Abstract
Patients with leukemia are predisposed to various coagulation abnormalities. Thrombosis and bleeding continue to be a major cause of morbidity and mortality in leukemias. The pathophysiology of these disorders is unique, and not only the disease but also the treatment and other factors play a role. There has been an increase in the understanding of these disorders in leukemias. However, it is still difficult to predict when and which patients will have these complications. The evidence for the management of coagulation abnormalities in leukemias is still evolving and not as established as in solid malignancies. The management of these disorders is complex, and making clinical decisions is often challenging. In the era of specialization, where there are different hematologists looking after benign- and malignant-hematology patients, opinions of thrombosis experts are often sought by leukemia specialists. This review aims to bridge the gap in the knowledge of these disorders between these specialists.
Keywords:
Introduction
Coagulation disorders are common in leukemia patients. The incidence of thromboembolism (TE) in hematologic malignancies (including lymphoma and myeloma) stands at 4% per year. This is the fourth most common cause after pancreatic (11%), brain (8%), and lung cancers (4.4%).Citation1 The incidence of bleeding is the highest of all malignancies by virtue of the disease-related thrombocytopenia itself. Coagulation disorders seen in lymphoma, myeloma, and other solid malignancies are beyond the scope of this review. The reader may refer to excellent reviews and guidelines on these topics.Citation2,Citation3 For the purpose of simplicity, we deal with each leukemia type with a case vignette, followed by epidemiology, pathophysiology, and management issues. All patients provided written informed consent for their case details to be published.
Coagulation disorders in acute lymphoblastic leukemia Case vignette
GK, a 39-year-old woman diagnosed with pre-B-cell acute lymphoblastic leukemia (ALL), standard risk was started on the Berlin–Frankfurt–Münster (BFM)-90 protocol. Her blood counts at presentation were hemoglobin 45 g/L, platelets 18×109/L, and white-cell count 1.2×109/L. She received native Escherichia coli l-asparaginase as part of the induction therapy. In the fourth week after completion of the l-asparaginase course, she presented with generalized tonic–clonic seizures and right-sided hemiparesis. Computed tomography suggested bifrontal hemorrhage. Magnetic resonance venography of brain confirmed superior sagittal sinus thrombosis. Her blood counts were hemoglobin 80 g/L, platelets 85×109/L, and white-cell count 2.8×109/L. Her fibrinogen levels were normal throughout the course of l-asparaginase. She was started on a therapeutic dose of low-molecular-weight heparin (LMWH). LMWH was dose-modified for thrombocytopenia during the intensive phase. She was not rechallenged with l-asparaginase during the reinduction phase. She remains in complete remission, with minimal residual disease negative at end of induction. LMWH was continued for 6 months. Her focal neurological deficit recovered, and she had no recurrence of thrombosis.
Epidemiology
The reported incidence of TE in childhood ALL varies from 1.1% to 36.7%.Citation4 This wide variation is due to differences in TE diagnosis and treatment protocols. This incidence is even higher in adolescent and young adult (34%) and adult patients (43%) on l-asparaginase.Citation5 The commonest sites for TE are central nervous system (CNS; 50%) and deep vein thrombosis (43%). The overall mortality of TE in ALL varies from 0 to 4.8%.Citation4 On the contrary, deaths due to bleeding in ALL are less common than in acute myeloid leukemia (AML).Citation6
Pathophysiology
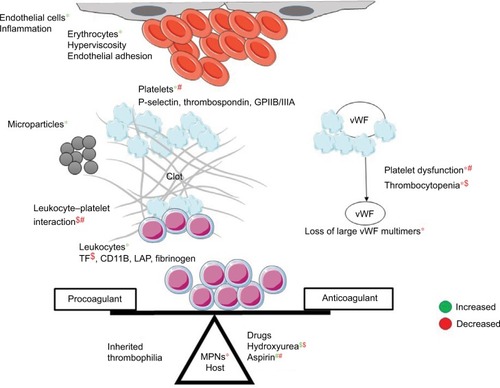
The clinical presentation of TE or bleeding is an outcome of the delicate balance between procoagulant and anticoagulant forces at play in a patient (). There are several studies showing increased thrombin generation shown by thrombin–antithrombin (AT) complexes at diagnosis and in initial therapy for ALL. Factor VIII, von Willebrand factor (vWF), and fibrinogen are positive acute phase reactants.Citation7 Besides this, ALL cells also express cancer procoagulant (CP).Citation8 CP activates factor X directly, independently of factor VII.Citation9 Disseminated intravascular coagulation (DIC) is underrecognized in ALL, with prevalence of around 14% at diagnosis and doubling to 27% during induction therapy.Citation10
Figure 1 Balance between procoagulant and anticoagulant forces in ALL and interactions among host, disease, and treatment related factors.
Abbreviations: ALL, acute lymphoblastic leukemia; CVC, central venous catheter; TFPI, tissue-factor pathway inhibitor; vWF, von Willebrand factor; AT, antithrombin; TM, thrombomodulin; FDPs, fibrin-degradation products.
Chemotherapy in ALL augments the thrombogenic potential. Of these, l-asparaginase, which depletes the ALL cells of the essential amino acid asparagine, also ends up depleting the procoagulant (fibrinogen, factors V, VII, VIII, IX, X, and XI) and anticoagulant (AT, plasminogen, protein C/S) proteins. l-Asparaginase may in fact cause a prothrombotic state, as it reverses the procoagulant proteins earlier than anticoagulant proteins.Citation11 E. coli asparaginase, which is more potent than Erwinia asparaginase, has more effect on the coagulation parameters.Citation12 Steroids add to the prothrombotic state by increasing plasma levels of prothrombin, factor VIII/vWF, and PAI1 and decreasing plasminogen and fibrinogen.Citation13 Dexamethasone may be associated with less risk of TE than prednisone.Citation14 Central venous lines are the other reason for TE, with incidence as high as 30%, depending on the technique and site of insertion.Citation15 A variable 18%–40% of cases may have inherited thrombophilia.Citation16 Use of granulocyte/granulocyte-monocyte colony-stimulating factors during episodes of neutropenia is also associated with thrombosis at an incidence of 1.2% and 4.2%, respectively. This is through increased tissue-factor (TF) and factor-VIII levels.Citation17 T-cell ALL patients are at higher risk of both TE and hemorrhagic complications, due to hyperleukocytosis.Citation18 Thrombocytopenia – at diagnosis or therapy-related – is one of the major factors contributing to bleeding in ALL. Infections can tilt the balance either way of systemic inflammatory response syndrome or consumptive coagulopathy.
Investigations
Recommended tests include activated partial thromboplastin time (aPTT), international normalized ratio (INR), and fibrinogen levels (AT optional) prior to, during native asparaginase dosing, and 1 week after polyethylene glycol–asparaginase therapy. For prevention of TE, research using AT prophylaxis have shown reduced incidence of TE, but this was not powered for efficacy, and hence the role of AT replacement remains inconclusive.Citation19 Though prophylactic fresh frozen plasma/cryoprecipitate to replace AT is associated with no CNS TE events, neither it nor LMWH lower the incidence of TE on l-asparaginase.Citation20,Citation21 Some centers use both anticoagulation and AT replacement for AT levels <60%.Citation22 At our center, we give cryoprecipitate for fibrinogen <100 mg/dL.
Treatment
Development of TE while on l-asparaginase used to lead to discontinuation of asparaginase in up to 75% patients, which led to inferior event-free survival outcomes.Citation23,Citation24 However, with current strategies of rechallenging asparaginase and continued anticoagulation, outcomes have been similar.Citation5 Current expert recommendations are to discontinue asparaginase only for CTCAE (Common Terminology Criteria for Adverse Events) grade 4 CNS thrombosis or bleed. For all grade 3 events and grade 4 non-CNS events, asparaginase needs to be withheld till resolution of clinical signs and either anticoagulation or coagulant therapy is stable. Asparaginase may be resumed at lower doses and/or longer intervals. Asparaginase need not be withheld for asymptomatic lab abnormalities.Citation25 As regards prophylactic platelet transfusions, the restrictive strategy with the standard trigger set at 10×109/L has remained unchanged over the past decade.Citation26
There have been no prospective randomized control trials on anticoagulant choice, dose, and duration in patients with leukemia. Most recommendations have been derived from extrapolation from studies done in patients with solid-organ malignancies. These guidelines endorse the use of LMWH as first-line therapy during the first 3–6 months after the diagnosis of malignancy-associated venous TE (VTE) based on the 2003 CLOT study.Citation27–Citation30 There have been recent expert recommendations on managing thrombosis in the setting of leukemia with thrombocytopenia.Citation31–Citation33 The consensus for anticoagulation dose modification in the setting of thrombocytopenia is as given in and . For catheter-related VTE, recommendations are to keep the catheter and continue anticoagulation till the catheter is in place or at least 3 months, whichever is longer. Catheter removal is only required if the device is dysfunctional, infected, or not required. For non-catheter-related TE, anticoagulation is recommended for at least 6 months and indefinitely for active malignancy or persistence of risk factors for recurrence.Citation3 The decision to stop anticoagulation beyond 6 months in patients under treatment of a malignancy that is in complete remission is unclear. This is on a case-by-case basis after taking the risk:benefit ratio into consideration. To summarize, in this case, the patient had a grade 4 CNS vascular event on l-asparaginase, despite normal fibrinogen levels. She was managed with dose-modified anticoagulation as mentioned, and not re-challenged with l-asparaginase.
Table 1 Acute thrombosis (0–30 days after diagnosis of VTE)
Table 2 Chronic thrombosis (>30 days after diagnosis of VTE)
Coagulation disorders in acute myeloid leukemia
Case vignette
RM, a 28-year-old lady, presented with a 4-day history of gangrenous changes in both hands (left > right) and feet. On clinical examination, she had absent ulnar, dorsalis pedis, and posterior tibial artery pulse bilaterally. Her investigations revealed hemoglobin 63 g/L, platelets 39×109/L, and white cell count 33.2×109/L with 85% blasts + promyelocytes. Her coagulogram showed PT 20 seconds, control 14 seconds, INR 1.4, aPTT 31 seconds, control 25–32 seconds, and elevated d-dimer and fibrin-degradation products. Her fibrinogen levels were normal, however. She was started on treatment with all-trans retinoic acid (ATRA) and arsenic on suspicion of acute promyelocytic leukemia (APML) and DIC. This is the first line at our center, even in high-risk APML.Citation34 She was given prophylactic steroids plus hydroxyurea to prevent differentiation syndrome. Computed tomography angiography confirmed the presence of arterial thrombosis in the distal ulnar and posterior tibial arteries. This is a rare presentation of APML, but included here to emphasize the management issues in this case. Given her state of established gangrene with line of demarcation and DIC, she could not be started on any vascular intervention or anticoagulation/antiplatelets. ATRA + arsenic and platelet support was continued. She attained complete remission at the end of 4 weeks. She underwent bilateral below-knee amputation with left phalangeal disarticulation for her dry gangrene 6 months later. She continues to be in remission 4 years later. This outcome is similar to what has been described in case reports.Citation35
Epidemiology
Most cases of AML-M3/APML have DIC at diagnosis. The incidence of DIC in AML-non-M3 is 10%–50%, depending upon the subtype of leukemia and diagnostic criteria for DIC.Citation36,Citation37 The incidence of thrombosis in AML-non-M3 and APML at diagnosis is 3.2% and 9.6%, respectively. The same at follow-up is 1.7%–8.5% and 8.4%–11% respectively.Citation38,Citation39 In APML, most cases occur before or during induction therapy with ATRA. Arterial events are commoner than venous events. Thrombosis and severe hemorrhage co-occur in 15% of cases.Citation40 The incidence of isolated severe bleeding remains high in APML – around 21%. The case-fatality rate of these episodes can be as high as 50%. The incidence of early-death rates in APML has remained unchanged over the years: at 5%–10%, even in the ATRA era.Citation41 The incidence of thrombosis in APML at our center is 7.4% (n=136), with equal numbers of arterial and venous TE. The incidence of severe bleeds is 28%, with the early-death rate due to bleeding being 7.4% (Varma et al, unpublished data). Predictors of thrombosis include elevated white-cell count, Bcr3 isoform, FLT3 internal tandem duplication, and expression of CD2 and CD15 on promyelocytes.Citation42 Though not a coagulation defect in principle, hyperleukocytosis can be seen in AML when the white-cell count is >100×109/L. This leads to leukostasis and vascular occlusion in any vital organ.Citation43
Pathophysiology
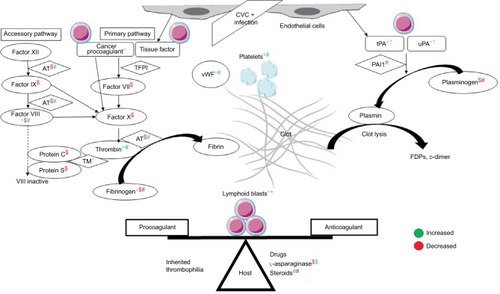
The DIC seen in APML is a double-edged sword for thrombosis and bleeding (). Procoagulant forces are CP expressed on leukemic promyelocytes.Citation44 TF from endothelial cells is exposed by cytokines (IL1 and TNFα) released from apoptotic leukemic cells.Citation45–Citation47 TF is the site of activation of factor VII. TF-expressing microparticles in APML have pro-coagulant activity.Citation48 Anticoagulant forces are elevated uPA and tPA and low PAI1.Citation49,Citation50 Leukemic promyelocytes express annexin II, which accelerates the conversion of plasminogen to plasmin and thus causes primary fibrinolysis.Citation51 Cerebral endothelial cells also express this annexin II, which explains the high incidence of intracerebral bleeds seen in APML.Citation52 Emerging evidence points to podoplanin expression on leukemic promyelocytes causing platelet aggregation as a novel mechanism for bleeding.Citation53 The role of proteases like elastase and chymotrypsin released from leukemic promyelocytes on fibrinolysis, if any, is minor.Citation54 ATRA can reverse these changes through various mechanisms of reduced expression of TF, CP, and annexin II and counteracting the effect of cyto-kines.Citation55 ATRA may in fact tilt the balance to a prothrombotic state, as it reverses the procoagulant proteins earlier than anticoagulant proteins, similar to l-asparaginase.Citation56 A novel cell-death pathway termed “ETosis” has been described recently in APML blasts treated with ATRA. This process releases intact chromatin in the extracellular space. This extracellular chromatin has multifold effects of increasing thrombin and plasmin generation and causes fibrinolysis resistance and endothelial activation.Citation57
Figure 2 Pathophysiology of disseminated intravascular coagulation in APML and the role of ATRA in counteracting it.
Abbreviations: APML, acute promyelocytic leukemia; ATRA, all-trans retinoic acid; CVC, central venous catheter; TFPI, tissue-factor pathway inhibitor; TF-MPs; TF-expressing microparticles; vWF, von Willebrand factor; AT, antithrombin; TM, thrombomodulin; FDPs, fibrin-degradation products.
Investigations
Routine coagulation tests may reveal overt DIC with prolongation of PT, variable aPTT, low fibrinogen levels and platelet counts, and elevated d-dimer and fibrin-degradation products.Citation58 However, these variables do not correlate well with the severity of bleeding or thrombosis.Citation41 No single test can confirm or rule out DIC. The International Society on Thrombosis and Haemostasis overt DIC score may miss subclinical DIC in acute leukemia.Citation10 A recent study showed that a high d-dimer level >4 mg/L was most predictive for thrombosis in AML-non-M3 patients.Citation59 Other tests of activated clotting like prothrombin fragment 1+2, thrombin–AT complex, and fibrinopeptide A may be helpful, but are not routinely available. Elevated white-cell count (>20×109/L) is an independent predictor of early hemorrhagic death in APL.Citation60
Treatment
Both ATRA and arsenic trioxide (ATO) can reverse the coagulopathy of APML within 4–11 days. This underscores the importance of starting ATRA in the emergency department whenever a diagnosis of APML is suspected. The incidence of thrombosis in the ATRA era is higher than in the pre-ATRA era.Citation40 However, the incidence of TE in ATRA + ATO is lower than in ATRA + chemotherapy in non-high-risk APML patients.Citation61 European Leukemia Net guidelines recommend fresh frozen plasma, fibrinogen, and/or cryoprecipitate to maintain the fibrinogen concentration above 100–150 mg/dL. In APML, the platelet-transfusion threshold is more liberal, and the aim is to maintain a count >30–50×109/L. The role of heparin, tranexamic acid, or other anticoagulant or antifibrinolytic therapy is unclear and not recommended as part of routine practice.Citation62 On the contrary, combining ATRA with tranexamic acid may lead to fatal thromboembolism.Citation63 There is insufficient evidence to recommend thrombopoietin mimetics, recombinant factor VIIa, antifibrinolytics, desmopressin, activated protein C, or recombinant human soluble thrombomodulin to prevent or treat bleeding in hematological malignancies.Citation64–Citation66 The role of leukapheresis in hyperleukocytosis to prevent early mortality is also unclear; in fact, it may lower platelet counts and fibrinogen and prolong prothrombin time.Citation67,Citation68 Early cytoreductive chemotherapy and supportive care with platelets, fresh frozen plasma, cryoprecipitate, or fibrinogen concentrates are the only recommended measures to prevent or treat bleeding associated with DIC in AML.Citation69 In summary, the patient had APML with DIC manifesting as acute arterial thrombosis of the extremities. She was managed with ATRA + ATO and supportive transfusions without anticoagulation. She survived the leukemia, but lost her limbs to gangrene.
Coagulation disorders in myeloproliferative neoplasms
Case vignette
MS, a 19-year-old man, presented with a 1-month history of abdominal pain. He had a massive splenomegaly with thrombosis of the splenoportal axis. His blood counts at presentation were hemoglobin 108 g/L, platelets 668×109/L, and white cells 5.6×109/L, with a normal differential count. His bone marrow suggested a diagnosis of essential thrombocytosis (ET). His JAK2V617F-mutation status was positive. The final diagnosis was high-risk ET with splanchnic vessel thrombosis. On upper gastrointestinal endoscopy, he had no esophageal varices, but had multiple small gastric varices at diagnosis. He was given LMWH and bridged to warfarin titrated to an INR of 2–3. Aspirin was withheld, due to gastric varices. He was also started on hydroxyurea 500 mg orally twice a day titrated to a normal platelet count. He had an episode of hematemesis a year later, requiring interruption of warfarin and glue injection of the gastric varices. Given the risk of gastric variceal bleeding with aspirin, and considering the risk:benefit ratio of anticoagulation, he was restarted on warfarin. The plan is to continue indefinite anticoagulation, with periodic upper gastrointestinal endoscopy for varices.
Epidemiology
Of the chronic myeloproliferative neoplasms (MPNs), polycythemia vera (PV), ET, and primary myelofibrosis (PMF) are most associated with thrombosis and bleeding. The prevalence of TE at the time of diagnosis in PV, ET, PMF is 4%–11%, 2%–8%, and 3%–7%, respectively. The incidence of TE thereafter is 2%, 0.6%, and 0.6% per year, respectively.Citation70 Arterial thrombosis (70%) is more common than venous TE (30%). MPNs are also the etiology in abdominal splanchnic vessel thrombosis (extra- + intrahepatic veins leading to Budd–Chiari syndrome [BCS], portal vein thrombosis, and mesenteric vein thrombosis). The prevalence of latent or manifest MPNs is 40% in BCS and 30% in portal vein thrombosis. JAK2V617F mutation without manifest MPNs is seen in 17.1% of BCS and 15.4% of portal vein thrombosis.Citation71 In chronic myeloid leukemia (CML), tyrosine-kinase inhibitors increase the risk of arterial (4.78%) and venous (0.72%) TE. The risk is higher with newer tyrosine-kinase inhibitors (0.96%) than imatinib (0.27%).Citation72 In contrast to thrombosis, serious bleeding occurs in 5.5% of MPN patients.Citation73 The incidence of dasatinib-induced platelet dysfunction leading to serious bleeding in CML patients is 7%.Citation74 The incidence of thrombosis in PV at our center is 25%, with equal numbers of arterial and venous events.Citation75 The incidence of thrombosis and bleeding in ET at our center is 33.3% and 8.3%, respectively. A quarter of thrombotic events are arterial (Varma et al, unpublished data).
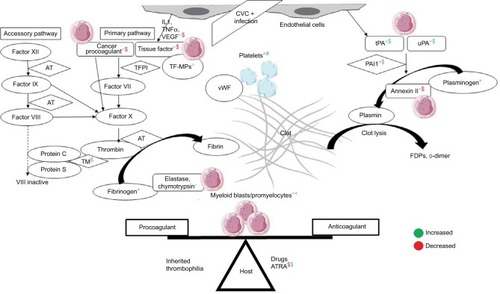
Pathophysiology
The mechanism of thrombosis in MPNs is multifactorial (). Besides thrombocytosis, platelets aggregate due to upregulation of p-selectin, thrombospondin and GPIIB/IIIA receptors.Citation76 Besides leukocytosis, activated leukocytes form aggregates with platelets.Citation77,Citation78 Erythrocytosis causes hyperviscosity; erythrocytes also show increased adherence to vascular endothelia.Citation79 Other mechanisms of thrombosis include microparticles and inflammation-mediated activation of endothelia.Citation80,Citation81 Using novel gene-expression meta-analysis, certain coagulation-related genes have been identified to be associated with thrombosis in MPN. These include IGF2R, PROS1, SELPLG, and ITGB2.Citation82 The etiology of bleeding in MPN is multifactorial. Acquired von Willebrand syndrome is seen in patients with platelet counts >10×109/L.Citation83 At these high counts, vWF binds to platelets and undergoes proteolysis with a resultant depletion of large multimers.Citation84 Besides this, there is evidence of platelet dysfunction in ET.Citation85 Other reasons for bleeding include treatment for disease and TE, thrombocytopenia due to disease progression, hypersplenism, liver dysfunction, and acquired hemophilia.Citation86
Investigations
Acquired von Willebrand syndrome should be ruled out in all patients with platelet counts >10×109/L before starting these patients on aspirin. Diagnosis of acquired von Willebrand syndrome involves showing a reduced function:antigen ratio (vWF:Act/Ag, vWF:Act or ristocetin-cofactor assay<30%) and loss of high-von Willebrand multimers.Citation87
Treatment
Risk factors for recurrent thrombosis in PV and ET are age >60 years, history of thrombosis, JAK2/MPL-mutation status, JAK2-allele burden, and cardiovascular (tobacco use, hypertension or diabetes mellitus, leukocytosis >11×109/L) in ET.Citation88 The goal of treatment in PV/ET is to prevent thrombohemorrhagic complications. Phlebotomy to achieve a hematocrit level <45% is standard treatment in all PV patients.Citation89 All low-risk PV and ET patients, except those with acquired von Willebrand syndrome, should get low-dose aspirin (40–100 mg/day). For high-risk PV or ET patients, hydroxyurea is recommended to target a platelet count in the normal range. All these measures reduce the risk of vascular events, including thrombosis and bleeding.Citation90 Anagrelide is falling out of favor, due to its increased risk of arterial thrombosis and major bleeding.Citation91 The requirement of phlebotomy on hydroxyurea correlates with the risk of thrombosis in PV patients.Citation92 Both aspirin and hydroxyurea reduce platelet–leukocyte complex formation and downregulation of leukocyte TF expression by hydroxyurea.Citation78,Citation93 Ruxolitinib, a JAK2 inhibitor, is approved to treat MF and hydroxyurea-intolerant PV. It causes thrombocytopenia in 68% of patients and grade 3–4 thrombocytopenia in 13% of patients.Citation94 A meta-analysis has shown that ruxolitinib reduces the risk of both arterial and venous thrombosis in PV and PMF patients. This is believed to be due to inhibition of JAK-mediated inflammation by ruxolitinib.Citation95
As regards treatment of VTE events, standard LMWH and vitamin K antagonists (VKAs) are used. The risk:benefit ratio of bleeding versus recurrent thrombosis needs to considered on a case-by-case basis. The combination of LMWH/VKAs and aspirin increases the risk of bleeding to 2.8% per patient-year.Citation73 The decision to stop anticoagulant therapy at 3–6 months is influenced by the preferences of an informed patient and risk of thrombosis. Recurrent VTE/cerebral or hepatic vein thrombosis, life-threatening VTE, and progressive MPNs uncontrolled with cytoreductive therapy would require indefinite treatment.Citation96 Because the risk of recurrent thrombosis is doubled on stopping anticoagulation and the risk of bleeding on VKA is the same as the non-MPN population, secondary prophylaxis should be continued for an indefinite period.Citation97 Aspirin should be continued in patients stopping anticoagulation. There are sparse data on the use of direct oral anticoagulants in hematological malignancies. These show no significant risk reduction in major bleeding compared to LMWH.Citation98 However, there are ongoing randomized trials addressing this issue.Citation99 If their use is considered, attention must be given to interactions with drugs used for treatment of the underlying disease ().Citation100 To summarize, the young patient had high-risk JAK2 + ET and splenoportal vein thrombosis. He was managed with hydroxyurea and VKAs. He could not be given aspirin, due to the presence of gastric varices. He will need indefinite anticoagulation, given the risk of recurrent thrombosis in this population.
Table 3 Drug interactions between DOACs and TKIs
Coagulation disorders in chronic lymphocytic leukemia
Case vignette
HK, a 62-year-old lady, with known chronic lymphocytic leukemia (CLL) with 11q deletion and unmutated IGHV after early relapse on bendamustine–rituximab, was started on ibrutinib 420 mg daily for bulky lymphadenopathy in April 2016. Her complete blood counts at baseline were hemoglobin 100 g/L, platelets 79×109/L, and absolute lymphocyte count 231×109/L. Her baseline coagulogram was normal (PT 15 seconds, INR 1.2, aPTT 32 seconds, control 32 seconds). Within 2 weeks, her absolute lymphocyte count had risen to 412×109/L and platelets had dropped to 44×109/L. She had gum bleeding with a spontaneous hematoma of 10×15 cm in her left gluteal region. HK had grade 1 thrombocytopenia at baseline. She developed grade 3 thrombocytopenia with major but non-life-threatening bleeding. Her repeat coagulogram was normal (PT 14 seconds, control 14 seconds, INR 1, aPTT 31 seconds, control 32 seconds). This drop in platelet counts was due to ibrutinib, and was held till the resolution of hematoma and platelet count >50×109/L. Ibrutinib was restarted at the same dose. There was no recurrence of bleeding. At 1-year follow-up, her platelet count is up to 100×109/L.
Epidemiology
The incidence of at least one episode of severe bleeding in CLL is reported to be as high as 18%.Citation101 This is often seen with autoimmune or disease-related thrombocytopenia. Acquired hemophilia with inhibitors to factor VIII are rare causes of bleeding.Citation102 Bleeding assumes much more importance in the era of ibrutinib. While early studies showed major bleeding episodes occurred in 9% and 4% of CLL patients on anticoagulants and antiplatelets, later studies have this incidence at 2% and 1%, respectively.Citation103,Citation104 CLL has not been associated with a high incidence of thrombosis. However, recent studies have shown incidence rates may be as high as other leukemias – 5%–11%.Citation105,Citation106 The risk factors for VTE is these studies were age >60 years, advanced stage of CLL, CLL treatment, and inherited thrombophilia.
Pathophysiology
At baseline, CLL patients have impaired platelet function assessed by platelet-function assay using epinephrine and adenosine diphosphate. Collagen-induced platelet aggregation is further impaired on initiating ibrutinib. Though factor VIII and vWF levels are elevated at baseline in most patients, their levels decline with ibrutinib. Low levels of factor VIII, vWF, and epinephrine-closure time on platelet-function assay predict bleeding in patients taking ibrutinib. There is no difference in platelet counts in patients who do and do not bleed. Bleeding risk decreases over time.Citation107
Investigations
Recommended tests include PT, aPTT, INR, and platelet counts at baseline. Bone-marrow examination should be done at baseline in thrombocytopenic patients to confirm or rule out a diagnosis of autoimmune thrombocytopenia. PT, aPTT, INR, and platelet counts should be repeated whenever there is clinical bleeding. Platelet counts should be repeated before each monthly cycle.
Treatment
Patients need to be told to report any bleeding episodes and hold ibrutinib for any medical or dental procedures. Ibrutinib needs to be held for at least 3–7 days pre- and postsurgery, depending upon the surgery and risk of bleeding.Citation108 While there are no guidelines to hold ibrutinib if thrombocytopenia is due to disease, ibrutinib may be held for drug-related grade 4 thrombocytopenia (<25×109/L) or grade 3 thrombocytopenia (<50×109/L) with bleeding. It is restarted when platelet count rises to ≥50×109/L.Citation109 Treatment of idiopathic thrombocytopenic purpura, disease-related thrombocytopenia, and acquired hemophilia involves steroids or immunosuppression to treat underlying CLL. Anticoagulation is required in 5%–10% of patients on ibrutinib who develop atrial fibrillation.Citation110 Using direct oral anticoagulants in this setting needs interactions with ibrutinib to be taken in to consideration ().Citation111 Patients on concurrent anticoagulants or anti-platelets should be watched for bleeding.Citation112 The CLL patient mentioned in the vignette had grade 4 thrombocytopenia with non-life-threatening bleeding on ibrutinib. This mandated holding ibrutinib till platelet recovery. Subsequently, her platelet counts rose to >100×109/L, as has been suggested to happen in 68% of patients on ibrutinib by 6 months.Citation107
Conclusion
In summary, coagulation disorders are common in leukemia. Thrombosis is as common as in solid malignancies. It is difficult to predict which patients will have bleeding and/or thrombosis. We need better predictors and coagulation tests to identify such patients. More research with prospective randomized control studies is needed on the role of novel oral anticoagulants, anticoagulant choice, dosing, and duration in hematologic malignancies.
Acknowledgments
The authors acknowledge the assistance of Dr Pankaj Malhotra, Dr Parathan Karunakaran, and Dr Ram Nampoothiri in providing the data related to the clinical vignettes and institutional data on coagulation disorders in leukemia patients.
Disclosure
The authors report no conflicts of interest in this work.
References
- HorstedFWestJGraingeMJRisk of venous thromboembolism in patients with cancer: a systematic review and meta-analysisPLoS Med201297e100127522859911
- LymanGHBohlkeKKhoranaAAVenous thromboembolism prophylaxis and treatment in patients with cancer: American Society of Clinical Oncology clinical practice guideline update 2014J Clin Oncol201533665465625605844
- National Comprehensive Cancer NetworkCancer-associated venous thromboembolic disease: version 1.2016 Available from: https://www.nccn.org/professionals/physician_gls/pdf/vte.pdfAccessed June 1, 2017
- AthaleUHChanAKThrombosis in children with acute lymphoblastic leukemia – part I: epidemiology of thrombosis in children with acute lymphoblastic leukemiaThromb Res2003111312513114678808
- GraceRFDahlbergSENeubergDThe frequency and management of asparaginase-related thrombosis in paediatric and adult patients with acute lymphoblastic leukaemia treated on Dana-Farber Cancer Institute consortium protocolsBr J Haematol2011152445245921210774
- AthaleUHChanAKHemorrhagic complications in pediatric hematologic malignanciesSemin Thromb Hemost200733440841517525898
- AthaleUHChanAKThrombosis in children with acute lymphoblastic leukemia – part II: pathogenesis of thrombosis in children with acute lymphoblastic leukemia – effects of the disease and therapyThromb Res200311145199212
- AlessioMGFalangaAConsonniRCancer procoagulant in acute lymphoblastic leukemiaEur J Haematol199045278812209822
- GordonSGFranksJJLewisBCancer procoagulant A: a factor X activating procoagulant from malignant tissueThromb Res197562127137234638
- DixitAChatterjeeTMishraPDisseminated intravascular coagulation in acute leukemia at presentation and during induction therapyClin Appl Thromb Hemost200713329229817636191
- ZakarijaAKwaanHCAdverse effects on hemostatic function of drugs used in hematologic malignanciesSemin Thromb Hemost200733435536417525893
- DuvalMSuciuSFersterAComparison of Escherichia coli- asparaginase with Erwinia-asparaginase in the treatment of childhood lymphoid malignancies: results of a randomized European Organisation for Research and Treatment of Cancer – Children’s Leukemia Group phase 3 trialBlood20029982734273911929760
- IsacsonSEffect of prednisolone on the coagulation and fibrinolytic systemsScand J Haematol1970732122165447966
- Nowak-GöttlUAhlkeEFleischhackGThromboembolic events in children with acute lymphoblastic leukemia (BFM protocols): prednisone versus dexamethasone administrationBlood200310172529253312517808
- MaleCChaitPAndrewMHannaKJulianJMitchellLCentral venous line-related thrombosis in children: association with central venous line location and insertion techniqueBlood2003101114273427812560228
- AthaleUHChanAKThrombosis in children with acute lymphoblastic leukemia – part III: pathogenesis of thrombosis in children with acute lymphoblastic leukemia – effects of host environmentThromb Res2003111632132714698648
- BarbuiTFinazziGGrassiAMarchioliRThrombosis in cancer patients treated with hematopoietic growth factors: a meta-analysisThromb Haemost19967523683718815592
- GiordanoPDel VecchioGCSantoroNThrombin generation in children with acute lymphoblastic leukemia: effect of leukemia immunophenotypic subgroupsPediatr Hematol Oncol200017866767211127398
- MitchellLGAndrewMHannaKA prospective cohort study determining the prevalence of thrombotic events in children with acute lymphoblastic leukemia and a central venous line who are treated with l-asparaginase: results of the Prophylactic Antithrombin Replacement in Kids with Acute Lymphoblastic Leukemia Treated with Asparaginase (PARKAA) studyCancer200397250851612518376
- LauwMNvan der HoltBMiddeldorpSMeijersJCCornelissenJJBiemondBJVenous thromboembolism in adults treated for acute lymphoblastic leukaemia: effect of fresh frozen plasma supplementationThromb Haemost2013109463364223364346
- SibaiHSekiJTWangTQVenous thromboembolism prevention during asparaginase-based therapy for acute lymphoblastic leukemiaCurr Oncol2016234e355e36127536184
- Hunault-BergerMChevallierPDelainMChanges in anti-thrombin and fibrinogen levels during induction chemotherapy with l-asparaginase in adult patients with acute lymphoblastic leukemia or lymphoblastic lymphoma: use of supportive coagulation therapy and clinical outcome – the CAPELAL studyHaematologica200893101488149418728028
- SilvermanLBGelberRDDaltonVKImproved outcome for children with acute lymphoblastic leukemia: results of Dana-Farber consortium protocol 91–01Blood20019751211121811222362
- OttNRamsayNKPriestJRSequelae of thrombotic or hemorrhagic complications following L-asparaginase therapy for childhood lymphoblastic leukemiaAm J Pediatr Hematol Oncol19881031911953177809
- StockWDouerDDeAngeloDJPrevention and management of asparaginase/pegasparaginase-associated toxicities in adults and older adolescents: recommendations of an expert panelLeuk Lymphoma201152122237225321827361
- SchifferCAAndersonKCBennettCLPlatelet transfusion for patients with cancer: clinical practice guidelines of the American Society of Clinical OncologyJ Clin Oncol20011951519153811230498
- LymanGHKhoranaAAFalangaAAmerican Society of Clinical Oncology guideline: recommendations for venous thromboembolism prophylaxis and treatment in patients with cancerJ Clin Oncol200725345490550517968019
- KearonCAklEAComerotaAJAntithrombotic therapy for VTE disease: Antithrombotic Therapy and Prevention of Thrombosis, 9th ed – American College of Chest Physicians evidence-based clinical practice guidelinesChest20121412 Supple419Se494S22315268
- EstcourtLJStanworthSJDoreeCHopewellSTrivellaMMurphyMFComparison of different platelet count thresholds to guide administration of prophylactic platelet transfusion for preventing bleeding in people with haematological disorders after myelosuppressive chemotherapy or stem cell transplantationCochrane Database Syst Rev201511CD010983
- LeeAYLevineMNBakerRILow-molecular-weight heparin versus a coumarin for the prevention of recurrent venous thromboembolism in patients with cancerN Engl J Med2003349214615312853587
- CarrierMKhoranaAAZwickerJNobleSLeeAYManagement of challenging cases of patients with cancer-associated thrombosis including recurrent thrombosis and bleeding: guidance from the SSC of the ISTHJ Thromb Haemost20131191760176523809334
- EasawJCShea-BudgellMAWuCMCanadian consensus recommendations on the management of venous thromboembolism in patients with cancer: part 2 – treatmentCurr Oncol201522214415525908913
- ManthaSMiaoYWillsJParameswaranRSoffGAEnoxaparin dose reduction for thrombocytopenia in patients with cancer: a quality assessment studyJ Thromb Thrombolysis201743451451828205078
- VarmaSYanamandraUKhadwalAHigh risk APML treated successfully with four cycles of ATO and ATRA combination in resource constrained settingsBlood2015126233322
- KalkEGoedeARosePAcute arterial thrombosis in acute promyelocytic leukaemiaClin Lab Haematol200325426727012890169
- YanadaMMatsushitaTSuzukiMDisseminated intravascular coagulation in acute leukemia: clinical and laboratory features at presentationEur J Haematol200677428228716856920
- UchiumiHMatsushimaTYamaneAPrevalence and clinical characteristics of acute myeloid leukemia associated with disseminated intravascular coagulationInt J Hematol200786213714217875527
- De StefanoVSoràFRossiEThe risk of thrombosis in patients with acute leukemia: occurrence of thrombosis at diagnosis and during treatmentJ Thromb Haemost2005391985199216102104
- VuKLuongNVHubbardJA retrospective study of venous thromboembolism in acute leukemia patients treated at the University of Texas MD Anderson Cancer CenterCancer Med201541273525487644
- RashidiASilverbergMLConklingPRFisherSIThrombosis in acute promyelocytic leukemiaThromb Res2013131428128923266518
- TallmanMSAbutalibSAAltmanJKThe double hazard of thrombophilia and bleeding in acute promyelocytic leukemiaSemin Thromb Hemost200733433033817525890
- BrecciaMAvvisatiGLatagliataROccurrence of thrombotic events in acute promyelocytic leukemia correlates with consistent immunophenotypic and molecular featuresLeukemia2007211798316932337
- ZuckermanTGanzelCTallmanMSRoweJMHow I treat hematologic emergencies in adults with acute leukemiaBlood2012120101993200222700723
- FalangaAAlessioMGDonatiMBBarbuiTA new procoagulant in acute leukemiaBlood19887148708753355894
- NawrothPPHandleyDAEsmonCTSternDMInterleukin 1 induces endothelial cell procoagulant while suppressing cell-surface anticoagulant activityProc Natl Acad Sci U S A19868310346034643486418
- BevilacquaMPPoberJSMajeauGRFiersWCotranRSGimbroneMARecombinant tumor necrosis factor induces procoagulant activity in cultured human vascular endothelium: characterization and comparison with the actions of interleukin 1Proc Natl Acad Sci U S A19868312453345373487091
- GreenoEWBachRRMoldowCFApoptosis is associated with increased cell surface tissue factor procoagulant activityLab Invest19967522812898765328
- KwaanHCRegoEMRole of microparticles in the hemostatic dysfunction in acute promyelocytic leukemiaSemin Thromb Hemost201036891792421049391
- BennettBBoothNACrollADawsonAAThe bleeding disorder in acute promyelocytic leukaemia: fibrinolysis due to u-PA rather than defibrinationBr J Haematol19897145115172496742
- SakataYMurakamiTNoroAMoriKMatsudaMThe specific activity of plasminogen activator inhibitor-1 in disseminated intra-vascular coagulation with acute promyelocytic leukemiaBlood1991779194919571708294
- MenellJSCesarmanGMJacovinaATMcLaughlinMALevEAHajjarKAAnnexin II and bleeding in acute promyelocytic leukemiaN Engl J Med199934013994100410099141
- KwaanHCWangJWeissIExpression of receptors for plasminogen activators on endothelial cell surface depends on their originJ Thromb Haemost20042230631214995994
- LavalléeVPMarquisMBordeleauMETranscriptional landscape of APL identifies aberrant podoplanin expression as a defining feature and missing link for the bleeding disorder of this diseaseBlood2016128221075
- OudijkEJNieuwenhuisHKBosRFijnheerRElastase mediated fibrinolysis in acute promyelocytic leukemiaThromb Haemost200083690690810896247
- FranchiniMDi MinnoMNCoppolaADisseminated intravascular coagulation in hematologic malignanciesSemin Thromb Hemost201036438840320614391
- RundeVAulCHeyllASchneiderWAll-trans retinoic acid: not only a differentiating agent, but also an inducer of thromboembolic events in patients with M3 leukemiaBlood19927925345351730098
- CaoMLiTHeZPromyelocytic extracellular chromatin exacerbates coagulation and fibrinolysis in acute promyelocytic leukemiaBlood2017129131855186428053193
- BarbuiTFalangaADisseminated intravascular coagulation in acute leukemiaSemin Thromb Hemost200127659360411740683
- LibourelEJKlerkCPvan NordenYDisseminated intravascular coagulation at diagnosis is a strong predictor for thrombosis in newly diagnosed acute myeloid leukemiaBlood2016128141854186127354723
- ManthaSGoldmanDADevlinSMDeterminants of fatal bleeding during induction therapy for acute promyelocytic leukemia in the ATRA eraBlood2017129131763176728082441
- PlatzbeckerUAvvisatiGCicconiLImproved outcomes with retinoic acid and arsenic trioxide compared with retinoic acid and chemotherapy in non-high-risk acute promyelocytic leukemia: final results of the randomized Italian-German APL0406 trialJ Clin Oncol201735660561227400939
- SanzMAGrimwadeDTallmanMSManagement of acute promyelocytic leukemia: recommendations from an expert panel on behalf of the European LeukemiaNetBlood200911391875189118812465
- HashimotoSKoikeTTatewakiWFatal thromboembolism in acute promyelocytic leukemia during all-trans retinoic acid therapy combined with antifibrinolytic therapy for prophylaxis of hemorrhageLeukemia199487111311158035603
- DesboroughMHadjinicolaouAVChaimaniAAlternative agents to prophylactic platelet transfusion for preventing bleeding in people with thrombocytopenia due to chronic bone marrow failure: a meta-analysis and systematic reviewCochrane Database Syst Rev201610CD01205527797129
- EstcourtLJDesboroughMBrunskillSJAntifibrinolytics (lysine analogues) for the prevention of bleeding in people with haematological disordersCochrane Database Syst Rev20163CD00973326978005
- Martí-CarvajalAJAnandVSolàITreatment for disseminated intravascular coagulation in patients with acute and chronic leukemiaCochrane Database Syst Rev20156CD008562
- OberoiSLehrnbecherTPhillipsBLeukapheresis and low-dose chemotherapy do not reduce early mortality in acute myeloid leukemia hyperleukocytosis: a systematic review and meta-analysisLeuk Res201438446046824472688
- Van de LouwAEffect of leukapheresis on blood coagulation in patients with hyperleukocytic acute myeloid leukemiaTransfus Apher Sci201756221421928041822
- ThachilJFalangaALeviMLiebmanHDi NisioMManagement of cancer-associated disseminated intravascular coagulation: guidance from the SSC of the ISTHJ Thromb Haemost201513467167525556711
- CasiniAFontanaPLecompteTPThrombotic complications of myeloproliferative neoplasms: risk assessment and risk-guided managementJ Thromb Haemost20131171215122723601811
- SmalbergJHArendsLRVallaDCKiladjianJJJanssenHLLeebeekFWMyeloproliferative neoplasms in Budd-Chiari syndrome and portal vein thrombosis: a meta-analysisBlood2012120254921492823043069
- HaguetHDouxfilsJMullierFChatelainCGrauxCDognéJMRisk of arterial and venous occlusive events in chronic myeloid leukemia patients treated with new generation BCR-ABL tyrosine kinase inhibitors: a systematic review and meta-analysisExpert Opin Drug Saf201716151227852118
- De StefanoVZaTRossiERecurrent thrombosis in patients with polycythemia vera and essential thrombocythemia: incidence, risk factors, and effect of treatmentsHaematologica200893337238018268279
- Quintás-CardamaAKantarjianHRavandiFBleeding diathesis in patients with chronic myelogenous leukemia receiving dasatinib therapyCancer2009115112482249019280591
- VarmaSSharmaAMalhotraPKumariSJainSVarmaNThrombotic complications of polycythemia veraHematology200813631932319055858
- JensenMKBrownPNLundBVNielsenOJHasselbalchHCIncreased platelet activation and abnormal membrane glycoprotein content and redistribution in myeloproliferative disordersBr J Haematol2000110111612410930987
- FalangaAMarchettiMEvangelistaVPolymorphonuclear leukocyte activation and hemostasis in patients with essential thrombocythemia and polycythemia veraBlood200096134261426611110700
- FalangaAMarchettiMVignoliABalducciDBarbuiTLeukocyte-platelet interaction in patients with essential thrombocythemia and polycythemia veraExp Hematol200533552353015850829
- WautierMPEl NemerWGanePIncreased adhesion to endothe-lial cells of erythrocytes from patients with polycythemia vera is mediated by laminin α5 chain and Lu/BCAMBlood2007110389490117412890
- DucheminJUgoVIanottoJCLecucqLMercierBAbgrallJFIncreased circulating procoagulant activity and thrombin generation in patients with myeloproliferative neoplasmsThromb Res2010126323824220656333
- BarbuiTCarobbioAFinazziGInflammation and thrombosis in essential thrombocythemia and polycythemia vera: different role of C-reactive protein and pentraxin 3Haematologica201196231531821173097
- JhaPKVijayASahuAAshrafMZComprehensive gene expression meta-analysis and integrated bioinformatic approaches reveal shared signatures between thrombosis and myeloproliferative disordersSci Rep201663709927892526
- BuddeUvan GenderenPJAcquired von Willebrand disease in patients with high platelet countsSemin Thromb Hemost19972354254319387201
- BuddeUDentJABerkowitzSDRuggeriZMZimmermanTSSubunit composition of plasma von Willebrand factor in patients with the myeloproliferative syndromeBlood1986686121312173535924
- MooreSFHunterRWHarperMTDysfunction of the PI3 kinase/Rap1/integrin αIIbβ3 pathway underlies ex vivo platelet hypoactivity in essential thrombocythemiaBlood201312171209121923243278
- AppelmannIKreherSParmentierSDiagnosis, prevention, and management of bleeding episodes in Philadelphia-negative myeloproliferative neoplasms: recommendations by the Hemostasis Working Party of the German Society of Hematology and Medical Oncology (DGHO) and the Society of Thrombosis and Hemostasis Research (GTH)Ann Hematol201695570771826916570
- TiedeAPriesackJWerwitzkeSDiagnostic workup of patients with acquired von Willebrand syndrome: a retrospective single-centre cohort studyJ Thromb Haemost20086456957618208537
- TefferiABarbuiTPolycythemia vera and essential thrombocythemia: 2017 update on diagnosis, risk-stratification, and managementAm J Hematol20179219410827991718
- MarchioliRFinazziGSpecchiaGCardiovascular events and intensity of treatment in polycythemia veraN Engl J Med20133681223323216616
- BarbuiTBarosiGBirgegardGPhiladelphia-negative classical myeloproliferative neoplasms: critical concepts and management recommendations from European LeukemiaNetJ Clin Oncol201129676177021205761
- HarrisonCNCampbellPJBuckGHydroxyurea compared with anagrelide in high-risk essential thrombocythemiaN Engl J Med20053531334516000354
- Alvarez-LarránAPérez-EncinasMFerrer-MarínFRisk of thrombosis according to need of phlebotomies in patients with polycythemia vera treated with hydroxyureaHaematologica2017102110310927686377
- MaugeriNGiordanoGPetrilliMPInhibition of tissue factor expression by hydroxyurea in polymorphonuclear leukocytes from patients with myeloproliferative disorders: a new effect for an old drug?J Thromb Haemost20064122593259816959024
- VerstovsekSMesaRAGotlibJA double-blind, placebo-controlled trial of ruxolitinib for myelofibrosisN Engl J Med2012366979980722375971
- SamuelsonBTVeselySKChai-AdisaksophaCScottBLCrowtherMGarciaDThe impact of ruxolitinib on thrombosis in patients with polycythemia vera and myelofibrosis: a meta-analysisBlood Coagul Fibrinolysis201627664865226569516
- KreherSOchsenreitherSTrappeRUProphylaxis and management of venous thromboembolism in patients with myeloproliferative neoplasms: consensus statement of the Haemostasis Working Party of the German Society of Hematology and Oncology (DGHO), the Austrian Society of Hematology and Oncology (ÖGHO) and Society of Thrombosis and Haemostasis Research (GTH e.V.)Ann Hematol201493121953196325307456
- BarbuiTDe StefanoVManagement of venous thromboembolism in myeloproliferative neoplasmsCurr Opin Hematol201724210811427875375
- CarrierMCameronCDellucACastellucciLKhoranaAALeeAYEfficacy and safety of anticoagulant therapy for the treatment of acute cancer-associated thrombosis: a systematic review and meta-analysisThromb Res201413461214121925457583
- YoungAPhillipsJHancocksHAnticoagulation therapy in selected cancer patients at risk of recurrence of venous thromboembolismThromb Res2016140Suppl 1S172S173
- Lexicomp: drug interactions Available from: https://www.upto-date.com/drug-interactions/?source=responsive_home#di-analyzeAccessed September 10, 2017
- GifkinsDMMatchoAYangHXuYGoodenMAWildgustMIncidence of major hemorrhage among CLL and MCL patients compared to the general elderly population: an analysis of the US SEER-Medicare linked databaseBlood2015126233268
- MahipalABilgramiSAcquired hemophilia in chronic lymphocytic leukemiaLeuk Lymphoma20074851026102817487748
- ByrdJCFurmanRRCoutreSETargeting BTK with ibrutinib in relapsed chronic lymphocytic leukemiaN Engl J Med20133691324223782158
- ByrdJCBrownJRO’BrienSIbrutinib versus ofatumumab in previously treated chronic lymphoid leukemiaN Engl J Med2014371321322324881631
- WhittleAMAllsupDJBaileyJRChronic lymphocytic leukaemia is a risk factor for venous thromboembolismLeuk Res201135341942121156322
- SimkovičMVodárekPMotyčkováMVenous thromboembolism in patients with chronic lymphocytic leukemiaThromb Res201513661082108626467608
- LipskyAHFarooquiMZTianXIncidence and risk factors of bleeding-related adverse events in patients with chronic lymphocytic leukemia treated with ibrutinibHaematologica2015100121571157826430171
- Imbruvica (ibrutinib) [package insert]Horsham (PA)Janssen Biotech2017
- BC Cancer AgencyBCCA protocol summary for treatment of previously untreated chronic lymphocytic leukemia or small lymphocytic lymphoma with chromosome 17 p deletion using ibrutinib2017 Available from: http://www.bccancer.bc.ca/chemotherapy-protocols-site/Documents/Lymphoma-Myeloma/ULYFIBRU_Protocol.pdfAccessed August 30, 2017
- LeongDPCaronFHillisCThe risk of atrial fibrillation with ibrutinib use: a systematic review and meta-analysisBlood2016128113814027247135
- ChaiKLRowanGSeymourJFBurburyKCarneyDTamCSPractical recommendations for the choice of anticoagulants in the management of patients with atrial fibrillation on ibrutinibLeuk Lymphoma201758122811281428504030
- JonesJAHillmenPCoutreSUse of anticoagulants and anti-platelet in patients with chronic lymphocytic leukaemia treated with single-agent ibrutinibBr J Haematol2017178228629128397242