?Mathematical formulae have been encoded as MathML and are displayed in this HTML version using MathJax in order to improve their display. Uncheck the box to turn MathJax off. This feature requires Javascript. Click on a formula to zoom.
?Mathematical formulae have been encoded as MathML and are displayed in this HTML version using MathJax in order to improve their display. Uncheck the box to turn MathJax off. This feature requires Javascript. Click on a formula to zoom.ABSTRACT
Rotavirus (RV) diarrhea is one of the most common cause of childhood morbidity and mortality in the world. The World Health Organization has recommended RV vaccines’ use in national immunization programs since 2009. However, access to vaccines remain limited, particularly for most low- and middle-income countries where the burden of the disease is high. The Philippines is a lower-middle income country in Asia where RV vaccination remains limited. Recent studies in the Philippines indicate an estimated vaccine effectiveness of 60% against RV hospitalization, and a 50–60% reduction of all cause diarrhea among children aged under 5 within the population. Furthermore, we estimate that 225 rotavirus cases can be prevented per 1000 children vaccinated against RV. This information will be crucial as policymakers decide on expanding RV vaccination nationwide.
Introduction
Globally, diarrhea is the fifth leading cause of mortality, responsible for 446,000 deaths among children under 5 years of age in 2016.Citation1 Diarrhea is also a leading cause of morbidity and results in long term adverse health outcomes.Citation2 The most common cause of diarrhea in childhood is rotavirus.Citation3
Rotavirus vaccine was recommended by the World Health Organization (WHO) in 2009 for use in all national immunization programs and must be prioritized in countries where deaths due to rotavirus diarrhea are substantial.Citation4 At that time, two available rotavirus vaccines were licensed internationally and available at reduced prices for Gavi-eligible countries. However, introduction of RV vaccines in middle- and lower-middle income countries, particularly in Asia have been slow. As of 2016, the WHO Southeast Asia and Western Pacific Regions had the fewest countries that introduced RV vaccines.Citation5 We present the experience in the Philippines, a lower-middle income country in Asia, where RV vaccine introduction remains limited to selected regions.
Rotavirus in the Philippines
Diarrhea was the second leading cause of death in children 1–4 years of age and the 6th leading cause of death in infants in 2014 in the Philippines.Citation6 Since the 1980s, rotavirus has been described as one of the leading cause of hospitalized and outpatient diarrhea for children.Citation7–Citation16 Studies from the 1980s to early 2000s have estimated that RV was the cause of 20–40% of all diarrhea cases, which varies in different settings (i.e., hospitalization vs. outpatient consults). The most recent study, performed in an urban area from 2005 to 2006, estimated the burden of RV at 31% among diarrheal hospitalizations, 30% among emergency consults for diarrhea, and 15% among diarrheal outpatient consults in children <5 years old.Citation17
Considering the significant burden of diarrhea, the Philippines was the first country in Asia to introduce the monovalent RV (RV1) (Rotarix®, GSK) vaccine in 2012 in its routine immunization program. At that time of initial roll-out, RV vaccination was limited to the families who belonged to the lowest economic quintile and were receiving conditional cash transfer (CCT) from the government. However, implementation proved to be difficult. First, families in the program were not evenly distributed throughout the country, hence delivery of RV vaccines was complicated and required knowledge of the geographic distribution of the targeted families. Second, not all families in the program have children who were aged 6 to 15 weeks, which was the recommended age group to receive the first dose of the vaccine at that time of introduction. The difficulties encountered in targeting resulted in low vaccination coverage. At the same time, some sectors felt that funding may be better allocated to other priorities instead of an expensive vaccine for diarrheal diseases. It was argued that improving the implementation of other preventive measures such as exclusive breastfeeding, improvements in nutrition, hygiene, and water quality; and the implementation of the Integrated Management of Childhood Illness (IMCI), Oral Rehydration Therapy (ORT) and Zinc Supplementation will improve outcomes for diarrhea. At that time, information from clinical trials reported varying vaccine efficacy depending on the region where the study was conducted ranging from 81% in Latin America to 42.7% in Bangladesh.Citation18 Hence, policymakers requested the Expanded Programme on Immunization (EPI) of the Department of Health (DOH) to collate more information on the burden of rotavirus and assess the effectiveness of the RV vaccine in the Philippines.
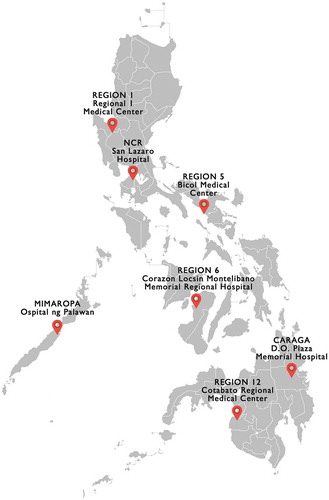
In 2012, the rotavirus sentinel surveillance was established in the Philippines in a phased manner in seven hospitals distributed across the different regions in the country (). Children under five years of age who underwent treatment with intravenous rehydration for acute diarrhea in a surveillance hospital are included in the surveillance. Diarrhea is defined using the standard WHO case definition as the passage of 3 or more stools within a 24 hour period for ≤14 days as a child years of age.Citation19 Specimens are collected and sent to the Research Institute for Tropical Medicine (RITM), where ELISA Immunoassay for RV confirmation of suspected cases was performed. In 2012, the CARAGA Region had the highest number of reported cases of diarrhea. Since this was also the region with one of the highest poverty rates in the country,Citation20 the sentinel hospital in CARAGA, the D.O. Plaza Hospital (DOPH) was chosen as the site for the RV vaccine effectiveness assessment.
Rotavirus vaccine effect in the Philippines
In 2014, using the platform of the rotavirus surveillance in DOPH, an effectiveness assessment was initiated. Only children eligible to participate in the surveillance and eligible to have received the RV vaccine were included. RV1 vaccine was given at 6 and 10 weeks of age together with oral polio vaccine. Vaccination status was verified in the clinic records. Results show that at least one dose of RV1 vaccine, was found to have a vaccine effectiveness (VE) of 60% (24–79%) against RV hospitalization and 64% (11–85%) against severe RV diarrhea.Citation21 Using information from the study, we calculated the number of RV cases that can be prevented per 1,000 vaccinated with the following formula:
Among children older than 8 months, we found that approximately 225 cases of RV can be prevented per 1,000 children vaccinated.
A parallel impact assessment was also conducted by comparing diarrheal admissions and outpatient consults in an area where RV1 was introduced and an area where RV was yet to be introduced.Citation22 In this study, the declines in the total number of hospitalizations from all-cause diarrhea was observed at 28%, 56%, 63%, and 59%, across the 4 years post-routine RV1 immunization, consecutively. In contrast, no similar reductions were seen in the area where no vaccination occurred.
We also investigated other factors that may affect all-cause diarrhea cases such as breastfeeding rates, changes in access to clean water and improved sanitation in the area where vaccination occurred. We found no changes in any of these factors during the years reviewed. The reduction in the hospitalized cases was not limited to the targeted population but was also seen in children older than 1 year, which may suggest herd effects. The extension of the vaccine’s effect to the unvaccinated population (older children), and non-vaccine targets (immunocompromised patients, pregnant women, elderly), dramatically expands the vaccine’s potential benefit in the community.
Prioritizing rotavirus vaccines
RV vaccines were shown to perform differently in various settings, with higher efficacyCitation23 and effectivenessCitation24,Citation25 seen in higher income countries and those with low mortality. The VE of 60% of any dose of RV1 vaccine against RV hospitalization is comparable to the results of other middle-income countries (VE- 57%, 95% CI 47–66%, p < 0.001) in the recent meta-analysis.Citation25
The first two internationally available RV vaccines: RV1 (Rotarix®, GSK) and RV5 (Rotateq®, Merck), were WHO prequalified in 2009 and 2008, respectively. WHO prequalification allows United Nation agencies to procure certain products including vaccines. Despite the availability of these two vaccines, RV vaccine demand was slower than anticipated. As of 2016, 110 countries representing 69% of the global birth cohort still have not adopted RV vaccine into their national immunization programs.Citation5 Each country may have different reasons for the delay in RV vaccine adoption, some of these may include programmatic challenges, lack of cold chain capacity, concerns over long-term vaccine pricing particularly for non-Gavi eligible countries, and sustainable supply availability.Citation26 In the Philippines, cold chain capacity was increased in 2014, paving the way for introduction of new vaccines. The Philippines has never been Gavi-eligible and was only one of two middle-income countries to procure RV1 vaccines through UNICEF from 2014 to 2016, with the cost of ~US$15 per 2-dose course.Citation26 The cost of procurement of RV1 in 2012 was more than the costs of procurement for all traditional EPI vaccines (BCG, DPT-HepB-Hib, measles, OPV). Costs of vaccine and budget allocation are important considerations particularly in lower-middle income countries where limited resources require prioritization of different interventions. Although one study has shown that the RV1 vaccine is cost-effective when the full course costs ~US$20.6,Citation27 another study using a dynamic transmission model and a full course vaccine cost of US$19.7 showed otherwise.Citation28
In some Asian countries, including the Philippines, a private market for vaccines exist.Citation29 Previously, new vaccines are only available in the private clinics and the costs for RV vaccines in the market in 2018 ranged from US$34 to $44 per dose.Citation30 The Philippines’ EPI estimates that approximately 10% of the targeted population obtain their immunizations from private clinics of pediatricians or general practitioners. In 2010, as new vaccines become available, specific line items for vaccine financing were included in the national budget allowing earlier adoption of vaccines into the national immunization programs.
In March and September 2018, two new RV vaccines, the monovalent 116E strain (Rotavac®, Bharat Biotech International, India) and the pentavalent G1, G2, G3, G4, and G9 (Rotasiil®, Serum Institute of India, India), respectively achieved WHO prequalification. Rotavac® has a vaccine efficacy of 53.6% for severe RV diarrhea in IndiaCitation31 while Rotasiil® has efficacies of 60.5% to 66.7% in IndiaCitation32 and Niger,Citation33 respectively. These vaccines cost less, with Rotavac’s price in India at US$2.85 for a full courseCitation34 and Rotasiil® is estimated to cost less than US$6 for a full course.Citation35 Furthermore, Rotasiil® has the distinct advantage over the other vaccines as being more heat stableCitation33 and can be used outside the cold chain. Since 2016, phased introduction of RV vaccines began in India, which has the highest burden of RV disease globally.
Lower middle-income countries receive minimal support from Gavi and other funding agencies for upscaling of their immunization programs. Most low-income countries supported by Gavi, meanwhile, are facing issues on the sustainability of the program once the support is withdrawn. With the background of limited resources and competing priorities, economic analysis is crucial for most countries on new vaccine introduction in the immunization program. Newer vaccines released in the market may change the cost-benefit ratio to favor the use of vaccines in most of Gavi-countries, and low- and middle-income countries without Gavi support. Newer vaccines also have distinct properties that may change how the vaccines work in real-life settings.
In the Philippines, the policymakers sought for additional evidence to assist in the decision-making for the introduction of RV vaccines in the routine immunization. Equitable access to life-saving vaccines is important for all countries to achieve the sustainable development goals (SDGs). The status of RV vaccine introduction in the Philippines reflects the decision of most of lower middle income countries in Asia in the slow adoption of the vaccine in the immunization program. In this paper, we present the information requested by policymakers to inform their decisions for possible expansion of RV vaccine nationwide.
Disclosure of potential conflicts of interest
No potential conflicts of interest were disclosed.
References
- G. B. D. Diarrhoeal Disease Collaborators. Estimates of the global, regional, and national morbidity, mortality, and aetiologies of diarrhoea in 195 countries: a systematic analysis for the Global Burden of Disease Study 2016. Lancet Infect Dis. 2018. doi:https://doi.org/10.1016/S1473-3099(18)30362-1.
- Troeger C, Colombara DV, Rao PC, Khalil IA, Brown A, Brewer TG, Guerrant RL, Houpt ER, Kotloff KL, Misra K, et al.. Global disability-adjusted life-year estimates of long-term health burden and undernutrition attributable to diarrhoeal diseases in children younger than 5 years. Lancet Glob Health. 2018;6:e255–e269. doi:https://doi.org/10.1016/S2214-109X(18)30045-7.
- Troeger C, Khalil IA, Rao PC, Cao S, Blacker BF, Ahmed T, Armah G, Bines JE, Brewer TG, Colombara DV, et al.. Rotavirus vaccination and the global burden of rotavirus diarrhea among children younger than 5 years. JAMA Pediatr. 2018;172:958–965. doi:https://doi.org/10.1001/jamapediatrics.2018.1960.
- World Health Organization. Rotavirus vaccines: an update. Wkly Epidemiol Rec. 2009;84:533–540.
- Abou-Nader AJ, Sauer MA, Steele AD, Tate JE, Atherly D, Parashar UD, et al.. Global rotavirus vaccine introductions and coverage: 2006–2016. Hum Vaccin Immunother. 2018;14:2281–2296. doi:https://doi.org/10.1080/21645515.2018.1470725.
- Department of Health. 2014 Philippine Health Statistics. 2016; [ accessed 2018 Oct 26]. https://www.doh.gov.ph/sites/default/files/publications/2014PHS_PDF.pdf.
- Adkins HJ, Escamilla J, Santiago LT, Ranoa C, Echeverria P, Cross JH. Two-year survey of etiologic agents of diarrheal disease at San Lazaro Hospital, Manila, Republic of the Philippines. J Clin Microbiol. 1987;25:1143.
- Arciaga MR, Santana-Arciaga RT, Cristobal FL, Nazareth B, Roces MCR, Grafil I, et al.. Community response to a rotavirus diarrhea outbreak in Zamboanga City. West Mindanao Health Res J. 2002;3:33–47.
- Bravo LC, Saniel MC, Rogacion JM, Santos-Ocampo PD. Enteropathogens in acute diarrhea: clinical indicators. Phil J Pediatr. 1989;38:78–83.
- Lucero MG, Saniel MC, Geronimo JG, Ang CV, Leano FT, Mate RB, et al.. Etiology of diarrhea in hospitalized children. Phil J Microbiol Infect Dis. 1984;13:17–24.
- Paje-Villar E, Co BG, Carandang EH, Raymundo A, Lagamayo E, Hart CA, et al.. Diarrheas among Filipino infants and children: clinical and laboratory correlations. Santo Tomas J Med. 1992;41:53–63.
- San Pedro MC, Walz SE. A comprehensive survery of pediatric diarrhea at a private hospital in Metro Manila. Southeast Asian J Trop Med Public Health. 1991;22:203.
- Saniel MC. Prospective study of diarrhea in infants and young children of a peri-urban Philippine community: morbidity patterns and etiologies. Trans Nat Aca Sci Tech Philipp. 1986;8:183–187.
- Saniel MC, Moriles RR, Monzon OT, Salazar NP, Leano FT, Trajano EC, Sombrero LT, Mate RB, Villanueva JA, Geronimo JE. The relative importance of various enteropathogens in the etiology of acute diarrhea: a hospital-based study in urban Philippines. 14th SEAMIC Workshop; 1988; Tokyo (Japan).
- Santos MIBL, Daag J, Bravo LC. Rotavirus acute gastroenteritis among Filipino children in year 2001. Pediatr Infect Dis Soc Philipp J. 2002;6:11–19.
- Villa F. The prevalence and clinical profile of rotavirus diarrhea in a community hospital. Phil J Pediatr. 1994;43:183–187.
- Carlos CC, Inobaya MT, Bresee JS, Lagrada ML, Olorosa AM, Kirkwood CD, et al.. The burden of hospitalizations and clinic visits for rotavirus disease in children aged <5 years in the Philippines. J Infect Dis. 2009;200(Suppl 1):S174–81.doi:https://doi.org/10.1086/605044.
- Fischer Walker CL, Black RE. Rotavirus vaccine and diarrhea mortality: quantifying regional variation in effect size. BMC Public Health. 2011;11(Suppl 3):S16. doi:https://doi.org/10.1186/1471-2458-11-S3-S16.
- World Health Organization Department of Immunization Vaccines and Biologicals. Generic protocol for monitoring impact of rotavirus vaccination of gastroenteritis disease. Geneva (Switzerland): World Health Organization; 2008.
- National Statistical Coordination Board. Poverty statistics: Agusan del Sur. Manila, Philippines: Philippine Statistical Authority; 2010.
- Lopez AL, Daag JV, Esparagoza J, Bonifacio J, Fox K, Nyambat B, Parashar UD, Ducusin MJ, Tate JE. Effectiveness of monovalent rotavirus vaccine in the Philippines. Sci Rep. 2018;8:14291. doi:https://doi.org/10.1038/s41598-018-32595-9.
- Lopez AL, Raguindin PF, Esparagoza J, Fox K, Batmunkh N, Bonifacio J, Parashar UD, Tate JE, Ducusin MJ. Impact of rotavirus vaccine on diarrheal hospitalization and outpatient consultations in the Philippines: first evidence from a middle-income Asian country. Vaccine. 2018;36:3308–3314. doi:https://doi.org/10.1016/j.vaccine.2018.04.058.
- Soares-Weiser K, MacLehose H, Ben-Aharon I, Goldberg E, Pitan F, Cunliffe N. Vaccines for preventing rotavirus diarrhoea: vaccines in use. Cochrane Database Sys Rev. 2010;5. doi:https://doi.org/10.1002/14651858.CD008521.
- Burnett E, Jonesteller CL, Tate JE, Yen C, Parashar UD. Global impact of rotavirus vaccination on childhood hospitalizations and mortality from Diarrhea. J Infect Dis. 2017;215:1666–1672. doi:https://doi.org/10.1093/infdis/jix186.
- Hungerford D, Vivancos R, Read JM, Iturriza-Gomicronmara M, French N, Cunliffe NA. Rotavirus vaccine impact and socioeconomic deprivation: an interrupted time-series analysis of gastrointestinal disease outcomes across primary and secondary care in the UK. BMC Med. 2018;16. doi:https://doi.org/10.10.1186/s12916-017-0989-z.
- UNICEF Supply Division. Rotavirus vaccine: supply & demand update. 2016; [ accessed 2018 Oct 28]. https://www.unicef.org/supply/files/Rotavirus_Vaccine_Supply_and_Demand_Update_-_October_2016.pdf.
- Lee I-H, Standaert B, Nievera MC, Jossie. R. Cost-effectiveness analysis of universal mass vaccination of Rotarix in the Philippines. PIDSPJ. 2014;15:15–29. http://www.pidsphil.org/journal_summary.php?id=178.
- Lam HY, Wu DB, Rivera AS, Alejandria MM, Velasco GN, Sison OT, Ladia MA, Mantaring JB, Santillan M. Assessing the cost-effectiveness of a Universal Rotavirus Vaccination program for the Philippines using a dynamic transmission model. Value Health. 2015;18:A225. doi:https://doi.org/10.1016/j.jval.2015.03.1308.
- Amarasinghe A, Davison L, Diorditsa S. Engagement of private providers in immunization in the Western Pacific region. Vaccine. 2018;36:4958–4962. doi:https://doi.org/10.1016/j.vaccine.2018.01.008.
- MIMS Philipppines. Rotarix and Rotateq. 2018; [ accessed Oct 28]. https://www.mims.com.
- Bhandari N, Rongsen-Chandola T, Bavdekar A, John J, Antony K, Taneja S, Goyal N, Kawade A, Kang G, Rathore SS, et al.. Efficacy of a monovalent human- bovine (116E) rotavirus vaccine in Indian infants: a randomised, double-blind, placebo-controlled trial. Lancet. 2014;383:2136–2143. doi:https://doi.org/10.1016/S0140-6736(13)62630-6.
- Kulkarni PS, Desai S, Tewari T, Kawade A, Goyal N, Garg BS, Kumar D, Kanungo S, Kamat V, Kang G, et al.. A randomized Phase III clinical trial to assess the efficacy of a bovine-human reassortant pentavalent rotavirus vaccine in Indian infants. Vaccine. 2017;35:6228–6237. doi:https://doi.org/10.1016/j.vaccine.2017.09.014.
- Isanaka S, Guindo O, Langendorf C, Matar Seck A, Plikaytis BD, Sayinzoga-Makombe N, McNeal MM, Meyer N, Adehossi E, Djibo A, et al.. Efficacy of a Low-Cost, Heat-Stable Oral Rotavirus Vaccine in Niger. N Engl J Med. 2017;376:1121–1130. doi:https://doi.org/10.1056/NEJMoa1609462.
- UNICEF Supply Division. Vaccine price data. 2016; [ accessed 2018 Oct 28]. https://www.unicef.org/supply/files/180705_Rota.pdf.
- Deen J, Lopez AL, Kanungo S, Wang XY, Anh DD, Tapia M, Grais RF. Improving rotavirus vaccine coverage: can newer-generation and locally produced vaccines help? Hum Vaccin Immunother. 2018;14:495–499. doi:https://doi.org/10.1080/21645515.2017.1403705.