Abstract
Background: Antidepressant prescribing has dramatically increased in Scotland, and the cause is unknown. Objective: To investigate if the increase in antidepressant prescribing coincided with a reduction in prescribing of anxiolytics and hypnotics; to investigate this relationship at practice level; and to explore whether general practitioners (GPs) explain the increase by their increased use for anxiety. Methods: Study design: analysis of routine prescribing data and interviews with GPs. Setting: Scottish general practices. Participants: 942 practices included in the analysis. Sixty-three GPs in 30 practices completed interviews. Main outcome measures: Quantity of antidepressants, anxiolytics, and hypnotics prescribed. Relationship at practice level between anxiolytic/hypnotic and antidepressant prescribing. Spontaneous comments by GPs about prescribing antidepressants for anxiety. Results: Antidepressant prescribing increased from 28.9 million defined daily doses (DDDs) in 1992/3 to 128.3 million in 2004/5. Anxiolytic/hypnotic prescribing fell from 64.2 million to 55.1 million DDDs. There was a weak, positive correlation between levels of antidepressant and anxiolytic/hypnotic prescribing (+0.084, p=0.010). GPs treated anxiety with antidepressants, although many described an overlap between anxiety and depression. Some spontaneously identified a relationship with benzodiazepine prescribing when asked to explain the increase in antidepressant prescribing. Conclusion: A small part of the increase in antidepressant prescribing is due to substitution for benzodiazepines to treat anxiety.
Introduction
Prescriptions for antidepressant drugs have been rising steadily in Scotland since the beginning of the 1990s Citation[1], and this rise has been mirrored in many other European countries Citation[2–5]. In 1992, 1.16 million prescriptions for antidepressant drugs were dispensed in the community in Scotland. By 2006, this had risen more than three-fold to 3.53 million (Prescribing Information System, Information Services Division, Scotland [ISD Scotland]). The reasons for this increase are not clear. There has been no increase in the incidence or prevalence of depression in Scotland, general practitioners (GPs) do not appear to be making a diagnosis of depression more frequently, and there is no evidence that patients are presenting more frequently with depressive symptoms to their GPs Citation[6].
Hollinghurst and colleagues suggested several explanations for the rise in antidepressant prescribing, including the broadening range of indications for which antidepressants are prescribed Citation[7]. The British National Formulary (BNF) states that it may be appropriate to use an antidepressant for chronic anxiety (of longer than 4 weeks’ duration) and that generalized anxiety disorder unresponsive to buspirone or to a benzodiazepine should be treated with an antidepressant Citation[8]. It further states that antidepressants are generally used for panic disorders and phobias. Although sedative antidepressants are not recommended for the treatment of insomnia, there is evidence that these drugs are prescribed for this indication Citation[9]. The National Institute for Health and Clinical Excellence recommends that benzodiazepines should not be used beyond 2 to 4 weeks for generalized anxiety disorder and suggest that a selective serotonin re-uptake inhibitor (SSRI) may be offered for longer-term management Citation[10].
This study is part of a larger mixed-methods research project that investigated the causes of the increase in antidepressant prescribing in Scotland. We aimed to find out if the increase in antidepressant prescribing coincided with a reduction in benzodiazepine prescribing and prescribing for other anxiolytic and hypnotic drugs. We also investigated the relationship between antidepressant prescribing and anxiolytic/hypnotic prescribing at the level of the individual practice. Finally, we elicited the views of GPs about antidepressant prescribing for anxiety.
Methods
Quantitative
Prescribing data were taken from the Prescribing Information System maintained by ISD Scotland. The information relates to prescriptions dispensed in the community in Scotland. The vast majority of these prescriptions are written by GPs. Data were extracted for 12 financial years: 1992/3 to 2004/5. Prescriptions were classified based on the therapeutic groupings used in the BNF Citation[8]. For antidepressants, all drugs in BNF section 4.3 were included. This includes: 4.3.1 tricyclics and related antidepressant drugs; 4.3.2 monoamine oxidase inhibitors; 4.3.3 selective serotonin re-uptake inhibitors; and 4.3.4 other antidepressant drugs. For hypnotics, we included benzodiazepines and the “Z” drugs (zaleplon, zolpidem, and zopiclone), but excluded chloral and derivatives, chlormethiazole, antihistamines, and alcohol, which are also included in section 4.1.1. For anxiolytics, we included benzodiazepines and buspirone, which are contained in BNF section 4.1.2, but excluded beta-blockers and meprobamate, which are also included in this section.
The amount of prescribing was measured using defined daily doses (DDDs) Citation[11]. These are units representing the usual, daily, adult maintenance dose for the main indication of the drug. This enables comparisons across different formulations. For the analysis of national trends, these DDDs were divided by the population of Scotland to account for (small) changes in population over time.
Prescribing information was extracted by prescriber and linked to general practices. Prescriptions written by prescribers who are not permanent practice members (e.g., out-of-hours cover, locums, GP registrars) are not attributed to specific practices but are included in the national trends.
Standardized prescribing ratios (SPR) for antidepressants and anxiolytics/hypnotics were determined by calculating the expected rate of prescribing of these drugs in practices, given the age/sex distribution of the practice population, using STAR-PU values for these drugs Citation[12]. The SPRs are inaccurate if the prescribing data do not cover the whole year (if the practice opens or closes) or if there are large changes in population size during the year. In the practice-level analysis, we excluded practices with SPRs below the 1st or above the 99th percentiles.
The correlation between the crude DDD per-capita figures was compared to the correlation between the SPRs. This shows the influence of accounting for differences in population demography. Additional population, practice, and GP characteristics that influence the prescribing of anxiolytics, hypnotics, and antidepressants were determined by a backwards stepwise linear regression of the SPR. The differences left unexplained by the regression—the residuals—were then correlated. This demonstrates the degree of correlation once practice population size, age, sex, and other characteristics affecting prescribing are accounted for.
This analysis was carried out in STATA 8. The practice-level analyses were weighted by population size and restricted to the 942 practices that had complete data for all the variables. All practices were included in the analysis of national trends.
Qualitative
A purposive sample of 30 practices was selected from across Scotland to include practices that had high, medium, and low levels of prescribing and practices that had shown a high, medium, and low rate of increase in antidepressant prescribing. Practices were selected blind to their identity but, to ensure that the views of a wide range of Scottish GPs was included, there was a mix of practices with respect to gender and age of partners, number of partners, size of practice, training status, deprivation, and rurality. Most health board areas (n=15) in Scotland were represented in the study. Practices were initially contacted by letter and followed up by telephone 1 or 2 weeks later with a request that at least half of the doctors in the practice participate in the study. The semi-structured interviews were with a single GP, or group of GPs, face to face in their place of work, or by telephone. The interviewer was blind to the prescribing patterns of the practice. Interviews lasted around 60 min, and were taped and transcribed verbatim. Data analyses were inductive and continuous, and were systematically managed using the Nvivo data-handling package. Transcripts were read by S.M. and M.M., and views on emergent themes and categories were compared. Although GPs were not specifically asked about the relationship between antidepressant prescribing and anxiolytic/hypnotic prescribing, the topic guide included the following relevant questions:
Why do you think prescribing of antidepressants has increased?
What other conditions apart from depression do you treat with antidepressants?
Do you think there has been a change in the way that antidepressants have been prescribed?
How do you make the decision to prescribe an antidepressant?
How do you choose which drug to prescribe?
Results
Quantitative
Relationship between antidepressant and anxiolytic/hypnotic prescribing in Scotland
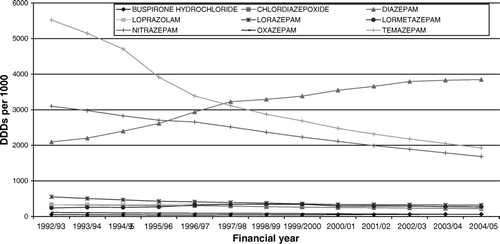
During the period of a steady increase in prescribing of antidepressant drugs in Scotland from 28.9 million DDDs in 1992/3 to 128.23 million DDDs in 2004/5, there has been a reduction in overall anxiolytic/hypnotic prescribing (). Overall DDDs of anxiolytics/hypnotics fell from 64.2 million in 1992/3 to 55.1 million in 2004/5.
Figure 1. Defined daily doses (DDDs) per 1000 population for benzodiazepines,'Z' drugs and buspirone, and antidepressants by financial years 1992/3 to 2004/5.
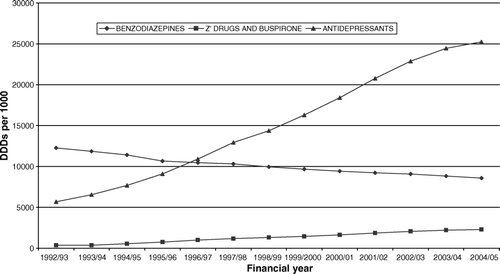
The rise in antidepressant prescribing during the period between 1992/3 and 2004/5 is largely attributable to a rise in prescriptions for SSRIs and other newer drugs ().
Figure 2. Defined daily doses (DDDs) of antidepressants by the British National Formulary Subsection in Scotland for 1992/3 to 2005/6.
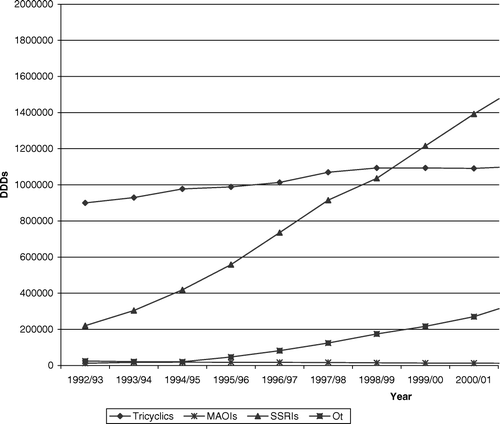
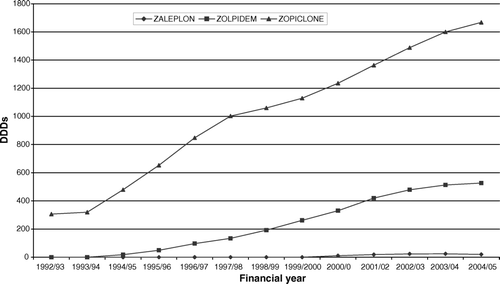
During the same period the most commonly prescribed anxiolytics/hypnotics were diazepam, temazepam, and nitrazepam. There has been a steady rise in diazepam prescribing (from 10.7 million DDDs in 1992/3 to 19.5 million in 2004/5), but a marked fall in prescriptions for temazepam (from 28.1 million DDDs in 1992/3 to 9.8 million in 2004/5) and a less steep but still substantial fall in prescriptions for nitrazepam (from 15.8 million DDDs in 1992/3 to 8.6 million DDDs in 2004/5) (). Prescriptions for buspirone have fluctuated around a low level during this period (0.27 million DDDs in 1992/3 and 0.32 million in 2004/5).There has been a steady increase in prescribing of the “Z” drugs during this period ().
Relationship between antidepressant and anxiolytic/hypnotic prescribing at practice level
A weak, positive correlation of +0.059 (p=0.073) was found between antidepressant and anxiolytic/hypnotic prescribing DDDs per head, i.e., practices that prescribe higher levels of antidepressants also tend to prescribe higher levels of anxiolytics/hypnotics. The correlation between the age/sex-standardized rates (SPRs) is stronger (+0.185, p<0.001). The characteristics that were found to influence the SPR of both groups of drugs were: the level of limiting long-term illness in the population; rural or urban location; GP age and sex composition; practice size (number of patients registered at the practice); and place of birth of GPs. When these characteristics were accounted for, the correlation became weaker but remained positive (+0.084, p=0.010).
Qualitative: Interviews with GPs
Sixty-three GPs were interviewed in 30 practices.
Some GPs spontaneously identified a relationship with benzodiazepine prescribing when asked to account for the increase in antidepressant prescribing.
So, I think that (SSRI use) might have been a reason for increase and, I think, also at the same time, we are seeing diazepam use drop substantially, and it may be that there was a knock on effect there. I'm not quite sure how that would happen because its obviously a treatment for different condition but that would be, I would wonder whether there was any kind of connection with any drop in diazepam or benzodiazepine use. (PR1 GPB)
I would say the indications for use has increased, not just for depression but other things as well, using it for some people with extreme anxiety or using things for obsessive compulsive sort of things as well. We use quite a lot of citalopram, I would say particularly for the very anxious people. (PR1 GPC)
Paroxetine, I used to give out a lot for, particularly for anxiety, again because there was some evidence for that. (PR6 GPE)
The sort of people we see are just unhappy, dissatisfied with life, anxiety symptoms are far more common than depression but mostly it's a mixed picture, sometimes both. And we know perfectly well that antidepressants are good for anxiety as well so probably more people being treated for anxiety than for actual depression, it's a huge overlap. (PR9 GPA)
Discussion
Strengths and limitations of this study
Prescribing data are robust because all prescriptions written by GPs, and dispensed by pharmacists, are collected centrally in Scotland so that the costs to pharmacists can be reimbursed. The availability of such data allows for accurate identification of longitudinal trends in prescribing of antidepressants and anxiolytics/hypnotics. The mixed-methods approach used in the study enabled us to extend our exploration of prescribing data with prescribers’ views on their own changing practice. However, prescriptions are not linked to diagnostic data in Scotland, and so we cannot confirm the proportion of antidepressants prescribed for anxiety or anxiety-related problems in this study.
Summary of main findings
The steady increase in antidepressant prescribing in the period since 1992 has coincided with a smaller decrease in anxiolytic/hypnotic prescribing. There is a tendency for practices with the highest levels of prescribing of antidepressants to have the highest levels of prescribing of anxiolytics/hypnotics. In part, this reflects the characteristics of the practice population. For example, there are higher levels of prescribing of both antidepressants and anxiolytics/hypnotics in areas of higher socioeconomic deprivation and population morbidity. The remainder of the variation is likely to be related to the propensity of individual GPs to prescribe psychotropic medication and to practice-specific patterns of patient demand. Local patterns of drug dependence may also be important. Combined benzodiazepine and opioid drug dependence is common in urban areas of Scotland, and it is possible that some of the variation in prescribing levels between practices may be attributable to maintenance prescribing of benzodiazepines Citation[13–15].
In the interviews, GPs described their use of antidepressants, particularly SSRIs, to treat anxiety, but most of those who raised this issue described treating mixed anxiety and depression rather than distinct diagnoses of either. GPs prescribing antidepressants for patients with these mixed mood disorders find themselves in something of a dilemma. Psychotropic drugs receive regulatory approval on the basis of effectiveness in discrete diagnoses Citation[16], and yet mixed mood disorders are the commonest presentation of affective disorder Citation[17]. The prescription of antidepressant drugs in such circumstances may thus reflect a pragmatic solution to the problems posed both by the artificial nature of current psychiatric nosology and by drug-licensing processes Citation[16].
Comparison with existing literature
In a smaller study of 139 East London general practices, Hull et al. found a modest fall in anxiolytic and hypnotic prescribing during a period of almost doubling of antidepressant prescribing Citation[18]. They found no evidence of an association between antidepressant prescribing and anxiolytic prescribing suggesting that GPs who prescribe low rates of antidepressants do not use anxiolytics as an alternative. They did not address the issue of GPs prescribing more antidepressants as a substitute for anxiolytics for chronic anxiety. Our findings support Hollinghurst et al.'s suggestion that part of the increase in antidepressant prescribing may be due to a broadening of the indications for SSRIs to include anxiety Citation[7]. This can, however, only account for a small part of the rise in antidepressant prescribing.
Implications for future research or clinical practice
Future research should continue to investigate a range of potential causes for the increase in antidepressant prescribing. The most likely reasons that will explain the increase in antidepressant prescribing, in our view, are the artificial inflation of levels of prescribing due to the use of DDDs to measure the volume of prescribing because SSRIs are much more difficult to prescribe at lower doses than the defined daily dose, and prescribing for longer periods of time in response to guideline recommendations Citation[10].
Interventions aimed at influencing the antidepressant prescribing patterns of GPs need to understand and acknowledge the complex interaction of patient, practice, and prescriber characteristics.
Conclusion
A small part of the increase in antidepressant prescribing in Scotland appears to be linked to the reduction in the use of benzodiazepines for the treatment of chronic anxiety and mixed anxiety and depression conditions as recommended in guidelines.
Acknowledgements
We would like to thank the GPs who participated in the interviews.
Details of funding
This study is part of a larger project funded by the Chief Scientist Office of the Scottish Executive Health Department (reference number CZH/4/198). The work is independent of the funder and does not necessarily reflect its views.
Declaration of interest: The authors report no conflicts of interest. The authors alone are responsible for the content and writing of the paper.
References
- Philp AV, Watson L, Muir R Mental health in Scotland: information sources and selected insights. Edinburgh: NHS Scotland Information and Statistics Division; 2002. Available at URL: http://www.isdscotland.org/isd/files/sources_insights2002pdf.pdf ( accessed 8 May 2006).
- Reseland S, Bray I, Gunnell D. Relationship between antidepressant sales and secular trends in suicide rates in the Nordic countries. Br J Psychiatry 2006; 188: 354–8
- Helgasson T, Tomasson H, Zoega T. Antidepressants and public health in Iceland: time series analysis of national data. Br J Psychiatry 2004; 184: 157–62
- Guaiana G, Andretta M, Corbari L, Mirandola M, Sorio A, D'Avanzo B, et al. Antidepressant drug consumption and public health indicators in Italy, 1955 to 2000. J Clin Psychiatry 2005; 66: 750–5
- Van Marwijk H, Bijl D, Herman J, de Haan M. Antidepressant prescription for depression in general practice in the Netherlands. Pharm World Sci 2001; 23: 46–9
- Munoz-Arroyo R, Sutton M, Morrison J. Exploring potential explanations for the increase in antidepressant prescribing in Scotland using secondary analysis of routine data. Br J Gen Pract 2006; 56: 423–8
- Hollinghurst S, Kessler D, Peters TJ, Gunnell D. Opportunity cost of antidepressant prescribing in England: analysis of routine data. Br Med J 2005; 330: 339–61
- British National Formulary. British Medical Association and Royal Pharmaceutical Society of Great Britain. Volume 52 (September 2006). Available at URL: www.bnf.org/bnf/ ( accessed 24 February 2007).
- James SP, Mendelson WB. The use of trazodone as a hypnotic: a critical review. J Clin Psychiatry 2004; 65: 752–5
- URL: http://guidance.nice.org.uk/CG22/guidance/pdf/English ( accessed 18 March 2007).
- National Prescribing Centre. Available at URL: http://www.npc.co.uk/publications/prescribing Terms/frames.htm ( accessed 12 May 2006).
- Prescribing support unit website: http://www.ic.nhs.uk/psu/measure/presmeas/copy_of_starpus/ ( accessed 12 May 2006).
- Gruer L, Wilson P, Scott R, Elliott L, Macleod J, Harden K, et al. General practitioner centred scheme for treatment of opiate dependent drug injectors in Glasgow. Br Med J 1997; 314: 1730–5
- HMSO. Drug misuse and dependence – guidelines on clinical management. London: HMSO; 1999.
- Hutchinson SJ, Taylor A, Gruer L, Barr C, Mills C, Elliott L, et al. One-year follow-up of opiate injectors treated with oral methadone in a GP-centred programme. Addiction 2000; 95: 1055–106
- Shorter E, Tyrer P. Separation of anxiety and depressive disorders: blind alley in psychopharmacology and classification of disease. Br Med J 2003; 327: 158–60
- Jenkins R, Lewis G, Bebbington P, Brugha T, Farrell M, Gill B. The national psychiatric morbidity surveys of Great Britain—initial findings from the household survey. Psychol Med 1997; 27: 775–89
- Hull SA, Aquino P, Cotter S. Explaining variation in antidepressant prescribing rates in East London: a cross sectional study. Fam Pract 2005; 22: 37–42