ABSTRACT
The relationships between care environment, resilience, and social factors in orphaned and separated adolescents and youths (OSAY) in western Kenya are complex and under-studied.Survey responses from OSAY living in Charitable Children’s Institutes (CCI) and family-based care settings (FBS) in Uasin Gishu County, Kenya were used to examine the associations between 1) care environment and resilience; 2) care environment and factors thought to promote resilience (e.g. social, family, and peer support); and 3) resilience and these same resilience-promoting factors, using multivariable linear and logistic regressions. This cross-sectional study included 1202 OSAY (50.4% female) aged 10–26 (mean = 16; SD = 3.5). The mean resilience score in CCIs was 71 (95%CI = 69–73) vs. 64 (95%CI = 62–66) in FBS. OSAY in CCIs had higher resilience (β = 7.67; 95%CI = 5.26–10.09), social support (β = 0.26; 95%CI = 0.14–0.37), and peer support (β = 0.90; 95%CI = 0.64–1.17) than those in FBS. OSAY in CCIs were more likely to volunteer than those in FBS (OR = 3.72; 95%CI = 1.80–7.68), except in the male subgroup. Family (β = 0.42; 95%CI = 0.24–0.60), social (β = 4.19; 95%CI = 2.53–5.85), and peer (β = 2.13; 95%CI = 1.44–2.83) relationships were positively associated with resilience in all analyses. Volunteering was positively associated with resilience (β = 5.85; 95%CI = 1.51–10.19). The factor most strongly related to resilience in both fully adjusted models was peer support. This study found a strong relationship between care environment and resilience. Care environment and resilience each independently demonstrated strong relationships with peer support, social support, and participating in volunteer activities. Resilience also had a strong relationship with familial support. These data suggest that resilience can be developed through strategic supports to this vulnerable population.
Abbreviations: 95%CI - 95% Confidence intervalAMPATH - Academic Model Providing Access to HealthcareCASSS - Child and Adolescent Social Support ScaleCCI - Charitable Children’s InstitutesCTQ - Childhood Trauma QuestionnaireFBS - Family-based care settingICAST-CH - ISPCAN Child Abuse Screening Tool for Children a HomeMSPSS - Multidimensional Scale of Perceived Social SupportMTRH – Moi Teaching and Referral HospitalMU - Moi UniversityOSAY - Orphaned and separated adolescents and youthsOSCAR - Orphaned and Separated Children’s Assessments Related to Their Health and Well-BeingOR - Odds ratioRS14 - Resilience ScaleSD - Standard deviationSDQ - Strengths and Difficulties QuestionnaireSE - Standard ErrorUG - Uasin Gishu
Introduction
While the exact definition of resilience has been the subject of much debate, it is often considered the ability of a system to adapt to and recover from challenges (Masten, Citation2018; L. Theron et al., Citation2020; Ungar, Citation2019). It is most commonly understood as a capacity for overcoming adversity, emerging from the interaction of complex adaptive systems (Masten, Citation2018). An individual’s resilience develops through interactions with, and the development of, diverse internal and external resources and supports. These include multiple pathways and dynamic systems of individual, relational, family, and community attributes (Masten, Citation2018; L. Theron et al., Citation2020).
Perseverance, purpose, equanimity, authenticity, and self-reliance comprise the resilience core, which together with coping techniques promote individual-level effective crisis navigation and positive adaptation (The Resilience Center, Citation2017). Relational and family-based elements include secure attachments with caregivers/parents, peers, and extended social and community groups (Masten, Citation2018). Activities such as sport, civic, and religious participation may support resilience by increasing engagement with external support systems and strengthening the resilience core (Masten, Citation2018; Mistry et al., Citation2009; Ngwenya et al., Citation2021; L. C. Theron et al., Citation2013). Connections with cultural traditions, spirituality, and nature have been likewise linked to increased resilience (Ingulli & Lindbloom, Citation2013; L. C. Theron et al., Citation2013). The nature and importance of individual systems vary contextually, culturally, and throughout the life-course (Masten, Citation2018; L. C. Theron et al., Citation2013). A study seeking to conceptualize Afri-centric youth resilience identified similar systems-based themes to Euro-centric research; however, it emphasized collectivist philosophies and family/community systems over relationships with a single adult or cohesive primary family bonds (L. C. Theron et al., Citation2013). Understanding the origins of resilience may offer important insight into avenues for mitigating the effects of adverse life events on vulnerable populations including orphaned and separated adolescents and youths (OSAY).
As of 2018, sub-Saharan Africa was home to approximately 50 million OSAY (UNICEF, Citation2019). More than 90% are cared for by extended family; however, a combination of HIV/AIDS, poverty, and urbanization has left many families unable to provide adequate care for OSAY (Embleton et al., Citation2014; L. C. Theron et al., Citation2013). This has led to the emergence of alternate models of care including Charitable Children’s Institutions (CCI) (orphanages and rescue centers) and community-based programs of family-based care settings (FBS; Embleton et al., Citation2014). Negative impacts of institutionalization on child development, strong cultural preferences, and high profile, historic examples of abuse and neglect have led to global recommendations for deinstitutionalization; moving children from CCIs to FBS (Gulaid, Citation2004; Save the Children UK, Citation2003; UNICEF, Citation2004). However, in countries with weak infrastructure, studies have shown greater heterogeneity in wellbeing within care environments than between them and some OSAY in CCIs have demonstrated better outcomes than those in FBS (Atwoli et al., Citation2014; Braitstein et al., Citation2013; Embleton et al., Citation2017; Gayapersad et al., Citation2019; Jelsma et al., Citation2011; Whetten et al., Citation2014, Citation2009; Williamson et al., Citation2017). These include a study that found FBS were often less equipped than CCIs to provide for the physical, mental, spiritual, and social needs of OSAY in Kenya (Embleton et al., Citation2014).
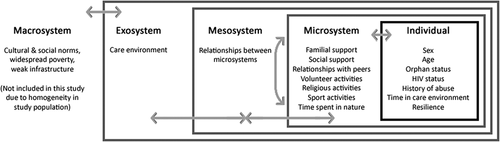
The current study uses Bronfenbrenner’s socio-ecological framework to approach understanding the dynamic and complex relationship between OSAY, their environment, social factors, and resilience (; Bronfenbrenner, Citation1979). This model includes five systems of influence: (1) Macrosystem: cultural and social norms, geography, and civil and legal infrastructure (not included in this study due to the geographic homogeneity of all participants); (2) Exosystem: formal and informal settings, care environment; (3) Mesosystem: relationships between Microsystems; (4) Microsystem: interpersonal relationships and interactions with family, caregivers, peers, community, and activities; and 5) Individual: internal characteristics. In this model, the benefits of care in CCIs over FBS (Exosystem-level) may stem in part from some CCIs attempts to emulate a family-like environment including strong bonds with caregivers, peers, and participation in community-building religious, civic, and sport activities (Microsystem-level); factors which may also impact resilience (Individual-level; Gayapersad et al., Citation2019). Understanding these relationships is important for facilitating safe and effective deinstitutionalization and fostering similar benefits in FBS.
Figure 1. Application of Bronfenbrenner’s socio-ecological framework for care environment, social factors, and resilience in OSAY.
The aim of this study was to estimate the context-specific associations between care environment, resilience, and social factors in the Kenyan OSAY population. Our primary hypothesis was that care in CCIs would be positively associated with resilience, as CCIs in this context may better meet the complex needs of OSAY including fostering stronger community systems, central to Afri-centric concepts of youth resilience. Our secondary hypothesis was that one or more social factors would be associated with both resilience and care in CCIs.
Methods
Study setting
This study occurred in Uasin Gishu (UG) County, Kenya. In 2019, UG County was home to approximately 1,152,671 individuals from 304,943 households; 36.8% aged ≤14 years (Kenya National Bureau of Statistics, Citation2019, Citation2020b). In 2016, approximately 36.9% of UG County residents aged <18 years were living in multidimensional poverty, as defined by UNICEF’s Multiple Overlapping Deprivation Analysis (Kenya National Bureau of Statistics, Citation2020c). In 2019, the capital of UG County, Eldoret, had a population of 475,716 (Kenya National Bureau of Statistics, Citation2020a). The city is home to Moi University (MU), Moi Teaching and Referral Hospital (MTRH), and the Academic Model Providing Access to Healthcare (AMPATH) program, which is a collaboration between MTRH, MU, and a consortium of universities from North America (Einterz et al., Citation2007).
Procedures and participants
This study uses data from the Orphaned and Separated Children’s Assessments Related to Their Health and Well-Being (OSCAR) (R01HD060478) longitudinal cohort study, described in detail previously (Embleton et al., Citation2014; Kamanda et al., Citation2013). Begun in 2010, with near universal inclusion of CCIs and a random representative sample of FBS households, the study used annual surveys including clinical and psychosocial encounters to investigate the effects of care environment on the physical and mental health of OSAY, ≤18 years old at baseline, in Uasin Gishu County. Phase II began in 2016 and aims to explain the results of Phase I with a focus on individual and interpersonal factors, such as psychological resilience, that may promote well-being within and between care environments.
This study uses cross-sectional Phase II data from 1202 of 1231 participants. Exclusions included age (n = 28), as psychological assessments were not administered to OSAY aged <10, and residing in an ineligible environment of self-care at data collection (n = 1). Complete data were obtained from 1016 OSAY (incomplete n = 187); however, individuals with limited missing data, including ‘refuse to answer’, were only excluded from analyses using the affected variables. Data cleaning occurred first in the field and discrepancies or missing information were verified with the participant on site (Kamanda et al., Citation2013).
Human subjects protections
Study protocols for this and the parent OSCAR study were approved by the Research Ethics Board at University of Toronto, the Institutional Research Ethics Committees of Moi University College of Health Sciences and Moi Teaching and Referral Hospital, and Indiana University’s Institutional Review Board. In brief, all participants provided written assent, with fingerprints used when individuals could not sign their names. Informed consent was obtained from the heads of each household in cases of FBS and the Director of each CCI. A project psychologist reviewed all psychological assessments for red flags on suicidality, markers of active abuse, or if the participant posed a likely threat to themselves or others. OSCAR study staff followed up on these cases (Kamanda et al., Citation2013).
Instruments
Resilience was measured using the 14-item Resilience Scale (RS14) with a 7-point response scale as a continuous measure (Wagnild, Citation2009). Social support was measured with the 12-item Multidimensional Scale of Perceived Social Support (MSPSS) using a 5-point response scale as a continuous measure (Zimet et al., Citation1988). Family support was measured with the 10-item Parent subscale of the Child and Adolescent Social Support Scale (CASSS) with a 4-point adaptation of the frequency response as a continuous measure (Kerres Malecki & Kilpatrick Demary, Citation2002). Peer support was measured with the 5-item Peer Problems subscale of the Strengths and Difficulties Questionnaire (SDQ) with a 3-point response as a continuous measure (Escueta et al., Citation2014). A history of abuse was measured using the ISPCAN Child Abuse Screening Tool for Children at Home (ICAST-CH) for OSAY <18 years of age and the Childhood Trauma Questionnaire (CTQ) for OSAY age ≥18 (Bernstein, Citation1998; Zolotor et al., Citation2009). Abuse was treated as binary with any individual scoring ‘moderate’ or ‘severe’ in any of the emotional, sexual, or physical abuse subscales considered positive for abuse. Additional instrument information can be found in Supplementary Table S1.
Variables
Analysis 1: The independent variable was care environment (CCI vs. FBS). Dependent variables were resilience, social support, family support, and peer relationships (continuous), involvement in religious, sport, and volunteer activities (yes/no), and time in nature (<2/≥2 hours/week). Potential confounding variables included age (continuous), sex (female/male), orphaned/separated status (maternal/paternal/double/non-orphan), HIV status (positive/negative), history of abuse (yes/no), and time in care environment at data collection (<6 months/6-24 months/2-5 years/>5 years). Sub-group analysis variables included age (<18/≥18 years), sex, and reason for time in nature (pleasure/work).
Analysis 2: The independent variables included social support, family support, and peer relationships (continuous), involvement in religious, sport, and volunteer activities (yes/no), and time in nature (<2/≥2 hours/week). The dependent variable was resilience (continuous). Potential confounding and sub-group analysis variables remained unchanged from analysis 1.
Data on involvement in sport, volunteer, and religious activities, and time spent in nature were only available for individuals age <18.
Statistical analysis
Following descriptive analyses, bivariable and multivariable (with adjustments listed above) linear and logistic regression models were fitted to independently explore the relationships between care environment, resilience, and each social variable. Interaction terms were fitted to detect subgroup differences. All models were fitted using generalized estimating equations to allow for any clustering effects on standard errors of households or institutes (248 clusters: 15 CCI & 233 FBS). False discovery rate was controlled at 5% to account for multiple comparisons in hypothesis testing. All analyses used two-tailed tests and were conducted using SAS 9.1 (SAS Institute Inc, Citation2002).
Results
The sample comprised 1202 OSAY; 606 females and 596 males. Ages ranged from 10 to 26 years (mean = 16.4; SD = 3.5), with most (65%) under 18 years old. Two-thirds lived in FBS, one-third in CCIs (). Distribution of sex did not vary by age. A higher proportion aged <18 lived in CCIs compared to older participants (37% vs. 26%).
Table 1. Sample description
Resilience scores ranged from 14 to 98 with a mean score of 66 (SD = 19), considered moderately resilient (Wagnild, Citation2009). Social support scores ranged from 1 to 5 with a mean score of 4.3 (SD = 0.8), considered moderate (Zimet, Citation2016). Family support scores ranged from 10 to 40 with a mean score of 27.4 (SD = 7.6). Peer support scores ranged from 6 to 15 with a mean score of 12.4 (SD = 2.0), considered within the normal range (Escueta et al., Citation2014). None of resilience, social, family, or peer support varied significantly by sex. Individuals ≥18 years of age demonstrated higher levels of resilience (mean = 69 vs. 65) than younger OSAY. Older individuals also demonstrated statistically significant, though likely clinically non-significant, increased levels of social support (mean = 4.4 vs. 4.2) and family support (mean = 28 vs. 27) as compared to younger individuals. Peer support did not vary by age ().
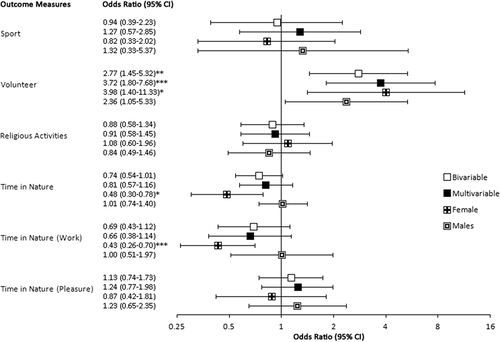
All β-coefficients and odds ratios (OR) were estimated in multivariable analyses of all participants unless specified. Reference categories are defined in ) and 3. OSAY in CCIs had greater resilience (β = 7.67; 95%CI = 5.26–10.09), social support (β = 0.26; 95%CI = 0.14–0.37), and peer support (β = 0.90; 95%CI = 0.64–1.17) than their peers living in FBS in all analyses. OSAY age <18 in CCIs were more likely than those in FBS to volunteer in their communities (OR = 3.72; 95%CI = 1.80–7.68). Females in CCIs were less likely than those in FBS to spend ≥2 hours per week in nature (OR = 0.48; 95%CI = 0.30–0.78; care environment*sex β = −0.76; 95%CI = −1.32-(−0.19)). No relationship was found between care environment and time spent in nature in the full sample (OR = 0.81; 95%CI = 0.57–1.16) or in males (OR = 1.01; 95%CI = 0.74–1.40). No statistically significant relationship was found between care environment and family support (β = 0.06; 95%CI = −0.89–1.01), involvement in sports (OR = 1.27; 95%CI = 0.57–2.85), or religious activities (OR = 0.91; 95%CI = 0.58–1.45) in any analysis ()). Additional information is available in Supplementary TableS 2 and Supplementary Figure S1(a,b).
Figure 2. (a). Associations between care environment (independent variable) and social-psychological factors (dependent variables) estimated through linear regression analyses (b). Associations between care environment (independent variable) and social-psychological factors (dependent variables) estimated through logistic regression analyses.
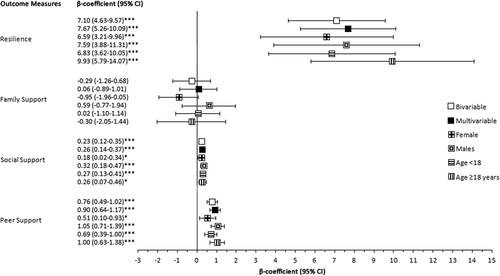
Figure 3. Associations between social-psychological factors (independent variables) and resilience (dependent variable) estimated through linear regression analyses.
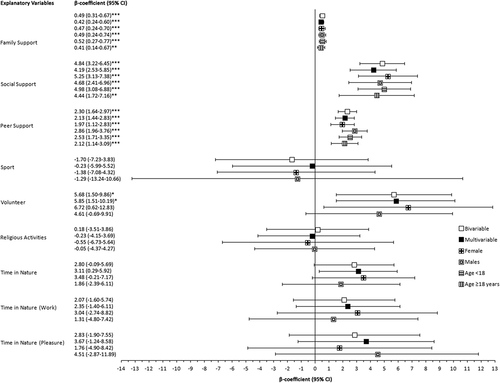
Resilience was positively associated with family support (β = 0.42; 95%CI = 0.24–0.60), social support (β = 4.19; 95%CI = 2.53–5.85), and peer support (β = 2.13; 95%CI = 1.44–2.83) in all unadjusted, adjusted, and sub-analyses. Participating in volunteer activities was positively associated with resilience in individuals <18 years of age (β = 5.85; 95%CI = 1.51–10.19), though the relationship was not statistically significant when divided by sex (female: β = 6.72; 95%CI = 0.62–12.83; male: β = 4.61; −0.69–9.91). No statistically significant relationship existed between resilience and involvement in sports (β = −0.23; 95%CI = −4.15–3.69), religious activities (β = −0.23; 95%CI = −4.15–3.69), or spending time in nature (β = 3.11; 0.29–5.92) (). Additional information is available in Supplementary Table S3 and Supplementary Figure S1(a).
An additional analysis showed that in a model containing all social variables, peer support demonstrated the strongest relationship with resilience in both age groups (data not shown).
Discussion
This study suggests a strong relationship between care environment and resilience and identifies factors that may facilitate this relationship. The mean resilience score was 66, considered moderately-low to moderate. Consistent with most previous studies, resilience did not vary by sex and increased with age (Bonanno et al., Citation2007; Damásio et al., Citation2011; Losoi et al., Citation2013).
Care environment was strongly associated with resilience, with OSAY in CCIs demonstrating significantly higher resilience than FBS. OSAY in CCIs also had higher levels of several social factors which themselves had strong relationships with resilience. This is consistent with the socio-ecological framework in which resilient individuals are able to draw upon resources from multiple levels in order to support healthy functioning when confronted with stressors (Bronfenbrenner, Citation1979; L. Theron et al., Citation2020). In this model, CCIs may encourage positive social factors, such as peer support, social support, and volunteering, and both care environment and social factors may have a role in building resilience. This is supported by a 2019 study of OSAY in Kenya that found that some CCIs purposefully model the care environment after a village or single family and that engaging in family-related activities within institutionalized care environments can lead to the development of novel, non-consanguineous family identities in which OSAY feel supported and cared for – factors central to resilience (Gayapersad et al., Citation2019).
In this study, family, peer, and social support were all positively related to resilience. Social and peer support have previously been found to foster recovery from trauma (Bonanno et al., Citation2007). A British study found social support from peers, mentors, and family to be instrumental to one’s resilience and ability to withstand and thrive in high pressure situations (Sarkar & Fletcher, Citation2014). Another study found that individuals with medium social support were 30% less likely to be resilient than those with high levels (Bonanno et al., Citation2007). Through thematic analysis of interviews with rural adolescents, a South African study also found familial, peer, and social relationships to be closely related to hope; a central component of resilience (Ngwenya et al., Citation2021). As OSAY in CCIs had higher levels of social and peer support than those in FBS, the positive relationship between CCIs and resilience may be partly because CCIs facilitate positive social and peer relationships. This may suggest targets to promote resilience in FBS.
Volunteering was also strongly related to resilience, consistent with studies from the United States and China that demonstrated a positive relationship between volunteering or involvement in extracurricular activities and building resilience in vulnerable populations (Klinedinst & Resnick, Citation2014; Zhao et al., Citation2014). However, we did not find a significant relationship of resilience with several other variables identified in previous studies including feelings of connectedness with nature, time spent in nature, and religiosity (Ingulli & Lindbloom, Citation2013; Mizuno et al., Citation2018; Puffer et al., Citation2012). We also were not able to replicate the relationship with sports, perhaps because the high level of participation, 96%, resulted in low statistical power (Zhao et al., Citation2014).
The study has several strengths. The large sample size provides good statistical power to detect most true relationships of interest. The sampling frame, with a representative sample of FBS households and near universal inclusion of CCIs, minimizes the potential for selection bias. OSAY studies have traditionally focused on CCIs without an FBS comparison group, which we included. This study provides unprecedentedly detailed information on care environment, day to day activities, and psychological variables.
The inability of cross-sectional analyses to determine causality is our primary limitation. While associations can be demonstrated, the direction of the causal relationship cannot be determined and reverse-causation may occur. Central relationships were examined separately in OSAY age 10–17 and ≥18. Within sub-group heterogeneity was not examined due to sample size limitations. Future longitudinal analyses will help produce further evidence on causality and explore age-related heterogeneity.
Tools measuring psychological traits innately introduce error and difference between actual measurements and theoretical constructs. To minimize associated risks, English-language tools validated in the OSCAR or similar samples were used with minor modifications (Supplementary Table S1) (Hoosen et al., Citation2018; Sutherland et al., Citation2020). The same tools were used in FBS and CCI settings, minimizing potential measurement variance.
Missing data may be non-random, for example, due to non-response to sensitive questions or loss to follow-up at Phase II, affecting internal and external validity. To minimize bias due to missing data and improve sensitive information accuracy, questionnaires were self-administered and confidentiality was assured. Completeness was checked on site with immediate follow-up on incomplete questions. Levels of missing data were low. All variables with >5% missingness were investigated; no factors predictive of missingness were found.
This study is the first to examine the relationships between care environment, social factors, and resilience in the Kenyan OSAY population. It demonstrates strong positive relationships between CCIs and psychological resilience and identifies family support, social support, peer relationships, and volunteer activities as factors that may facilitate the development of resilience through adolescence and early adulthood and serve as potential targets, individually or through strategic social and community-building activities, for initiatives seeking to improve resilience in this vulnerable population. By better understanding this complex issue, policy makers may support evidence based, cost-effective programming that encourages the health, wellbeing, and the social and economic potential of OSAY in any care environment, while reproducing the contextual strengths of institutionalized care within the preferred FBS, facilitating safe and effective deinstitutionalization.
Supplemental Material
Download MS Word (155.8 KB)Acknowledgments
We wish to gratefully acknowledge the Chiefs, Assistant Chiefs, and Village Elders of the Locations of Pioneer, Kapsoya, Koisagat, Ol’Lenguse, Olare, Tarakwa, Kipsinende and Kapyemit for their support and leadership. We also wish to acknowledge all the residents of these Locations and in particular the many households caring for vulnerable members of their community, notably orphaned and separated children, children with physical and mental disabilities, and the elderly. We particularly want to acknowledge the County and District Children’s Officers for their dedication to protecting the children of Uasin Gishu County, as well as the Uasin Gishu Children’s Services Forum. This study would not have been possible without the willing participation of the children and youth participants and their guardians and we would like to acknowledge and thank them. The enthusiasm and commitment of the staff and volunteers of the OSCAR study have not gone unnoticed and we the authors wish to thank them for their efforts and engagement with this project.
Disclosure statement
No potential conflict of interest was reported by the author(s).
Supplementary material
Supplemental data for this article can be accessed here
Additional information
Funding
Notes on contributors
Sarah C. Sutherland
Sarah C. Sutherland is a PhD candidate in Epidemiology at the Dalla Lana School of Public Health, University of Toronto. She received her MSc Epidemiology and Honours BHSc Health Sciences from the University of Ottawa.
Harry S. Shannon
Dr. Harry S. Shannon is a professor emeritus at McMaster University in Hamilton, Ontario. Shannon also holds a status appointment in the Dalla Lana School of Public Health at the University of Toronto. Dr. Shannon was previously chair of the Methodology Working Group for the Canadian Longitudinal Study on Aging. Shannon’s research interests have included workplace health and safety, especially the role of organizational factors and interventions to create safe workplaces.
David Ayuku
Dr. David Ayuku is a professor of Clinical Psychology, Moi University School of Medicine in the Department of Mental Health & Behavioural Sciences. He received his PhD in Clinical Psychology from University Maastricht, and MA Clinical Psychology from Texas Southern University, Houston Texas. He is the site Principal Investigator of a ten-year observational cohort study funded by the National Institutes of Health funded examining the effect of care environment and care characteristics on orphaned children, called the ‘Orphaned and Separated Children’s Assessments Related to their (OSCAR’s) Health and Well-Being Study’.
David L. Streiner
Dr. David L. Streiner is an emeritus professor in the Department of Psychiatry and Behavioural Neurosciences at McMaster University and a professor in the Department of Psychiatry at the University of Toronto. He is a clinical psychologist by training, and was the founding director of the Applied Research Unit at the Baycrest Centre, and the Assistant V.P. of Research there. His main areas of interest are quality of life in those with medical disorders; evaluation of therapies for psychiatric disorders; and interventions for the homeless mentally ill. He has co-authored or edited nine books in the areas of statistics, epidemiology, public health, and scale development.
Olli Saarela
Dr. Olli Saarela is an Associate Professor at the Dalla Lana School of Public Health, University of Toronto. He received his PhD from the University of Helsinki, Finland. He is a biostatistician with methodological research interests in the fields of causal inference, Bayesian inference and analysis of survival and event history data. He also has more than 15 years of experience in collaborative statistical work in health research.
Lukoye Atwoli
Dr. Lukoye Atwoli is a Professor of Psychiatry and the Dean of the Medical College, East Africa at the Aga Khan University. He is also the Associate Director of the Aga Khan University Brain and Mind Institute. Prof Atwoli formerly held the position of Dean at Moi University’s School of Medicine (2014-2019). He holds the MBChB degree from Moi University, a Master of Medicine degree in Psychiatry from the University of Nairobi, and a PhD in Psychiatry and Mental Health from the University of Cape Town. His research currently focuses on Trauma (including childhood trauma) and Posttraumatic Stress Disorder (among other outcomes of trauma exposure), but he continues to nurture an interest in general hospital psychiatry, substance use, and HIV and mental health. He is a member of the World Health Organisation’s World Mental Health Surveys Consortium and has published widely on psychiatric epidemiology.
Paula Braitstein
Dr. Paula Braitstein is Associate Professor of epidemiology in the Dalla Lana School of Public Health. Paula is the holder of a prestigious research Chair of Applied Public Health from the Canadian Institutes of Health Research. Her research foci are concentrated on the HIV prevention-care continuum, specifically HIV implementation research in sub-Saharan Africa, and vulnerable and marginalized children and adolescents, including orphans, street-involved children and youth. She is the Principal Investigator of the cohort study upon which this analysis is based.
References
- Atwoli, L., Ayuku, D., Hogan, J., Koech, J., Vreeman, R., Ayaya, S., Braitstein, P., & Elhai, J. D. (2014). Impact of domestic care environment on trauma and posttraumatic stress disorder among orphans in Western Kenya. PloS One, 9(3), e89937. https://doi.org/https://doi.org/10.1371/journal.pone.0089937
- Bernstein, D. P. (1998). Childhood trauma questionnaire: A retrospective self-report : Manual. Psychological Corporation.
- Bonanno, G. A., Galea, S., Bucciarelli, A., & Vlahov, D. (2007). What predicts psychological resilience after disaster? The role of demographics, resources, and life stress. Journal of Consulting and Clinical Psychology, 75(5), 671–682. https://doi.org/https://doi.org/10.1037/0022-006X.75.5.671
- Braitstein, P., Ayaya, S., Nyandiko, W., Kamanda, A., Koech, J., Gisore, P., Atwoli, L., Vreeman, R., Duefield, C., Ayuku, D., & Chaturvedi, S. (2013). Nutritional status of Orphaned and separated children and adolescents living in community and institutional environments in Uasin Gishu County, Kenya. PloS One, 8(7), e70054. https://doi.org/https://doi.org/10.1371/journal.pone.0070054
- Bronfenbrenner, U. (1979). The ecology of human development: Experiments by nature and design. Harvard University Press.
- Damásio, B., Borsa, J., & Silva, J. (2011). 14-item Resilience Scale (RS-14): Psychometric properties of the Brazilian version. Journal of Nursing Measurement, 19(3), 131–145. https://doi.org/https://doi.org/10.1891/1061-3749.19.3.131
- Einterz, R., Kimaiyo, S., Mengech, H., Khwa-Otsyula, B., Esamai, F., Quigley, F., & Mamlin, J. (2007). Responding to the HIV pandemic: The power of an academic medical partnership. Academic Medicine : Journal of the Association of American Medical Colleges, 82(8), 812–818. https://doi.org/https://doi.org/10.1097/ACM.0b013e3180cc29f1
- Embleton, L., Ayuku, D., Kamanda, A., Atwoli, L., Ayaya, S., Vreeman, R., Nyandiko, W., Gisore, P., Koech, J., & Braitstein, P. (2014). Models of care for orphaned and separated children and upholding children’s rights: Cross-sectional evidence from Western Kenya. BMC International Health and Human Rights, 14(9), 1–18. https://doi.org/https://doi.org/10.1186/1472-698X-14-9
- Embleton, L., Nyandat, J., Ayuku, D., Sang, E., Kamanda, A., Ayaya, S., Nyandiko, W., Gisore, P., Vreeman, R., Atwoli, L., Galarraga, O., Ott, M. A., & Braitstein, P. (2017). Sexual behavior among Orphaned adolescents in Western Kenya: A comparison of institutional- and family-based care settings. Journal of Adolescent Health, 60(4), 417–424. https://doi.org/https://doi.org/10.1016/j.jadohealth.2016.11.015
- Escueta, M., Whetten, K., Ostermann, J., & O’Donnell, K., & The Positive Outcomes for Orphans (POFO) Research Team. (2014). Adverse childhood experiences, psychosocial well-being and cognitive development among orphans and abandoned children in five low income countries. BMC International Health and Human Rights, 14(6), 1–13 doi:https://doi.org/https://doi.org/10.1186/1472-698X-14-6.
- Gayapersad, A., Ombok, C., Kamanda, A., Tarus, C., Ayuku, D., & Braitstein, P. (2019). The production and reproduction of kinship in charitable children’s institutions in Uasin Gishu County, Kenya. Child & Youth Care Forum, 48(6), 797–828. https://doi.org/https://doi.org/10.1007/s10566-019-09506-8
- Gulaid, L. (2004). The framework for the protection, care and support of orphans and vulnerable children living in a world with HIV and AIDS. UNICEF. https://gsdrc.org/document-library/the-framework-for-the-protection-care-and-support-of-orphans-and-vulnerable-children-living-in-a-world-with-hiv-and-aids
- Hoosen, N., Davids, E. L., de Vries, P. J., & Shung-King, M. (2018). The Strengths and Difficulties Questionnaire (SDQ) in Africa: A scoping review of its application and validation. Child and Adolescent Psychiatry and Mental Health, 12(1), 6. https://doi.org/https://doi.org/10.1186/s13034-017-0212-1
- Ingulli, K., & Lindbloom, G. (2013). Connection to nature and psychological resilience. Ecopsychology, 5(1), 52–55. https://doi.org/https://doi.org/10.1089/eco.2012.0042
- Jelsma, J., Davids, N., & Ferguson, G. (2011). The motor development of orphaned children with and without HIV: Pilot exploration of foster care and residential placement. BMC Pediatrics, 11(1), 11. https://doi.org/https://doi.org/10.1186/1471-2431-11-11
- Kamanda, A., Embleton, L., Ayuku, D., Atwoli, L., Gisore, P., Ayaya, S., Vreeman, R., & Braitstein, P. (2013). Harnessing the power of the grassroots to conduct public health research in sub-Saharan Africa: A case study from Western Kenya in the adaptation of community-based participatory research (CBPR) approaches. BMC Public Health, 13(1), 91. https://doi.org/https://doi.org/10.1186/1471-2458-13-91
- Kenya National Bureau of Statistics. (2019). 2019 Kenya population and housing census Volume I: Population by county and sub-county (p. 49). https://www.knbs.or.ke/?wpdmpro=2019-kenya-population-and-housing-census-volume-i-population-by-county-and-sub-county
- Kenya National Bureau of Statistics. (2020a). 2019 Kenya population and housing census Volume II: Distribution of POPULATION BY ADMINISTRATIVE UNITS (p. 270). https://www.knbs.or.ke/?wpdmpro=2019-kenya-population-and-housing-census-volume-ii-distribution-of-population-by-administrative-units
- Kenya National Bureau of Statistics. (2020b). 2019 Kenya population and housing census Volume III: Distribution of population by age, sex and administrative units (p. 526). https://www.knbs.or.ke/?wpdmpro=2019-kenya-population-and-housing-census-volume-iii-distribution-of-population-by-age-sex-and-administrative-units
- Kenya National Bureau of Statistics. (2020c). Comprehensive poverty report (p. 151). https://www.genderinkenya.org/publication/comprehensive-poverty-report
- Kerres Malecki, C., & Kilpatrick Demary, M. (2002). Measuring perceived social support: Development of the child and adolescent social support scale (CASSS). Psychology in the Schools, 39(1), 1–18. https://doi.org/https://doi.org/10.1002/pits.10004
- Klinedinst, N. J., & Resnick, B. (2014). Resilience and volunteering: A critical step to maintaining function among older adults with depressive symptoms and mild cognitive impairment. Topics in Geriatric Rehabilitation, 30(3), 181–187. https://doi.org/https://doi.org/10.1097/TGR.0000000000000023
- Losoi, H., Turunen, S., Wäljas, M., Helminen, M., Öhman, J., Julkunen, J., & Rosti-Otajärvi, E. (2013). Psychometric properties of the finnish version of the Resilience Scale and its short version. Psychology, Community & Health, 2(1), 1–10. https://doi.org/https://doi.org/10.5964/pch.v2i1.40
- Masten, A. S. (2018). Resilience theory and research on children and families: Past, present, and promise. Journal of Family Theory & Review, 10(1), 12–31. https://doi.org/https://doi.org/10.1111/jftr.12255
- Mistry, R., McCarthy, W. J., Yancey, A. K., Lu, Y., & Patel, M. (2009). Resilience and patterns of health risk behaviors in California adolescents. Preventive Medicine, 48(3), 291–297. https://doi.org/https://doi.org/10.1016/j.ypmed.2008.12.013
- Mizuno, Y., Hofer, A., Frajo‐Apor, B., Wartelsteiner, F., Kemmler, G., Pardeller, S., Suzuki, T., Mimura, M., Fleischhacker, W. W., & Uchida, H. (2018). Religiosity and psychological resilience in patients with schizophrenia and bipolar disorder: An international cross-sectional study. Acta Psychiatrica Scandinavica, 137(4), 316–327. https://doi.org/https://doi.org/10.1111/acps.12838
- Ngwenya, N., Barnett, T., Groenewald, C., & Seeley, J. (2021). Complex trauma and its relation to hope and hopelessness among young people in KwaZulu-Natal, South Africa. Vulnerable Children and Youth Studies, 16(2), 166–177. https://doi.org/https://doi.org/10.1080/17450128.2020.1865593
- Puffer, E. S., Watt, M. H., Sikkema, K. J., Ogwang‐Odhiambo, R. A., & Broverman, S. A. (2012). The protective role of religious coping in adolescents’ responses to poverty and sexual decision‐making in rural Kenya. Journal of Research on Adolescence, 22(1), 1–7. https://doi.org/https://doi.org/10.1111/j.1532-7795.2011.00760.x
- The Resilience Center. (2017). RS14. https://www.resiliencecenter.com/rs14
- Sarkar, M., & Fletcher, D. (2014). Ordinary magic, extraordinary performance: Psychological resilience and thriving in high achievers. Sport, Exercise, and Performance Psychology, 3(1), 46–60. https://doi.org/https://doi.org/10.1037/spy0000003
- SAS Institute Inc. (2002). Sas 9.1.3 help and documentation. SAS Institute Inc.
- Save the Children UK. (2003). A last resort: The growing concern about children in residential care. International Save the Children Alliance. https://resourcecentre.savethechildren.net/node/2644/pdf/2644.pdf
- Sutherland, S. C., Shannon, H. S., Ayuku, D., Streiner, D. L., Saarela, O., Atwoli, L., Braitstein, P., & Mazulyte-Rasytine, E. (2020). Reliability and validity of the RS14 in orphaned and separated adolescents and youths in Western Kenya. PLOS ONE, 15(11), e0241699. https://doi.org/https://doi.org/10.1371/journal.pone.0241699
- Theron, L., Ruth Mampane, M., Ebersöhn, L., & Hart, A. (2020). Youth resilience to drought: Learning from a group of South African adolescents. International Journal of Environmental Research and Public Health, 17(21), 7896. https://doi.org/https://doi.org/10.3390/ijerph17217896
- Theron, L. C., Theron, A. M. C., & Malindi, M. J. (2013). Toward an African definition of resilience: A Rural South African community’s view of resilient basotho youth. Journal of Black Psychology, 39(1), 63–87. https://doi.org/https://doi.org/10.1177/0095798412454675
- Ungar, M. (2019). Designing resilience research: Using multiple methods to investigate risk exposure, promotive and protective processes, and contextually relevant outcomes for children and youth. Child Abuse & Neglect, 96(Complete), 104098. https://doi.org/https://doi.org/10.1016/j.chiabu.2019.104098
- UNICEF. (2004). Children in residential care: The Zimbabwean experience. https://bettercarenetwork.org/library/the-continuum-of-care/residential-care/children-in-residential-care-the-zimbabwean-experience
- UNICEF. (2019). UNICEF data warehouse. Retrieved February 21, 2021, from. https://data.unicef.org/dv_index
- Wagnild, G. (2009). The Resilience Scale user’s guide for the US English version of the Resilience Scale and the 14-item Resilience Scale (RS–14). Resilience Center.
- Whetten, K., Ostermann, J., Pence, B. W., Whetten, R. A., Messer, L. C., Ariely, S., O’Donnell, K., Wasonga, A. I., Vann, V., Itemba, D., Eticha, M., Madan, I., Thielman, N. M., & Newell, M.-L., & The Positive Outcomes for Orphans (POFO) Research Team. (2014). Three-Year change in the wellbeing of orphaned and separated children in institutional and family-based care settings in five low- and middle-income countries. PLoS ONE, 9(8), e104872. https://doi.org/https://doi.org/10.1371/journal.pone.0104872
- Whetten, K., Ostermann, J., Whetten, R. A., Pence, B. W., O’Donnell, K., Messer, L. C., Thielman, N. M., & Ho, J., & The Positive Outcomes for Orphans (POFO) Research Team. (2009). A comparison of the wellbeing of orphans and abandoned children ages 6–12 in institutional and community-based care settings in 5 less wealthy nations. PLoS ONE, 4(12), e8169. https://doi.org/https://doi.org/10.1371/journal.pone.0008169
- Williamson, K., Landis, D., Shannon, H., Gupta, P., & Gillespie, L.-A. (2017). The impact of protection interventions on unaccompanied and separated children in humanitarian crises. Oxfam; Feinstein International Center; UKAID. https://doi.org/https://doi.org/10.21201/2017.8883
- Zhao, J., Chi, P., Li, X., Tam, C. C., & Zhao, G. (2014). Extracurricular interest as a resilience building block for children affected by parental HIV/AIDS. AIDS Care, 26(6), 758–762. https://doi.org/https://doi.org/10.1080/09540121.2013.845290
- Zimet, G. (2016). Multidimensional Scale of Perceived Social Support (MSPSS) - Scale Items and Scoring Information. Retrieved Febrary 21, 2021, from https://www.researchgate.net/publication/311534896_Multidimensional_Scale_of_Perceived_Social_Support_MSPSS_ -_Scale_Items_and_Scoring_Information
- Zimet, G., Dahlem, N., Zimet, S., & Farley, G. (1988). The multidimensional scale of perceived social support. Journal of Personality Assessment - J PERSONAL ASSESS, 52(1), 30–41. https://doi.org/https://doi.org/10.1207/s15327752jpa5201_2
- Zolotor, A. J., Runyan, D. K., Dunne, M. P., Jain, D., Péturs, H. R., Ramirez, C., Volkova, E., Deb, S., Lidchi, V., Muhammad, T., & Isaeva, O. (2009). ISPCAN Child Abuse Screening Tool Children’s Version (ICAST-C): Instrument development and multi-national pilot testing. Child Abuse & Neglect, 33(11), 833–841. https://doi.org/https://doi.org/10.1016/j.chiabu.2009.09.004