ABSTRACT
Assessing vaccine hesitancy and its determinants is pivotal to optimize vaccine acceptance in anticoagulated patients, given that this population has been described to have a higher risk of severe COVID-19-related complications. This study assessed the moderator role of patients’ health engagement on the relationship between health literacy and vaccine hesitancy. A web-based survey was performed in Italy during the first wave (June–August 2020) and the second wave (October 2020–March 2021) of the COVID-19 pandemic, enrolling 288 patients. The rates of vaccine hesitancy reported during the first pandemic wave were 38.4% and 30.8% during the second wave (when a vaccine was available) (p = .164). A moderation analysis was performed to assess the role of health engagement in influencing the relationship from health literacy to vaccine hesitancy. Patients’ health engagement enhanced the effects of health literacy on decreasing vaccine hesitancy (p < .001), suggesting that co-construction strategies for communicative action are pivotal.
Introduction
Several studies recently conducted on the general population demonstrated that social-cultural features and psychological antecedents were predictors of the COVID-19 vaccine acceptance. Graffigna et al. estimated that 41% of The Italian citizens, during the first wave of the COVID-19 pandemic (March–June 2020), were hesitant or unwilling toward receiving COVID-19 vaccines.Citation1 The authors also highlighted that promoting patients’ health engagement (PHE), defined as the psychological process of emotional maturation from a position of disengagement regarding health-related challenges toward a position of engagement,Citation2 is pivotal in the educational campaigns to enhance the citizen–science alliance and the levels of patients’ health literacy (HL).Citation1 HL is the individual’s capacity to obtain, understand, and function the essential information and services to best manage health-related decisions.Citation3 Thus, monitoring the rates of vaccine hesitancy (VH), defined as a delay in acceptance or refusal of vaccines despite the availability of vaccination services,Citation4 and the determinants of VH over the several steps of the vaccination campaign in country-specific settings is highly informative to evaluate the trends and enhance the communication strategies.
Oral anticoagulation therapy (OAC) is one of the main therapeutic chronic treatments involving roughly 2% of the Italian population,Citation5 mainly recommended for the primary and secondary prevention of venous thromboembolism and stroke in patients with non-valvular atrial fibrillation (NVAF).Citation6 This population has been described as more vulnerable to possible severe COVID-19 complications, considering previous evidence describing their moderate level of HL and low treatment adherence to some clinical and socio-demographic features, such as high rates of elderly and frail patients.Citation5,Citation7,Citation8 For this reason, their vaccination against COVID-19 is a priority.Citation9 Furthermore, some studies regarding the influenza vaccination described that specific anticoagulated patients’ concerns about the vaccine administration route (i.e., intramuscular injection) and the possible administration-related clinical complications (e.g., muscular hematomas or the variability of time in therapeutic range) could undermine the vaccine acceptance.Citation10,Citation11 Therefore, optimizing the confidence of anticoagulated patients on vaccine acceptance is particularly strategic for achieving the success of the COVID-19 vaccine rollout.
PHE has been described as positively associated with well-being and health outcomes.Citation12 Although the role of PHE has been tested as a predictor for several health-related outcomes, Graffigna et al. demonstrated that PHE has a direct effect in determining lower rates of VH.Citation13 In accordance with this theoretical framework,Citation12 we made the hypothesis that promoting PHE might enhance the effect of HL in decreasing VH in a specific population of anticoagulated patients. Therefore, the involvement of patients in preventive behaviors (i.e., PHE) could optimize their capacity to find, understand, and use health services (i.e., HL). This knowledge may help healthcare professionals to adopt proactive and effective communication strategies to improve vaccine acceptance in the anticoagulated population. This study had two aims: first, to describe VH in people treated with OAC during the COVID-19 pandemic, before and after the availability of the COVID-19 vaccines in Italy; and, second, to assess the moderator role of PHE on the relation between HL and VH.
Materials and methods
Study design
We have conducted an interim analysis during the tail-end of the first Italian epidemic wave (June–August 2020) and the second wave (October 2020-March 2021). Data collection was done through a web-based survey to provide an epidemiological description of VH among the Italian anticoagulated population. The web-based survey targeted adult patients (age ≥ 18 years) on OAC who were willing to participate. A snowball sampling technique was adopted to obtain sufficient data to describe the phenomenon of VH in the population studied. The participants who answered the survey could invite other eligible people into OAC treatment from their network contacts, and no incentives were provided.
We used the SurveyMonkey® software for data collection, and only the principal investigator of the project (AM) had the faculty to monitor the response rate and consult the results. The generated survey link was broadcasted through the social websites most frequently questioned by the oral anticoagulated population in Italy. Following methodological indications,Citation14 an overall survey completeness rate higher than 40% was set out to ensure data reporting quality, considering that data were collected only via a digital internet-based source. The Checklist for Reporting Results of Internet E-Survey (CHERRIES) was used to ensure a complete description of the e-survey methodology (see Supplementary File 1).Citation15
Data collection and measures
The web-based survey was developed considering patients’ peculiarities in managing OAC described in the literature and their possible challenges during the COVID-19 pandemic to collect data in a sample during the first Italian epidemic wave (June–August 2020) and additional data in an independent sample during the second wave (October 2020–March 2021). To avoid response bias, participants could fill out the web-based survey only once, using their IP address. The form used for data collection was composed of two sections. The first section was related to the respondents’ socio-demographic and clinical profile (15 questions). The second section focused on specific questions about the patients’ challenges in managing OAC during the COVID-19 pandemic (seven questions); overall, the length of the survey was nine pages.
HL and PHE were measured through valid and reliable tools available in the Italian language. HL has been measured using the European Health Literacy Survey Questionnaire (HLS-EU-Q6).Citation16 The HLS-EU-Q6 is a self-reported tool composed of six items measuring the patients’ skills in finding, understanding, and judging health information on their health status. The difficulties perceived by patients in implementing specific HL skills were rated on a four-point Likert scale (1 = very difficult; 2 = fairly difficult; 3 = fairly easy; 4 = very easy). The final score has been computed through the mean of the values of each item. PHE has been measured using the PHE scale adapted for the specific pandemic condition.Citation17 The PHE scale is a self-reported tool composed of five ad-hoc items measuring patients’ psychological readiness to take an active role in their clinical condition in four main stages (i.e., blackout, arousal, adhesion, and eudaimonic project) and intermediate phases. The unachieved synergy among the different subjective dimensions at each stage of the process could undermine the patients’ ability to engage in their health. The final score has been computed through the median of the values of each item, ranging from 1 (low PHE) to 7 (high PHE). Finally, without the availability of a valid and reliable tool to assess VH for the Italian settings, it has been assessed through a single closed question: “If there was the availability of a vaccine against COVID-19, would you be in favour of vaccination?”; the response was based on a three-point Likert scale: 1 (no vaccine hesitancy), 2 (high vaccine hesitancy), 3 (unwilling or moderate vaccine hesitancy).
Data analysis
Descriptive statistics were adopted to assess the distribution of the measured variables. All missing data were managed by pairwise deletion for omitting cases based on the variables included in the analysis, and an alpha level equal to .05 was considered significant for all statistical tests. IBM SPSS Statistics version 24 and Mplus version 7.1 were used for the analysis.
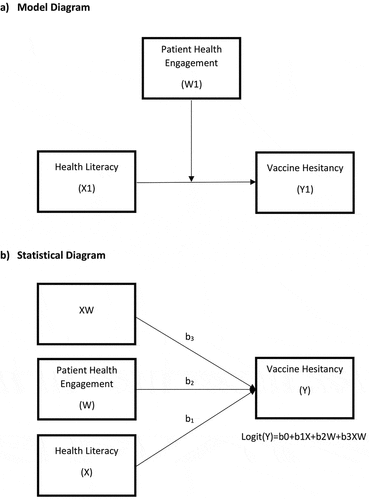
The framework of structural equation modeling was employed to assess the relation between HL (independent variable, X1) and VH (dependent variable, Y1), considering the possible moderator role of PHE (W1) on the same relation (). The weighted least squares (WLS) estimator was used to estimate the unknown parameters of the equation. Precisely, we have tested a basic moderation model with one dichotomous moderator (adequate PHE with values >5 versus inadequate PHE with values ≤5), a continuous independent variable (HL) and a dichotomous dependent variable (“hesitant and unwilling toward vaccination” versus “not hesitant”): logit(VH) = b0+ b1HL+b2PHE+b3HL*PHE; then, the equation could be synthesized as follows: logit(VH) = (b0+ b2PHE) + (b1+ b3PHE)HL. Slope analysis was conducted to interpret the conditional effects of the independent variable (HL) on VH at different PHE levels to facilitate the interpretation of the investigated moderating effects.
Ethical consideration
This study has been accepted by the Institutional Review Board of the promoter. All respondents carefully read the rationale and aim of the study on the welcome page of the survey before providing their consensus to proceed. Data has been managed according to the Italian privacy law (law 101/2018), ensuring the confidentiality and anonymity of the responses; proprietary survey software and local servers were used to ensure data protection.
Results
We enrolled 288 anticoagulated patients during the first and second waves of the COVID-19 pandemic, with an overall survey completeness rate higher than 50% and the mean time necessary to complete the questionnaire equal to 6 min. All sample characteristics are described in . Notably, the levels of HL and PHE were relatively medium-low, with values equal to 2.38-±5.18 and 4.49 ± 1.35, respectively. HL (t(164) = −1.68; p-value = 0,094) and PHE (t(164) = 1.25; p-value = 0.215) in the responders of the first and second waves did not differ. The cumulative VH (hesitant and unwilling toward vaccination) was present in 35.6% of the sample encompassing those who answered that they would not take any COVID-19 vaccines (11.6%) and those who reported important doubts on taking the vaccine (24%).
Table 1. Sample characteristics (n = 288)
In detail, the VH of participants (n = 184) who answered during the first pandemic wave in Italy (when vaccines against COVID-19 were not available) had a cumulative rate of 38.4% (highly hesitant participants = 14.5% and unwilling toward vaccination = 23.9%). VH of participants (n = 104) who answered during the second pandemic wave (when vaccines against COVID-19 were available) had a cumulative rate of 30.8% (highly hesitant participants = 6.6% and unwilling toward vaccination = 24.2%). The rates of VH between the two pandemic waves did not significantly differ (χ2(2) = 3.6; p-value = 0.164).
The rates of VH and adequate PHE in the overall sample and considering the subgroups of patients with high and low HL are described in , as well as stratifying results considering the answers in the first and second waves. The rates of VH did not differ between subgroups of patients with high and low health literacy in the overall sample (p-value = 0.501), in answers collected during the first waves (p-value = 0.708), and in the subsample collected during the second wave (p-value = 0.663). Conversely, the rates of adequate PHE differed between subgroups of patients with high and low health literacy in the overall sample (p-value = 0.001), in answers collected during the first waves (p-value = 0.007), and in the subsample collected during the second wave (p-value = 0.025).
Table 2. Vaccine hesitancy and patient health engagement in patients with low and high health literacy
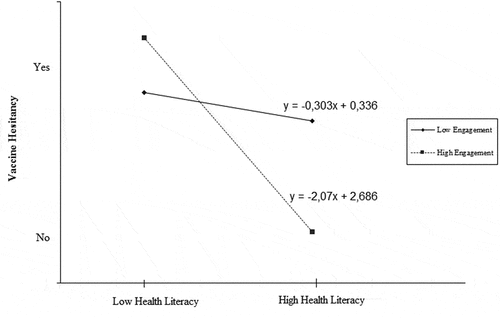
The employed model showed that the moderating effect of PHE in modulating the association between HL and VH [exp(b) = −.101; P < .001] was significant [exp(b) = −.589; P < .001]. Higher levels of HL were associated with lower rates of VH. As shows, the slope analysis employed to interpret the moderating effect of PHE on the association between HL and VH showed that higher levels of PHE (scores > 5 of the PHE scale) significantly enhanced the strength of the association between high HL and lower rates of VH. Precisely, the slope analysis for decomposing the moderating effect of PHE on the relationship from HL to VH provides two different scenarios (two different slopes): the first slope (continuous line) compared associations between HL and VH only in the subgroup with low PHE and within that group, patients with greater HL showed slightly lower VH (slight slope). The second comparison (the dashed line) focused on highlighting associations between HL and VH only in the subgroup with high PHE, and within that group, patients with greater HL showed lower VH with a substantial slope. The differences between slopes (gradient of slope = −0.6901; t-value of slope for high HL = −4.258; p-value of slope for high PHE < 0.001) suggested that PHE enhances the effects of HL on lowering VH levels.
Discussion
This study shows the key role of PHE in moderating the relationship between HL and VH: increasing patients’ engagement in vaccine campaigns is relevant in building up a true alliance between vaccine recipients and healthcare providers. Patients are not merely passive recipients of communication strategies, but they should be deeply involved as co-builders of interventions in public health, such as in a vaccination campaign.Citation18 The emerging results support the role of PHE and HL as determinants of VH in the anticoagulated population, as has been previously described in other populations.Citation19–22 This population could be more fearful of vaccination and potential vaccine-related effects, as they present limited levels of PHE and HL. In this scenario, a multi-professional management approach is fundamental to address the complexity of the VH phenomenon and fill organizational gaps that could undermine the implementation of educational interventions (such as lack of time, shortage of healthcare providers, and weak communication skills).
In the anticoagulated population, the level of VH was moderate during the first and second waves of the COVID-19 pandemic: the sample perception in the first sample during the first wave is not statistically different from the perception of the sample enrolled during the second wave, despite the availability of COVID-19 vaccines during the second pandemic wave. This fact suggests two considerations. The first consideration is given by the potential effects of infodemic in generating misconceptions and weak risk communication strategies adopted by healthcare providers and policymakers between the first and second epidemic waves in Italy that might have undermined vaccine acceptance despite the availability of vaccines.Citation18,Citation23,Citation24 The second consideration is the starting low levels of HL and PHE in the anticoagulated population.Citation22 The current infodemic related to the rare thromboembolic adverse events of the COVID-19 vaccines amplified the uncertainty toward vaccine safety, increasing the demand for unsuitable or unwarranted clinical investigations (e.g., genetic testing for thrombotic or bleeding disorders) both in the general population and in the population at risk.Citation25
Furthermore, the low literacy of patients in researching and using health information and engaging in the vaccination strategies may have undermined vaccine acceptance promptly. Overall, in Italy, the positive attitudes and beliefs toward vaccination could be considered under-optimal. For example, the flu vaccination coverage rate in the targeting population remains steadily low compared to the levels recommended by the national immunization prevention plan (PNPV) 2017–2019, and during the COVID-19 pandemic, the national-level trends of immunization uptake for other non-communicable diseases significantly decreased.Citation26
This study presents some limitations. Firstly, the number of participants involved in this interim analysis is low compared to the overall number of Italian patients treated with OAC; this result can be in part explained as an implicit limit of web-based survey approach available for internet users only. Second, the measurements were assessed using self-reported tools, and the socially desirable bias cannot be excluded from the answers. Third, the independent samples in the two time-points of the study suggest high caution in generalizing the results. Fourthly, the samples were not powered to be representative of the Italian patients in OAC and were based on a convenience approach; for these reasons, the inferential analyses have to be interpreted with caution.
Conclusion
PHE enhances the effects of HL in decreasing VH among patients treated with OAC. Considering that the described levels of PHE and HL were generally limited in this study, we suggest greater attention in implementing educational and communicative strategies for anticoagulated patients.
Supplemental Material
Download ()Acknowledgments
We wish to thank all the participants, patient associations, and scientific societies who supported the initiative, such as the Italian federation of anticoagulated patient associations (Feder-AIPA), Anticoagulazione.it, and the Italian association of adult congenital heart disease (AICCA).
Disclosure statement
No potential conflict of interest was reported by the author(s).
Supplementary material
Supplemental data for this article can be accessed on the publisher’s website at https://doi.org/10.1080/21645515.2021.1984123.
Additional information
Funding
References
- Graffigna G, Palamenghi L, Barello S, Stefania B. “Cultivating” acceptance of a COVID-19 vaccination program: lessons from Italy. Vaccine. 2020;38(48):7585–86. doi:10.1016/j.vaccine.2020.10.025.
- Graffigna G, Barello S, Bonanomi A, Cipresso P. The role of Patient Health Engagement model (PHE-model) in affecting patient activation and medication adherence: a structural equation model. PLoS One. 2017;12(6):e0179865. doi:10.1371/journal.pone.0179865.
- Batterham RW, Hawkins M, Collins PA, Buchbinder R, Osborne RH. Health literacy: applying current concepts to improve health services and reduce health inequalities. Public Health. 2016;132:3–12. doi:10.1016/j.puhe.2016.01.001.
- MacDonald NE, Eskola J, Liang X, Chaudhuri M, Dube E, Gellin B, Goldstein S, Larson H, Manzo ML, Reingold A, et al. Vaccine hesitancy: definition, scope and determinants. Vaccine. 2015;33:4161–64. doi:10.1016/j.vaccine.2015.04.036.
- Palareti G, Antonucci E, Migliaccio L, Erba N, Marongiu F, Pengo V, Poli D, Testa S, Tosetto A, Tripodi A, et al. Vitamin K antagonist therapy: changes in the treated populations and in management results in Italian anticoagulation clinics compared with those recorded 20 years ago. Intern Emerg Med. 2017;12(8):1109–19. doi:10.1007/s11739-017-1678-9.
- Hart RG, Pearce LA, Aguilar MI. Meta-analysis: antithrombotic therapy to prevent stroke in patients who have nonvalvular atrial fibrillation. Ann Intern Med. 2007;146(12):857–67. doi:10.7326/0003-4819-146-12-200706190-00007.
- Magon A, Arrigoni C, Moia M, Mancini M, Dellafiore F, Manara DF, Caruso R. Determinants of health-related quality of life: a cross-sectional investigation in physician-managed anticoagulated patients using Vitamin K antagonists. Health Qual Life Outcomes. 2020;18(1). doi:10.1186/s12955-020-01326-y.
- Palareti G, Antonucci E, Legnani C, Mastroiacovo D, Poli D, Prandoni P, Tosetto A, Pengo V, Testa S, Ageno W. Bleeding and thrombotic complications during treatment with direct oral anticoagulants or vitamin K antagonists in venous thromboembolic patients included in the prospective, observational START2-register. BMJ Open. 2020;10(11):e040449. doi:10.1136/bmjopen-2020-040449.
- SISET. Vaccinazioni anti covid-19 per pazienti con trombosi/trombofilia: indicazioni pratiche. Siset 2021. [accessed 2021 Aug 28]. https://www.siset.org/?option=com_content&view=article&id=339 .
- Poli D, Chiarugi L, Capanni M, Antonucci E, Abbate R, Gensini G, Prisco D. Need of more frequent international normalized ratio monitoring in elderly patients on long-term anticoagulant therapy after influenza vaccination. Blood Coagul Fibrinolysis. 2002;13(4):297–300. doi:10.1097/00001721-200206000-00004.
- Iorio AM, Camilloni B, Basileo M, Guercini F, Conti S, Ferrante F, Paccamiccio E, Iaboni S, Vecchioli M, Iorio A. Influenza vaccination in patients on long-term anticoagulant therapy. Vaccine. 2006;24(44–46):6624–28. doi:10.1016/j.vaccine.2006.05.036.
- Barello S, Palamenghi L, Graffigna G. The mediating role of the patient health engagement model on the relationship between patient perceived autonomy supportive healthcare climate and health literacy skills. Int J Environ Res Public Health. 2020;17(5):1–13. doi:10.3390/ijerph17051741.
- Graffigna G, Palamenghi L, Boccia S, Barello S. Relationship between citizens’ health engagement and intention to take the covid-19 vaccine in Italy: a mediation analysis. Vaccines. 2020;8(4):1–11. doi:10.3390/vaccines8040576.
- Kongsved SM, Basnov M, Holm-Christensen K, Hjollund NH. Response rate and completeness of questionnaires: a randomized study of internet versus paper-and-pencil versions. J Med Internet Res. 2007;9(3):e25. doi:10.2196/jmir.9.3.e25.
- Eysenbach G. Improving the quality of web surveys: the Checklist for Reporting Results of Internet E-Surveys (CHERRIES). J Med Internet Res. 2004;6(3):e34. doi:10.2196/jmir.6.3.e34.
- Lorini C, Lastrucci V, Mantwill S, Vettori V, Bonaccorsi G. Measuring health literacy in Italy: a validation study of the HLS-EU-Q16 and of the HLS-EU-Q6 in Italian language, conducted in florence and its surroundings. Ann Ist Super Sanità. 2019;55:10–18.
- Graffigna G, Barello S, Bonanomi A, Lozza E. Measuring patient engagement: development and psychometric properties of the Patient Health Engagement (PHE) scale. Front Psychol. 2015;6:274. doi:10.3389/fpsyg.2015.00274.
- Burgess RA, Osborne RH, Yongabi KA, Greenhalgh T, Gurdasani D, Kang G, Falade AG, Odone A, Busse R, Martin-Moreno JM, et al. The COVID-19 vaccines rush: participatory community engagement matters more than ever. Lancet. 2021;397(10268):8–10. doi:10.1016/S0140-6736(20)32642-8.
- Larson HJ, Clarke RM, Jarrett C, Eckersberger E, Levine Z, Schulz WS, Paterson P. Measuring trust in vaccination: a systematic review. Hum Vaccin Immunother. 2018;14(7):1609. doi:10.1080/21645515.2018.1459252.
- Reno C, Maietti E, Fantini MP, Savoia E, Manzoli L, Montalti M, Gori D. Enhancing COVID-19 vaccines acceptance: results from a survey on vaccine hesitancy in Northern Italy. Vaccines. 2021;9(4):378. doi:10.3390/vaccines9040378.
- Robertson E, Reeve KS, Niedzwiedz CL, Moore J, Blake M, Green M, Katikireddi SV, Benzeval MJ. Predictors of COVID-19 vaccine hesitancy in the UK household longitudinal study. Brain Behav Immun. 2021;94:50. doi:10.1016/j.bbi.2021.03.008.
- Turhan Z, Dilcen HY, Dolu İ. The mediating role of health literacy on the relationship between health care system distrust and vaccine hesitancy during COVID-19 pandemic. Curr Psychol. 2021;1–10.
- Biasio LR, Bonaccorsi G, Lorini C, Pecorelli S. Assessing COVID-19 vaccine literacy: a preliminary online survey. Human Vaccines & Immunotherapeutics. 2020;17:1304–12. doi:10.1080/2164551520201829315.
- Kricorian K, Civen R, Equils O. COVID-19 vaccine hesitancy: misinformation and perceptions of vaccine safety. Hum Vaccin Immunother. 2021;1–8. [accessed 2021 Aug 28]. https://www.tandfonline.com/doi/abs/10.1080/21645515.2021.1950504 .
- SISET SIGU Indicazioni sulla prescrizione di test genetici per trombofilia [Internet]; 2021. [accessed 2021 Aug 28]. http://www.siset.org/congressi/2-non-categorizzato/345-la-societa-italiana-per-lo-studio-emostasi-e-trombosi-siset-e-la-societa-italiana-di-genetica-umana-sigu-su-vaccinazione-per-covid-19-e-rischio-di-eventi-trombotici-indicazioni-sulla-prescrizione-di-t .
- SISET, SIGU. Indicazioni sulla prescrizione di test genetici per trombofilia. 2021. [accessed 2021 Aug 28]. http://www.siset.org/congressi/2-non-categorizzato/345-la-societa-italiana-per-lo-studio-emostasi-e-trombosi-siset-e-la-societa-italiana-di-genetica-umana-sigu-su-vaccinazione-per-covid-19-e-rischio-di-eventi-trombotici-indicazioni-sulla-prescrizione-di-t .