ABSTRACT
Background
1
1. please could you change corrresponding author email from [email protected] to [email protected]
People with mild intellectual disability (ID) experience a higher prevalence of mental health (MH) problems in comparison to the general population, yet there is little consensus on the most appropriate type and nature of services for support and treatment for this specific group of individuals.Objective
The objective of this scoping review is to explore the current evidence for the organization, structure, and delivery of mental health services for people with mild ID.
Methods
The PRISMA-SCr (Preferred Reporting Items for Systematic reviews and Meta-Analyses extension for Scoping Reviews) checklist was followed. Online databases were used to identify systematic reviews, meta-analyses, scoping reviews, or guidelines published between 2003 and 2020. Articles were reviewed using Roever & Zoccai criteria for critical appraisal of systematic reviews and meta-analyses.
Results
130 records were identified, of which 91 were longlisted. Of these, 28 articles were shortlisted after review of abstracts prior to review of full-text papers. The review included 11 studies: one meta-analysis, eight systematic reviews, and two scoping reviews. These studies approached the provision of mental health services for individuals with mild ID from various angles – including service organization and access, therapies, and patient feedback.
Conclusions
According to the Roever & Zoccai criteria, there was a lack of high-quality evidence, which limited the findings and conclusions. The available evidence suggested that despite higher levels of psychopathology there is not a corresponding consideration in care for individuals with mild ID in general psychiatric services. There was no conclusive evidence on better level of services or outcomes being provided either by the general psychiatric services or specialist ID psychiatric services. Some evidence was found for intensive case management and assertive outreach for individuals with mild ID, but this was not replicated in further studies.
In terms of treatment, there was no high-quality evidence found for pharmacological interventions, with some limited evidence around psychological therapy for the treatment of depression in this vulnerable population. Overall, it was found that an increase in staff training would be beneficial in terms of timely access to services and appropriate treatment.
There is a need for inclusive, evidence-based guidance as regards service development for people with mild ID and MH problems.
Abbreviations: ID: intellectual disability; MH: mental health; CBT: Cognitive Behavioral Therapy; RCT: randomized controlled trial; ACT: assertive community treatment; ECT: electroconvulsive therapy
BACKGROUND
Adults with intellectual disability (ID) have a higher rate of mental illness in comparison to the general population (Bhaumik et al., Citation2008; Sheehan et al., Citation2015). A systematic review has established a wide-ranging prevalence of 14–75% for clinically distinguishable mental illness in people with ID (Buckles, Citation2013). It is quite likely that the true prevalence is much greater than that of 20% of individuals in the general population (Singleton et al., Citation2001) and that figures will underestimate the scope of psychiatric illness in the ID population, due to under-diagnosis caused by, for example, diagnostic overshadowing (Sheehan & Paschos, Citation2013).
The International Classification of Diseases version 11 (ICD 11) informs that a mild disorder of intellectual development is to be considered when the condition has originated in the developmental period and characterized by significantly below average social adaptive behavioral and intellectual functioning (two to three times standard deviation below the mean 0.1–2.3%). Individuals with mild ID constitute the majority of the ID population (Harris, Citation2006). The relative burden of psychiatric morbidity in this group highlights the need that psychiatric services are accessible, appropriate, and equitable (Sheehan & Paschos, Citation2013). It is therefore important that both the management of specific psychiatric conditions and delivery of effective health-care systems are based upon sound evidence. The House of Commons (UK) learning disability overview of policy and services (Parkin, Citation2016) makes it clear that the UK Government’s mandate is to narrow the gap in health inequalities for people with ID. Further to this, the Welsh Government’s “Improving Lives Programme” for people with ID (Irranca-Davies et al., Citation2018) emphasizes the need for a whole government approach and integration of services to help improve life chances, services and allow for more effective use of funding. The report highlights the importance of reasonable adjustments in all mainstream services for people with ID to reduce health inequalities, and access to specialist services when needed. This is also acknowledged in NICE guidelines relating to management of common mental health problems in people with mild ID (NICE, 2011).
The model of MH service provision for ID has developed and transformed over time, with the closure of large institutions of the 19th and 20th centuries. Between 1971 and 2000 the number of individuals with ID living in hospitals dropped by over 90% – with the majority being rehoused in small staffed residences within the community (Cumella, Citation2007). A significant proportion of these individuals would have required specialist support. The relatively rapid relocation to the community would have been challenging for community mental health services that had little previous experience of ID (Sheehan & Paschos, Citation2013). There continue to be people placed or living inappropriately in hospitals or institutions in the UK and the ongoing closure and reduction of these facilities is at the forefront of the UK government’s ongoing work (Parkin, Citation2016) following the Winterbourne report (Bubb, Citation2014). This seismic shift from inpatient to community care emphasizes the need for a joined-up approach with general mental health services to provide appropriate support for these individuals.
The process of de-institutionalization has resulted in different service structures for individuals with ID internationally. For example, in the UK, the Community Learning Disability Teams (CLDT) were developed in order to meet both the physical and MH needs of an individual (Hamlin & Oakes, Citation2008). The concern with this model of care has been the by-passing of mainstream services and therefore potentially less equitable access to the required specialist service (Hassiotis et al., Citation2000) – in particular for those people with mild ID with less support needs. In the UK, there exist specific training competencies in the Psychiatry of Intellectual Disability specialty training scheme (RCPsych, Citation2017). However, the political and clinical thinking is that people with ID, where possible, should be supported and enabled to access mainstream services to ensure inclusion. While those with moderate to profound ID by the nature of their needs gravitate to specialist services, there is a lack of clarity in political and clinical establishments as to how best care needs should be organized for those with borderline and mild ID.
By comparison, in the United States, there has been a reliance on the more “mainstream” health-care systems – however, with resultant concerns regarding “insufficient capacity to meet the specialist needs of the ID population” (Balogh et al., Citation2016). The Australian model of care has been historically similar to that of the United States. It has been recognized that people with ID need specialist support if they are to access generic services (New South Wales Ministry of Health, Citation2012). The differing approaches to MH care for ID internationally will all have strengths and weaknesses, and the national context from which evidence has arisen should be taken into consideration when comparing outcomes.
Objectives
Individuals with mild ID make up the majority of the ID population (Harris, Citation2006) and there is increased psychiatric morbidity in this population (Borthwick‐Duffy, Citation1994; Holden & Gitlesen, Citation2004). However, there is little consensus on how mental health services should be organized and delivered for this subgroup, with evidence of international variation. The objective of this scoping review is to explore the breadth of evidence for the structure and delivery of mental health services for people with mild ID, taking into consideration patient experience (Bombard et al., Citation2018). The specific research questions (RQs) are:
RQ1) What models of service for mental health care exist for people with mild ID?
RQ2) What is the scope of the evidence for specific models of care and treatment?
RQ3) What is the experience of patients with mild ID accessing mental health care?
METHODS
Agency
The scoping review was required by the Royal College of Psychiatrists (RCPsych) as a rapid-scan of the evidence in order to inform RCPsych College Report 226: Mental Health services for adults with mild intellectual disabilities (Shankar et al., Citation2020).
Protocol
The review protocol was drafted using the Preferred Reporting Items for Systematic reviews and Meta-Analyses extension for Scoping Reviews (PRISMA-SCr) (Tricco et al., Citation2018). Study protocol available on request.
Inclusion Criteria
The inclusion criteria were developed using the PCC (Population, Concepts, and Context framework (Peters, Citation2020).
Population
People with mild ID (adults over 16 years)
Concept
The current provision of mental health services for individuals with a mild ID, including models of care and treatment. The experience of people with mild ID accessing mental health services.
Context
Mental Health Services
Focus on the current provision of general MH services therefore excluded studies from the forensic setting.
Types of Evidence Source
Systematic review, meta-analysis, service review, or guideline regarding MH service, provision, or access. Publication date within the past 15 years in English.
The rationale for excluding primary research was the requirement for a rapid-scan of existing evidence and literature for the purpose of informing about existing evidence for the RCPsych CR 226 (Shankar et al., Citation2020).
Information Sources
A computerized search using the following databases was undertaken: Cochrane Library, Medline, Medline Inprocess, Embase, PsychINFO, Trip and NICE Evidence. This was for English language, peer reviewed journals published between 10th January 2003 and 10th January 2018. An updated literature search was undertaken covering the period 15th January 2017–15th January 2020.
The initial search was undertaken in 2018 and an updated search undertaken in 2020 to ensure the article included all the relevant and most up to date articles. There was intentional overlap of the second search to ensure no articles were missed.
Hand search of the bibliography of editorial reviews, and relevant journals was also undertaken.
Search
An example of the search strategy is available (see Appendix A)
Selection of Sources of Evidence
When the search terms (see Appendix A) were combined on the individual databases the resulting titles were screened by two of authors (CW, GM). To ensure consistency amongst reviewers, the titles and abstracts were independently reviewed, then discussed and consensus reached by both authors for inclusion. Full-text articles were then reviewed and selected with a discussion with the third author (RS) for any articles where consensus could not be reached. For the updated search the same approach was undertaken involving three of the authors (CW, GM, and DM) with consensus support from RS.
Data Charting Process
Data charting was undertaken by two authors (DM and CW). An agreed process for data extraction was agreed prior to initiation by all authors and tabulated. Disagreements were resolved through discussion between the two reviewers, and, when necessary, adjudication from RS.
Data Items
Data were extracted on article characteristics (title and type of review, date of publication), the objectives of the review, and the main findings specific to mild ID (Appendix B).
Critical Appraisal of Individual Sources of Evidence
The quality of all sources of evidence was assessed utilizing the Roever & Zoccai criteria for Critical Appraisal of Systematic Review and Meta-analyses (Roever & Zoccai, Citation2015).
Synthesis of Results
The studies were grouped together according to the main objectives and research questions. For example, RQ1: Models of service for MH care: general service appraisal. The grouped studies were then tabulated and main findings presented with an appraisal of the quality of the evidence in the final column.
RESULTS
Selection of Sources of Evidence
outlines the search results.
Figure 1. Results of search strategy as per PRISMA guidance for the current provision of mental health services for individuals with a mild ID as per (Moher et al., 2009).
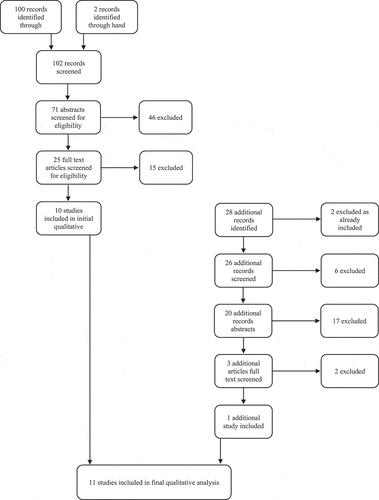
One hundred records were initially identified by database searches, and a further two by hand searching. From the 102 studies screened a total of 71 abstracts were reviewed by the authors and selected as described. Twenty-five articles were selected at this stage. Upon reviewing the full text of these studies, a further 15 were excluded because the articles were opinion, commentary or editorial pieces, primary research or not directly relevant to the research questions.
An updated search was undertaken covering 2017–2020 using the same search criteria. The time frame was intentionally overlapped with the initial search to ensure no relevant articles were missed. To ensure consistency, all new articles found in the updated search were reviewed by all authors. One further study was identified for inclusion (Robertson et al., Citation2019).
Review Characteristics
show a summary assessment of each review. Each table focusses on a different aspect of the research questions. Individual studies’ design, aim and the main findings for mild ID are tabulated.
Table 1. General service appraisal
Table 2. Inpatient care
Table 3. Community care
Table 4. Interventions for adults with mild intellectual disabilities and mental ill health
Table 5. Patient feedback
Critical Appraisal within Sources of Evidence
All of the included studies were assessed for methodological quality (Roever & Zoccai, Citation2015) which is shown in the final column of the four tables. Although the majority of reviews were found to be of medium or high quality, it is important to note the common theme, that the evidence included within each review was generally of low quality. This follows the phenomenon of “garbage in, garbage out” (Egger et al., Citation2001; Yuan & Hunt, Citation2009) whereby no matter how good a review is, the strength of the information synthesized will be limited by what original studies are available and included.
High-quality reviews (Balogh et al., Citation2016; Chaplin, Citation2004; Chaplin, Citation2009); Osugo & Cooper, Citation2016; Robertson et al., Citation2019) included: consideration of risk of bias, limitations clear (for example, differing methodologies made valid comparisons difficult), comment on low quality of included studies (lack of randomized controlled trial), and inclusion of a wide range and design of studies. Medium quality reviews (Chaplin, Citation2011; Hemmings et al., Citation2009; Kosiowski et al., Citation2016) contained many of the features of the high-quality reviews but comparison of studies was not permitted due to varied study design and methods, or there was a low number of included studies. Low-quality reviews (Slevin et al., Citation2008; Whittle et al., Citation2017) used varied literature methods and objectives leading to a lack of consistent measures of quality of the retrieved studies, and in the case of Slevin et al. (Citation2008) a systematic review was unable to be undertaken due to paucity of evidence found.
Results of individual sources of evidence:
RQ1: WHAT MODELS OF SERVICE FOR MENTAL HEALTH CARE EXIST FOR PEOPLE WITH MILD ID?
General Service Appraisal: Organization or Access to Services –
Five systematic reviews were identified regarding the organization or access to MH services for individuals with ID. Balogh et al. (Citation2016) conducted a systematic review according to the Cochrane Database of Systematic Review criteria. Nothing specific was included in the overall analysis relating specifically to mild ID. Nonetheless, Balogh et al. (Citation2016) describes one study (Hassiotis et al., Citation2001) that shows that individuals with mild or borderline ID in receipt of care from intensive case-management teams with small case-loads spent fewer days in hospital, and had fewer hospital readmissions for a psychiatric reason. The participants of this study were identified as a subset of individuals with unrecognized borderline or mild ID (subset UK700 trial) and a concurrent psychotic illness. However, two further studies (both also UK based) were unable to replicate this finding in populations under the care of community learning disability teams with broader psychiatric diagnoses and more significant cognitive impairments (Martin et al., Citation2005; Oliver et al., Citation2005). Upon consideration of intellectual disability as a whole, there was little evidence for organizational interventions; such as increased frequency or intensity of service delivery, that could impact upon psychiatric, behavioral or psychological morbidity (Balogh et al., Citation2016). Community-based specialist behavioral therapy may slightly decrease behavioral problems (Hassiotis et al., Citation2009). Overall, Balogh et al. (Citation2016) surmised that there was a need for coordinated and targeted services with clear responsibilities to best meet the needs of this population.
Chaplin (Citation2004, Citation2009) undertook two systematic reviews with similar methods to assess the difference in outcome for people with ID and mental disorder treated in general or specialized ID MH services. Chaplin (Citation2004) was unable to find conclusive evidence favoring either option due to the paucity of good-quality literature. It was highlighted that staff working in general services perceived that they lacked training in ID, and that individuals with mild ID had reduced access to their service. The systematic review was replicated in 2009, and more recent studies included (Chaplin, Citation2009). Within this review, two studies commented upon borderline intellectual function. Those who fell in to the borderline intellectual functioning category had a higher rate of psychopathology and disability than those without ID but do not receive a relative increase in care from general psychiatric services (Bouras & Holt, Citation2004). Outcomes for people with borderline intellectual functioning may be aided by intensive case management (Hassiotis et al., Citation2001). Across the range of ID, Chaplin (Citation2009) concluded that general psychiatric care could be improved by specially trained staff, and in-reach from community ID teams.
Whittle et al. (Citation2017) undertook a scoping review in order to identify barriers and facilitators to access to MH services for individuals with ID. There was no discussion of evidence for individuals with mild ID, however there were common themes found across the literature for ID in general. Barriers to access MH services included diagnostic overshadowing, lack of skilled staff, and failure to integrate services. Enablers included a multidisciplinary approach, collaborative working, and clear referral pathways.
Robertson et al. (Citation2019) conducted a systematic review in order to establish the current knowledge base for the health care of people with ID from ethnic minority groups in the UK. There was very limited good-quality evidence on this topic, due to low study numbers. However, the evidence was suggestive of there being further inequality in access to services for people with ID from ethnic minority groups. One study included within the review, (McGrother et al., Citation2002), highlighted that the sample may not have been representative for people with mild ID due to less frequent access of specialist ID services by people with mild ID.
RQ2: WHAT IS THE SCOPE OF THE EVIDENCE FOR SPECIFIC MODELS OF CARE AND TREATMENT?
Inpatient Care –
Chaplin (Citation2011) undertook a systematic review of psychiatric services for ID, in particular for inpatient care. The review included a trial (Lunsky et al., Citation2010) that examined the outcome of individuals by level of ID on a specialized inpatient unit in Canada. The individuals with mild ID improved substantially on the Global Assessment of Functioning; however, the length of stay, and improvement in psychiatric symptoms did not differ (Lunsky et al., Citation2010). For the full range of ID, Chaplin (Citation2011) included two studies (Hall et al., Citation2006; Xenitidis et al., Citation2004) that showed positive outcomes in terms of symptoms and function on a general ward where staff had received extra training. Direct comparison of general as opposed to specialist ID services showed mixed results (Hemmings et al., Citation2009); those with more complex needs were less likely to have them met on a general adult ward. Those discharged from specialist units were prescribed less medication upon discharge (S. E. White et al., Citation2010).
Community Care –
Slevin et al. (Citation2008) undertook a structured review of community learning disability teams in order to consider challenges to effective working. The review raised concerns with regard to those with mild ID and dual diagnosis, that is, autism or ADHD, and not fitting specific social care or health criteria, therefore being excluded or experiencing long delays in access. Concerns as to barriers to good community care in community ID teams were adequate specialist skills. Conversely, in general services, concerns were raised regarding staff having the adequate skills to meet the needs of an individual with ID, with inadequately trained staff being a barrier to equitable mental health care. This could infringe individuals’ rights under human rights legislation.
Hemmings et al. (Citation2009) reviewed the preceding 3-years evidence for community services, ID and MH problems. The evidence for Assertive Community Outreach (ACT) was discussed; including Hassiotis et al. (Citation2001) UK700 trial data; as well as the subsequent controlled trials by Martin et al. (Citation2005) and Oliver et al. (Citation2005). As mentioned previously, the follow-up trials were unable to replicate the UK700 trial data results, finding no significant differences between assertive and standard community outreach.
Therapeutic Interventions –
Two systematic reviews were published in 2016 examining the evidence base for therapeutic interventions for adults with mild ID and MH problems. Osugo and Cooper (Citation2016) identified that group cognitive behavioral therapy (CBT) was found by four studies (McCabe et al., Citation2006; McGillivray et al., Citation2008; McGillivray, Citation2013; McGillivray & Kershaw, Citation2015) to be effective for the treatment of depressive symptoms, which was maintained at follow-up. Group exercise was found to have a positive effect upon anxiety and depressive symptoms (Carmelli et al., Citation2009; Carraro & Gobbi, Citation2014). Five papers explored the use of antipsychotics (Antonacci & de Groot, Citation2000; Bokszanska et al., Citation2003; Shedlack et al., Citation2005; Thalayasingam et al., Citation2004; Williams et al., Citation2000) and two antidepressants (Bhaumik et al., Citation1995; Bhaumik & Wildgust, Citation1996). All showed efficacy; however, concerns regarding study design and methodology were highlighted. There were no randomized controlled trials; most were uncontrolled, not standardized and on the whole, retrospective studies. There was no investigation of sensitivity or differential dosing schedule – therefore the “much quoted” hypothesis of increased sensitivity to side effects of psychotropics for people with ID was not explored, and therefore could cause sub-optimal dosing and treatment (Osugo & Cooper, Citation2016).
Similarly, Kosiowski et al. (Citation2016), found non-conclusive results for therapeutic interventions. A meta-analysis of the available evidence (11 randomized controlled trials and one non-randomized study) showed no statistically significant effect size for – behavioral problems, depressive symptoms, anxiety, quality of life or function. Treatment for depressive symptoms (all CBT) showed the effect size as just below significance, which might have been caused by low-power studies. The methodology of the included studies varied widely and Kosiowski et al. (Citation2016) commented upon the issue of standardization and definition within these trials. For example, how “behavioural problems” was defined. This included a range from “anger” to a definite mental illness, such as “depression.”
RQ3: WHAT IS THE EXPERIENCE OF PATIENTS WITH MILD ID ACCESSING MENTAL HEALTH CARE?
Patient Feedback –
A scoping review was undertaken by Venville et al. (Citation2015) to investigate and compare the experiences of individuals with ID and MH problems in mainstream adult and specialist ID facilities. This reported that negative experiences in mainstream psychiatric services appeared to be more pronounced (in comparison specialist ID facilities) with an increased likelihood of physical restraint. Patients felt poorly informed about treatment options. In comparison, specialist ID services were viewed as offering limited opportunities for education and therapy. One study (Chinn et al., Citation2011) reported patients being verbally abused in specialist psychiatric inpatient units away from their home area. Integrated services, for example, ID in-reach on a general ward had positive feedback (Parkes et al., Citation2007). Patients described feeling more settled with an increased understanding of medications and made positive comments about nursing staff. When the experience of individuals from ethnic minority groups was examined, individuals self-identifying as black reported fewer positive experiences (Bonell et al., Citation2012). There was less consensus of experience reported by black in comparison to white participants, which could suggest a more varied experience of services and support. The authors commented upon the lack of qualitative research in this area, and called for research that is more inclusive with consideration given to increased suggestibility leading to bias (Venville et al., Citation2015).
DISCUSSION
This scoping review included eleven studies: one meta-analysis, eight systematic reviews, and two scoping reviews. The objective of the review was to explore the breadth of evidence for the structure and delivery of mental health services for people with mild ID, taking into consideration patient experience. The evidence was explored focusing upon three specific research questions regarding evidence for current models of service, current care and treatment, and the experience of people with mild ID.
IMPLICATIONS FOR CLINICAL PRACTICE
There is evidence to suggest that people with mild intellectual disability accessing mental health services benefit from improved staff training (Hall et al., Citation2006; Xenitidis et al., Citation2004) and integrated services (Parkes et al., Citation2007). There is also some weaker evidence to suggest that intensive case management (Hassiotis et al., Citation2001) can result in better outcomes for people with borderline or mild intellectual disability and comorbid mental illness.
A lack of resources results in poorer outcomes (Bouras & Holt, Citation2004). Furthermore, individuals with intellectual disability from ethnic minority groups have even poorer experiences (Robertson et al., Citation2019). This is further exacerbated by a lack of good-quality research on pharmacological and psychological interventions for people with mild intellectual disabilities (Osugo & Cooper, Citation2016).
IMPLICATIONS FOR SERVICE DEVELOPMENT AND FUTURE RESEARCH
A significant amount of progress is needed to unify access to services that people with mild ID have. In the United Kingdom, there is no agreed National model of integration of general mental health services with learning disability services (Hawramy, Citation2020). Farnklin et al. (Citation2019) makes note of the challenges in delivering specialized ID services and suggests a consultation-liaison model between general and specialist services to aid accessibility for service users. The Royal College of Psychiatrists (Shankar et al., Citation2020) provide a good-practice framework to inform and enable psychiatrists and service leads to provide high-quality care for this patient group. This framework supports the use of The Green Light Toolkit (Department of Health, Citation2017) which utilizes a self-assessment checklist to evaluate current provision, in line with National guidance.
The drive to improve equitable mental health care for all is further emphasized in a report by the National Collaborating Center for Mental Health (NCMH, Citation2019). This aims to ensure that all MH care is responsive to the strengths of each individual and to achieve equality for all. In particular, it discusses access to psychological services for people with ID. It notes that appropriate care and treatment should be accessible to all, which is in line with the Equality Act (Equality Act, Citation2010), with duty of care imposed on service providers to make reasonable adjustments for people with disabilities.
STRENGTHS AND LIMITATIONS
The strengths of this review include following the PRISMA-SCr (Tricco et al., Citation2018) assessment of the quality of systematic reviews using well-known criteria (Roever & Zoccai, Citation2015) and we have utilized a broad search strategy. Limitations may include that by only including systematic reviews and service appraisals there is potential that we may have missed evidence that hadn’t been included in any of these systematic reviews, unpublished interventions and gray literature. The conclusions made by the individual papers included need to be considered in the context of the quality of evidence they are drawn from.
CONCLUSION
This scoping review aimed to review the evidence with regard to MH services and treatment for mental disorders in individuals with mild ID. A lack of high-quality evidence for individuals with MH problems and mild ID was a continued concern throughout the review. The lack of high-quality evidence is likely to reflect a lack of research evidence rather than therapeutic effect size. There are additional ethical and methodological difficulties of recruitment of people with ID into studies in terms of consent, adequate subjects, and suggestibility in qualitative research.
There is the potential for improved outcomes with increased staff training and awareness as well as therapeutic interventions such as CBT. A common theme of needing targeted and well-coordinated services was identified, however delays with access to services for individuals with dual diagnosis was noted. There was a lack of data on the interaction between, and distinct roles and responsibilities of, ID and MH services. The review also found a lack of coherent service models, co-ordination between treating agencies, and of specific inclusion for ID within MH policy.
Utilizing the current evidence, no clear conclusions regarding MH services and treatment for mental disorders in individuals with mild ID can be drawn. There is a need for further good-quality research, including from the patient perspective and expert by experience. At this stage, there is no clear evidence for divergence from evidence-based guidelines and normal good practice for MH problems in the general population. A debate continues as to where, and from whom, individuals with mild ID should receive care and treatment. However, an increase in awareness and training would be beneficial in terms of timely access to services and appropriate treatment.
There is a need for inclusive, evidence-based guidelines for people with mild ID accessing MH services. However, without good-quality evidence, the services developed will always be based upon extrapolated and standardized evidence.
Ethical Conduct Statement
This is a scoping review and as such does not require any ethical approval as no new information has been gathered.
Data Statement
All relevant data could be made available upon reasonable request to the corresponding author.
Acknowledgments
The authors would like to acknowledge the support of the Royal College of Psychiatrists Sarah George, Library services manager, Cwm Taf Morgannwg University Healthboard for support with the literature searches.
Disclosure Statement
CW, DM and GM report no conflict. RS has received institutional and research support and personal fees from LivaNova, UCB, Eisai, Veriton Pharma, GW Pharma, and Desitin outside the submitted work. The authors CW, GM, and RS have also been contributors to the Royal College of Psychiatrists college report CR226 Mental Health services for adults with mild intellectual disability.
Three of the authors of this review were involved in preparing the Royal College of Psychiatrists college report 226: Mental Health services for adults with mild intellectual disabilities (Shankar et al., Citation2020).
Additional information
Funding
Notes
1. please could you change corrresponding author email from [email protected] to [email protected]
References
- Antonacci, D. J., & de Groot, C. M. (2000). Clozapine treatment in a population of adults with mental retardation. Journal of Clinical Psychiatry, 61(1), 22–25. https://doi.org/https://doi.org/10.4088/JCP.v61n0106
- Balogh, R., et al. (2016). Organising healthcare services for persons with intellectual disability. Cochrane Database of Systematic Reviews, ART CD007492(4).
- Bhaumik, S., Collacott, R. A., Gandhi, D., Duggirala, C., & Wildgust, H. J. (1995). A naturalistic study in the use of antidepressants in adults with learning disabilities and affective disorders. Human Psychopharmacology: Clinical and Experimental, 10(4), 283–288. https://doi.org/https://doi.org/10.1002/hup.470100405
- Bhaumik, S., Tyrer, F. C., McGrother, C., & Ganghadaran, S. K. (2008). Psychiatric service use and psychiatric disorders in adults with intellectual disability. Journal of Intellectual Disability Research, 52(11), 986–995. https://doi.org/https://doi.org/10.1111/j.1365-2788.2008.01124.x
- Bhaumik, S., & Wildgust, H. J. (1996). Treatment outcomes including withdrawal phenomenon with fluoxetine and paroxetine in patients with learning disabilities suffering from affective disorders. Human Psychopharmacology: Clinical and Experimental, 11, 337–338.
- Bokszanska, A., et al. (2003). Risperidone and olanzapine in adults with intellectual disability: A clinical naturalistic study. International Clinical Psychopharmacology, 18, 285–291.
- Bombard, Y., Baker, G. R., Orlando, E., Fancott, C., Bhatia, P., Casalino, S., Onate, K., Denis, J.-L., & Pomey, M.-P. (2018). Engaging patients to improve quality of care: A systematic review. Implementation Science, 13(1). https://doi.org/https://doi.org/10.1186/s13012-018-0784-z
- Bonell, S., Underwood, L., Radhakrishnan, V., & McCarthy, J. (2012). Experiences of mental health services by people with intellectual disabilities from different ethnic groups: A Delphi consultation. Journal of Intellectual Disability Research, 56(9), 902–909. https://doi.org/https://doi.org/10.1111/j.1365-2788.2011.01494.x
- Borthwick‐Duffy, S. A. (1994). Epidemiology and prevalence of psychopathology in people with mental retardation. Journal of Consulting and Clinical Psychology, 62(1), 17–27. https://doi.org/https://doi.org/10.1037/0022-006X.62.1.17
- Bouras, N., & Holt, G. (2004). Mental health services for adults with learning disabilities. British Journal of Psychiatry, 184(4), 291–292. https://doi.org/https://doi.org/10.1192/bjp.184.4.291
- Bubb, S. (2014). Winterbourne view - Time for change. NHS England.
- Buckles, J. (2013). A systematic review of the prevalence of psychiatric disorders in adults with intellectual disability, 2003–2010. Journal of Mental Health Research in Intellectual Disabilities, 6(3), 181–207. https://doi.org/https://doi.org/10.1080/19315864.2011.651682
- Carmelli, E., Barak, S., Morad, M., & Kodesh, E. (2009). Physical exercises can reduce anxiety and improve quality of life among adults with intellectual disability. International SportMed Journal, 10, 77–86.
- Carraro, A., & Gobbi, E. (2014). Exercise intervention to reduce depressive symptoms in adults with intellectual disabilities. Peceptual and Motor Skills, 119(1), 1–5. https://doi.org/https://doi.org/10.2466/06.15.PMS.119c17z4
- Chaplin, R. (2004). General psychiatric services for adults with intellectual disability and mental illness. Journal of Intellectual Disability Research, 48(1), 1–10. https://doi.org/https://doi.org/10.1111/j.1365-2788.2004.00580.x
- Chaplin, R. (2009). New research into general psychiatric services for adults with intellectual disability and mental illness. Journal of Intellectual Disability Research, 53(3), 189–199. https://doi.org/https://doi.org/10.1111/j.1365-2788.2008.01143.x
- Chaplin, R. (2011). Mental health services for people with intellectual disabilities. Current Opinion in Psychiatry, 24(5), 372–376. https://doi.org/https://doi.org/10.1097/YCO.0b013e3283472524
- Chinn, D., Hall, I., Ali, A., Hassell, H., & Patkas, I. (2011). Psychiatric in-patients away from home: Accounts by people with intellectual disabilities in specialist hospitals outside their home localities. Journal of Applied Research in Intellectual Disabilities, 24(1), 50–60. https://doi.org/https://doi.org/10.1111/j.1468-3148.2010.00572.x
- Cooper, S. A., Smiley, E., Morrison, J., Williamson, A., & Allan, L. (2007). Mental ill-health in adults with intellectual disabilities: Prevalence and associated factors. British Journal of Psychiatry, 190(1), 27–35. https://doi.org/https://doi.org/10.1192/bjp.bp.106.022483
- Cumella, S. (2007). Chapter 22: Mental health and intellectual disability: The development of services. In N. Bouras & G. Holt (Eds.), Psychiatric and behavioural disorders in intellectual and developmental disabilities. Cambridge University Press.
- Department of Health. (2017). National development team for inclusion. Green light toolkit: A guide to auditing and improving your mental health service so that it is effective in supporting people with autism and people with learning disabilities. NDTI.
- Egger, M., Smith, G. D., & Altman, D. G. (2001). Chapter 3: Problems and limitations in conducting systematic reviews. In M. Egger, G. D. Smith, & D. G. Altman (Eds.), Systematic reviews in health care: Meta‐analysis in context, second edition (pp. 43–68). BMJ Publishing Group.
- Equality Act. (2010). Equality act. The Stationery Office: s.n.
- Farnklin, C., et al. (2019). Chromosomes, country, catatonia and contrasts: Intellectual disability and autism in Queensland. Sage Publications.
- Hall, I., Parkes, C., Samuels, S., & Hassiotis, A. (2006). Working across boundaries: Clinical outcomes for an integrated mental health service for people with intellectual disabilities. Journal of Intellectual Disability Research, 50(8), 598–607. https://doi.org/https://doi.org/10.1111/j.1365-2788.2006.00821.x
- Hamlin, A., & Oakes, P. (2008). Reflections on deinstitutionalization in the United Kingdom. Journal of Policy and Practice in Intellectual Disabilities, 5(1), 47–55. https://doi.org/https://doi.org/10.1111/j.1741-1130.2007.00139.x
- Harris, J. (2006). Intellectual disability: Understanding its development, causes, classification, evaluation, and treatment. Oxford University Press.
- Hassiotis, A., Barron, P., & O’Hara, J. (2000). Mental health services for people with learning disabilities - A complete overhaul is needed with strong links to mainstream services. British Medical Journal, 321(7261), 583–584. https://doi.org/https://doi.org/10.1136/bmj.321.7261.583
- Hassiotis, A., Robotham, D., Canagasabey, A., Romeo, R., Langridge, D., Blizard, R., Murad, S., & King, M. (2009). Randomized, single-blind, controlled trial of a specialist behavior therapy team for challenging behavior in adults with intellectual disabilities. American Journal of Psychiatry, 166(11), 1278–1285. https://doi.org/https://doi.org/10.1176/appi.ajp.2009.08111747
- Hassiotis, A., Ukoumunne, O. C., Byford, S., Tyrer, P., Harvey, K., Piachaud, J., Gilvarry, K., & Fraser, J. (2001). Intellectual functioning and outcome of patients with severe psychotic illness randomised to intensive case management: Report from the UK700 trial. British Journal of Psychiatry, 178(2), 166–171. https://doi.org/https://doi.org/10.1192/bjp.178.2.166
- Hawramy, M. (2020). Interface between community intellectual disability and general adult psychiatry services. BJPsych Advances, 1–7.
- Hemmings, C. P., O’Hara, J., McCarthy, J., Holt, G., Eoster, F., Costello, H., Hammond, R., Xenitidis, K., & Bouras, N. (2009). Comparison of adults with intellectual disabilities and mental health problems admitted to specialist and generic inpatient units. British Journal of Learning Disabilities, 37(2), 123–128. https://doi.org/https://doi.org/10.1111/j.1468-3156.2008.00532.x
- Holden, B., & Gitlesen, J. P. (2004). The association between severity of intellectual disability and psychiatric symptomatology. Journal of Intellectual Disability Research, 48(6), 556–562. https://doi.org/https://doi.org/10.1111/j.1365-2788.2004.00624.x
- Irranca-Davies, H., Palmer, K., & Goodall, A. (2018). Learning disability – Improving lives programme. Welsh Government.
- Kosiowski, N., Klein, K., Arnold, K., Kösters, M., Schützwohl, M., Salize, H. J., & Puschner, B. (2016). Effectiveness of interventions for adults with mild to moderate intellectual disabilities and mental health problems: Systematic review and meta-analysis. British Journal of Psychiatry, 209(6), 469–474. https://doi.org/https://doi.org/10.1192/bjp.bp.114.162313
- Lunsky, Y., White, S. E., Palucka, A. M., Weiss, J., Bockus, S., & Gofine, T. (2010). Clinical outcomes of a specialised inpatient unit for adults with mild to severe intellectual disability and mental illness. Journal of Intellectual Disability Research, 54(1), 64–69. https://doi.org/https://doi.org/10.1111/j.1365-2788.2009.01213.x
- Martin, G., Costello, H., Leese, M., Slade, M., Bouras, N., Higgins, S., & Holt, G. (2005). An exploratory study of assertive community treatment for people with intellectual disability and psychiatric disorders: Conceptual, clinical, and service issues. Journal of Intellectual Disability Research, 49(7), 516–524. https://doi.org/https://doi.org/10.1111/j.1365-2788.2005.00709.x
- McCabe, M. P., McGillivray, J. A., & Newton, D. C. (2006). Effectiveness of treatment programmes for depression among adults with mild/moderate intellectual disability. Journal of Intellectual Disability Research, 50(4), 239–247. https://doi.org/https://doi.org/10.1111/j.1365-2788.2005.00772.x
- McGillivray, J. (2013). The impact of staff initiated referral and intervention protocols on symptoms of depression in people with mild intellectual disability. Research in Developmental Disabilities, 34(2), 730–738. https://doi.org/https://doi.org/10.1016/j.ridd.2012.11.005
- McGillivray, J. A., & Kershaw, M. (2015). Do we need both cognitive and behavioural components in interventions for depressed mood in people with mild intellectual disability? Journal of Intellectual Disability Research, 59(2), 105–115. https://doi.org/https://doi.org/10.1111/jir.12110
- McGillivray, J. A., McCabe, M. P., & Kershaw, M. M. (2008). Depression in people with intellectual disability: An evaluation of a staff‐administered treatment program. Research in Developmental Disabilities, 29(6), 524–536. https://doi.org/https://doi.org/10.1016/j.ridd.2007.09.005
- McGrother, C. W., Bhaumik, S., Thorp, C. F., Watson, J. M., & Taub, N. A. (2002). Prevalence, morbidity and service need among South Asian and white adults with intellectual disability in Leicestershire, UK. Journal of Intellectual Disability Research, 46(4), 299–309. https://doi.org/https://doi.org/10.1046/j.1365-2788.2002.00391.x
- NCMH. (2019). Advancing mental health equality: Steps and guidance on commissioning and delivering equality in mental health care. National Collaborating centre for mental health.
- New South Wales Ministry of Health. (2012). Service framework to improve the healthcare of people with intellectual disability. s.n.
- NICE. (2011a). Clinical guidance 113: Generalised anxiety disorder and panic disorder in adults: Management. National institure for Health and Clinical Excellence.
- NICE. (2011b). Clinical guidance 123: Common mental health problems: Identification and pathways to care. National institute for Health and Care Excellence.
- Oliver, P. C., Piachaud, J., Tyrer, P., Regan, A., Dack, M., Alexander, R., Bakala, A., Cooray, S., Done, D. J., & Rao, B. (2005). Randomized controlled trial of assertive community treatment in intellectual disability: The TACTILD study. Journal of Intellectual Disability Research, 49(7), 507–515. https://doi.org/https://doi.org/10.1111/j.1365-2788.2005.00706.x
- Osugo, M., & Cooper, S.-A. (2016). Interventions for adults with mild intellectual disabilities and mental ill-health: A systematic review. Journal of Intellectual Disability Research, 60(6), 615–622. https://doi.org/https://doi.org/10.1111/jir.12285
- Parkes, C., Samuels, S., Hassiotis, A., Lynggaard, H., & Hall, I. (2007). Incorporating the views of service users in the development of an integrated psychiatric service for people with learning disabilities. British Journal of Learning Disabilities, 35(1), 23–29. https://doi.org/https://doi.org/10.1111/j.1468-3156.2006.00419.x
- Parkin, E. (2016). Learning disability - Overview of policy and services. House of Commons Library.
- Peters, M. (2020). Chapter 11: Scoping reviews. In E. Aromataris, Z. Munn, et al. (Eds.), JBI manual for evidence synthesis (pp. online). JBI.
- Pluye, P. et al. (2011). Proposal: A mixed methods appraisal tool for systematic mixed studies reviews. Retrieved May 18, 2020, from http://mixedmethodsappraisaltoolpublic.pbworks.com
- RCPsych. (2017). Specialists in the psychiatry of learning disability: A competency based curriculum for specialist training in psyhiatry. Royal College of Psychiatrists.
- Reiss, S. (1990). Prevalence of dual diagnosis in community-based day programs in Chicago metropolitan area. American Journal on Mental Retardation, 94, 578–585.
- Robertson, J., Raghavan, R., Emerson, E., Baines, S., & Hatton, C. (2019). What do we know about the health and health care of people with intellectual disabilities from minority ethnic groups in the United Kingdom? A systematic review. Journal of Applied Research in Intellectual Disabilities, 32(6), 1310–1334. https://doi.org/https://doi.org/10.1111/jar.12630
- Roever, L., & Zoccai, G. B. (2015). Critical appraisal of systematic review and meta-analyses. Evidence Based Medicine and Practice, 1(1), e106.
- Shankar, R., et al. (2020). Mental health services for adults with mild intellectual disability. College report 226. Royal college of Psychiatrists.
- Shedlack, K. J., Hennen, J., Magee, C., & Cheron, D. M. (2005). Assessing the utility of atypical antipsychotic medication in adults with mild mental retardation and comorbid psychiatric disorders. Journal of Clinical Psychiatry, 66(1), 52–62. https://doi.org/https://doi.org/10.4088/JCP.v66n0108
- Sheehan, R., et al. (2015). Mental illness, challenging behaviour, and psychotropic drug prescribing in people with intellectual disability: UK population based cohort study. British Medical Journal, 351.
- Sheehan, R., & Paschos, D. (2013). A comparison of different models to meet the mental health needs of adults with intellectual disabilities. Advances in Mental Health and Intellectual Disabilities, 7(3), 161–168. https://doi.org/https://doi.org/10.1108/20441281311320747
- Singleton, N., et al. (2001). Psychiatric morbidity among adults living in private households in 2000. HMSO.
- Slevin, E., Truesdale-Kennedey, M., McConkey Barr, O., & Taggart, L. (2008). Community learning disability teams: Developments, composition and good practice. Journal of Intellectual Disabilities, 12(1), 59–79. https://doi.org/https://doi.org/10.1177/1744629507083583
- Thalayasingam, S., Alexander, R. T., & Singh, I. (2004). The use of clozapine in adults with intellectual disability. Journal of Intellectual Disability Research, 48(6), 572–579. https://doi.org/https://doi.org/10.1111/j.1365-2788.2004.00626.x
- Tricco, A. C., Lillie, E., Zarin, W., O’Brien, K. K., Colquhoun, H., Levac, D., Moher, D., Peters, M. D. J., Horsley, T., Weeks, L., Hempel, S., Akl, E. A., Chang, C., McGowan, J., Stewart, L., Hartling, L., Aldcroft, A., Wilson, M. G., Garritty, C., Lewin, S., & Straus, S. E. (2018). PRISMA extension for scoping reviews (PRISMA-ScR): Checklist and explanation. Annals of Internal Medicine, 169(7), 467–473. https://doi.org/https://doi.org/10.7326/M18-0850
- Venville, A., Sawyer, A.-M., Long, M., Edwards, N., & Hair, S. (2015). Supporting people with an intellectual disability and mental health problems: A scoping review of what they say about service provision. Journal of Mental Health Research in Intellectual Disabilities, 8(3–4), 186–212. https://doi.org/https://doi.org/10.1080/19315864.2015.1069912
- White, P., Chant, D., Edwards, N., Townsend, C., & Waghorn, G. (2005). Prevalence of intellectual disability and comorbid mental illness in an Australian community sample. Australian & New Zealand Journal of Psychiatry, 39(5), 395–400. https://doi.org/https://doi.org/10.1080/j.1440-1614.2005.01587.x
- White, S. E., Lunsky, Y., & Grieve, C. (2010). Profiles of patients with intellectual disability and mental illness in specialized and generic units in an Ontario psychiatric hospital. Journal of Mental Health Research in Intellectual Disabilities, 3(3), 117–131. https://doi.org/https://doi.org/10.1080/19315864.2010.487632
- Whittle, E. L., Fisher, K. R., Reppermund, S., Lenroot, R., & Trollor, J. (2017). Barriers and enablers to accessing mental health services for people with intellectual disability: A scoping review. Journal of Mental Health Research in Intellectual Disabilities, 11(1), 69–102. https://doi.org/https://doi.org/10.1080/19315864.2017.1408724
- Williams, H., Clarke, R., Bouras, N., Martin, J., & Holt, G. (2000). Use of the atypical antipsychotics Olanzapine and Risperidone in adults with intellectual disability. Journal of Intellectual Disability Research, 44(2), 164–169. https://doi.org/https://doi.org/10.1046/j.1365-2788.2000.00284.x
- Xenitidis, K., Gratsa, A., Bouras, N., Hammond, R., Ditchfield, H., Holt, G., Martin, J., & Brooks, D. (2004). Psychiatric inpatient care for adults with intellectual disabilities: Generic or specialised units? Journal of Intellectual Disability Research, 48(1), 11–18. https://doi.org/https://doi.org/10.1111/j.1365-2788.2004.00586.x
- Yuan, Y., & Hunt, R. (2009). Systematic reviews: The good, the bad, and the ugly. The American Journal of Gastroenterology, 104(5), 1086–1092. https://doi.org/https://doi.org/10.1038/ajg.2009.118
Appendix A.
Search strategy
At this stage, search terms were kept broad, in order for as many studies to be found as possible. Searches were conducted in the Cochrane Library, Medline, Medline Inprocess, Embase, PsychINFO, and NICE Evidence. An example of the full search strategy from Medline in 2018 is included below.
Search terms were as follows:
Developmental disorder
Intellectual disability
Intellectual impairment
Learning disability
Learning disorder
Mental retardation
Mentally disabled person
Mild intellectual disability
Combined with:
Community mental
Community services
Delivery of healthcare
Health service accessibility
MH
MH services
It was noted that initially only 2 articles directly relating to mild ID were found by this method – therefore the search was repeated excluding the link for the term “mild” and “intellectual disability.” Included papers were also limited to systematic reviews, guidelines, or RCTs to keep within the aims of the project.
