ABSTRACT
Background
Policy promotes students and doctors becoming GPs, yet there exists little focus on GP trainers’ recruitment and retention.
Aim
To explore barriers and enablers facilitating the professional identity formation of a GP becoming a GP trainer.
Design and Setting
A qualitative case study within one training programme of the Scottish Deanery.
Method
Data were collected between January and November 2018 via semi-structured interviews with 16 GP trainers and 79 regulatory and policy documents. Thematic analysis was applied whilst a reflexive stance as a previous GP trainer was maintained.
Results
Findings indicate GPs become GP trainers through experiences and events across three predominant identities: ‘Becoming a Doctor’, ‘Becoming a GP’ and ‘Becoming a GP Trainer’. Impediment at any of these stages acts as a barrier. The GP trainer role suggests tendencies for clinicians to be understated in their achievements and abilities. GP trainers dually enact and role model that of clinician and teacher; time acts as a significant barrier. The Scottish Prospective Educational Supervisor Course (SPESC), or previous iterations, is a significant enabler. Royal College of GP’s contributions towards GP trainers is absent. GP trainer associations with out-of-hours services have changed over time. GP trainer/trainee relationships are essential enablers to a continued GP trainer professional identity.
Conclusion
The role of the GP trainer as a teacher needs highlighting. Processes that protect and maximise this role may enhance the positive contributions of being a teacher. Understanding these themes may enhance recruitment and retention of GP trainers.
Introduction
Within medicine, and medical education specifically, the concept of professional identity (PI) and its formation is an area that has gained attention in recent years [Citation1]. Currently, there exist several key influencing factors in the United Kingdom (UK) which are set to drive forward the engagement of the availability of general practitioners (GPs) and, more specifically, GP trainers for the future. The Royal College of GPs (RCGP) had set out a blueprint ‘ … to reverse the impacts of the increasing problems of workload and recruitment on the ability of GPs to deliver excellent patient care … ’ [Citation2, p.2]. One element of their argument was to expand the number of GPs, balanced by their concerns that 20% of the current workforce may retire in the next five years. It therefore makes sense, to establish what may be needed to encourage new, as well as retain existing GP trainers, in order to promote the continuation of the GP profession.
More recently, locally, RCGP Scotland had also provided a reinforcing message of the need to enhance the workforce target by 2024/25 that was based on whole-time equivalent figures and not just a headcount, thus effectively again seeking to call for a growth in GP numbers [Citation3]. A snapshot taken from the medical profession’s governing body, the General Medical Council (GMC), indicates that of the 289,115 registered doctors in the UK only 25% of these (72,318) are GPs, with GP trainers a smaller subset, 8035 (i.e. approximately 11% of the GP population) [Citation4]. Thus, it is imperative to ensure a match between creating new GPs whilst having sufficient trainers to implement such processes.
Whilst previous research has sought to examine the traits of GP trainers or their motivations in the past [Citation5,Citation6] there exists little evidence of current trainers’ perceptions of their workload and none via the lens of professional identity formation. Thus, the main aim of this study was to address the research question regarding ‘What are GPs’ barriers and enablers to becoming a GP trainer?’ In doing so, I have adopted a theoretical lens that applies the process of Symbolic Interactionism (SI) [Citation7]. SI can be described as, ‘ … how people act toward things based on the meaning those things have for them, and these meanings are derived from social interaction and modified through interpretation … ’ [Citation8, para 1]. In other words, in exploring the professional identity of the GP trainer or the becoming of a trainer, I was keen to move beyond the psychological world of traits and states into a socially interactive world [Citation9]. A world in which the GP already has a strong foothold when currently considered regarding doctor-patient collaborations [Citation10] and the social contracts we hold as key [Citation11]. Thus, by applying a reflexive thematic analysis with respect to informing policy and practices that influence GP trainer training, combined with semi-structured interviews of GP trainers, recommendations regarding the recruitment and retention of GP trainers can be outlined.
Method
Design
Qualitative methodology positioned this research as a type-2 case study [Citation12], with the evidence aligning with qualitative reporting guidelines [Citation13]. The premise of a type-2 case study is that the case under examination, once contextualised, is considered through multiple units of analysis. In this case, the context was that of the Scottish Deanery, drawing on geographical boundaries of one educational GP training programme as the case.
To place this in perspective, NHS Scotland, and by default the deanery, consists of 14 territorial health boards, and 7 special health boards (1 of which is NHS Education for Scotland (NES)) together with 5 Scottish medical schools [Citation14]. Geographically, the programme area spanned a region approximately 35 miles in radius from its central point, including both urban and rural GP populations as well as coastal and inland locations.
Data collection
There were two embedded units of analysis, namely: participant (GP trainer) interviews, and documentary sources, which were linked to GP trainer’s experiences past, present and future. Regarding participants as a unit of analysis, GPs belonging to any of the four categories in and having practised medicine within the programme area of the Scottish Deanery selected were eligible for inclusion. Thus, mixed, purposeful recruitment was performed [Citation15] bearing in mind these latter criteria. Participants were invited via an email and publicity leaflet that was sent on my behalf, by the local programme administrative team who agreed to act as an intermediary. Sixteen GPs indicated an interest; all respondents were followed up to arrange a one-to-one, semi-structured interview with me that was audio recorded. Their characteristics are summarised in . The interview guide () was initially piloted by two members of a GP academic department with no changes required. The interview schedule sought to align with characteristics of a doctor’s career pathway before moving towards questions of a GP trainer’s identity that aligned with SI theory.
Table 1. Summary of participants pre-interview data.
Table 2. Interview schedule.
In considering SI theory, Serpe and Stryker remind us that the concept of SI emerged latterly via Blumer, who was actually describing the ideas of Mead [Citation7]. SI can be said to build on the premise that the state of human nature is a social one. That society is created via social relationships, communication and interaction based on sociability, with society being a mirror in which people see themselves. The essence of structural SI allows for the examination of the role of social structure in life, understanding that actors and social structure relate to one another with self as a conduit through which we express ourselves [Citation7]. Importantly, SI identity theory can be summarised succinctly, in that ‘society’ impacts ‘self’ while in turn ‘self’ impacts ‘society’; a theory fitting through which to examine the social position of the GP trainer.
In respect of documentary evidence as a second unit of analysis, I have drawn from local and national informing policies, GP trainer website materials and other supporting records linked with GP training. These data sources were obtained from a series of websites and organisations and comprised policy documents (locally and nationally), legislation, updates and reports from the local deanery. Also collected were website snapshots and a set of miscellaneous other sources consisting of associated RCGP manifesto materials, RCGP communications and primary care workforce surveys and newsletters. Seventy-nine sources were collated and are summarised in .
Table 3. Summary of documentary sources.
Analysis
Interview audio data were transcribed verbatim and collated with policy and documentary materials using the electronic tool NVivo [Citation16]. Data were scrutinised using a reflexive thematic analysis [Citation17,Citation18]. Themes and sub-themes were developed on the basis of a reflexive, inductive, analytic viewpoint. In aligning with the current direction of approaches to such an analysis, the codes and themes were driven from an interpretative position regarding the concept of information power [Citation19], rather than a position of data saturation [Citation20].
A reflexive journal was maintained to aid in the charting of the developments of conceptualisations and links, thus aiming to imply that the reasoning was grounded in data and informed by sensitising concepts. Additionally, as the researcher, I sought to enhance my own position by undergoing the same semi-structured interview that was utilised with the participants in order to be appreciative of the nature of the questioning being undertaken and to enhance personal reflections of their PI as a previous GP trainer [Citation18]. A degree of data analysis triangulation was also supplemented by participants who consented to member checking (n = 8), using synthesised, analysed data [Citation21], all whom agreed with the themes and sub-themes that had been developed.
Results
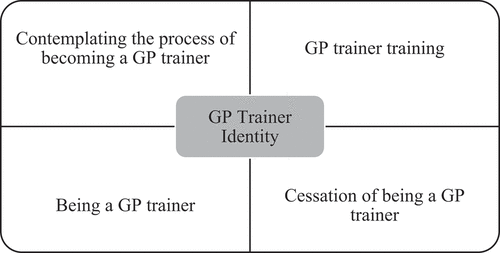
Results indicate GPs can arrive at the GP trainer role through experiences and events transitioning across three predominant identities: ‘Becoming a Doctor, ‘Becoming a GP’ and ‘Becoming a GP Trainer’. Impediment at any of these stages can act as a barrier in becoming a GP trainer. For the purposes of this article, this writing highlights the core, inner theme and six inter-linked sub-themes of ‘Becoming a GP Trainer’ which are summarised in .
Table 4. Summary of the thematic analysis.
External influences
Within this context of external influences, five dimensions affecting the PI of the GP trainer were specifically reiterated: the Scottish Prospective Educational Supervisor Course (SPESC), the deanery, out-of-hours (OOH) GP arrangements, political influences and the GP trainer’s group.
Fifteen of the participants spoke about the positive influences that SPESC or previous iterations of this had on the beginnings of their journey to fulfil a personal wish to become a GP trainer,
(P6) ‘ … if you’re in a supportive environment, if you’re enthusiastic and driven, that’s fine. You can do it. I think the SPESC course, from what I’ve seen of it, is pretty comprehensive … it teaches a lot of good stuff, in terms of practicalities but also the theories as well … ’
However, opinions were often divisive of the influence of the deanery, more so historically than in more recent times,
(P1) ‘… I mean, I had, I did have an unsettling experience as well, which actually, made me think twice about it, in which, there was an incident with a remedial trainee. And, um, where I didn’t feel supported … I felt let down by my partners at the time … also I have to say by the deanery as well …’
Several GPs were reflective of the fact that within their identity as a trainer, delivery of OOH service was an important element to take into consideration, perhaps more so from the older GP trainer who had been through different iterations of this service,
(P9) ‘… Well things about out-of-hours are important. It’s the same thing and I think one of the things that we realised later (handing OOH back in 2004 GP contract changes) was that we’d lost something enormous … ’
Whilst multiple documentary (n > 20) sources pointed towards the influences of policy and practice that underpinned the transformations of the PI of the clinicians, only three of the trainers alluded to political influences directly. RCGP’s influence was not mentioned. However, many (n = 10) of the trainers spoke of the usefulness of the GP trainer’s group in contributing towards their identity,
(P11) ‘… the other thing talking about trainers’ courses was there’s a very active [place name] trainer’s workshop and all the trainers in [place name] met regularly … ’
The GP practice
All of the participants (n = 16) spoke of their relationship with their GP practice. They primarily spoke about this positively, highlighting the role of the GP trainer and what this meant for the practice.
(P5) ‘… But I’d seen how enriching it was. I’d seen how it was helpful for the business model, I’d seen how it was helpful for the, you know, recruitment, I saw it was enriching for capacity and how it was enriching financially. There were lots of benefits to the practice, massively enriching for the whole education and the ethos and the practice culture. So, it was influential, yes, and I can’t envisage a practice without trainees you know …’
However, some participants (n = 9) did comment that were mindful about how well their work might not have been recognised within the practice environment.
(P6) ‘… I think there’s a perception out there that, and there’s a bit of reality actually, you know yourself, it is all hard work to get there …and there’s some, sort of, sacrifice in terms of time and effort and … but, also, in terms of the workplace-based assessment and the amount of that that we have to do … and some practices don’t have the ethos of education. They say they think they might, but they don’t …’
Characteristics of the GP trainer (self)
This sub-theme focuses on that which is the ‘self’ of the GP trainer. All of the participants articulated the concept of the GP trainer via characteristics or attributes that one might possess or expect to possess. A large number of the cohort (n = 11) were understated in their progression towards their medical career or their GP trainer persona, often speaking about the added value or enrichment that the identity brought to their lives.
(P14) ‘… I learn a lot from it, to be honest. It’s a really good way of keeping up to date. But also, there’s something really satisfying about trainees coming in, being not sure about what they’re doing, and actually seeing them blossom, and become competent, and seeing that progression …’
These commentaries of self-worth worth appeared to be reaffirmed irrespective of the gender of the participant as P7 echoed:
(P7) ‘…Always been a kind of a middle-of-the-road student and not … You know, I wasn’t in top classes or anything. I was just kind of a borderline, okay student. And not that anybody ever told me that I couldn’t do it, but, you know, a career’s guidance at one stage said that maybe I should look at geography and become a weather girl …’
Time
Unsurprisingly given the current climate of the NHS and GP workload, time was cited as a significant barrier in performing the role of the GP trainer by all of the participants (n = 16).
(P1) ‘… think recognising that it is hard work, and how you do that, I don’t know … and then valuing that hard work … somehow almost, I guess, if you could have a condition of becoming a trainer or a training practice, is that you should ensure that there is dedicated time for the trainer …’
In some cases, time proved to be the main and significant barrier to meaning that a GP trainer ultimately had to give up their PI as a trainer:
(P8) ‘… Yeah, the workload … I was already struggling to deal with the tutorial side of it. [GP partner name] used to do one tutorial a month. [A different GP partner name] did none … plus, obviously, extra supervision and things … And I possibly could have dropped a bit and had a bit more protected time, which I didn’t have. But I didn’t want to do that … Because I thought, well, my patients needed me to consult and I was torn two ways …’
The relationship with the GP trainee
All of the participants spoke about the importance in the relationship, often akin to apprenticeship, that was established between themselves and their GP trainee. Some comparisons were also made between the ‘good’ trainee and the ‘doctor in difficulty’ with many of the trainers (n = 12) noting that the latter cohort had the potential to be a significant barrier in its own right.
(P3) ‘… it’s really no different to an apprenticeship really is it, you know. I mean, I see that you’re going to learn from somebody who’s been working in that role for … for a while.’
Knowing when to be nurturing or supportively challenging was key.
(P6) ‘… I don’t see it as a hindrance at all. I love the feeling of nurturing someone through from virtually … Not nothing, they’re not, they don’t come with nothing. But, you know, rabbit in the headlights of being in GP training to confidence at the end of it …’
The role of the GP trainer
Lastly, interlinked with the apprenticeship model but specific to the GP trainer identity was the concept of the trainer undertaking a specific role (often that of the GP as a clinician) and modelling it for their trainees (n = 11).
(P3) ‘…I’d like to think that there’s more of an emphasis on actually just trying to demonstrate doing your job to someone else so they can learn. You know, rather than being two separate entities, you know, being a trainer and being a GP I would like to think that they’re not that dissimilar …’
However, an important element of this was their very specific role in terms of being a teacher, which they all (n = 16) highlighted.
(P4) ‘… I always felt that, and I always said this to everybody I come across, trainees and students, that being a doctor meant, meant being a teacher you know, because that’s what’s the whole idea …’
Discussion
Summary
Participants, combined with policy and practice, in this study, suggest that barriers and enablers towards becoming a GP training are construed of three predominant themes: ‘Becoming a Doctor’, ‘Becoming a GP’ and ‘Becoming a GP trainer’. All three contribute towards an embedded structure of PI formation, that can exist, from person to person, within the interactions that symbolise the GP trainer [Citation7]. The latter theme, in particular, holds several overlapping components that influence the GP trainer and are key given current national directives [Citation2,Citation3,Citation22].
Drawn from a symbolic interactionism [Citation7] perspective, the facilitating power that selected components direct towards the GP trainer’s professional identity (PI) are derived from the meaning and interpretations that can be attributed to them. Each of these ascribed components act in unison to influence the PI of the GP trainer, thus there exists the risk that one or more might act as a ‘tipping point’ to influence the GP trainer in continuing or relinquishing their role. This is certainly more powerful with the current tensions of the NHS [Citation23].
Strengths and limitations
A strength of this study is in the contemporaneous explorations of GP trainer’s thoughts and feelings, supplemented by policy and practice analysis. GPs have been drawn from across the spectrum of those contemplating being a GP, to those who have adopted that role, and even forgone it. Trustworthiness of this data and its transferability to other GP training settings has been considered from the outset, as well as the position of the researcher [Citation18,Citation24,Citation25]. Considerations were given to the geographical locations of these participants but the current landscape and urban/rural divides within this case study are best bounded by the programme deanery as ascribed previously, the geography being too diverse and complex [Citation3]. Likewise critical concepts aligned with elements of intersectionality [Citation26] were considered in analysis, with no overt patterns emerging.
Limitations of this study have arose from analysis been attributed to one single researcher, albeit reinforced via participant checking [Citation21]. Additionally, whilst participants have been selected from a wide-ranging area of one programme in the Scottish Deanery, nuances that are reflected within other contexts of the UK GP trainer population may have been overlooked. Data collection was completed before the emergence of Covid-19.
Comparison with existing literature
The importance of these findings’ centres on the latter theme of ‘Becoming a GP trainer’ as their relevance is unique and key at this time of writing. The former themes of ‘Becoming a Doctor’, and ‘Becoming a GP’, whilst vital to ensure the sequential development of the GP trainer, have been highlighted in the past. Previous policy [Citation27], longitudinal processes [Citation28] and newly emerging directions [Citation29] regarding undergraduate processes have come a significant way in contributing towards identity transformations of students and foundation doctors towards GP training.
Whilst evidence has previously acknowledged the importance of the GP trainee relationship [Citation30] and the connections between the GP trainer and their GP practice [Citation6], unreported to date is the tendency of the GP trainer to be understated in the nature of their achievements and abilities. This likely professional ‘invisibility’ can hide the challenges for the GP educator who juggles the roles of the clinician and the teacher [Citation31]. Thus, when it comes to bearing in mind how to highlight and celebrate the successes that evolve from becoming a GP trainer, organisations and individuals need to be mindful to encourage and reward such successes. My research aligns with current evidence regarding the challenges for the GP educator who juggles the role of the clinician and the teacher [Citation31]. Whilst the MRCGP exam is no longer a barrier to becoming a GP trainer per se, the role of RCGP thereafter remains absent of contribution.
Implications for research and practice
In terms of future research, it would be viable that a number of routes could be explored that might further promote the PI of the GP trainer and their associated connections. A focus specifically on the value and utility of the SPESC course given the changes that have evolved within GP trainer training and practice status in the last decade may be useful, as well as implementation of a standardised GP trainer training model, previously recommended, yet still to exist [Citation32]. Attention to the lived experiences of GP trainers’ training groups and current OOH arrangements would also be vital.
Regarding policy and practice the role of the GP trainer as a teacher and medical educator needs to be highlighted, beginning from early undergraduate days, and building on the descriptions and routes towards this professional identity, into postgraduate life. Deaneries need to consider emphasising and enhancing the status of the GP trainer, especially given the latter’s potential to be understated in nature. The RCGP should reconsider their position with respect to GP trainers and how they might better support them in the role; they currently appear as unrecognised as contributing towards the GP trainer professional identity. Time remains a significant barrier for the GP trainer, processes that protect and minimise this are likely to enhance the positive contributions of being a teacher and thus maintaining that role. In particular, a realistic workload.
Ethical approval
The Open University – Human Research Ethics Committee (HREC) ref: HREC/2721/McConville.
Acknowledgments
Thanks are provided to the participants who contributed their time.
Disclosure statement
This work forms part of an EdD via The Open University and was partially funded by RCGP Scientific Foundation Board under grant number SFB 2019-01.
Additional information
Funding
References
- Cruess RL, Cruess SR, Boudreau JD, et al. Reframing medical education to support professional identity formation. Acad Med. 2014 Nov;89(11):1446–1451.
- Royal College of General Practitioners. A vision for general practice in the future NHS [Internet]. Royal College of General Practitioners; 2015 [cited 2019 Jul 22]. Available from: http://www.rcgp.org.uk/campaign-home/~/media/files/policy/a-z-policy/the-2022-gp-a-vision-for-general-practice-in-the-future-nhs.ashx
- Royal College of General Practitioners (Scotland). From the frontline - the changing landscape of Scottish general practice. [Internet]. 2019 [cited 2021 Dec 21]. Available from: https://www.rcgp.org.uk/-/media/Files/RCGP-faculties-and-devolved-nations/Scotland/RCGP-Scotland/2019/RCGP-scotland-frontline-june-2019.ashx?la=en
- General Medical Council. GMC Data Explorer [Internet]. 2019 [cited 2019 May 4]. Available from: https://data.gmc-uk.org/gmcdata/home/#/
- Boendermaker PM, Conradi MH, Schuling J, et al. Core characteristics of the competent general practice trainer, a Delphi study. Adv Health Sci Educ. 2003;8(2):111–116.
- Waters M, Wall D. Educational CPD: an exploration of the attitudes of UK GP trainers using focus groups and an activity theory framework [Article]. Med Teach. 2008;30(8):250–259.
- Serpe RT, Stryker S. The symbolic interactionist perspective and identity theory. In: Schwartz SJ, Luyckx K, Vignoles VL, editors. Handbook of identity theory and research. Vol. 1. New York: Springer; 2011. p. 225–248.
- Society for the Study of Symbolic Interaction. About SSSI 2022. [cited 2022 21st February]. Available from: http://symbolicinteraction.org
- Joffe M, MacLeod S, Kedziora M, et al. GP trainers and trainees – trait and gender differences in personality: implications for GP training. Educ Primary Care. 2016;27(3):205–213.
- Glonti K, Struckmann V, Alconada A, et al. Exploring the training and scope of practice of GPs in England, Germany and Spain. Gac Sanit. 2017 Mar - Apr;33(2):148–155.
- Cruess RL, Cruess SR. Professionalism, communities of practice, and medicine’s social contract. J Am Board Fam Med. 2020;33(Supplement):S50–S56.
- Yin RK. Case study research: design and methods. 5th ed. USA: Sage Publications; 2014.
- O’Brien BC, Harris IB, Beckman TJ, et al. Standards for reporting qualitative research: a synthesis of recommendations. Acad Med. 2014 Sep;89(9):1245–1251.
- General Medical Council. National review of medical education and training in Scotland: 2017–18 [Internet]. 2018. [cited 2019 Dec 1]. Available from: https://www.gmc-uk.org/-/media/documents/gmc-national-review—scotland-national-report-2018-74421424.pdf
- Suri H. Purposeful sampling in qualitative research synthesis. Qual Res J. 2011 ;11(2):63–75.
- QSR International Pty Ltd. NVivo for mac [Internet]. 2017 [cited 2018 Feb 22]. Available from: http://www.qsrinternational.com/nvivo/nvivo-products/nvivo-for-mac
- Braun V, Clarke V. Thematic analysis. In: Cooper H, Camic PM, Long DL, et al., editors. APA handbook of research methods in psychology, Vol. 2: research designs: quantitative, qualitative, neuropsychological, and biological. Vol. 2. Washington DC: American Psychological Association; 2012. p. 57–71.
- Braun V, Clarke V. Reflecting on reflexive thematic analysis. Qualitative research in sport. Exer Health. 2019;11(4):589–597.
- Malterud K, Siersma VD, Guassora AD. Sample size in qualitative interview studies: guided by information power. Qual Health Res. 2016;26(13):1753–1760.
- Braun V, Clarke V. To saturate or not to saturate? Questioning data saturation as a useful concept for thematic analysis and sample-size rationales. Qual Res Sport Exerc Health. 2021;13(2):201–216.
- Birt L, Scott S, Cavers D, et al. Member checking: a tool to enhance trustworthiness or merely a nod to validation? Qual Health Res. 2016;26(13):1802–1811.
- Mahase E. GPs are being blamed for government failures in primary care, say doctors. BMJ. 2021;374:2234.
- Haynes L Experts fear dumbing down of GP training in post-COVID world [Internet]. 2020 [cited 2020 May 20]. Available from: https://www.gponline.com/experts-fear-dumbing-down-gp-training-post-covid-world/article/1683143
- Korstjens I, Moser A. Series: practical guidance to qualitative research. Part 4: trustworthiness and publishing. Eur J Gen Pract. 2017 Dec 5;24(1):120–124.
- Varpio L, Ajjawi R, Monrouxe LV, et al. Shedding the cobra effect: problematising thematic emergence, triangulation, saturation and member checking. Med Educ. 2017 Jan;51(1):40–50.
- Bi S, Vela MB, Nathan AG, et al. Teaching intersectionality of sexual orientation, gender identity, and race/ethnicity in a health disparities course. MedEdPORTAL. 2020;10970. [cited 2020 Aug 9]. https://www.mededportal.org/doi/abs/10.15766/mep_2374-8265.10970
- Gillies J, Bartlett M, Dowell J, et al. The Wass Report: moving forward 3 years on. Br J Gen Pract. 2020 May;70(694):228
- Bartlett M, Dowell J, Graham F, et al. Dundee’s longitudinal integrated clerkship: drivers, implementation and early evaluation. Educ Primary Care. 2019 Mar;30(2):72–79.
- Pope L, Dubras L. Delivering medical education for future healthcare needs: a community-focused challenge. Educ Primary Care. 2020;31(1):1–4. cited.
- Shanahan EM, van der Vleuten C, Schuwirth L. Conflict between clinician teachers and their students: the clinician perspective. Adv Health Sci Educ. 2019; journal article available at. doi:10.1007/s10459-019-09933-1
- Garth B, Kirby C, Nestel D, et al. A qualitative study of general practice supervisors professional identity. Aust J Gen Pract. 2019 Apr 26;48:315–320.
- Lyon-Maris J, Scallan S. Procedures and processes of accreditation for GP trainers: similarities and differences. Educ Primary Care. 2013;24(6):444–451.