ABSTRACT
Introduction
The mRNA vaccine technologies have progressed rapidly in recent years. The COVID-19 pandemic has accelerated the application of mRNA vaccines, with research and development and clinical trials underway for many vaccines. Application of the quality by design (QbD) framework to mRNA vaccine development and establishing standardized quality control protocols for mRNA vaccines are essential for the continued development of high-quality mRNA vaccines.
Areas covered
mRNA vaccines include linear mRNA, self-amplifying mRNA, and circular RNA vaccines. This article summarizes the progress of research on quality control of these three types of vaccines and presents associated challenges and considerations.
Expert opinion
Although there has been rapid progress in research on linear mRNA vaccines, their degradation patterns remain unclear. In addition, standardized assays for key impurities, such as residual dsRNA and T7 RNA polymerase, are still lacking. For self-amplifying mRNA vaccines, a key focus should be control of stability in vivo and in vitro. For circular RNA vaccines, standardized assays, and reference standards for determining degree of circularization should be established and optimized.
1. Introduction
The mRNA vaccine technologies using lipid nanoparticles (LNPs) as delivery system have progressed rapidly in recent years. In particular, the COVID-19 pandemic has accelerated the application of mRNA vaccines, which has led to revolutionary changes in the vaccine industry worldwide [Citation1–5]. The 2023 Nobel Prize in Physiology or Medicine was awarded to Katalin Karikó and Drew Weissman ‘for their discoveries concerning nucleoside base modifications that enabled the development of effective mRNA vaccines against COVID-19’ [Citation6]. Multiple mRNA vaccines encoding personalized new antigens showing promising results. mRNA technology has also been applied in cardiovascular, autoimmunological diseases, and rare diseases [Citation7,Citation8]. With continued developments in RNA chemistry and vaccinology, self-amplifying mRNA vaccines and circular RNA (circRNA) vaccines technologies have also demonstrated promising potential [Citation9–13]. A vaccine based on self-amplifying mRNA (sa-mRNA) has been approved for marketing in Japan [Citation14], and great strides have been made in preclinical and clinical trials of circRNA vaccines against COVID-19 and melanoma [Citation15,Citation16]. The advantages of mRNA vaccines include a short development cycle, rapid manufacturing, high clinical efficacy, good immunogenicity, availability for a broad group of recipients (not require the addition of adjuvants) and no requirement of a manufacturing plant with a high biosafety level (not based on live pathogens). The mRNA vaccines carry great potential for applications in infectious disease prevention and therapeutic vaccines for cancer [Citation17–20]. At the same time, there are also some challenges for mRNA vaccine, such as the risk of myositis and pericarditis in mRNA COVID-19 vaccines, the route of administration and targeted delivery [Citation21].
Currently, several mRNA vaccines have been approved for marketing () and hundreds of mRNA vaccines are undergoing clinical trials (). Due to this rapid development and application of mRNA vaccine technologies, quality control of mRNA vaccines has also become an important topic of research. This article discusses the progress of research on the quality control of vaccines and presents associated challenges and countermeasures to provide a reference for future studies on quality control of mRNA vaccines.
Table 1. mRNA vaccines currently approved for marketing or with emergency use authorization.
Table 2. mRNA vaccines currently in clinical trials (not include all).
2. Manufacturing processes for mRNA vaccines
2.1. Overview of the manufacturing process for linear mRNA vaccines and self-amplifying mRNA (sa-mRNA) vaccines
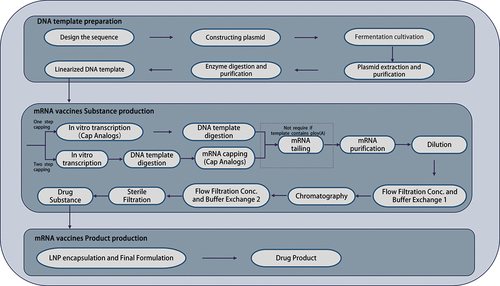
The process of linear mRNA vaccine and sa-mRNA vaccine production can be summarized as the preparation of plasmid DNA, preparation and purification of the linearized DNA template, in vitro transcription (IVT), mRNA processing and modification, mRNA purification, and lipid nanoparticle (LNP) encapsulation () [Citation48–50].
2.2. Overview of the manufacturing process for circRNA vaccines
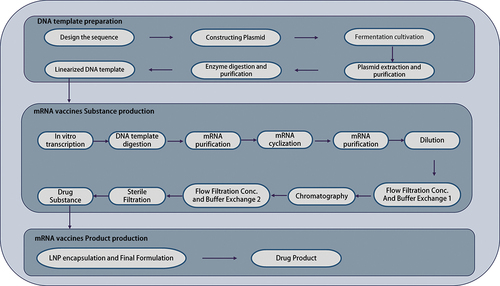
The manufacturing process for circRNA vaccines is similar to linear mRNA vaccines but requires in vitro transcription of the prepared RNA followed by a circularization reaction (). Compared to the sequence and structure of linear mRNA vaccines, the RNA structure of circRNA vaccines is circular and lacks a 5′ cap structure, thus relying on the internal ribosomal entry site (IRES) to initiate translation. In addition, it lacks a 3′ poly (A) tail structure, and its stability is instead enhanced by its circular structure [Citation51,Citation52]. Furthermore, circRNA vaccines also lack 5′ and 3′ untranslated regions (UTRs) but contain self-splicing sequences with group I or group II introns to induce circularization of their RNA precursors [Citation53,Citation54]. In addition, they can be circularized without such sequences using T4 RNA ligase, but this is little used in current manufacturing processes [Citation55,Citation56]. Finally, circRNA vaccines currently in development are manufactured without the use of modified nucleotides [Citation57].
3. Quality control of mRNA vaccines
3.1. Guidelines related to quality control
In December 2020, the World Health Organization (WHO) issued the technical document ‘Evaluation of the quality, safety, and efficacy of messenger RNA vaccines for the prevention of infectious diseases: Regulatory considerations’ (hereinafter referred to as the WHO guidelines), which addresses LNP-delivered, activity immunity, linear mRNA and sa-mRNA vaccines for the prevention of human infectious disease [Citation58]. The guidelines suggest areas of concern and regulatory considerations for key factors in vaccine production, quality control, non-clinical and clinical evaluation, as well as specific considerations for the development of multivalent mRNA vaccines or the modification of existing vaccine strains of certain pathogens (e.g. influenza virus or SARS-CoV-2), as appropriate. In addition to typical research and development registration considerations, the guidelines also provide recommendations for the rapid development of prioritized vaccines during public health emergencies [Citation58]. In February 2022, the United States Pharmacopeia (USP) issued the first edition of the ‘Analytical Procedures for mRNA Vaccine Quality – Draft Guidelines’ for linear mRNA vaccines and self-amplifying mRNA vaccines, which focuses on mRNA substances and provides methods for assessing quality attributes such as mRNA identity, purity, content, physical condition (integrity), and safety [Citation59].
In April 2023, the second edition of the ‘Analytical Procedures for mRNA Vaccine Quality – Draft Guidelines’ (hereafter referred to as the second edition of the USP guidelines) was issued for linear mRNA vaccines and self-amplifying mRNA vaccines, which applies to the whole life cycle of the entire mRNA vaccine product [Citation59]. Based on the concept of quality by design (QbD), characterization and release-testing are performed in three major stages: plasmid DNA templates, mRNA substances, and mRNA vaccines. Residual T7 RNA polymerase content was added as a new quality control item, and relevant assays for each quality control item were added, such as enzyme-linked immunosorbent assay (ELISA) for testing of residual dsRNA, high-performance liquid chromatography (HPLC) with Corona- charged aerosol detector (CAD) for qualitative and quantitative testing of the lipid component of LNPs [Citation55].
In April 2024, to meet the global need for common quality standards for mRNA vaccines across Europe and beyond, the European Pharmacopoiea is developing in parallel a series of three new general texts, mRNA vaccines for human use (5.36); mRNA substances for the production of mRNA vaccines for human use (5.39); DNA template for the preparation of mRNA substances (5.40), addressing key aspects related to the production and control of mRNA vaccines and their components, with the aim of supporting developers, manufacturers, regulatory agencies and national control laboratories worldwide [Citation60–62].
The Center for Drug Evaluation (CDE) of the National Medical Products Administration of China issued the ‘COVID-19 Prophylactic Vaccinology Technical Guidelines (Interim)’ (hereafter referred to as the CDE guidelines), which guides the research and development of mRNA vaccines in emergency situations and specifies the current basic requirements for this research [Citation63]. These guidelines generally apply only to non-self-amplifying mRNA vaccines; for self-amplifying mRNA vaccines, corresponding studies based on relevant product characteristics and attributes must also be conducted in accordance with these guidelines. These include template design; construction of plasmids containing the transcriptional templates; manufacturing processes; studies on quality characteristics; quality standards; stability studies; studies on the origin, selection, and quality standards of the packaging material in direct contact with the product; and periodic considerations for pharmacological development in emergency situations, as well as any changes in the process [Citation63]. In addition, other relevant technical guidelines issued by the WHO and other regulatory agencies should be consulted during quality control of mRNA vaccines, including non-clinical/clinical trials of vaccines, drug manufacturing, drug transportation and storage, vaccine stability studies, and post-marketing changes in vaccines [Citation64–72].
3.2. Quality attributes and quality standard development
Based on the manufacturing process of linear mRNA vaccines and sa-mRNA vaccines, the second edition of the USP guidelines specifies corresponding test items for the testing of plasmid templates, mRNA substances, and mRNA drug products, and recommends corresponding analytical methods (). These should be based on quality attributes and analytical methods, stable production of multiple batches, and relevant guidelines for establishing quality standards.
Table 3. Items and analysis assays for quality control of mRNA and sa-mRNA vaccines.
The circRNA vaccines also require quality control of degree of circularization due to the circularization reaction unique to their production process, but do not require quality attributes such as 5′ capping efficiency and 3′ poly(A) tail length [Citation59]. WHO guidelines suggest that quality standards can be relatively lenient in the early stages of development and that final standards should be based on the results of testing batches that have been confirmed safe and effective in clinical trials [Citation58]. The CDE guidelines require that vaccines submitted for approval for clinical use have preliminary quality standards based on process validation data. Risk control analysis should be conducted in accordance with relevant guidelines after marketing, and complete quality standards should be provided in conjunction with process validation [Citation63].
In 2002, the U.S. Food and Drug Administration (FDA) announced the ‘Pharmaceutical Current Good Manufacturing Practices (CGMPs) for the 21st Century’ initiative, introducing the concept of QbD as a basic tool for new drug development and quality control and proposing the use of process analytical technology (PAT) for implementation of QbD [Citation73]. Under the QbD framework, the development cycle starts with identifying patient requirements and using them to define the quality target product profile (QTPP). Subsequently, the critical quality attributes (CQA) of the product and its scope of use and risk assessment are established, integrating both clinical and non-clinical data on the safety and efficacy of the product. Next, the ranges of the critical process parameters (CPPs) are defined based on an understanding of how the manufacturing process influences the CQA of the product. Through this product – process understanding, a mathematical relationship between CPP and CQA is established to obtain a model of the vaccine production process at an operational level. The model is then used to determine the CPP ranges that result in the required CQA, from which a design space can be created and in which subspaces called normal operating ranges (NOR) are defined [Citation73].
A study utilized the design of experiments (DOE) tool in the QbD framework to construct an mRNA vaccine platform that could produce mRNA vaccines with a polydispersity index (PDI) ≤ 0.30 and particle size of 60–180 nm [Citation74]. By evaluating the factors affecting the efficacy and safety of mRNA vaccines, the QbD framework has been reported to yield a range of quality attributes, including RNA sequence integrity, RNA sequence accuracy, RNA yield, 5′ capping efficiency, residual host cell protein and DNA, residual template DNA, endotoxin, post-filtration pH, and salt concentration [Citation75].
3.3. Development and validation of assays
The WHO guidelines require that analytical methods are developed and validated for the identification, purity, and content of process-produced purified mRNA, as well as for key quality attributes, such as those affecting safety and quality. Furthermore, acceptable ranges of items related to methodological validation (e.g. precision) must be defined in accordance with these guidelines [Citation58]. The recently issued ICH Q14 and Q2 (R2) guidelines suggest that the development and validation of analytical methods for biologics based on the analytical quality by design (AQbD) framework and the product lifecycle concept, including the analytical target profile, technology selection, risk assessment, experimental design and optimization, method operational design regions, and ongoing monitoring, provide a basis for ensuring the long-term stability of the assay [Citation76,Citation77]. The CDE guidelines require that assay validation data provided at the time of submission be able to initially confirm the suitability of the assay. For CQA assays (such as encapsulation efficiency, capping efficiency, and potency.), information verifying consistency or suitability with the quality control and significance in the research and development phase and complete assay validation data should be provided at the marketing phase [Citation63].
3.4. Vaccine reference standards
WHO guidelines require vaccine manufacturers to establish reference standards for assay standardization; use mRNA vaccines from engineering-run batches as a reference in early development; identify and characterize suitable clinical trial batches for commercial manufacture in advanced development; provide information on reference standards when applying for marketing authorization; and select a suitable batch that has been clinically evaluated and fully characterized in terms of its chemical composition, purity, and biological activity, as a candidate reference material [Citation58]. The CDE guidelines require manufacturers to develop reference standards for determination of nucleic acid content, purity, and biological activity at the time of submission and provide preliminary research data on the source, preparation, test results, calibration process, and stability studies of the reference standards [Citation63]. To compare the test results of vaccines from different research institutions, international or national reference standards for key residual impurities such as double-stranded RNA (dsRNA) and T7 RNA polymerase and their biological activities in vitro should be developed to standardize and harmonize assays for key impurities and potency.
4. Challenges and countermeasures in the quality control of linear mRNA vaccines
4.1. Optimization of the defined CQA test method
At present, there are defined test methods for the CQA of mRNA vaccines, but some methods still need to be optimized. For example, mRNA capping can be completed by the co-transcription capping during the IVT process or the enzymatic capping after the IVT process. The commonly used Cap analogues include ARCA, Cap 0, and Cap 1 structural analogues. The existing test methods of cap efficiency are difficult to isolate and identify the RNA fragments of different cap analogues with high resolution. Thus, it needs to be optimized.
4.2. Applications of the QbD concept
Currently, the application of QbD in vaccine development, production, and quality control is less mature than in the development of small-molecule drugs [Citation78,Citation79]. To develop an mRNA vaccine using the QbD framework, the CQA of the finished vaccine should be fully considered during research, development, and design of the product, and the product should be optimized and improved to enhance its quality. It has been reported that the design of the mRNA vaccine production process requires a comprehensive understanding of the relationship between CQAs, CPPs, and CMAs. The introduction of multiple real-time monitoring tools (PAT) in the vaccine production process allows real-time monitoring of the vaccine CQA to ensure the quality of the finished product, thereby accelerating the research, development, production, and approval of mRNA vaccines.
The application of QbD and the design of experiments (DOE) tool allow the effects of CPPs in the production process on CQAs, as well as the design space, to be characterized. In addition, new mathematical models of qualitative and quantitative methods are integrated to evaluate the direction, degree, and characteristics of the effects of CPPs, such as nucleotide triphosphate and Mg2+ concentration, T7 RNA polymerase concentration, and reaction time on vaccine CQA, such as mRNA integrity and sequence accuracy. The models can be used to quantify and plot the effects of the four CPPs on mRNA yield, thereby yielding the operational design space for the mRNA preparation reaction system [Citation75]. Bryśkiewicz et al. concluded that the implementation of QbD in mRNA-LNP drug product development is closely associated with the structure of the delivery system and the main therapeutic targets. The quality target product profile (QTTP) of LNP formulations for RNA delivery are safety, efficacy and pharmaceutical. The CQA include particle size, polydispersity index (PDI), encapsulation efficiency, and lipid content. The CMA include nitrogen/phosphorus ratio, lipid type, and biodegradability. The CPP include temperature, microfluidics, and filtration. Since the CQA of these vaccines are determined by CMA and CPP, these are used to optimize the design of LNPs [Citation80].
4.3. Vaccine potency
Currently, mRNA vaccine potency is mainly evaluated using protein expression in vitro cellular assays. However, the composition of mRNA vaccines is more complex, and factors other than protein expression, such as ionizable cationic lipids, may affect vaccine immunogenicity. The content of major residual impurities also affects the in vivo activity of the vaccine [Citation59]. Therefore, developing methodology and standards for in vitro potency testing that accurately reflect in vivo vaccine activity remains a key bottleneck in quality control. An advantage of linear mRNA vaccines is that they substantially activate T cell immunity. However, standardization of vaccine-induced T cell immunity assays is difficult due to the large number of factors influencing the experimental process, which presents a major challenge for standardizing the evaluation of mRNA vaccine-induced T cell immune responses [Citation81].
4.4. Quality control of key residual impurities
The WHO publication ‘Evaluation of the quality, safety, and efficacy of messenger RNA vaccines for the prevention of infectious diseases: Regulatory considerations’ recommends that testing for residual levels of relevant impurities as part of quality control may be reduced or discontinued once production processes have been adequately validated for their suitable removal and production consistency has been demonstrated, if agreed upon by the national regulatory authority [Citation58]. For the quality control of major residual impurities, the development of standardized quality control methods and quality standards should fully consider the production process, the biological effects of the impurity, and the effect on the body.
Linear mRNA vaccines are produced with different lengths and structures of dsRNAs, such as complementary hairpin and double-stranded structures. Different dsRNAs activate innate immune responses with different characteristics; some dsRNAs act as adjuvants, whereas others may induce inflammation [Citation82–84]. Currently, ELISA or immunoblotting methods using J2/K2 monoclonal antibodies are used to detect residual dsRNA. Some studies have reported that dsRNAs of different shapes have different binding affinities to J2/K2 monoclonal antibodies, which can affect testing accuracy [Citation76]. The second edition of the ‘Analytical Procedures for mRNA Vaccine Quality – Draft Guidelines’ issued by the USP recommends the use of ELISA or immunoblotting methods based on K1/K2 monoclonal antibodies for dsRNA, but its suitability needs to be verified [Citation59].
It is therefore necessary to develop and optimize a standardized assay for residual dsRNA. Another possibility is to develop a cell-based assay for detecting residual dsRNA. It may also be possible to elucidate which types of residual dsRNA are present in vaccines after the production process is established, and then to perform quality control for these dsRNAs. The level of residual dsRNA has been reported to be less than 1 ng/μg RNA, but no data from studies using this as a quality criterion are currently available [Citation83]. In the second edition of the ‘Analytical Procedures for mRNA Vaccine Quality – Draft Guidelines’ issued by the USP, ELISA was newly added as an assay for quality control detection of residual T7 RNA polymerase [Citation59]. The development of standardized assays and reference ranges for the detection of residual T7 RNA polymerase should be evaluated.
4.5. Stability
Vaccine stability is crucial for determining the shelf life and preservation conditions for the vaccine [Citation85–87]. However, mRNA vaccine stability has not been thoroughly studied. The WHO publication ‘Evaluation of the quality, safety, and efficacy of messenger RNA vaccines for the prevention of infectious diseases: Regulatory considerations’ recommends that manufacturers provide national regulatory agencies with sufficient data to demonstrate the stability of the product under storage, distribution, and use conditions [Citation58]. A recent WHO Science Council report on mRNA vaccine technology highlighted that mRNA vaccine stability should be investigated under high-temperature conditions [Citation88]. Studies have found that oxidation and hydrolysis of the tertiary amine groups of ionizable cationic lipids in linear mRNA vaccines during long-term storage produces active components that undergo chemical reactions with the mRNA molecules, which leads to ineffective translation into proteins, thereby affecting vaccine immunogenicity [Citation89]. Conditions such as temperature, pH, light, humidity, buffer type, key storage items (such as cryoprotectants and dispersants), repeated freezing and thawing, and other relevant physical and chemical properties affect mRNA vaccine stability; attempts should be made to determine the degradation patterns of mRNA vaccines.
In addition, in vivo stability studies of linear mRNA vaccines should be conducted to provide a reference for improving vaccine immunogenicity. Storage stability has been reported to be affected by structural differences in nucleic acids and the degree of base pairing. Vaccines with a higher proportion of single-stranded RNA structures are less stable. The LNP structure is assembled in the microfluidic channel and fully developed post dialysis. This process affects the CQA of LNP – mRNA vaccines, including its stability [Citation90]. A study compared the effect of tangential flow filtration dialysis on the stability of mRNA vaccines using pH 7.6 buffer directly or using pH 4.0 buffer followed by pH 7.6 buffer; the two-step dialysis method resulted in good storage stability of the prepared mRNA vaccines, which were stored for at least six months at 5°C or − 20°C, with an increase in the particle size and a lower empty-carrier rate [Citation91]. A novel cationic lipid with three tertiary amine groups designed using supramolecular chemistry does improve binding to RNA, and the isomerization of hydroxyl and amide bonds in its structure improves the stability of LNP [Citation92]. Encapsulated mRNA vaccines were stored for two months at 4°C and 37°C; the formulations had stable properties and were well-tolerated in animals, suggesting that the stability of mRNA vaccines can be improved by optimizing the molecular design of LNP lipids [Citation92].
4.6. Quality control of LNPs
LNPs are used as the delivery system in mRNA vaccines [Citation93–95]. For novel excipients (e.g. cationic lipids), detailed information on the production process and quality control, including raw materials and intermediates, should be provided where possible. A detailed characterization of the LNPs should be performed, as well as a specific description of any formulation features that may affect the vaccine’s quality, safety and efficacy, the impacts of which should be considered in the formulation development process [Citation96]. The proportion of ionizable lipids in LNP lipid compositions affects the encapsulation rate of the mRNA vaccine and the nanoparticle self-assembly process; lipid species, the charge of the headgroup, and the hydrophobicity of the tail affect the particle size, morphology, and stability of the mRNA vaccine [Citation97].
The use of HPLC equipped with a CAD for qualitative and quantitative detection of lipid components in mRNA vaccines has been added to the second edition of the ‘Analytical Procedures for mRNA Vaccine Quality – Draft Guidelines’ issued by the USP [Citation55]. Ionizable cationic lipids in mRNA vaccines have been shown to activate the innate immune response and act as vaccine adjuvants. Cholesterol may also activate the innate immune response and act as a vaccine adjuvant, so it is necessary to investigate and elucidate biological functions in mRNA vaccines and to establish quality standards with respect to these functions [Citation98]. Some studies have reported that the presence of water in the inner core of the LNP affects the storage stability of mRNA vaccines, the amount of which is mainly related to the lipid composition and the internal structure after assembly with mRNA [Citation91].
5. Challenges and countermeasures in quality control of sa-mRNA vaccines
The production process of sa-mRNA vaccines is similar to linear mRNA vaccines, such that the quality control of linear mRNA vaccines can be used as a reference. However, specific test items, methods, and reference ranges arising from the characteristics of sa-mRNA vaccines, such as their longer sequences, warrant attention [Citation99,Citation100].
5.1. Stability
Since the additional RNA-dependent RNA polymerase encoded in sa-mRNA vaccines enables them to synthesize their own sequences up to approximately 7,000 bp in length, possibly making them more susceptible to degradation, research on the stability of sa-mRNA vaccines should be a priority; however, there are currently few studies on the stability of sa-mRNA vaccines [Citation101]. Whether certain specific base sequences or RNA spatial structures are susceptible to degradation, degradation patterns of these vaccines, and early and sensitive indicators that can be used to characterize the degradation that occurs in these vaccines have been investigated. The longer sequence leading to in vivo stability also warrants attention.
5.2. Application of QbD to optimize the in vitro transcription reaction system
The mRNA sequence identity, integrity, and purity are vaccine CQAs. The longer sequence of sa-mRNA vaccines is a major challenge for IVT, as is ensuring the accuracy, integrity, and purity of target product sequences. The proportions of each component of the in vitro transcription reaction system will be different from those of linear mRNA vaccines [Citation102]. Models should be constructed to investigate and quantify the impacts of CPP and CMA on the CQA of self-amplifying mRNA vaccines and the quality of the final product, as well as determine the operational design space based on a QbD framework and using DOE tools. The quality of linearized DNA templates has been shown to have a substantial impact on the in vitro transcription process for sa-mRNA vaccines [Citation103]. Samnuan et al. found that Mg2+ content and its interaction with nucleoside triphosphates substantially affected mRNA quality and yield, that acetate ions affected the in vitro transcription process to a greater extent than Cl− ions, that the addition of sodium acetate did not increase RNA yield further, and that pyrophosphatase was not essential for in vitro transcription [Citation104].
5.3. Quality control of key residual impurities
Key residual impurities are a CQA of sa-mRNA vaccines. The dsRNA of different structures and lengths is generated during in vitro transcription and mRNA preparation. In addition, sa-mRNA vaccines are replicated in vivo, such that the target mRNA sequences will also form dsRNA structures in the body. This situation leads to the activation of the innate immune response, which may be different from linear mRNA vaccines. Thus, the quality standard for residual dsRNA in sa-mRNA vaccines may differ from that of linear mRNA vaccines, necessitating further study. Like linear mRNA vaccines, the quality control study of residual T7 RNA polymerase should be carried out.
5.4. Quality control of particle size
Particle size has been shown to be a CQA for sa-mRNA vaccines and has major impacts on drug loading, stability, biodistribution, cellular uptake, endocytosis, and release, and immune response [Citation105–107]. Therefore, robust, and reliable particle size analysis methods are essential for meeting product quality consistency requirements for multiple batches of mRNA vaccine production. The mRNA vaccine particles are now widely believed to have a uniform spherical structure. The dynamic light scattering (DLS) has been used for the determination of its sizes [Citation105]. However, it was recently found, using different assay techniques, that sa-mRNA vaccines with different proportions of lipid components exhibited non-spherical, heterogeneous, ‘two-core’ structures with lipid and aqueous compartments and inter-particle variability [Citation108]. This ‘two-core’ structure is due to the increased pH during the preparation of the mRNA-LNP solution, which causes the ionizable lipids to become neutral and weakens the interaction with mRNA. This results in a separation between the hydrophilic (mRNA) and hydrophobic (lipid) cores, which are stabilized by amphiphilic DSPC lipids after separation. Further experiments have shown that increased numbers of these structures result in decreased encapsulation rates [Citation108]. Whether the non-spherical, inhomogeneous ‘dual-core structure’ affects the accuracy of particle size and size distribution results determined by DLS remains to be investigated. None of the current guidelines related to mRNA vaccines explicitly mention quality control of the morphological structure of mRNA vaccine particles.
6. Challenges and countermeasures in quality control of circRNA vaccines
The quality control of linear mRNA vaccines can still be used as a reference for the quality control of circRNA vaccines. However, unique test items, assays, and standard ranges resulting from the inherent characteristics of circRNA vaccines, such as quality control of degree of circularization, warrant attention.
6.1. Quality control of degree of circularization
Degree of circularization is a CQA of circRNA vaccines that is often determined using capillary electrophoresis (CE). However, because of the similar molecular weights of the mRNA circularization precursors and circRNA sequences, the resolution of the circularization rate is suboptimal when using this method, which affects the accuracy of the results [Citation102]. Therefore, with reference to the ICH Q2 and Q14 guidelines, circularization rate assays for circRNA vaccines have been developed and validated through a strategy of using assays with different underlying principles from existing assays or combinations of such assays. For example, a combination of CE and reversed-phase high-performance liquid chromatography can be considered [Citation76,Citation77].
When RNA is circularized by self-splicing with group I or group II introns, higher degree of circularization not only result in higher circRNA yields but are also conducive to vaccine quality control [Citation109]. Studies have shown that higher degree of circularization are not only associated with self-splicing introns but also with the target mRNA sequence, which may be due to the different spatial structures produced by different RNA sequences. In short, the two should be selected to match each other to produce a higher circularization rate. In recent studies, artificial intelligence has been used to screen for self-splicing intron sequence elements that match with target sequences before aligning with suitable sequences through experiments [Citation110–112]. In addition, the use of DOE tools can be used to optimize CPP and CMA to improve the circularization rate and model quantification to determine the operational design space [Citation98].
6.2. Quality control of key residual impurities
RNA homology arms are eliminated during the mRNA circularization process. Unsuccessfully circularized mRNA precursor molecules are circularized together with multiple mRNA molecules to form multimeric structures. The effect of these structures on vaccine efficacy should be determined experimentally, as well as whether these are process- or product-related impurities, along with the relevant quality standards [Citation109]. Current circRNA vaccines lack modified nucleotides, meaning that the dsRNA produced during in vitro transcription may be different from the dsRNA produced during linear mRNA vaccine production. The dsRNA is also produced during the circularization reaction, and the characteristics of innate immune response activation by circRNA may also differ from those of linear mRNA. Thus, the quality standards for residual dsRNA in circRNA vaccines may differ from those of mRNA vaccines, and studies on assays for detecting residual dsRNA in circRNA vaccines and their relevant quality standards should be conducted. In addition, the quality control study of residual T7 RNA polymerase should be carried out [Citation113,Citation114].
6.3. Stability
Although circRNA is more stable, it can still be cleaved by RNases. The molecular weight of open, circular mRNA is the same as that of the parent circRNA. Therefore, if molecular weight-based methods such as CE fail to distinguish between circRNA and nicked circular RNA, then the addition of a poly(A) tail to the 3′ end of the open circular mRNA may help in determining the content of open circular mRNA in the vaccine. However, the accuracy of this method may be affected by the efficiency of polyadenylation. Because circRNA and nicked circular mRNA have different structures, size exclusion-high-performance liquid chromatography (SEC-HPLC) can also be used to investigate whether circRNA and nicked circular mRNA can be effectively distinguished. Whether the circRNA molecules also undergo a chemical reaction with the lipid components of LNPs during long-term storage and affect translation efficiency also remains to be investigated. Studies have shown that proteins are expressed for a longer duration in vivo with circRNA vaccines than with linear mRNA vaccines, but there are no relevant studies indicating whether this is because circRNA vaccines are more stable and less susceptible to degradation in vivo or that they are more efficiently translated or have a longer translation duration [Citation115–117].
7. Expert opinion
The mRNA vaccine technologies have progressed rapidly in recent years, and the COVID-19 pandemic has accelerated the approval of mRNA vaccines for marketing. The mRNA vaccine technologies carry great potential for applications in infectious disease prevention and therapeutic vaccines for cancer; quality control of mRNA vaccines has also become an important issue of research [Citation118–121].
QbD is essential in the development of mRNA vaccine technologies, and the quality of the final vaccine product should be fully considered, already at the design phase. The CQA of mRNA vaccines is investigated and determined from CMA and CPP in conjunction with vaccine characteristics and relevant guidelines [Citation102,Citation103]. Corresponding quality control methods are developed and validated based on the AQbD framework and the product life cycle concept in accordance with the ICH Q14 and Q2 (R2) guidelines. Quality standards can be relatively lenient at the early stages of development, but final standards should be based on the results of testing batches that have been confirmed safe and effective in clinical trials [Citation76,Citation77].
There are still many challenges in quality control of the three mRNA vaccines (). The research on quality control of linear mRNA vaccines has made rapid progress. Some factors of the neutralization antibody detection assay affect the accuracy and repeatability of results, such as incubation time of virus and serum, cell inoculation density. Therefore, standardized assays for neutralizing antibody potency should be developed. The published study adopted the AQbD concept to establish standardized neutralization antibody analytical procedure for clinical samples immunized with COVID-19 vaccines, which could reduce the error in the laboratory, and provides a methodology for comparing the effectiveness of different COVID-19 vaccines [Citation79]. Standardized assays for degradation patterns and for key impurities, such as residual dsRNA and T7 polymerase, are still lacking, and reference standards with detailed scientific rationales should be developed [Citation54,Citation55]. Quality control of sa-mRNA vaccines and circRNA vaccines can be performed with reference to quality control of linear mRNA vaccines but should focus on in vivo and in vitro stability due to the longer sequence of sa-mRNA vaccines, which makes them more prone to degradation. In addition, the effects of nanoparticle morphology and structure on particle size also warrant attention [Citation93,Citation100].
Table 4. The summarization of challenges and countermeasures of mRNA vaccine quality control research.
For circular RNA vaccines, specific standardized assays and quality standards for determining degree of circularization should be established [Citation102,Citation107]. With increasing research on mRNA vaccines and the continuous development of mRNA vaccine technologies, the WHO and other national regulatory agencies should also continuously update and improve the guidelines for mRNA vaccines and establish international or national reference standards in a timely manner. It is the important to harmonize guidelines and reference standards internationally. For example, international or national reference standards for key residual impurities such as dsRNA and T7 RNA polymerase and their biological activities in vitro should be developed to standardize and harmonize assays for key impurities and potency, as well as provide tools for quality control and evaluation of mRNA vaccines worldwide.
Article highlights
mRNA vaccine technologies have progressed rapidly, and COVID-19 mRNA vaccines have already been approved for marketing. However, no guidelines or international reference standards for single-mRNA vaccines have yet been issued by the World Health Organization (WHO), the European Pharmacopoiea or national regulatory agencies.
mRNA vaccines include linear mRNA, self-amplifying mRNA, and circular RNA vaccines. Different types of vaccines have different sequences, structural characteristics, and mechanisms of immunity, which must be considered during quality control.
The degradation patterns of linear mRNA vaccines have not yet been elucidated and standardized assays for key impurities, such as residual dsRNA and T7 RNA polymerase, are still lacking. Standardized assays and reference standards are required to determine in vitro biological activity.
Since the longer sequence of self-amplifying mRNA vaccines makes them more prone to degradation, development of such vaccines should focus on controlling stability in vitro and in vivo, as well as the effects of nanoparticle morphology and structure on particle size determinations. For circular RNA vaccines, specific standardized assays, and appropriate quality standards for determining degree of circularization should be established.
Under the quality by design (QbD) framework, investigating the effects of critical material properties (CMAs) and critical process parameters (CPPs) on the critical quality attributes (CQA) of mRNA vaccines and creating the operational design space is a key element of mRNA vaccine development.
Declaration of interest
The authors have no relevant affiliations or financial involvement with any organization or entity with a financial interest in or financial conflict with the subject matter or materials discussed in the manuscript. This includes employment, consultancies, honoraria, stock ownership or options, expert testimony, grants, or patents received or pending, or royalties.
Reviewers disclosure
Peer reviewers on this manuscript have no relevant financial relationships or otherwise to disclose.
Author contributions
CY Hu and Y Bai conceived and drafted the manuscript; JY Liu, YP Wang, Q He, XX Zhang, FR Cheng provided valuable discussions; ZL Liang, QY Mao and M Xu revised the manuscript. All authors have read and approved the article.
Additional information
Funding
References
- He Q, Mao Q, Zhang J, et al. COVID-19 vaccines: current understanding on immunogenicity, safety, and further considerations. Front Immunol. 2021;12:669339. doi: 10.3389/fimmu.2021.669339
- Ye Z, Harmon J, Ni W, et al. The mRNA vaccine revolution: COVID-19 has launched the future of vaccinology. ACS Nano. 2023 Aug 22;17(16):15231–15253. doi: 10.1021/acsnano.2c12584
- Cheng F, Wang Y, Bai Y, et al. Research advances on the stability of mRNA vaccines. Viruses. 2023 Mar 2;15(3):668. doi: 10.3390/v15030668
- Mao Q, Xu M, He Q, et al. COVID-19 vaccines: progress and understanding on quality control and evaluation. Signal transduction and targeted therapy. Signal Transduct Target Ther. 2021 May 18;6(1):199. doi: 10.1038/s41392-021-00621-4
- Bai Y, He Q, Yang J, et al. B.1.351 SARS-CoV-2 variant exhibits higher virulence but less viral shedding than that of the ancestral strain in young nonhuman primates. Microbiol Spectr. 2022 Oct 26;10(5):e0226322. doi: 10.1128/spectrum.02263-22
- The Nobel Prize in physiology or medicine 2023. The Nobel Prize; [ cited 2023 Oct 2]. Available from: https://www.nobelprize.org/prizes/medicine/2023/press-release/
- Wang B, Pei J, Xu S, et al. Recent advances in mRNA cancer vaccines: meeting challenges and embracing opportunities. Front Immunol. 2023;14:1246682. doi: 10.3389/fimmu.2023.1246682
- Shen G, Liu J, Yang H, et al. mRNA therapies: pioneering a new era in rare genetic disease treatment. J Control Release. 2024 Apr 12;369:696–721. doi: 10.1016/j.jconrel.2024.03.056
- Bai Y, Wang Q, Liu M, et al. The next major emergent infectious disease: reflections on vaccine emergency development strategies. Expert Rev Vaccines. 2022 Apr;21(4):471–481. doi: 10.1080/14760584.2022.2027240
- Maruggi G, Mallett CP, Westerbeck JW, et al. A self-amplifying mRNA SARS-CoV-2 vaccine candidate induces safe and robust protective immunity in preclinical models. Mol Ther. 2022 May 4;30(5):1897–1912. doi: 10.1016/j.ymthe.2022.01.001
- Vogel AB, Lambert L, Kinnear E, et al. Self-Amplifying RNA vaccines give equivalent protection against influenza to mRNA vaccines but at much lower doses. Mol Ther. 2018 Feb 7;26(2):446–455. doi: 10.1016/j.ymthe.2017.11.017
- Beissert T, Perkovic M, Vogel A, et al. A Trans-amplifying RNA vaccine strategy for induction of potent protective immunity. Mol Ther. 2020 Jan 8;28(1):119–128. doi: 10.1016/j.ymthe.2019.09.009
- Zhu F, Ma S, Wen H, et al. Development of a novel circular mRNA vaccine of six protein combinations against Staphylococcus aureus. J Biomol Struct Dynamics. 2023 Dec;41(20):10525–10545. doi: 10.1080/07391102.2022.2154846
- Japan’s ministry of health, labour and welfare approves CSL and Arcturus therapeutics’ ARCT-154, the first self-amplifying mRNA vaccine approved for COVID in Adults. ARCTURUS. [ cited 2023 Nov 28]. Available from: https://ir.arcturusrx.com/news-releases/news-release-details/japans-ministry-health-labour-and-welfare-approves-csl-and
- Qu L, Yi Z, Shen Y, et al. Circular RNA vaccines against SARS-CoV-2 and emerging variants. Cell. 2022 May 12;185(10):1728–1744.e16. doi: 10.1016/j.cell.2022.03.044
- Li H, Peng K, Yang K, et al. Circular RNA cancer vaccines drive immunity in hard-to-treat malignancies. Theranostics. 2022;12(14):6422–6436. doi: 10.7150/thno.77350
- Yuan Y, Gao F, Chang Y, et al. Advances of mRNA vaccine in tumor: a maze of opportunities and challenges. Biomark Res. 2023 Jan 18;11(1):6. doi: 10.1186/s40364-023-00449-w
- Gote V, Bolla PK, Kommineni N, et al. A comprehensive review of mRNA vaccines. Int J Mol Sci. 2023 Jan 31;24(3):2700. doi: 10.3390/ijms24032700
- Chavda VP, Jogi G, Dave S, et al. mRNA-based vaccine for COVID-19: they are new but not unknown! Vaccines. 2023 Feb 22;11(3):507. doi: 10.3390/vaccines11030507
- Pardi N, Hogan MJ, Weissman D. Recent advances in mRNA vaccine technology. Curr Opin Immunol. 2020 Aug;65:14–20. doi: 10.1016/j.coi.2020.01.008
- Rzymski P, Szuster-Ciesielska A, Dzieciątkowski T, et al. mRNA vaccines: The future of prevention of viral infections? J med virol. 2023 Feb;95(2):e28572. doi: 10.1002/jmv.28572
- August 23, 2021 approval letter-comirnaty. Food and Drug Administration. [ cited 2021 Aug 23]. Available from: https://www.fda.gov/media/151710/download
- January 31, 2022 approval letter-SPIKEVAX. Food and Drug Administration; [cited 2022 Jan 31]. Available from: https://www.fda.gov/media/155815/download
- COVID-19 mRNA vaccine of CSPC has been put into emergency use in China. CSPC Holdings Company Limited; [cited 2023 Mar 22]. Available from: https://www.e-cspc.com/details/details_92_4894.html
- DAICHIRONA® for intramuscular injection (monovalent: original strain), mRNA COVID-19 vaccine, approved for manufacturing and marketing as booster vaccination in Japan. [cited 2023 Aug 2]. Available from: https://www.daiichisankyo.com/files/news/pressrelease/pdf/202307/20230802_E.pdf
- About the novel coronavirus mutant mRNA vaccine (Omicron XBB. 1.5) announcement of approval for emergency use. WALVAX Biotechnology Co. Ltd; [cited 2023 Dec 1]. Available from: https://static.cninfo.com.cn/finalpage/2023-12-01/1218497047.PDF
- COVID-19 bivalent mRNA vaccine of CSPC was put into emergency use. CSPC Holdings Company Limited; [cited 2023 Dec 1]. Available from: https://www.e-cspc.com/details/details_92_5210.html
- Sahin U, Oehm P, Derhovanessian E, et al. An RNA vaccine drives immunity in checkpoint-inhibitor-treated melanoma. Nature. 2020 Sep;585(7823):107–112. doi: 10.1038/s41586-020-2537-9
- Safety, tolerability, and immunogenicity of lk101 alone in participants with incurable solid tumors. ClinicalTrials.gov. [cited 2023 Sep 26]. Available from: https://clinicaltrials.gov/search?cond=NCT06054932
- A Study of mRNA-5671/V941 as monotherapy and in combination with pembrolizumab (V941-001). ClinicalTrials.gov; [cited 2019 May 14]. Available from: https://clinicaltrials.gov/search?cond=NCT03948763
- Intratumoral TriMix Injections in Early Breast Cancer Patients. ClinicalTrials.gov. [cited 2018 Dec 27]. Available from: https://clinicaltrials.gov/search?cond=NCT03788083
- Porciuncula A, Morgado M, Gupta R, et al. Spatial mapping and immunomodulatory role of the OX40/OX40L pathway in human non-small cell lung cancer. Clin Cancer Res. 2021 Nov 15;27(22):6174–6183. doi: 10.1158/1078-0432.CCR-21-0987
- A Phase II clinical trial comparing the efficacy of ro7198457 versus watchful waiting in patients with ctDNA-positive, resected stage II (High Risk) and Stage III colorectal cancer. ClinicalTrials.gov. [cited 2023 Dec 12]. Available from: https://clinicaltrials.gov/search?cond=NCT04486378
- An efficacy study of adjuvant treatment with the personalized cancer vaccine mRNA-4157 and pembrolizumab in participants with high-risk melanoma (KEYNOTE-942). ClinicalTrials.gov. [cited 2019 Jul 18]. Available from: https://clinicaltrials.gov/search?cond=NCT03897881
- COVID-19: A study to evaluate safety, reactogenicity and immunogenicity of the SARS-CoV-2 mRNA vaccine CVnCoV in adults with co-morbidities. ClinicalTrials.gov. [cited 2021 Apr 26]. Available from: https://clinicaltrials.gov/search?cond=NCT04860258
- A phase iii clinical study of a SARS-CoV-2 messenger ribonucleic acid (mRNA) vaccine candidate against COVID-19 in population aged 18 years and above. ClinicalTrials.gov. [cited 2021 Apr 15]. Available from: https://clinicaltrials.gov/search?cond=NCT04847102
- Essink B, Chu L, Seger W, et al. The safety and immunogenicity of two Zika virus mRNA vaccine candidates in healthy flavivirus baseline seropositive and seronegative adults: the results of two randomised, placebo-controlled, dose-ranging, phase 1 clinical trials. Lancet Infect Dis. 2023 May;23(5):621–633. doi: 10.1016/S1473-3099(22)00764-2
- A study of zika vaccine mRNA-1893 in adult participants living in endemic and non-endemic flavivirus areas. ClinicalTrials.gov. [cited 2021 Jun 8]. Available from: https://clinicaltrials.gov/search?cond=NCT04917861
- A study to evaluate the safety and efficacy of mRNA-1345 vaccine targeting respiratory syncytial virus (RSV) in Adults ≥60 Years of Age. ClinicalTrials.gov. [cited 2021 Nov 19]. Available from: https://clinicaltrials.gov/search?cond=NCT05127434
- A study to evaluate the safety and immunogenicity of a single dose of H1ssF-3928 mRNA-LNP in healthy adults. ClinicalTrials.gov. [cited 2023 Apr 5]. Available from: https://clinicaltrials.gov/study/NCT05755620?cond=NCT05755620&rank=1
- A Study of mRNA-1010 Seasonal Influenza Vaccine in Adults. ClinicalTrials.gov. [cited 2022 Jun 13]. Available from: https://clinicaltrials.gov/search?cond=NCT05415462
- Chawla SP, Van Tine BA, Pollack SM, et al. Phase II randomized study of CMB305 and atezolizumab compared with atezolizumab alone in soft-tissue sarcomas expressing NY-ESO-1. J Clin Oncol. 2022 Apr 20;40(12):1291–1300. doi: 10.1200/JCO.20.03452
- Study to Evaluate JCXH-211 as monotherapy in patients with malignant solid tumors. ClinicalTrials.gov. [cited 2023 Feb 14]. Available from: https://clinicaltrials.gov/search?cond=NCT05727839
- Crosby EJ, Hobeika AC, Niedzwiecki D, et al. Long-term survival of patients with stage III colon cancer treated with VRP-CEA(6D), an alphavirus vector that increases the CD8+ effector memory T cell to Treg ratio. J Immunother Cancer. 2020 Nov;8(2):e001662. doi: 10.1136/jitc-2020-001662
- Study of an individualized vaccine targeting neoantigens in combination with immune checkpoint blockade for patients with colon cancer. ClinicalTrials.gov. [cited 2022 Jul 13]. Available from: https://clinicaltrials.gov/search?cond=NCT05456165
- Crosby EJ, Acharya CR, Haddad AF, et al. Stimulation of oncogene-specific tumor-infiltrating T cells through combined vaccine and αPD-1 enable sustained antitumor responses against established HER2 Breast Cancer. Clin Cancer Res. 2020 Sep 1;26(17):4670–4681. doi: 10.1158/1078-0432.CCR-20-0389
- Study of GRT-R910 COVID-19 boost vaccine in healthy volunteers. ClinicalTrials.gov. [cited 2021 Dec 8]. Available from: https://clinicaltrials.gov/search?cond=NCT05148962
- Hu C, Liu J, Cheng F, et al. Amplifying mRNA vaccines: potential versatile magicians for oncotherapy. Front Immunol. 2023;14:1261243. doi: 10.3389/fimmu.2023.1261243
- Whitley J, Zwolinski C, Denis C, et al. Development of mRNA manufacturing for vaccines and therapeutics: mRNA platform requirements and development of a scalable production process to support early phase clinical trials. Transl Res. 2022 Apr;242:38–55. doi: 10.1016/j.trsl.2021.11.009
- Schlake T, Thess A, Fotin-Mleczek M, et al. Developing mRNA-vaccine technologies. RNA Biol. 2012 Nov;9(11):1319–1330. doi: 10.4161/rna.22269
- Zhang Y, Xue W, Li X, et al. The biogenesis of nascent circular RNAs. Cell Rep. 2016 Apr 19;15(3):611–624. doi: 10.1016/j.celrep.2016.03.058
- Niu D, Wu Y, Lian J. Circular RNA vaccine in disease prevention and treatment. Signal Transduct Target Ther. 2023 Sep 11;8(1):341. doi: 10.1038/s41392-023-01561-x
- Seephetdee C, Bhukhai K, Buasri N, et al. A circular mRNA vaccine prototype producing VFLIP-X spike confers a broad neutralization of SARS-CoV-2 variants by mouse sera. Antiviral Res. 2022 Aug;204:105370. doi: 10.1016/j.antiviral.2022.105370
- Chen C, Wei H, Zhang K, et al. A flexible, efficient, and scalable platform to produce circular RNAs as new therapeutics. 2022:2022–05.
- Bai Y, Liu D, He Q, et al. Research progress on circular RNA vaccines. Front Immunol. 2022;13:1091797. doi: 10.3389/fimmu.2022.1091797
- Li M, Wang Y, Wu P, et al. Application prospect of circular RNA-based neoantigen vaccine in tumor immunotherapy. Cancer Lett. 2023 Jun 1;563:216190. doi: 10.1016/j.canlet.2023.216190
- Mei Y, Wang X. RNA modification in mRNA cancer vaccines. Clin Exp Med. 2023 Oct;23(6):1917–1931. doi: 10.1007/s10238-023-01020-5
- Evaluation of the quality, safety and efficacy of messenger RNA vaccines for the prevention of infectious diseases: regulatory considerations. World Health Organization. [cited 2021 Dec 7]. Available from: https://www.who.int/publications/m/item/evaluation-of-the-quality-safety-and-efficacy-of-messenger-rna-vaccines-for-the-prevention-of-infectious-diseases-regulatory-considerations
- Analytical Procedures for mRNA Vaccine Quality. United States Pharmacopeia. 2022 Feb. Available from: https://www.uspnf.com/sites/default/files/usp_pdf/EN/USPNF/usp-nf-notices/gc-xxx-analytical-procedures-mRNA-vaccines.pdf
- mRNA vaccines for human use. European Pharmacopoeia. Available from: https://pharmeuropa.edqm.eu/app/phpa/content/issue36-2/53600E.htm
- mRNA substances for the production of mRNA vaccines for human use. European Pharmacopoeia. [cited 2024 Apr 4]. Available from: https://pharmeuropa.edqm.eu/app/phpa/content/issue36-2/53900E.htm
- DNA template for the preparation of mRNA substances. European Pharmacopoeia. 2024 Apr 04. Available from: https://pharmeuropa.edqm.eu/app/phpa/content/issue36-2/54000E.htm
- COVID-19 Prophylactic Vaccinology Technical Guidelines (Interim). National Medical Products Administration Center for Drug Evaluation. 2020 Aug. Available from: https://www.nmpa.gov.cn/xxgk/ggtg/qtggtg/20200814230916157.html
- Idänpään-Heikkilä JE. WHO guidelines for good clinical practice (GCP) for trials on pharmaceutical products: responsibilities of the investigator. Ann Med. 1994 Apr;26(2):89–94. doi: 10.3109/07853899409147334
- Good manufacturing practices for pharmaceutical products: supplementary guidelines for the manufacture of investigational pharmaceutical products for studies in humans. World Health Organization. 1994. Available from: https://iris.who.int/handle/10665/62229?&locale-attribute=en
- WHO. Guidelines on transmissible spongiform encephalopathies in relation to biological and pharmaceutical products. World Health Organization. 2003. Available from: https://www.who.int/publications/m/item/who-guidelines-on-transmissible-spongiform-encephalopathies
- Guidelines on Stability Evaluation of Vaccines, Annex 3, TRS No 962. World Health Organization. 2014. Available from: https://www.who.int/publications/m/item/guidelines-on-stability-evaluation-of-vaccines
- Guidelines on procedures and data requirements for changes to approved vaccines, Annex 4, TRS No 993. World Health Organization. 2015. Available from: https://www.who.int/publications/m/item/procedures-and-data-requirements-changes-to-approved-vaccines-annex-4-trs-no-993
- WHO good manufacturing practices for pharmaceutical products: Main principles. World Health Organization. 2014. Available from: https://www.who.int/publications/m/item/trs986-annex2
- Model guidance for the storage and transport of time and temperature sensitive pharmaceutical products. World Health Organization. 2011. Available from: https://www.who.int/publications/m/item/trs961-annex9-modelguidanceforstoragetransport
- Guidelines on the stability evaluation of vaccines for use under extended controlled temperature conditions. World Health Organization. 2016. Available from: https://www.who.int/publications/m/item/ectc-annex-5-trs-no-999
- Overview of end-to-end mRNA drug substance and drug product manufacturing processes and scale-up considerations. 2023 Jun 29. Available from: https://www.biophorum.com/download/overview-of-end-to-end-mrna-drug-substance-and-drug-product-manufacturing-processes-and-scale-up-considerations/
- Food and Drug Administration. Pharmaceutical Current Good Manufacturing Practices (CGMPs) for the 21st Century. Food and Drug Administration. 2004 Sep. Available from: https://www.fda.gov/media/77391/download
- Nag K, Sarker MEH, Kumar S, et al. DoE-derived continuous and robust process for manufacturing of pharmaceutical-grade wide-range LNPs for RNA-vaccine/drug delivery. Sci Rep. 2022 Jun 7;12(1):9394. doi: 10.1038/s41598-022-12100-z
- Daniel S, Kis Z, Kontoravdi C, et al. Quality by Design for enabling RNA platform production processes. Trends Biotechnol. 2022 Oct;40(10):1213–1228. doi: 10.1016/j.tibtech.2022.03.012
- ICH Harmonised Guideline Analytical Procedure Development Q14. ICH; [cited 2022 Mar 24]. Available from: https://database.ich.org/sites/default/files/ICH_Q14_Document_Step2_Guideline_2022_0324.pdf
- ICH Q2: Validation of analytical procedures (R2). ICH; [cited 2022 Mar 24]. Available from: https://database.ich.org/sites/default/files/ICH_Q2-R2_Document_Step2_Guideline_2022_0324.pdf
- Report PQfts CAR-BAP. Food and Pharmaceutical Quality for the 21st Century a Risk-Based Approach Progress Report Drug Administration. Food and Drug Administration Available from: https://www.fda.gov/about-fda/center-drug-evaluation-and-research-cder/pharmaceutical-quality-21st-century-risk-based-approach-progress-report
- Liu J, Bai Y, Liu M, et al. Standardized neutralization antibody analytical procedure for clinical samples based on the AQbD concept. Signal transduction and targeted therapy. Signal Transduct Target Ther. 2023 Apr 28;8(1):165. doi: 10.1038/s41392-023-01389-5
- Gurba-Bryśkiewicz L, Maruszak W, Smuga DA, et al. Quality by Design (QbD) and Design of Experiments (DOE) as a Strategy for Tuning Lipid Nanoparticle Formulations for RNA Delivery. Biomedicines. 2023 Oct 11;11(10):2752. doi: 10.3390/biomedicines11102752
- Mudd PA, Minervina AA, Pogorelyy MV, et al. SARS-CoV-2 mRNA vaccination elicits a robust and persistent T follicular helper cell response in humans. Cell. 2022 Feb 17;185(4):603.e15–613.e15. doi: 10.1016/j.cell.2021.12.026
- Paget M, Cadena C, Ahmad S, et al. Stress granules are shock absorbers that prevent excessive innate immune responses to dsRNA. Molecular Cell. 2023 Apr 6;83(7):1180–1196.e8. doi: 10.1016/j.molcel.2023.03.010
- Martínez J, Lampaya V, Larraga A, et al. Purification of linearized template plasmid DNA decreases double-stranded RNA formation during IVT reaction. Front Mol Biosci. 2023;10:1248511. doi: 10.3389/fmolb.2023.1248511
- Gholamalipour Y, Karunanayake Mudiyanselage A, Martin CT. 3’ end additions by T7 RNA polymerase are RNA self-templated, distributive and diverse in character-RNA-Seq analyses. Nucleic Acids Res. 2018 Oct 12;46(18):9253–9263. doi: 10.1093/nar/gky796
- Muramatsu H, Lam K, Bajusz C, et al. Lyophilization provides long-term stability for a lipid nanoparticle-formulated, nucleoside-modified mRNA vaccine. Mol Ther. 2022 May 4;30(5):1941–1951. doi: 10.1016/j.ymthe.2022.02.001
- Kim SC, Sekhon SS, Shin WR, et al. Modifications of mRNA vaccine structural elements for improving mRNA stability and translation efficiency. Mole Cell Toxicol. 2022;18(1):1–8. doi: 10.1007/s13273-021-00171-4
- Crommelin DJA, Anchordoquy TJ, Volkin DB, et al. Addressing the Cold Reality of mRNA Vaccine Stability. J Pharmaceut sci. 2021 Mar;110(3):997–1001. doi: 10.1016/j.xphs.2020.12.006
- WHO’s Science Council issues report on mRNA vaccine technology. World Health Organization. [cited 2023 Dec 13]. Available from: https://www.who.int/news/item/13-12-2023-who-s-science-council-issues-report-on-mrna-vaccine-technology
- Schoenmaker L, Witzigmann D, Kulkarni JA, et al. mRNA-lipid nanoparticle COVID-19 vaccines: Structure and stability. Int J Pharmaceut. 2021 May 15;601:120586. doi: 10.1016/j.ijpharm.2021.120586
- Gilbert J, Sebastiani F, Arteta MY, et al. Evolution of the structure of lipid nanoparticles for nucleic acid delivery: From in situ studies of formulation to colloidal stability. J Colloid Interface Sci. 2024 Jan 5;660:66–76. doi: 10.1016/j.jcis.2023.12.165
- Henderson MI, Eygeris Y, Jozic A, et al. Leveraging Biological buffers for efficient messenger RNA delivery via lipid nanoparticles. Mol Pharmaceut. [2022 Nov 7];19(11):4275–4285. doi: 10.1021/acs.molpharmaceut.2c00587
- Manning AM, Tilstra G, Khan AB, et al. Ionizable Lipid with supramolecular chemistry features for RNA delivery in vivo. Small (Weinheim an der Bergstrasse. Germany). 2023 Oct;19(41):e2302917. doi: 10.1002/smll.202302917
- Vlatkovic I. Non-immunotherapy application of LNP-mRNA: Maximizing Efficacy and Safety. Biomedicines. [2021 May 10];9(5):530. doi: 10.3390/biomedicines9050530
- Zong Y, Lin Y, Wei T, et al. Lipid Nanoparticle (LNP) enables mRNA delivery for cancer therapy. Adv Mater (Deerfield Beach, Fla). 2023 Dec;35(51):e2303261. doi: 10.1002/adma.202303261
- Kon E, Ad-El N, Hazan-Halevy I, et al. Targeting cancer with mRNA-lipid nanoparticles: key considerations and future prospects. Nat Rev Clin Oncol. 2023 Nov;20(11):739–754. doi: 10.1038/s41571-023-00811-9
- Kon E, Elia U, Peer D. Principles for designing an optimal mRNA lipid nanoparticle vaccine. Curr Opin Biotechnol. 2022 Feb;73:329–336. doi: 10.1016/j.copbio.2021.09.016
- Yang L, Gong L, Wang P, et al. Recent Advances in Lipid Nanoparticles for Delivery of mRNA. Pharmaceutics. 2022 Dec 1;14(12):2682. doi: 10.3390/pharmaceutics14122682
- Chen R, Wang SK, Belk JA, et al. Engineering circular RNA for enhanced protein production. Nature Biotechnol. 2023 Feb;41(2):262–272. doi: 10.1038/s41587-022-01393-0
- Maruggi G, Ulmer JB, Rappuoli R, et al. Self-amplifying mRNA-Based Vaccine Technology and Its Mode of Action. Curr Top Microbiol Immunol. 2022;440:31–70.
- Blakney AK, Ip S, Geall AJ. An Update on Self-Amplifying mRNA Vaccine Development. Vaccines. 2021 Jan 28;9(2):97. doi: 10.3390/vaccines9020097
- Schmidt C, Schnierle BS. Self-amplifying RNA vaccine candidates: Alternative Platforms for mRNA Vaccine Development. Pathogens. 2023 Jan 13;12(1). doi: 10.3390/pathogens12010138
- Ohage E, Iverson R, Krummen L, et al. QbD implementation and post approval lifecycle management (PALM). Biologicals. 2016 Sep;44(5):332–340. doi: 10.1016/j.biologicals.2016.06.007
- Kelley B, Cromwell M, Jerkins J. Integration of QbD risk assessment tools and overall risk management. Biologicals. 2016 Sep;44(5):341–351. doi: 10.1016/j.biologicals.2016.06.001
- Samnuan K, Blakney AK, McKay PF, et al. Design-of-experiments in vitro transcription yield optimization of self-amplifying RNA. 2021:2021.01.08.425833.
- Myatt DP, Wharram L, Graham C, et al. Biophysical characterization of the structure of a SARS-CoV-2 self-amplifying RNA (saRNA) vaccine. Biol Methods Protoc. 2023;8(1):bpad001. doi: 10.1093/biomethods/bpad001
- Belliveau NM, Huft J, Lin PJ, et al. Microfluidic synthesis of highly potent limit-size lipid nanoparticles for in vivo delivery of siRNA. Mol Ther Nucleic Acids. 2012 Aug 14;1(8):e37. doi: 10.1038/mtna.2012.28
- Yanez Arteta M, Kjellman T, Bartesaghi S, et al. Successful reprogramming of cellular protein production through mRNA delivered by functionalized lipid nanoparticles. Proc Natl Acad Sci USA. 2018 Apr 10;115(15):E3351–e3360. doi: 10.1073/pnas.1720542115
- Thelen JL, Leite W, Urban VS, et al. Morphological characterization of self-amplifying mRNA lipid nanoparticles. ACS Nano. 2024 Jan 16;18(2):1464–1476. doi: 10.1021/acsnano.3c08014
- Wesselhoeft RA, Kowalski PS, Anderson DG. Engineering circular RNA for potent and stable translation in eukaryotic cells. Nat Commun. 2018 Jul 6;9(1):2629. doi: 10.1038/s41467-018-05096-6
- Obi P, Chen YG. The design and synthesis of circular RNAs. Methods (San Diego. Calif). 2021 Dec;196:85–103. doi: 10.1016/j.ymeth.2021.02.020
- Müller S, Appel B. In vitro circularization of RNA. RNA Biol. 2017 Aug 3;14(8):1018–1027. doi: 10.1080/15476286.2016.1239009
- Chen X, Lu Y. Circular RNA: Biosynthesis in vitro. Front Bioeng Biotechnol. 2021;9:787881. doi: 10.3389/fbioe.2021.787881
- Mu X, Hur S. Immunogenicity of in vitro-transcribed RNA. Acc Chem Res. 2021 Nov 2;54(21):4012–4023. doi: 10.1021/acs.accounts.1c00521
- Triana-Alonso FJ, Dabrowski M, Wadzack J, et al. Self-coded 3’-extension of run-off transcripts produces aberrant products during in vitro transcription with T7 RNA polymerase. J Biol Chem. 1995 Mar 17;270(11):6298–6307. doi: 10.1074/jbc.270.11.6298
- Xie J, Ye F, Deng X, et al. Circular RNA: A promising new star of vaccine. J Transl Int Med. 2023 Dec;11(4):372–381. doi: 10.2478/jtim-2023-0122
- Wesselhoeft RA, Kowalski PS, Parker-Hale FC, et al. RNA circularization diminishes immunogenicity and can extend translation duration in vivo. Molecular Cell. 2019 May 2;74(3):508–520.e4. doi: 10.1016/j.molcel.2019.02.015
- Wan J, Wang Z, Wang L, et al. Circular RNA vaccines with long-term lymph node-targeting delivery stability after lyophilization induce potent and persistent immune responses. MBio. 2023 Dec 11;15(1):e0177523. doi: 10.1128/mbio.01775-23
- Teo SP. Review of COVID-19 mRNA Vaccines: BNT162b2 and mRNA-1273. J Pharm Pract. 2022 Dec;35(6):947–951. doi: 10.1177/08971900211009650
- Tan T, Deng ST, Wu BH, et al. mRNA vaccine – a new cancer treatment strategy. Curr Cancer Drug Targets. 2023;23(9):669–681. doi: 10.2174/1568009623666230222124424
- Jin Y, Hou C, Li Y, et al. mRNA vaccine: how to meet the challenge of SARS-CoV-2. Front Immunol. 2021;12:821538. doi: 10.3389/fimmu.2021.821538
- Duan LJ, Wang Q, Zhang C, et al. Potentialities and challenges of mRNA vaccine in cancer immunotherapy. Front Immunol. 2022;13:923647. doi: 10.3389/fimmu.2022.923647