Abstract
Intertrigo is a common inflammatory dermatosis of opposing skin surfaces that can be caused by a variety of infectious agents, most notably candida, under the effect of mechanical and environmental factors. Symptoms such as pain and itching significantly decrease quality of life, leading to high morbidity. A multitude of predisposing factors, particularly obesity, diabetes mellitus, and immunosuppressive conditions facilitate both the occurrence and recurrence of the disease. The diagnosis of candidal intertrigo is usually based on clinical appearance. However, a range of laboratory studies from simple tests to advanced methods can be carried out to confirm the diagnosis. Such tests are especially useful in treatment-resistant or recurrent cases for establishing a differential diagnosis. The first and key step of management is identification and correction of predisposing factors. Patients should be encouraged to lose weight, followed up properly after endocrinologic treatment and intestinal colonization or periorificial infections should be medically managed, especially in recurrent and resistant cases. Medical treatment of candidal intertrigo usually requires topical administration of nystatin and azole group antifungals. In this context, it is also possible to use magistral remedies safely and effectively. In case of predisposing immunosuppressive conditions or generalized infections, novel systemic agents with higher potency may be required.
Background
Intertrigo (intertriginous dermatitis) is a clinical inflammatory condition that develops in opposing skin surfaces in response to friction, humidity, maceration, or reduced air circulation.Citation1 This common skin disorder may be localized in a small area or involve larger surfaces. Lesions mostly develop in the neck, axilla, sub-mammary fold, and perineum, while other sites may also be involved including antecubital, umbilical, perianal, and interdigital areas as well as abdominal folds, eyelids, and the retroauricular area.Citation1–Citation3
The main factor in the development of the lesions is the mechanical friction on the skin that initially appears as a minimal erythema of the folds. Heat, reduced aeration, humidity, and maceration facilitate intertrigo. Although the condition may occur in both genders and all races, it is more common in diabetic obese individuals residing in hot and humid climates and in bed-ridden or elderly subjects. Urinary or fecal incontinence, inadequate personal hygiene, malnutrition, immunosuppression, and occlusive clothing are among other predisposing factors. Infants are also more likely to develop intertrigo due to drooling and short neck structure with prominent skin folds and a flexed position.Citation2 Many yeasts (particularly Candida) and molds, bacteria, and viral infectious agents may aggravate intertrigo by colonizing on the skin ().
Table 1 Infectious agents commonly found in intertrigo
Intertrigo may transform into a life-long chronic condition. It generally has an insidious onset with symptoms such as itching, pain, burning, or prickling sensations in skin fold areas.Citation7 Initially it presents itself as mildly erythematous papillae or plaques, quickly developing into an exudative erosion, fissures, macerations, and crusts. Erythema due to secondary infections, increased inflammation, papullo-pustules, and bad odor may develop.Citation1,Citation2,Citation7
Diagnosis of intertrigo and its complications are generally based on clinical manifestations and basic microbiological investigations. Microbiological cultures, potassium hydroxide (KOH) preparation, and Gram’s staining may guide the therapy when used for differentiating primary and secondary infections. Wood’s light examination can be used to identify a Pseudomonas, Malassezia, or erythrasma infection more quickly than would a culture. Despite the absence of a characteristic histopathological appearance, biopsy may be required in treatment-resistant cases of intertrigo in order to exclude other skin disorders such as psoriasis or lichen planus.Citation1,Citation2
Treatment of intertrigo should generally focus on the removal of predisposing factors, followed by appropriate use of topical or systemic antimicrobial agents as well as low-potency corticosteroids, if required.
Candida species
Taxonomically, Candida belongs to the phylum Ascomycetes, class Blastomycetes, order Cryptococcales, family Cryptococcaceae, and genus Candida.Citation31 These microorganisms have a diameter of 3–5 μm with a two-layered cell wall. Among more than 200 Candida species identified, only 15 may be associated with primary Candida infections.Citation32 Yeasts associated with Candida species can be found in the normal flora of human skin as well as in the mucosal covering of the gastrointestinal system, genito-urinary system, and respiratory system, in addition to the soil and a variety of foods.Citation31 Human colonization starts on the first day after birth and continues throughout the life-cycle as an opportunistic pathogen. Candida albicans is responsible for the majority of Candida-related noninvasive skin and mucosal candidiasis. However, a more than 50% increase in the incidence of non-albicans Candida species have recently been reported including C. glabrata, C. parapsilosis, C. tropicalis, C. krusei, C. lusitaniae, C. dubliniensis, and C. guilliermondii.Citation33 Each of these organisms exhibits characteristic virulence potential, antifungal susceptibility, and epidemiology.Citation34
Pathogenesis of candidal infection
C. albicans is a part of the normal flora in skin and genital and/or intestinal mucosa in 70% of healthy individuals.Citation35 Similar to many other opportunistic microorganisms of the skin, it exists as a commensal yeast in individuals with an intact immune system. It may lead to mucocutaneous or systemic infections under appropriate conditions.
Many Candida species are known to produce virulence factors like proteases. Species lacking these virulence factors are considered less pathogenic.Citation36–Citation39 Mechanisms of pathogenicity for Candida albicans may be summarized as below: secretion of hydrolases, molecules that mediate adhesion to with concomitant invasion into host cells, the yeast-to-hypha transition, biofilm formation, contact sensing and thigmotropism, phenotypic switching, and a variety of fitness attributes.Citation37
As is the case with all pathogens, the innate immunity of the skin represents the first step of the host defense against Candida.Citation40 Pathogenic invasion is a rather complex process and is initiated through disruption of the physical barrier by the transformation of Candida on the skin from yeast to hypha form. The capability of the yeasts to adhere to epithelium is a strong stimulant for the hyphal transformation and represents the most important step in tissue penetration.Citation37,Citation39–Citation41 Hyphae of C. albicans exhibit stronger epithelial adhesion than yeasts. More aggressive C. albicans species that have no ability to produce hyphae cannot attach to epithelium. Breakdown of the physical barrier with fungal invasion allows the spread of C. albicans to underlying vascular tissues, and then to distant organs. While transformation into the hypha form is a critical virulence factor both for epithelial penetration and phagocyte attachment of C. albicans, the yeast form is required for the development of systemic infection and dissemination.Citation38,Citation41
The contest between the host and Candida involves more specific and complex molecular mechanisms; the recognition of fungal cell wall components, activation of the immune cell signal pathways of the host, and release of cytokines and chemokines.Citation41 Formation of hyphae by C. albicans is also known to represent a very important factor that induces cytokine responses from epithelial cells.Citation42 The importance of cytokine and chemokine production has been underlined almost universally in all studies investigating the epithelial responses to C. albicans. Infected epithelial cells have been found to produce IL-lα/β, IL-6, G-CSF, GM-CSF, and TNFα, in addition to chemokines and cytokines such as RANTES, IL-8, and CCL20.Citation38,Citation43–Citation45
An examination of the immune mechanisms of the skin against C. albicans reveals that the defense barrier initiated with the stromal cells such as keratinocytes and melanocytes as well as the defense proteins released by these cells continues with the pattern recognizing receptors such as Dectin-1 and Toll-like receptor. Individuals with mutations or gene polymorphisms in pathways of these receptors have been found to be more susceptible to Candida infections.Citation46 The major mechanisms of innate immunity against candida infections include neuropeptides such as calcitonin gene-related peptide (CGRP) released in areas where the physical barrier is disrupted, IL-23 release from the dendritic cells, and activation of neutrophils recruited via IL-17 release from γδ T cells that is stimulated by the release of IL-23. On the other hand, IL-17 pathways represent an important component of the adaptive immunity against Candida infections through induction of effector and cytotoxic T lymphocytes.Citation35
Predisposing factors for candidal infections
The main determinant of the non-pathogenic commensal colonization versus pathogenic behavior is the balance between fungal proliferation and the innate and adaptive defenses of the host.Citation41 This balance is disturbed in favor of Candida as a result of various factors that predispose the individual to intertrigo ().
Table 2 Predisposing factors for Candida infections.
Clinical forms of candidal skin infection
C. albicans is responsible for approximately 80–90% of all skin infections caused by Candida species. It is an oval-shaped thermal dimorphic yeast with a diameter of 2–6 × 3–9 μm that can produce budding cells, pseudo-hyphae, and true hyphae. Skin infections encompass numerous forms with varying clinical terminology used to describe them. Although the clinical variants of skin infections have been clearly defined in the literature, currently no consensus regarding a standard classification system exists. In a 1996 classification by the American Academy of Dermatology’s Guidelines/Outcomes Committee,Citation47 the infections have been defined on the basis of their location and appearance as follows: cutaneous (intertriginous agents), oral (intra-oral mucosa), genital (vagina and penis), nail unit, and chronic mucocutaneous. However, different clinical classification systems have been proposed in many dermatological or other textbooks, or reviews.Citation31,Citation49–Citation51,Citation57,Citation58,Citation62–Citation65
Regardless of the size of the lesion, Candida infections involving skin folds should be classified under the candidal intertrigo heading, based on the definition intertriginous dermatitis ().
Table 3 Clinical presentations and locations of intertriginous candidal infections
Candidal intertrigo
C. albicans has a predilection for moist and macerated skin folds. The most frequent type of clinical presentation in hairless skin is intertrigo. Pruritic, erythematous, macerated skin areas are observed in intertriginous areas with satellite vesicopustules. The characteristic pustulae rapidly rupture, leading to the formation of collaret type erythematous surface, from which the necrotic epidermis may be easily removed.Citation9,Citation87
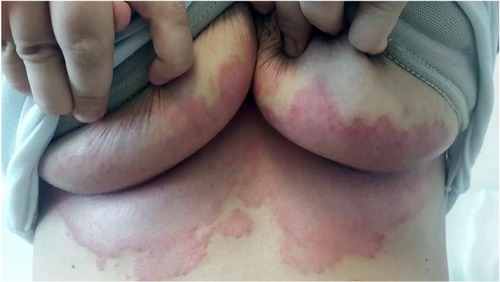
Candidal intertrigo of larger skin folds usually involves the axilla, gluteal, infra-mammary, and genito-crural fold (). The moisture and increased temperature on the surface of opposing skin folds provide a suitable medium for the growth of Candida and bacteria. Humid and hot weather, tight underclothes, poor hygiene, and inflammatory skin conditions such as psoriasis may increase the risk of candidal infections.Citation9 Diabetes mellitus and obesity represent the leading predisposing factor. Xerostomia, hyperhidrosis, occlusive wearings, occupational factors, use of corticosteroids or wide spectrum antibiotics, and immunosuppression including HIV infection may also increase the risk.Citation3,Citation51,Citation68,Citation88,Citation89
Diaper candidiasis
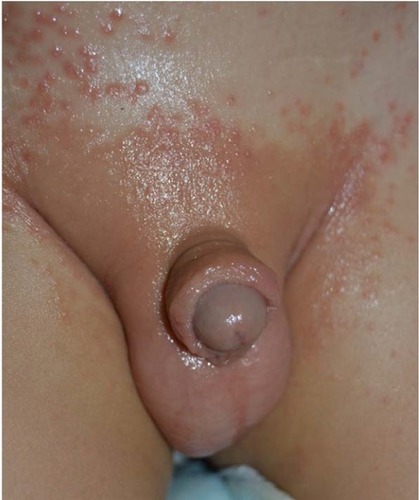
Diaper dermatitis is an acute and inflammatory skin reaction in the diaper area (). It is generally caused by the yeast colonizing in the gastrointestinal system. Chronic occlusion with wet clothes facilitates the infection. With prevalence ranges between 7 and 35%, it most commonly occurs in infants between 9 and 12 months of age, and may also be seen in adults requiring incontinence pads.Citation10 Infants with Candida diaper dermatitis generally have colonization in their gastrointestinal system with positive stool cultures for Candida. In infants with very low birth weight ≤ 1500 g, candidal colonization of the rectum and stools can be detected in 21–62.5%.Citation90
Lesions typically start in the perianal region, and spread over the perineum and inguinal area. Not all cases of diaper dermatitis may be caused by Candida, but diaper dermatitis due to candidiasis involves the skin folds. Multiple small erythematous desquamated pustules and satellite lesions extending along the borders of large maculae represent significant findings for diagnosis.Citation51,Citation88,Citation90
Granuloma gluteale infantum is a reaction developing Candida that causes opaque, reddish, irregular papules and/or nodules on the background of an erythematous surface in the diaper area. This is a reactive condition developing due to chronic irritant contact dermatitis caused by urinary incontinence or chronic diarrhea.Citation63,Citation89,Citation91 Diagnosis is generally straightforward, and biopsy may be required to rule out mast cell tumors, pseudolymphoma, lymphoma, and leukemic infiltration.Citation92
Angular cheilitis (perleche)
This condition is characterized by erythema, maceration, transverse fissures, and pain in the corners of the mouth. Although it is localized in the skin folds on the lips, it is classified within the group of oral candidal infections. Recurrent oral candidiasis is a common finding in HIV-infected subjects and is an important prognostic marker.Citation78 In HIV-positive patients, it may occur without other signs when the CD4+ lymphocyte count declines below 200/μL.Citation93 Frequently, it occurs due to use of lip liners in younger individuals, while skin sagging may be a causative factor in the elderly. Tooth loss, ill-fitting dental fixtures, and malocclusion represent other predisposing factors.Citation78,Citation88,Citation89 It may occur concomitantly with submental and cervical intertrigo, particularly in infants and debilitated patients with salivary discharge.
Erosio interdigitalis blastomycetica
Candidal intertrigo settling between the fingers, also termed as erosio interdigitalis blastomycetica (EIB), is an infectious condition that may develop by a candidal or polymicrobial infection. It usually affects the third and fourth fingers or toes due to physical inactivity, moisture, soap, water retention, or disruption of the skin barrier. The moisture under a ring may cause maceration and irritation, facilitating secondary infections with C. albicans. Lesions may cause oval, macerated, whitish lesions that may extend to the lateral borders. Generally, one or more fissures with a reddish-base are present in the middle of the lesions. As the disease progresses the macerated skin is peeled off, leaving an eroded area in which the protruding epidermis is surrounded by a white collar.Citation51 Microbiological cultures suggest that Candida and gram negative bacilli play a role in the development of this condition.Citation94 Very often, it develops as an occupational disease due to chronic maceration in individuals with chronic contact with water such as cooks, barmen, barmaids, dishwasher, housewives, or dentists. Diabetes mellitus is a predisposing disease for EIB, and EIB is an important cutaneous manifestation of diabetes.Citation9,Citation82 Thus, in patients diagnosed with EIB, a diagnosis of de novo or uncontrolled diabetes should be considered.Citation81 The differential diagnosis includes erythrasma and irritant contact dermatitis.Citation9,Citation82
Toe web candidiasis
It is an EIB-like intertriginous Candida infection, commonly occurring in the fourth interdigital space of the toes. It may be asymptomatic or cause mild symptoms. Moist working conditions and use of tight and closed shoes for prolonged periods of time may induce this condition.Citation2,Citation51 The skin exhibits white, macerated, and thickened epidermis. Its appearance is very similar to that of tinea pedis, and significant erythema and desquamation may occur as well.Citation2,Citation51
Perianal, perineal and intergluteal candidosis
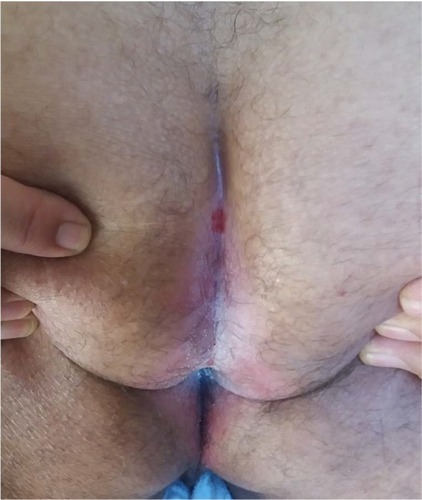
Perianal, perineal, and genitocrural areas are naturally moist areas of the skin.Citation9 Intertrigo may develop as an extension of vulvovaginal or intestinal candidiasis or due to spreading from one area to another.Citation9,Citation49,Citation64 Initially, it may present as severe perineal and anal pruritus accompanied by severe itching and burning sensation. An erythematous, oozy dermatitis together with maceration is observed in involved areas (). Also satellite lesions in the form of papules or pustules may be observed in the margins of erythematous-macerated plaques and eroded areas.Citation50,Citation84 Absence of satellite lesions does not rule out a diagnosis of candidiasis.Citation51
In cases where the cause of the condition is vulvovaginal or intestinal candidiasis, the disease may exhibit a recurrent and chronic course. Acute genitocrural intertrigo may also develop as a maculopapular eruption in HIV-infected subjects.Citation2
Differential diagnosis of candidal intertrigo
Numerous infectious agents, mainly bacteria and dermatophytes, may lead to similar clinical presentations in the areas affected by Candida intertrigo in addition to a variety of mucocutaneous disorders that can mimic the inflammation in the lesions. Some of these conditions have been presented in according to the involved site in intertrigo.
Table 4 Most common differential diagnoses for intertriginous dermatitis on skin-fold areas
Preventing recurrent infections
Preventive measures for recurrent intertrigo are used to support the therapy and represent the first step in management. The affected area(s) should be kept dry, clean, and cool with good airing and minimization of skin friction at the fold site. Good hygiene should be maintained in the infected area. Patients should be advised to wear cotton underwear, light clothing in hot and humid weather conditions, and should be warned regarding outdoor activities. Open shoes may help to prevent intertrigo of the toes.Citation2,Citation95
Maceration or irritation due to incontinence should be minimized or eliminated totally if possible. Cleansers, driers, emollients, and skin barrier creams may prove to be useful in such cases.Citation7
Laboratory diagnosis of intertrigo
The clinical appearance of candidal intertrigo usually suffices for a diagnosis. However, laboratory investigations and confirmatory tests may be required, particularly in chronic, resistant, and recurrent cases.Citation51 The simplest examination technique involves identification of the presence of pseudo-hyphae or yeast forms under direct microscopic examination of the samples obtained through scraping and smears that have been prepared with KOH and calcofluor white staining. Also, fluorescent microscopy and trypan blue examination may be used for that purpose. Differentiation between the species, assimilation and fermentation tests are applied on Candidal cultures.Citation58 More advanced techniques rarely required in the clinical practice include PCR, electron microscopy, and microchip diagnostic tests. Biopsy may be performed for the differential diagnosis from psoriasis as well as from dermatoses and dermatophytoses such as tinea. Identification of septa-free hyphae and yeast forms in PAS-stained histopathological samples is diagnostic for Candida.
Treatment of candidal intertrigo
Specific treatment of candidal intertrigo depends on the location, severity, and depth of the infection. Also, the treatment may be guided by the stage of the infection, i.e. acute, subacute, or chronic.Citation58 Initially, the active Candida infection should be medically managed, followed by skin drying measures to reduce the risk of recurrence, and finally by the correction of predisposing factors ().Citation62,Citation84
Topical anti-fungal agents are the mainstay of treatment in Candidal intertrigo. Topical anti-fungal agents represent the first step in management in mild cases of candidiasis. Nystatin and azole topical antifungals including miconazole, ketoconazole, or clotrimazole may be used twice daily for 2–4 weeks.Citation84 Time-tested magistral preparations may also aid in treatment. In acute lesions, Domeboro® solution (Moberg Pharma North America LLC, Cedar Knolls, NJ, USA), Castellani paint (ICM Pharma, Singapore), or vinegar–water solutions may be applied twice daily for 5–10 minutes. After drying, a mixture of zinc oxide, talc, and glycerin may be administered twice daily. In subacute lesions, after cleansing with benzoyl peroxide, Castellani stain, or vinegar, topical antifungals may be administered. In chronic lesions, rinsing lotion containing zinc-talk applied twice daily may be beneficial. Also, night-time application of antifungal/corticosteroid combinations may be recommended.Citation58 For itchy and painful lesions, an antifungal agent combined with corticosteroids (mostly hydrocortisone) may also be added to the treatment. In cases with local hyperhidrosis, anti-perspiration agents such as 20% aluminum chloride can be used in the long term. If maceration or moisture is present, astringent and antiperspirant solutions may be applied following antifungal creams.
In extensive, severe, and resistant intertrigo, systemic anti-fungal treatment is required. Oral fluconazole at a dose of 50–100 mg/day or itraconazole at a dose of 200 mg/day may be recommended for a total duration of 2–6 weeks until symptoms resolve. For pediatric cases, the recommended fluconazole and itraconazole doses are 6 mg/kg/day and 5–10 mg/kg/day, respectively.Citation84
Diaper candidiasis
Diaper candidiasis can be generally managed with topical antifungal agents. Nystatin ointment or powder is commonly used, with a clinical cure rate of approximately 85%.Citation90 Treatment with other azoles such as clotrimazole and miconazole may also give successful results. Despite similar mycological cure rates, miconazole is more effective than nystatin for symptomatic relief.Citation79,Citation80
For concomitant bacterial infections or irritation, combination of 1% hydrocortisone with antimicrobial agents such as sodium fusidate or clioquinole may be used. If recurrent diaper candidiasis is related to oral and intestinal colonization, addition of oral nystatin suspension may elicit a clinical response.Citation51
Angular cheilitis (perleche)
Angular cheilitis (perleche), when secondary to a Candida infection of the oral mucosa, should be brushed regularly, together with twice daily administration of an antiseptic oral rinse solution such as chlorhexidine gluconate (0.12%, suspension) or Gentian violet 0.5% solution.Citation59,Citation104 Patients with xerostomia should be encouraged to increase water consumption, and sugar-free lozenges should be advised to increase salivation.Citation59
Interdigital candidiasis (EIB and toe web candidiasis)
Special applicators may be recommended for drying the inter-toe spaces in interdigital candidiasis (EIB and toe web candidiasis).Citation9 Also, triggering factors should be avoided. For treatment, topical antifungal agents (azole antifungals) are generally adequate. Good outcomes have been reported with filtering paper adsorbed with Castellani stain.Citation51,Citation105 In recurrent or resistant cases, systemic itraconazole, terbinafine, or amorolfine may be used.
Correction of predisposing factors
Obese patients should be encouraged to lose weight, and diabetes should be under good control.Citation7,Citation81 Patients with large and sagging breasts may benefit from breast reduction surgery.Citation2,Citation106 For excessive sweating between the breasts, sweat-absorbing towels may be utilized. If present, predisposing factors (malocclusion, teeth loss, etc.) should be corrected in patients with angular cheilitis. For anatomical problems, the depth of skin folds may be reduced by injection of cosmetic filling material.Citation9 Topical or systemic administration of corticosteroids may also lead to chronic or recurrent candidiasis via immune suppression.Citation47,Citation62,Citation78 Wide spectrum antibiotics may also lead to Candida colonization and pathogenicity by disrupting the saprophytic flora of the skin and mucosal membranes. A detailed history of medication should be obtained to avoid unnecessary use of antibiotics and corticosteroids.Citation47,Citation50,Citation62,Citation64,Citation107 If high doses are involved, oral contraceptives with lower estrogen content should be preferred. For the recurrent intertrigo of the perianal area and its surroundings due to intestinal colonization, nystatin may be given.Citation32 Nutritional deficiencies such as iron and B2 deficiency may facilitate mucocutaneous candidiasis.Citation58,Citation59,Citation53 Patients wearing rings should be recommended to keep the skin under the ring dry and clean. Good aeration with open shoes may be recommended for toe web intertrigo. In cases with chronic incontinence, regular and absorbing hygienic products should be utilized for skin care.
Prognosis
Candidal intertrigo has a good prognosis in healthy immunocompetent individuals with no co-morbidites, and complete resolution of symptoms may be achieved with correct diagnosis and appropriate topical treatment. Ideally, in all cases with intertriginous candidiasis, all predisposing and provoking factors should be totally eliminated; if that is not possible, then these factors may be reduced. In more severe and recurrent cases of vaginal, oral, or chronic mucocutaneous candidiasis, systemic antifungals generally yield good results.
Disclosure
The authors report no conflicts of interest in this work.
References
- VakhariaPIntertrigo2017 http://emedicine.medscape.com/article/1087691Accessed August 1, 2017
- JannigerCKSchwartzRASzepietowskiJCReichAIntertrigo and common secondary skin infectionsAm Fam Physician200572583383816156342
- WolfROumeishOYParishLCIntertriginous eruptionClin Dermatol201129217317921396557
- BeureyJWeberMPerceboisGEtude clinique et mycologique des intertrigos des pieds [Clinical and mycologic study of intertrigo of the feet]Phlebologie19692217379 French4237853
- ColdironBMMandersSMPersistent Candida intertrigo treated with fluconazoleArch Dermatol199112721651661990982
- de AndradeMFNishinariKPuech-LeãoPIntertrigo em pacientes com linfedema de membro inferior. Correlacao clinico-laboratorial [Intertrigo in patients with lower limb lymphedema. Clinical and laboratory correlation]Rev Hosp Clin Fac Med Sao Paulo199853135 Portuguese9659735
- KalraMGHigginsKEKinneyBSIntertrigo and secondary skin infectionsAm Fam Physician201489756957324695603
- KatohTGuidelines for diagnosis and treatment of mucocutaneous candidiasisNihon Ishinkin Gakkai zasshi [Jap J Med Mycol.]2009504207212 Japanese
- MetinADilekNDemirserenDDFungal infections of the folds (intertriginous areas)Clin Dermatol201533443744726051058
- TüzünYWolfRBağlamSEnginBDiaper (napkin) dermatitis: a fold (intertriginous) dermatosisClin Dermatol201533447748226051065
- VeraldiSRapid relief of intertrigo-associated pruritus due to Candida albicans with isoconazole nitrate and diflucortolone valerate combination therapyMycoses201356Suppl 1414323574026
- BahmaeiMDehghanPKachueiRBabaeiHMohammadiRInterdigital intertrigo due to Fusarium oxysporumCurr Med Mycol201621434628681012
- BissanATIkenMDoumbiaMOu-KheddaNEl AlaouiMLmimouniBFusarioses superficielles a Fusarium solani chez un immunocompetent et un immunodeprime diagnostiquees a l’Hopital militaire de Rabat [Fusarioses to Fusarium solani in an immunocompetent and immunocompromised diagnosed in military hospital of Rabat]J Mycol Med2017273382386 French28478967
- DiongueKNdiayeMBadianeASIntertrigo interorteils a Fusarium solani a Dakar [Tinea pedis due to Fusarium solani in Dakar]J Mycol Med2015252155158 French25835156
- DiongueKNdiayeMDialloMAFungal interdigital tinea pedis in Dakar (Senegal)J Mycol Med201626431231627184614
- NéjiSTrabelsiHCheikhrouhouFFusarioses diagnostiquees au laboratoire d’un CHU en Tunisie: etude epidemiologique, clinique et mycologique [Fusariosis diagnosed in the laboratory of an UH in Tunisia: epidemiological, clinical and mycological study]J Mycol Med2013232130135 French.aw23725904
- RomanoCPresentiLMassaiLInterdigital intertrigo of the feet due to therapy-resistant Fusarium solaniDermatology1999199217717910559592
- VaronAGNouerSABarreirosGSuperficial skin lesions positive for Fusarium are associated with subsequent development of invasive fusariosisJ Infect2014681858923994063
- BazinJCHutinelBIntertrigos mycosiques et lymphangites [Fungal intertrigo and lymphangitis (author’s transl)]J Mal Vasc198052107108 French7462828
- KaracaSKulacMCetinkayaZDemirelREtiology of foot intertrigo in the District of Afyonkarahisar, Turkey: a bacteriologic and mycologic studyJ Am Podiatr Med Assoc2008981424418202333
- de GonzálezMIMendozaMBastardo de AlbornozMApitz-CastroREfectos del ajoeno sobre dermatofitos, Candida albicans y Malassezia furfur [Activity of ajoene on dermatophytes, Candida albicans and Malassezia furfur.]Rev Iberoam Micol1998154277281 Spanish18473517
- KatohTKagawaSIshimotoMMalassezia intertrigo, a new clinical entityMycoses198831115585623216878
- GoraniAOrianiAKleinEFVeraldiSCase report. Erythrasmoid pityriasis versicolorMycoses20014411–1251651711820268
- BeaulieuPLe GuyadecTPonties-LerouxBBoutchneiSGrosseteteGMilletPCas pour diagnostic: intertrigo a Pseudomonas aeruginoasa [A case for diagnosis: Pseudomonas aeruginosa intertrigo]Ann Dermatol Venereol19921193223225 French1605530
- BlockSLTricky triggers of intertrigoPediatr Ann201443517117624877486
- DekioIMatsukiSMoritaEHigh carriage rate of Staphylococcus aureus and Streptococcus agalactiae in nine cases of fungus-free intertrigo of the toe cleftInt J Dermatol201453448448622834698
- AdisenEOnderMViral infections of the folds (intertriginous areas)Clin Dermatol201533442943626051057
- BandyopadhyayDGhoshSKMucocutaneous features of Chikungunya fever: a study from an outbreak in West Bengal, IndiaInt J Dermatol200847111148115218986446
- CalikogluESoravia-DunandVAPerriardJSauratJHBorradoriLAcute genitocrural intertrigo: a sign of primary human immunodeficiency virus type 1 infectionDermatology2001203217117311586020
- YellJASinclairRMannSFlemingKRyanTJHuman papillomavirus type 6-induced condylomata: an unusual complication of intertrigoBr J Dermatol199312855755778389184
- López-MartinezRCandidosis, a new challengeClin Dermatol201028217818420347660
- PappasPGKauffmanCAAndesDRClinical Practice Guideline for the Management of Candidiasis: 2016 Update by the Infectious Diseases Society of AmericaClin Infect Dis2016264e1e50
- PfallerMAAndesDRDiekemaDJEpidemiology and outcomes of invasive candidiasis due to non-albicans species of Candida in 2,496 patients: data from the Prospective Antifungal Therapy (PATH) Registry 2004–2008PLoS ONE201497e10151024991967
- SullivanDJWesternengTJHaynesKABennettDEColemanDCCandida dubliniensis sp. nov.: phenotypic and molecular characterization of a novel species associated with oral candidosis in HIV-infected individualsMicrobiology1995141Pt 7150715217551019
- KashemSWKaplanDHSkin immunity to Candida albicansTrends Immunol201637744045027178391
- KühbacherABurger-KentischerARuppSInteraction of Candida species with the skinMicroorganisms20175232
- MayerFLWilsonDHubeBCandida albicans pathogenicity mechanismsVirulence201442119128
- NaglikJRMoyesDLWachtlerBHubeBCandida albicans interactions with epithelial cells and mucosal immunityMicrobes Infect20111312–1396397621801848
- HöfsSMogaveroSHubeBInteraction of Candida albicans with host cells: virulence factors, host defense, escape strategies, and the microbiotaJ Microbiol201654314916926920876
- BrownGDInnate antifungal immunity: the key role of phagocytesAnnu Rev Immunol20112912120936972
- QinYZhangLXuZInnate immune cell response upon Candida albicans infectionVirulence20167551252627078171
- MoyesDLRunglallMMurcianoCA biphasic innate immune MAPK response discriminates between the yeast and hyphal forms of Candida albicans in epithelial cellsCell Host Microbe20108322523520833374
- SchallerMMailhammerRGrasslGSanderCAHubeBKortingHCInfection of human oral epithelia with Candida species induces cytokine expression correlated to the degree of virulenceJ Invest Dermatol2002118465265711918712
- VillarCCKashlevaHMitchellAPDongari-BagtzoglouAInvasive phenotype of Candida albicans affects the host proinflammatory response to infectionInfect Immun20057384588459516040970
- WeindlGNaglikJRKaeslerSHuman epithelial cells establish direct antifungal defense through TLR4-mediated signalingJ Clin Invest2007117123664367217992260
- WangXvan de VeerdonkFLNeteaMGBasic genetics and immunology of Candida infectionsInfect Dis Clin North Am20163018510226897063
- Guidelines of care for superficial mycotic infections of the skin: mucocutaneous candidiasis. Guidelines/Outcome Committee. American Academy of DermatologyJ Am Acad Dermatol19963411101158543679
- De BrittoLJYuvarajJKamarajPPoopathySVijayalakshmiGRisk factors for chronic intertrigo of the lymphedema leg in southern India: a case-control studyInt J Low Extrem Wounds201514437738326353823
- HayRJAshbeeHRFungal infectionsGriffithsCBarkerJBleikerTChalmersRCreamerDRook’s Textbook of Dermatology9thChichester, West SussexJohn Wiley & Sons Inc201632.5632.70
- HessenMTWalshSRFerriFFMucocutaneous candidiasis2010 https://www.clinicalkey.com/-!/content/medical_topic/21-s2.0-1014515Accessed August 8, 2017
- JamesWDAndrewsGCBergerTGElstonDMDiseases resulting from fungi and yeastsJamesWDBergerTElstonDAndrews’ Diseases of the Skin: Clinical Dermatology12thPhiladelphia, PASaunders Elsevier2016285318
- LisboaCSantosADiasCAzevedoFPina-VazCRodriguesACandida balanitis: risk factorsJ Eur Acad Dermatol Venereol201024782082620002652
- LuSYPerception of iron deficiency from oral mucosa alterations that show a high prevalence of Candida infectionJ Formos Med Assoc2016115861962727133388
- MamathaKVShubhaUJainCMClinical evaluation of the efficacy of Khadiradi yoga avachoornana in Kachchu with special reference to genitoinguinal intertrigoAyu201031446146522048540
- NdiayeMTalebMDiattaBAEtiology of intertrigo in adults: a prospective study of 103 casesJ Mycol Med2017271283227554869
- RockwellPGAcute and chronic paronychiaAm Fam Physician20016361113111611277548
- RyanKJRayCGCandida, Aspergillus, Pneumocystis, and other opportunistic fungiRyanKJRayCGSherris Medical Microbiology6thNew YorkMcGraw-Hill Education Medical2014729743
- ScheinfeldNSCutaneous candidiasis2017 http://emedicine.medscape.com/article/1090632-overviewAccessed August 8, 2017
- SharonVFazelNOral candidiasis and angular cheilitisDermatol Ther201023323024220597942
- SilvermanRASchwartzRHStreptococcal intertrigo of the cervical folds in a five-month-old infantPediatr Infect Dis J201231887287322549438
- SparberFLeibundGut-LandmannSInterleukin 17-mediated host defense against Candida albicansPathogens20154360661926274976
- AsieduDKCandidiasis, cutaneousFerriFFFerri’s Clinical Advisor 2018: 5 Books in 1AmsterdamElsevier Science Health Science2017234235.e231
- HabifTPSuperficial fungal infectionsHabifTPClinical Dermatology: A Color Guide to Diagnosis and Therapy6thPhiladelphia, PASaunders2016487533
- HayRJFungal infections of the skinOlafssonJHHayRJAntibiotic and Antifungal Therapies in DermatologySwitzerlandSpringer2016157186
- KauffmanCACandidiasisGoldmanLSchaferAIGoldman-Cecil Medicine25thPhiladelphia, PAElsevier/Saunders201620792083.e2072
- MistiaenPvan Halm-WaltersMPrevention and treatment of intertrigo in large skin folds of adults: a systematic reviewBMC Nurs201091220626853
- WilmerENHatchRLResistant “candidal intertrigo”: could inverse psoriasis be the true culprit?J Am Board Fam Med201326221121423471936
- ValentiLTopical treatment of intertriginous candidal infectionMycoses200851Suppl 44445
- TerzievaKElsnerPA case of intertrigo resistant to treatment – what is your diagnosis?J Dtsch Dermatol Ges201513216917125631143
- SmithSMMilamPBFabbroSKGruAAKaffenbergerBHMalignant intertrigo: a subset of toxic erythema of chemotherapy requiring recognitionJAAD Case Rep20162647648127981223
- Santiago-et-Sanchez-MateosJLBeàSFernándezMPérezBHartoAJaénPBotulinum toxin type A for the preventive treatment of intertrigo in a patient with Darier’s disease and inguinal hyperhidrosisDermatol Surg200834121733173719076902
- NazzaroGVairaFCoggiAGianottiRA 42-year-old woman with a submammary intertrigoInt J Dermatol20135291035103623962260
- López-CorominasVYagüeFKnöpfelNStreptococcus pyogenes cervical intertrigo with secondary bacteremiaPediatr Dermatol2014312e71e7224456009
- ImamTHCassarinoDPatailHKhanNRefractory intertrigo in the right inguinal crease: challengeAm J Dermatopathol201739862928727599
- DowdMLAnsellLHHusainSGrossmanMEPapular acantholytic dyskeratosis of the genitocrural area: a rare unilateral asymptomatic intertrigoJAAD Case Rep20162213213427051853
- McKayCMcBridePMuirJPlantar verrucous carcinoma masquerading as toe web intertrigoAustralas J Dermatol2012532e20e2222571577
- Butragueño LaisecaLToledo Del CastilloBMarañón PardilloRCervical intertrigo: think beyond fungiRev Chil Pediatr201687429329426987275
- KirkpatrickCHChronic mucocutaneous candidiasisPediatr Infect Dis J200120219720611224843
- HoegerPHStarkSJostGEfficacy and safety of two different antifungal pastes in infants with diaper dermatitis: a randomized, controlled studyJ Eur Acad Dermatol Venereol20102491094109820553355
- BlancoDvan RossemKA prospective two-year assessment of miconazole resistance in Candida spp with repeated treatment with 025% miconazole nitrate ointment in neonates and infants with moderate to severe diaper dermatitis complicated by cutaneous candidiasisPediatr Dermatol201330671772423675632
- ChiriacAChiriacAEPintealaTFoiaLBrzezinskiPErosio blastomycetica interdigitale sign of Candidiasis and diabetes!Bangladesh J Med Sci2014131105106
- AdamsSPDermacase. Erosio interdigitalis blastomyceticaCan Fam Physician20024827127711889885
- GjessingHCIntertrigo; saerlig omtale av perianal, (retro) aurikulaer og periokulaer intertrigo [Intertrigo, with special consideration on perianal, retroauricular and periocular intertrigo]Tidsskr Nor Laegeforen19537312488490 Norwegian13102448
- ParkerERDellavalleRPRosenTOforiAOCandidal intertrigo2013 last updated Jul 2017; https://www.uptodate.com/contents/candidal-intertrigo/Accessed August 12, 2017
- TulipanLIntertrigo (chafing) treated with tannic acid and brilliant greenJ Am Med Ass19411161415181519
- DoganBKarabudakOTreatment of candidal intertrigo with a topical combination of isoconazole nitrate and diflucortolone valerateMycoses200851Suppl 4424318783567
- JanikMPHeffernanMPYeast infections: candidiasis and tinea (pityriasis) versicolorWolfKGoldsmithLAKatzSIGilchrestBAPallerASLeffellDJFitzpatrick’s Dermatology in General Medicine7thNew YorkMcGraw-Hill Medical200818221830
- VermaSHeffernanMFungal infectionsWolffKGoldsmithLKatzSGilchrestBPallerALeffellDFitzpatrick’s Dermatology in General Medicine7thNew YorkMcGraw-Hill Medical200818071821
- ElewskiBEHugheyLCSoberaJOHayRFungal diseasesBologniaJLJorizzoJLSchafferJVDermatology3rd[Edinburgh]Elsevier/Saunders201212511284
- RowenJLMucocutaneous candidiasisSemin Perinatol200327540641314626505
- RashidAArthroconidia as vectors of dermatophytosisCutis2001675 Suppl232311398259
- PryzbillaBRueffFContact dermatitisBurgdorfWHCBraun-FalcoOBraun-Falco’s Dermatology3rdHeidelbergSpringer2009491540
- ReissEShadomyHJLyonGMFundamental Medical MycologyHoboken, NJJohn Wiley & Sons2012250301
- LooDSCutaneous fungal infections in the elderlyDermatol Clin2004221335015018008
- DraijerLWFolmerHNHG-Farmacotherapeutische richtlijn IntertrigoHuisarts en Wetenschap20075013335
- BazexJIntertrigo. Diagnostic orientationRev Prat19924213168916921455143
- BenkalfateLZeinKle GallFChevrant-BretonJRivalanJle PogampPCalcified intertrigo, a rare cause of cutaneous calcinosisAnn Dermatol Venereol199512211–127897928729828
- CarletonAA case of pseudomembiunous intertrigoBr J Dermatol1943556154158
- CollierCWithin the fold: treatments of intertrigoJAAD2007562AB126
- HonigPJFriedenIJKimHJYanACStreptococcal intertrigo: an underrecognized condition in childrenPediatrics20031126 Pt 11427142914654624
- KeCLChenCCLinCTChenGSChaiCYChengSTFluvoxamine-induced bullous eruption mimicking hand-foot syndrome and intertrigo-like eruption: rare cutaneous presentations and elusive pathogenesisJ Am Acad Dermatol200655235535616844531
- KorverGERonaldHPetersenMJAn intertrigo-like eruption from pegylated liposomal doxorubicinJ Drugs Dermatol20065990190217039658
- PlazaAISanchoMIMilletPUErythematous, vesicular, and circinate lesions in a 78-year-old female – benign familial pemphigusAn Bras Dermatol201792343944029186274
- MillsopJWFazelNOral candidiasisClin Dermatol201634448749427343964
- SundaramSVSrinivasCRThirumurthyMCandidal intertrigo: treatment with filter paper soaked in Castellani’s paintIndian J Dermatol Venereol Leprol200672538638717050941
- ChadbourneEBZhangSGordonMJClinical outcomes in reduction mammaplasty: a systematic review and meta-analysis of published studiesMayo Clin Proc200176550351011357797
- DingXYanDSunWZengZSuRSuJEpidemiology and risk factors for nosocomial non-Candida albicans candidemia in adult patients at a tertiary care hospital in North ChinaMed Mycol201553768469026229153