riaz M, Capasso R, et al. The effect of nasal surgery on continuous positive airway pressure device use and therapeutic treatment pressures: a systematic review and meta-analysis. Sleep. 2015;38:279–286.
- Barry MJ, Edgman-Levitan S. Shared decision making – the pinnacle of patient-centered care. N Engl J Med. 2012;366:780–781.10.1056/NEJMp1109283