Abstract
Non-suicidal self-injury (NSSI) is a common behavior, particularly among adolescents and young adults. Impulsivity has been implicated as an important factor associated with NSSI, however prospective longitudinal research is lacking. Moreover, the relationship between impulsivity and other risk factors for NSSI is unclear. By examining longitudinal models including impulsivity, attachment, and distress we hope to elucidate the nature of the association between impulsivity and NSSI. 1,686 community-recruited young people (ages 14–25) with no NSSI in the past year were followed up for one year, completing self-report measures of the above factors. Impulsivity independently predicted new onset of NSSI over and above other risk factors, indicating heightened impulsivity is a prospective risk factor for NSSI. Psychological distress mediated the parenting-NSSI association.
Rates of self-harm peak during adolescence (Moran et al., Citation2012) with a prevalence of between 17% and 29% (Plener, Libal, Keller, Fegert, & Muehlenkamp, Citation2009; Swannell, Martin, Page, Hasking, & St John, Citation2014). Non-suicidal self-injury (NSSI) is any intentional self-harm in the absence of suicidal intent (Nock, Citation2010). As well as causing physical harm, NSSI is strongly associated with a number of other negative outcomes, including mental illness and suicide (Gittelman Klein & Gittelman, Citation1995; Wilkinson, Kelvin, Roberts, Dubicka, & Goodyer, Citation2011; Wilkinson, Qiu, Neufeld, Jones, & Goodyer, Citation2018). Therefore understanding the etiological pathways that lead to NSSI is of paramount importance (Laye-Gindhu & Schonert-Reichl, Citation2005).
Impulsivity has been a major focus of NSSI research and has been repeatedly associated with NSSI in cross-sectional studies (for a meta-analysis see Hamza, Willoughby, & Heffer, Citation2015). Impulsivity may increase the likelihood of people engaging in behaviors such as NSSI that have potentially serious and lasting consequences (Lynam, Miller, Miller, Bornovalova, & Lejuez, Citation2011). NSSI may be a largely impulsive action as it can usually be performed quickly and with little preparation (Nock, Citation2010) (Nock & Prinstein, Citation2005). As the bulk of research on impulsivity and NSSI has been cross-sectional, however, the direction of the association between impulsivity and NSSI is unclear (Hamza et al., Citation2015; Liu, Trout, Hernandez, Cheek, & Gerlus, Citation2017). Four small (n = 55–209) longitudinal studies of impulsivity and NSSI provided only weak evidence that greater impulsivity is predictive of NSSI (Black & Mildred, Citation2013; Chapman, Derbidge, Cooney, Hong, & Linehan, Citation2009; Glenn & Klonsky, Citation2011; Peterson & Fischer, Citation2012), and one larger longitudinal study (n = 4,799) found no evidence of an association (Mars et al., Citation2014). It is possible, therefore, that greater impulsivity is somehow a result of repeated engagement in NSSI. For example, young people who engage in NSSI may become accustomed to impulsive behavior by spending time with peers who also engage in NSSI and other impulsive activities (O’Connor, Rasmussen, & Hawton, Citation2009), or they may score themselves more highly on impulsivity questionnaires because they think NSSI must be an impulsive action (Janis & Nock, Citation2009). Repeated engagement in NSSI or chronic psychological distress associated with NSSI may have neurotoxic effects (Lupien, McEwen, Gunnar, & Heim, Citation2009), which may impair impulse control. Hamza and colleagues (Citation2015) conclude, therefore, that there is still a need for larger longitudinal studies to clarify role of impulsivity in the etiology of NSSI.
The apparent association between impulsivity and NSSI may also be confounded by the complex relationship between impulsivity and other risk factors such as psychological distress (Marshall-Berenz, Vujanovic, & MacPherson, Citation2011). While the association between impulsivity and NSSI remained in some studies that controlled for other risk factors for NSSI including gender, depression, anxiety, and childhood trauma (Arens, Gaher, & Simons, Citation2012; Black & Mildred, Citation2013; Glenn & Klonsky, Citation2010, Citation2011), in other such studies the association disappeared (Bornovalova, Tull, Gratz, Levy, & Lejuez, Citation2011; Carli et al., Citation2010; Evren, Cinar, Evren, & Celik, Citation2012; Rodav, Levy, & Hamdan, Citation2014; Sacks, Flood, Dennis, Hertzberg, & Beckham, Citation2008). As such, it is unclear if impulsivity is itself a significant predictor of NSSI, or if it is simply associated with other more meaningful antecedents of NSSI. Longitudinal models with multiple risk factors are needed to clarify the nature of the relationship between impulsivity and NSSI.
Adolescents who engage in NSSI experience both greater physiological arousal to, and lower tolerance of, distress (Nock & Mendes, Citation2008). For these young people, distress may interact with impulsivity to override adaptive behavioral controls, in keeping with a stress-diathesis model in which the confluence of distress and a predisposition for impulsive actions produces NSSI (Mann, Waternaux, Haas, & Malone, Citation1999). As NSSI provides relief from distress, and the relief is generally more immediate and salient than the consequences of NSSI (Nock & Prinstein, Citation2005), NSSI may be a particularly appealing coping strategy for impulsive people (Cyders & Smith, Citation2008).
Poor child-parent relationships, those typified by dysfunction, conflict, insecure attachment, or a lack of positive interaction, are also strongly associated with NSSI (Tatnell, Kelada, Hasking, & Martin, Citation2014). In cross-sectional work, psychological distress was found to mediate this association (Hallab & Covic, Citation2010). Early child-parent interactions play a key role in both emotion regulation and impulse control development as children learn to regulate their emotions and behaviors from their parents’ responses (Londerville & Main, Citation1981). It is possible, therefore, that both distress and impulsivity mediate the parenting-NSSI association, however this has yet to be tested with longitudinal data. Among adolescents, positive child-parent relationships are associated with lower self-reported impulsivity (Scott, Levy, & Pincus, Citation2009). Conversely, impulsive and distressed children are more difficult to parent (Johnston & Mash, Citation2001) and hence may receive less positive parenting. Again, longitudinal analyses are necessary in order to clarify the direction of the association between these factors.
HYPOTHESES
A review of the existing literature on risk factors and correlates of NSSI (Fliege, Lee, Grimm, & Klapp, Citation2009) concluded that future research should examine models that test mediations and effects of multiple risk and protective factors together, which we intend to do with the present study. Addressing a lack of longitudinal evidence, we set out to demonstrate a prospective association between impulsivity and NSSI, controlling for the previously demonstrated mediational pathway from parenting to NSSI via psychological distress (Hallab & Covic, Citation2010). Specifically, we hypothesized that impulsivity could increase the risk of new onset NSSI through:
Interacting with distress (moderation)
As consequence of a lack of positive parenting (mediation)
As an independent risk factor
METHODS
Participants
This study was conducted on data collected as part of the on-going U-Change (Understanding & Characterizing Healthy Adolescent-to-Adult Neurodevelopmental Growth Effects) arm of the Neuroscience in Psychiatry Network (NSPN) (NSPN.org.uk) programme (Kiddle et al., Citation2018; St Clair et al., Citation2017). NSPN is a venture from the University of Cambridge and University College London, which launched in November 2012, with the aim of researching how the adolescent mind and brain develop into early adulthood.
The sample in the present study comprised 2,432 participants (age in years: M = 19, SD = 3, range = 14–25; 54% girls). Participants were primarily sampled from age-sex-registers from general medical practices in two British regions (Cambridgeshire and Peterborough, and north London). Invitation letters were sent by GPs to eligible individuals on the study’s behalf. The aim was to have 200 participants in each of the ten gender-age bins (14/15, 16/17, 18/19, 20/21, 22/23/24), a target that was exceeded for all bins. Informed consent was obtained for all participants over age 16. Informed assent was obtained for all participants under 16 as well as informed consent from their parent/guardian. Participants who completed the first questionnaire package were sent another questionnaire package comprising the same instruments one year later; median interval for follow-up 1 was exactly 1 year (365 days) and the Inter-Quartile Range (IQR) was 85 days. Since our primary outcome variable is new onset of NSSI, the present sample was restricted to participants that reported having no NSSI at the first wave of data collection and who had complete data on all other key variables at baseline (n = 1,686).
Measures
Impulsivity
The Barratt Impulsivity Scale (BIS) (Patton, Stanford, & Barratt, Citation1995) is a widely used and well-validated (Stanford et al., Citation2009) 30-item self-report measure of three putative dimensions of impulsivity: (1) motor impulsivity (acting without or before thinking), (2) non-planning impulsivity (failing to consider consequences of actions, particularly in the long term), and (3) attentional impulsivity (making decisions quickly and acting upon them without sufficient consideration). A meta-analysis of four studies using the BIS as a measure of impulsivity in relation to NSSI found that NSSI was associated with greater impulsivity across all three BIS subscales and effect sizes across subscales were similar (Hamza et al., Citation2015).
General distress
Self-rating scales of psychological/psychiatric symptoms are often strongly correlated, making it difficult to draw conclusions from traditional regression models that include all dimensions of psychiatric wellbeing or illness as independent variables. Using NSPN data, we have shown that a bifactor model (in which the shared variance of multiple related factors is subsumed by a general factor with orthogonal specific factors) fittted symptom-level data better than alternative models (St Clair et al., Citation2017). The bifactor model included 118 items from measures of depression, anxiety, obsessions and compulsions, antisocial behavior; self-esteem; wellbeing; and schizotypy. The best fitting solution yielded a general distress factor, which accounted for 77% of the variance in the model, in addition to five specific non-correlated factors. In the present study, only the general distress factor will be examined.
Parenting
The Positive Parenting Questionnaire (PPQ) is a self-report questionnaire comprising 26 statements about a wide range of experiences of being positively parented, with higher scores indicating more positive parenting. The PPQ was developed for use with the NSPN study, and evidence for its psychometric validity has been previously demonstrated with this sample: Chronbach’s alpha = 0.96, intraclass correlation across time points = 0.76 (Cassels, Citation2018).
NSSI
The Drug, Alcohol and Self-Injury questionnaire (DASI) was developed by the authors as a self-report measure of cigarette, alcohol and drug use and NSSI. Our primary outcome variable in the present study was NSSI engagement over the past year. This was derived from combining data from two binary questions: “Have you tried to hurt yourself on purpose without trying to kill yourself?,” referring to the last month and the last 12 months (excluding the last month). These questions were applied at both waves of data collection. We have demonstrated reliability and validity of this question through finding similar population prevalence of NSSI in two separate community studies (Wilkinson et al., Citation2018), and high convergent validity (r = 0.66) with another well-validated multi-item measure of self-harm behavior, the Self-Harm Inventory (Sansone, Wiederman, & Sansone, Citation1998), in a third community sample of adolescents (Cassels, Citation2018). Using a single-item measure of NSSI is common in NSSI research and has previously been shown to render consistent estimates of prevalence (Muehlenkamp, Claes, Havertape, & Plener, Citation2012).
Analysis Procedure
We explored the role of impulsivity as a prospective risk factor for NSSI, alongside a previously demonstrated model in which parenting is associated with NSSI through psychological distress. We began by testing whether our proposed risk factors (impulsivity, distress, lack of positive parenting) were prospectively associated with new onset of NSSI on the univariate level with point-biserial correlations. We also explored the effects of age, gender, and age by gender interactions in predicting NSSI with separate logistic regressions. Gender and participants’ age were controlled for in all subsequent analyses where they were not the primary variables of interest.
The stress-diathesis hypothesis that the association between distress and NSSI is moderated by impulsivity was tested with an interaction term between distress and impulsivity at T1 predicting onset of NSSI by T2 in a logistic regression.
Cross-lagged analyses using structural equation modeling were used to clarify the directionality of the associations between positive parenting and impulsivity and distress. If impulsivity or distress were found to be influenced by positive parenting, they could be potential mediators of the parenting-NSSI association. The final mediation model was tested using the user-written binary logistic mediation package (Ender, Citation2011) for Stata. Robust confidence intervals for direct and indirect effects were estimated using 2000 bootstrap repetitions.
Analyses were conducted using STATA, version 14 (StataCorp, Citation2015). A threshold of 5% was used for statistical significance, as predictor variables were correlated and only one primary outcome variable was used.
RESULTS
Attrition
At baseline, 2,291 (94%) participants reported on NSSI, of which 1,829 (79.83%) reported no past-year NSSI. Of this latter group, 1,208 (66%) provided data on NSSI at the one-year follow-up (T2), and 67 (6%) reported having engaged in NSSI by T2. shows comparisons between the 1,208 participants that provided data at both time points and the 621 that did not. Participants who did not provide NSSI data at T2 were more likely to be older, to be boys, were more impulsive, reported less positive parenting, and more general distress, although effect sizes (Cohen’s d) were small.
TABLE 1. Descriptive and comparison statistics between participants with (n = 1,208) and without (n = 621) follow-up NSSI data.
As there are significant predictors of missingness at T2, data cannot be presumed to be missing completely at random, potentially biasing estimates (Sterne et al., Citation2009). Therefore, we performed multiple imputation of model variables using chained equations, producing 54 imputed datasets, a greater number than the percentage of missing outcome data (White, Royston, & Wood, Citation2011). The imputation model comprised all time points of all item-level data from the bifactor model, PPQ, BIS, NSSI, as well as background variables from (179 variables in total), which predicted T2 NSSI and missingness in T2 NSSI. All analyses were performed on imputed T2 data based on complete baseline cases of those with no reported engagement in NSSI over the past 12 months at T1 (n = 1,686).
Univariate Predictors of NSSI
shows that lower positive parenting, greater general distress, and higher impulsivity on all BIS subscales at T1 were significantly correlated (all p < 0.02) with new onset of NSSI by T2. As NSSI was associated with greater impulsivity across all three BIS subscales, in keeping with the meta-analysis by Hamza and colleagues (Citation2015), only the BIS total score will be examined in subsequent analysis. Socioeconomic status was not associated with new onset of NSSI by T2.
TABLE 2. Point-biserial correlations with new NSSI at T2.
Girls were significantly more likely than boys to report engaging in NSSI within the past year at T2 (OR = 1.33, p = 0.004, 95% CI: 1.093–1.612). There was no significant effect of age (b = 0.15, p = 0.363, 95% CI: −0.017–0.046). The age by gender interaction was significant (b = 0.10, p = 0.002, 95% CI: 0.038–0.167), with boys being more likely to report NSSI if they were older (b = 0.07, p = 0.003, 95% CI: 0.022–0.113), whereas NSSI among girls was not associated with age (b = −0.03, p = 0.132, 95% CI: −.080–0.010). Gender and age were specified as covariates in all further analyses.
Moderation Effects
The interaction term between impulsivity and distress in predicting onset of NSSI was non-significant (b = 0.01, p = 0.310, 95% CI: −0.006–0.018).
Directions of Relationships Between Risk Factors for NSSI
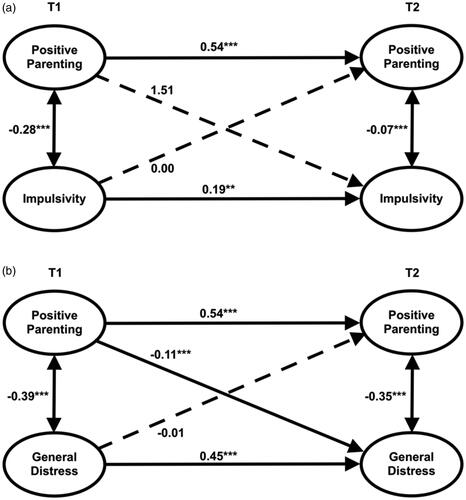
Cross-lagged analyses showed that neither positive parenting nor impulsivity at T1 significantly predicted the other at T2 (). Therefore, impulsivity cannot mediate the parenting-NSSI association. Conversely, positive parenting at T1 predicted lower general distress at T2 and not the reverse (). As such, distress may mediate the parenting-NSSI association.
FIGURE 1. Path diagram of the cross-lagged analyses of the effect of positive parenting and general impulsivity(1a)/distress(1b) at T1 on positive parenting and general distress at T2 controlling for their mutual effects. Indirect and direct effects of the model are reported in . **Significant at p < 0.01; ***Significant at p < 0.001. The models display standardized coefficients (95% confidence intervals shown in parentheses) of the effects of positive parenting and impulsivity(1a)/distress(1b) at T1 on positive parenting and impulsivity/distress at T2 controlling for their mutual effects. Pathways significant at p < 0.05 are shown with a solid line.
A Psychosocial Model for New Onset of NSSI
Main effects from the binary logistic multiple mediation analysis are shown in ; the indirect, direct and total effect are shown in . The main effects of T1 positive parenting, general distress, and impulsivity on new onset NSSI by T2 were all significant. Older age was an additional significant independent predictor of onset of NSSI (b = −0.005, p = 0.001, 95% CI: −0.008 to −0.002). Female sex was not associated with new NSSI (b = 0.02, p = 0.097, 95% CI: −0.034–0.003). The direct effect of positive parenting on NSSI was significant, as was the indirect effect of positive parenting on NSSI through lower general distress, shown in .
FIGURE 2. Path diagram of the mediation model of the effect of T1 positive parenting on new onset of NSSI over the next year, mediated by T1 general distress; independent effects of T1 impulsivity are included. *Significant at p < 0.05; **Significant at p < 0.01; ***Significant at p < 0.001. The model displays standardized coefficients (95% confidence intervals shown in parentheses) of the main effects of T1 positive parenting on T1 general distress, and of T1 general distress, impulsivity, and positive patenting on new onset of NSSI by T2. Age, gender, and impulsivity were controlled for at every level of analyses. Pathways significant at p < 0.05 are shown with a solid line with coefficients in bold.
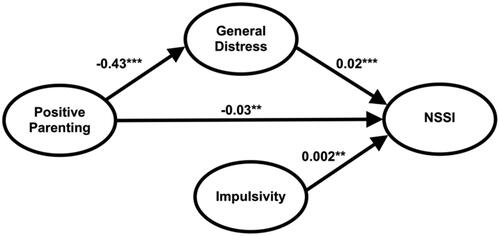
TABLE 3. Indirect and direct effects of the mediation model shown in .
The above analyses with imputed data closely resemble full case analyses except on a few minor points. In full case analyses (which by nature have a smaller sample and lower power), the direct effect of positive parenting on NSSI was not significant (b = −0.13, 95% CI = −0.28–0.01). There were some different results with sex and age; effects were always in the same direction (full raw data findings available from first author).
DISCUSSION
In this paper, we demonstrated that impulsivity was independently predictive of new cases of NSSI, even when accounting for positive parenting and general distress. As our sample was restricted to participants with no past year NSSI at baseline when impulsivity was measured, reverse causation is unlikely. While impulsivity has been previously associated with NSSI, of the four longitudinal studies of self-reported impulsivity reviewed by Hamza and colleagues (Citation2015), longitudinal links between impulsivity and NSSI were only found by Black and Mildred (Citation2013) and they did not control for NSSI or other confounds at Time 1. Thus, the present longitudinal findings provide some of the first and most robust support for a prospective association between impulsivity and new onset of NSSI. We also tested a stress-diathesis model in which impulsivity may moderate the general distress-NSSI association. The interaction was non-significant, indicating that while impulsivity and distress are both independently predictive of future NSSI, the effect is additive rather than multiplicative.
While there were small cross-sectional associations between positive parenting and lower impulsivity, neither factor at T1 was prospectively predictive of the other at T2. It is therefore impossible to draw conclusions about directionality of the association between these two variables. This lack of prospective association between positive parenting and impulsivity was unexpected in light of research demonstrating the key role played by positive early child-parent interactions in the development of impulse control (Londerville & Main, Citation1981; Scott et al., Citation2009). It is possible that impulsivity develops during a critical period in the context of early child-parent relationships and is largely stable and independent of positive parenting by adolescence. Alternatively, impulse deficits may develop from more severe proximal family dysfunction than was measured in our scale of parenting. The association between parenting quality and impulsivity across the developmental life course warrants further investigation.
Using longitudinal prospective data, we also replicated previous cross-sectional findings showing that the parenting-NSSI association is partially mediated by distress (Hallab & Covic, Citation2010). This finding suggests that positive parenting decreases rates of NSSI by reducing levels of contingent psychological distress, which in turn, reduces rates of new onset NSSI. We also found that while parenting was associated with distress one year later, the converse was not true, in keeping with a large body of literature demonstrating the broad impact of child-parent relationships on children’s emotional wellbeing (DeKlyen & Greenberg, Citation2008).
Clinical Implications
Positive parenting, psychological distress, and impulsivity are all potentially useful areas of therapeutic focus in regard to NSSI. We have provided evidence that impulsivity may also be a risk factor for future engagement in NSSI. Therefore, addressing impulsivity (for example through psychological training or pharmacological intervention) may be an effective means of lowering the risk of NSSI, if the association is found to be causal.
Working to encourage positive parenting may be an effective way of reducing NSSI both directly and through reduced psychological distress. In keeping with this idea, Attachment Based Family Therapy (ABFT) (Diamond, Reis, Diamond, Siqueland, & Isaacs, Citation2002), which focuses on improving communication and support in child-parent relationships, has already been shown to be effective at reducing both depression and suicidality among adolescents (Diamond et al., Citation2010), two factors closely related to NSSI. However, the present study’s lack of prospective associations between positive parenting and impulsivity may indicate that family focused therapeutic attempts at reducing NSSI will not be fully effective alone amongst young people for whom impulsivity is a key factor in their NSSI engagement.
Limitations
Although this study is one of only a few longitudinal studies on the association between NSSI and impulsivity, it still only comprised two waves of data collection, which limits the extent to which definitive conclusions around directionality and mediation can be drawn. We tried to ameliorate this through use of cross-lagged analyses to establish the direction of any associations between different proposed predictors of NSSI, however, an ideal study would comprise three waves of data collection or more. Moreover, as this study was observational as opposed to experimental, we cannot rule out the possibility of residual confounding or definitively establish causal associations between our variables. Experimental trials in which impulsivity, positive parenting, or distress are manipulated and the effect on NSSI behavior is observed will be necessary to definitely establish whether these factors hold a causal association with NSSI.
The study also suffered from significant attrition (33.95%) on the key outcome variable, NSSI. While attrition is an issue faced by most longitudinal research, and was addressed in part in the current study by the use of multiple imputation, data missing not at random may nevertheless lead to biased results.
The study also relied on self-report measures for most of the key variables, including NSSI, positive parenting, impulsivity, and distress. This presents issues around self-report bias. In particular, participants who were distressed as baseline may have rated their parenting as less positive. While these effects were reduced by data on impulsivity and parenting being collected in advance of incidence of self-harm, further studies would benefit from data being collected from an informant.
The NSSI questionnaire only asked about past year, not lifetime, NSSI. While unlikely, it is possible that distal NSSI may have influenced impulsivity or experiences of parenting. It is also possible that participants who had greater than a year between research assessments who self-harmed soon after the first assessment would have been misclassified as no-NSSI, reducing effect sizes.
Finally, recruiting participants through volunteers and GP networks may have resulted in a non-representative sample that was skewed toward those with physical or psychiatric conditions.
CONCLUSION
Despite the above limitations, this study demonstrated that impulsivity, psychological distress, and a lack of positive parenting predict higher rates of new onset cases of NSSI over the following year. This is the first study to our knowledge to demonstrate a robust prospective link between impulsivity and NSSI, indicating that improving impulse control may be an effective way of lessening NSSI among adolescents and young adults. Concordant with prior cross-sectional work (Hallab & Covic, Citation2010), our study has demonstrated longitudinally that much of the well-established association between parent-child relationships and NSSI could be accounted for by the association between positive parenting and lower psychological distress. Future studies are needed to further investigate the observed associations between parenting quality and impulsivity across the developmental lifespan, and the efficacy of therapeutic approaches using impulsivity and parenting as target for NSSI treatment and intervention.
AUTHOR NOTES
Matthew Cassels, Sharon Neufeld Anne-Laura van Harmelen Ian Goodyer, and Paul Wilkinson, Developmental Psychiatry, University of Cambridge, Cambridge, UK.
ACKNOWLEDGEMENTS
We would like to thank the NSPN sample for their participation.
DISCLOSURE STATEMENT
The funders had no role in the design and conduct of the study; collection, management, analysis, and interpretation of the data; and preparation, review, or approval of the manuscript. The authors have no conflicts of interest.
Additional information
Funding
REFERENCES
- Arens, A. M., Gaher, R. M., & Simons, J. S. (2012). Child maltreatment and deliberate self‐harm among college students: Testing mediation and moderation models for impulsivity. The American Journal of Orthopsychiatry, 82(3), 328–337. doi:10.1111/j.1939-0025.2012.01165.x
- Black, E. B., & Mildred, H. (2013). Predicting impulsive self-injurious behavior in a sample of adult women. The Journal of Nervous and Mental Disease, 201(1), 72–75. doi:10.1097/NMD.0b013e31827ab1da
- Bornovalova, M. A., Tull, M. T., Gratz, K. L., Levy, R., & Lejuez, C. W. (2011). Extending models of deliberate self-harm and suicide attempts to substance users: Exploring the roles of childhood abuse, posttraumatic stress, and difficulties controlling impulsive behavior when distressed. Psychological Trauma: Theory, Research, Practice, and Policy, 3(4), 349–359. doi:10.1037/a0021579
- Carli, V., Jovanović, N., Podlesek, A., Roy, A., Rihmer, Z., Maggi, S., … Sarchiapone, M. (2010). The role of impulsivity in self-mutilators, suicide ideators and suicide attempters — A study of 1265 male incarcerated individuals. Journal of Affective Disorders, 123(1-3), 116–122. doi:10.1016/j.jad.2010.02.119
- Cassels, M. T. (2018). Predictors and correlates of adolescent non-suicidal self-injury (PhD thesis). University of Cambridge, Cambridge.
- Chapman, A. L., Derbidge, C. M., Cooney, E., Hong, P. Y., & Linehan, M. M. (2009). Temperament as a prospective predictor of self-injury among patients with borderline personality disorder. Journal of Personality Disorders, 23(2), 122–140. doi:10.1521/pedi.2009.23.2.122
- Cyders, M. A., & Smith, G. T. (2008). Emotion-based dispositions to rash action: Positive and negative urgency. Psychological Bulletin, 134(6), 807–828. doi:10.1037/a0013341
- DeKlyen, M., & Greenberg, M. T. (2008). Attachment and psychopathology in childhood. In J. Cassidy & P. R. Shaver (Eds.), Handbook of attachment: Theory, research, and clinical applications (pp. 637–665). New York: Guilford Press. Retrieved from http://psycnet.apa.org/psycinfo/2008-13837-028.
- Diamond, G. S., Reis, B. F., Diamond, G. M., Siqueland, L., & Isaacs, L. (2002). Attachment-Based family therapy for depressed adolescents: A treatment development study. Journal of the American Academy of Child and Adolescent Psychiatry, 41(10), 1190–1196. doi:10.1097/00004583-200210000-00008
- Diamond, G. S., Wintersteen, M. B., Brown, G. K., Diamond, G. M., Gallop, R., Shelef, K., & Levy, S. (2010). Attachment-based family therapy for adolescents with suicidal ideation: A randomized controlled trial. Journal of the American Academy of Child and Adolescent Psychiatry, 49(2), 122–131. doi:10.1016/j.jaac.2009.11.002
- Ender, P. (2011). binary_mediation: Indirect effects with binary dv and/or mv. Retrieved March 30, 2017, from http://www.ats.ucla.edu/stat/stata/faq/binary_mediation.htm.
- Evren, C., Cinar, O., Evren, B., & Celik, S. (2012). Relationship of self-mutilative behaviours with severity of borderline personality, childhood trauma and impulsivity in male substance-dependent inpatients. Psychiatry Research, 200(1), 20–25. doi:10.1016/j.psychres.2012.03.017
- Fliege, H., Lee, J.-R., Grimm, A., & Klapp, B. F. (2009). Risk factors and correlates of deliberate self-harm behavior: A systematic review. Journal of Psychosomatic Research, 66(6), 477–493. doi:10.1016/j.jpsychores.2008.10.013
- Gittelman Klein, R., & Gittelman, R. (1995). Is panic disorder associated with childhood separation anxiety disorder? Clinical Neuropharmacology, 18, S7–S14. 10.1097/00002826-199518002-00003.
- Glenn, C. R., & Klonsky, E. D. (2010). A multimethod analysis of impulsivity in nonsuicidal self-injury. Personality Disorders: Theory, Research, and Treatment, 1(1), 67–75. doi:10.1037/a0017427
- Glenn, C. R., & Klonsky, E. D. (2011). Prospective prediction of nonsuicidal self-injury: A 1-year longitudinal study in young adults. Behavior Therapy, 42(4), 751–762. doi:10.1016/j.beth.2011.04.005
- Hallab, L., & Covic, T. (2010). Deliberate self-harm: The interplay between attachment and stress. Behaviour Change, 27(2), 93–103. doi:10.1375/bech.27.2.93
- Hamza, C. A., Willoughby, T., & Heffer, T. (2015). Impulsivity and nonsuicidal self-injury: A review and meta-analysis. Clinical Psychology Review, 38, 13–24. doi:10.1016/j.cpr.2015.02.010
- Janis, I. B., & Nock, M. K. (2009). Are self-injurers impulsive?: Results from two behavioral laboratory studies. Psychiatry Research, 169(3), 261–267. doi:10.1016/j.psychres.2008.06.041
- Johnston, C., & Mash, E. J. (2001). Families of children with attention-deficit/hyperactivity disorder: Review and recommendations for future research. Clinical Child and Family Psychology Review, 4(3), 183–207. doi:10.1023/A:1017592030434.
- Kiddle, B., Inkster, B., Prabhu, G., Moutoussis, M., Whitaker, K. J., Bullmore, E. T., … Jones, P. B. (2018). Cohort profile: The NSPN 2400 cohort: A developmental sample supporting the Wellcome Trust NeuroScience in Psychiatry Network. International Journal of Epidemiology, 47(1), 18–19g. doi:10.1093/ije/dyx117
- Laye-Gindhu, A., & Schonert-Reichl, K. A. (2005). Nonsuicidal self-harm among community adolescents: Understanding the “whats” and “whys” of self-harm. Journal of Youth and Adolescence, 34(5), 447–457. doi:10.1007/s10964-005-7262-z
- Liu, R. T., Trout, Z. M., Hernandez, E. M., Cheek, S. M., & Gerlus, N. (2017). A behavioral and cognitive neuroscience perspective on impulsivity, suicide, and non-suicidal self-injury: Meta-analysis and recommendations for future research. Neuroscience and Biobehavioral Reviews, 83, 440–450. 10.1016/j.neubiorev.2017.09.019.
- Londerville, S., & Main, M. (1981). Security of attachment, compliance, and maternal training methods in the second year of life. Developmental Psychology, 17(3), 289–299. doi:10.1037/0012-1649.17.3.289
- Lupien, S. J., McEwen, B. S., Gunnar, M. R., & Heim, C. (2009). Effects of stress throughout the lifespan on the brain, behaviour and cognition. Nature Reviews. Neuroscience, 10(6), 434–445. doi:10.1038/nrn2639
- Lynam, D. R., Miller, J. D., Miller, D. J., Bornovalova, M. A., & Lejuez, C. W. (2011). Testing the relations between impulsivity-related traits, suicidality, and nonsuicidal self-injury: A test of the incremental validity of the UPPS model. Personality Disorders, 2(2), 151–160. doi:10.1037/a0019978
- Mann, J. J., Waternaux, C., Haas, G. L., & Malone, K. M. (1999). Regular articles toward a clinical model of suicidal behavior in psychiatric patients. American Journal of Psychiatry, 156(156), 181–189. Retrieved from https://www.researchgate.net/profile/Kevin_Malone/publication/13299020_Toward_a_clinical_model_of_suicidal_behavior/links/0fcfd5118dcd9a23d5000000.pdf.
- Mars, B., Heron, J., Crane, C., Hawton, K., Kidger, J., Lewis, G., … Gunnell, D. (2014). Differences in risk factors for self-harm with and without suicidal intent: Findings from the ALSPAC cohort. Journal of Affective Disorders, 168, 407–414. doi:10.1016/j.jad.2014.07.009
- Marshall-Berenz, E. C., Vujanovic, A. A., & MacPherson, L. (2011). Impulsivity and alcohol use coping motives in a trauma-exposed sample: The mediating role of distress tolerance. Personality and Individual Differences, 50(5), 588–592. doi:10.1016/j.paid.2010.11.033
- Moran, P., Coffey, C., Romaniuk, H., Olsson, C., Borschmann, R., Carlin, J. B., & Patton, G. C. (2012). The natural history of self-harm from adolescence to young adulthood: A population-based cohort study. The Lancet, 379(9812), 236–243. doi:10.1016/S0140-6736(11)61141-0
- Muehlenkamp, J. J., Claes, L., Havertape, L., & Plener, P. L. (2012). International prevalence of adolescent non-suicidal self-injury and deliberate self-harm. Child and Adolescent Psychiatry and Mental Health, 6, 10. doi:10.1186/1753-2000-6-10
- Nock, M. K. (2010). Self-injury. Annual Review of Clinical Psychology, 6(1), 339–363. doi:10.1146/annurev.clinpsy.121208.131258
- Nock, M. K., & Mendes, W. B. (2008). Physiological arousal, distress tolerance, and social problem-solving deficits among adolescent self-injurers. Journal of Consulting and Clinical Psychology, 76(1), 28–38. doi:10.1037/0022-006X.76.1.28
- Nock, M. K., & Prinstein, M. J. (2005). Contextual features and behavioral functions of self-mutilation among adolescents. Journal of Abnormal Psychology, 114(1), 140–146. doi:10.1037/0021-843X.114.1.140
- O’Connor, R. C., Rasmussen, S., & Hawton, K. (2009). Predicting deliberate self-harm in adolescents: A Six month prospective study. Suicide and Life-Threatening Behavior, 39(4), 364–375. doi:10.1521/suli.2009.39.4.364
- Patton, J. H., Stanford, M. S., & Barratt, E. S. (1995). Factor structure of the Barratt impulsiveness scale. Journal of Clinical Psychology, 51(6), 768–774. doi:10.1002/1097-4679(199511)51:6<768::AID-JCLP2270510607>3.0.CO;2-1
- Peterson, C. M., & Fischer, S. (2012). A prospective study of the influence of the UPPS model of impulsivity on the co-occurrence of bulimic symptoms and non-suicidal self-injury. Eating Behaviors, 13(4), 335–341. doi:10.1016/j.eatbeh.2012.05.007
- Plener, P. L., Libal, G., Keller, F., Fegert, J. M., & Muehlenkamp, J. J. (2009). An international comparison of adolescent non-suicidal self-injury (NSSI) and suicide attempts: Germany and the USA. Psychological Medicine, 39(9), 1549–1558. doi:10.1017/S0033291708005114
- Rodav, O., Levy, S., & Hamdan, S. (2014). Clinical characteristics and functions of non-suicide self-injury in youth. European Psychiatry: Psychiatry, 29(8), 503–508. doi:10.1016/j.eurpsy.2014.02.008
- Sacks, M. B., Flood, A. M., Dennis, M. F., Hertzberg, M. A., & Beckham, J. C. (2008). Self-mutilative behaviors in male veterans with posttraumatic stress disorder. Journal of Psychiatric Research, 42(6), 487–494. doi:10.1016/j.jpsychires.2007.05.001
- Sansone, R. A., Wiederman, M. W., & Sansone, L. A. (1998). The Self-Harm Inventory (SHI): Development of a scale for identifying self-destructive behaviors and borderline personality disorder. Journal of Clinical Psychology, 54(7), 973–983. doi:10.1002/(SICI)1097-4679(199811)54:7<973::AID-JCLP11>3.0.CO;2-H
- Scott, L. N., Levy, K. N., & Pincus, A. L. (2009). Adult attachment, personality traits, and borderline personality disorder features in young adults. Journal of Personality Disorders, 23(3), 258–280. doi:10.1521/pedi.2009.23.3.258
- St Clair, M. C., Neufeld, S., Jones, P. B., Fonagy, P., Bullmore, E. T., Dolan, R. J., … Goodyer, I. M. (2017). Characterising the latent structure and organisation of self-reported thoughts, feelings and behaviours in adolescents and young adults. PLoS One, 12(4), e0175381. doi:10.1371/journal.pone.0175381
- Stanford, M. S., Mathias, C. W., Dougherty, D. M., Lake, S. L., Anderson, N. E., & Patton, J. H. (2009). Fifty years of the Barratt Impulsiveness Scale: An update and review. Personality and Individual Differences, 47(5), 385–395. doi:10.1016/j.paid.2009.04.008
- StataCorp. (2015). Stata statistical software: Release 14. College Station, TX: StataCorp LP.
- Sterne, J. A. C., White, I. R., Carlin, J. B., Spratt, M., Royston, P., Kenward, M. G., … Carpenter, J. R. (2009). Multiple imputation for missing data in epidemiological and clinical research: Potential and pitfalls. BMJ (Clinical Research Ed.), 338(1), b2393–b2393. doi:10.1136/bmj.b2393
- Swannell, S. V., Martin, G. E., Page, A., Hasking, P., & St John, N. J. (2014). Prevalence of nonsuicidal self-injury in nonclinical samples: Systematic review, meta-analysis and meta-regression. Suicide & Life-Threatening Behavior, 44(3), 273–303. doi:10.1111/sltb.12070
- Tatnell, R., Kelada, L., Hasking, P., & Martin, G. (2014). Longitudinal analysis of adolescent NSSI: The role of intrapersonal and interpersonal factors. Journal of Abnormal Child Psychology, 42(6), 885–896. doi:10.1007/s10802-013-9837-6
- White, I. R., Royston, P., & Wood, A. M. (2011). Multiple imputation using chained equations: Issues and guidance for practice. Statistics in Medicine, 30(4), 377–399. doi:10.1002/sim.4067
- Wilkinson, P. O., Kelvin, R., Roberts, C., Dubicka, B., & Goodyer, I. (2011). Clinical and psychosocial predictors of suicide attempts and nonsuicidal self-injury in the adolescent depression antidepressants and psychotherapy trial (ADAPT). The American Journal of Psychiatry, 168(5), 495–501. doi:10.1176/appi.ajp.2010.10050718
- Wilkinson, P. O., Qiu, T., Neufeld, S., Jones, P. B., & Goodyer, I. M. (2018). Sporadic and recurrent non-suicidal self-injury before age 14 and incident onset of psychiatric disorders by 17 years: Prospective cohort study. The British Journal of Psychiatry, 212(4), 222–226. doi:10.1192/bjp.2017.45.
