?Mathematical formulae have been encoded as MathML and are displayed in this HTML version using MathJax in order to improve their display. Uncheck the box to turn MathJax off. This feature requires Javascript. Click on a formula to zoom.
?Mathematical formulae have been encoded as MathML and are displayed in this HTML version using MathJax in order to improve their display. Uncheck the box to turn MathJax off. This feature requires Javascript. Click on a formula to zoom.Abstract
Purpose
The formulation of topical ophthalmic products with appropriate therapeutic effect and patient compliance is a major challenge. To increase the efficiency of the ocular delivery of the drug, the enhancement of water solubility and the contact time of the drug on the surface of the cornea are necessary. In this work, prednisolone (PR)-containing eye drops were formulated with antimicrobial, mucoadhesive biopolymer and PR–cyclodextrin inclusion complex. This approach can be used for the development of innovative ophthalmic formulations.
Materials and methods
After adjusting the optimal physiological parameters, the amount of the required cyclodextrin for the highest penetration of PR was determined by dialysis membrane diffusion study. The viscosity, surface tension and mucoadhesion of the eye drops were measured. The microbiological effectiveness of zinc-hyaluronate (ZnHA) was investigated by a standard method of the European Pharmacopoeia.
Results
In this case, no significant difference of surface tension was measured in products with different amounts of cyclodextrin. According to the results of the tensile test, ZnHA as a mucoadhesive biopolymer improves the mucoadhesion of ophthalmic products. The antimicrobial stability of formulations preserved by ZnHA meets requirement B of the European Pharmacopoeia.
Conclusion
It can be stated that the innovative PR-containing compositions are suitable for producing mucoadhesive, properly preserved aqueous ophthalmic solutions with increased bioavailability attributes.
Introduction
Topical ocular drug delivery is restricted by barriers, such as eye blinking and lachrymal secretion, which result in low bioavailability after application. Solving this problem is a major challenge in the field of research and development and necessary because topically applied formulations have the highest patient adherence in the treatment of eye diseases.Citation1
In order to reach an optimal efficiency, the transcorneal penetration of the drug is important. The cornea is composed of five layers: the lipophilic epithelium, the hydrophilic stroma between Descemet’s membrane and Bowman’s layer, and the lipophilic endothelium. To complete the optimal transcorneal penetration, a balance in the hydrophilicity and lipophilicity of the drug and the vehicle is needed. The continuous secretion of tear fluid rapidly dilutes and washes out the applied eye drop and limits the contact time of drugs on the eye surface.Citation2
In ophthalmic surgery, glucocorticoid derivatives like prednisolone (PR), dexamethasone and fluorometholone are widely used for postoperative inflammation prophylaxis. Due to their low aqueous solubility, they are present on the market primarily in suspension formulations. When there is a risk of severe inflammation, especially after cornea transplantation, anti-inflammatory steroid therapy is needed by giving a subconjunctival or subretinal injection.Citation2,Citation3 Instead of these complicated and uncomfortable invasive applications, it would be more acceptable to use noninvasive, topical, water-soluble corticosteroid-containing eye drop formulations with higher efficiency.
One of the ways to increase efficiency on the eye surface is to solubilize the active pharmaceutical ingredient (API) in aqueous system, thereby ensuring that the optimal concentration of the drug appears near the epithelium of the cornea. Cyclodextrins (CDs) can solubilize lipophilic, water-insoluble drugs with suitable molecular size and structure, so they can be formulated in aqueous solutions. These cyclic oligosaccharides consist of α-(1,4) linked α-d-glucopyranose units. As a result of the lipophilic cavity of CD, an inclusion complex forms with the lipophilic drug molecules, due to thermodynamic interactions.Citation4–Citation7 This complex is soluble in water because of the hydrophilic external surface of CD and can be dissociated in the aqueous tear fluid. As a result, equilibrium is achieved between the complexed and non-complexed components. The determination of the optimal concentration of CD is important. With the proper amount of CD, the API can be in aqueous solution permanently, so a sufficient amount of drug molecules appears at the surface of the cornea, which induces the increase of drug permeation. If the concentration of CD is too low, it is not able to bring about the required water solubility of the drug, whereas too much CD decreases the amount of free, permeable drug molecules at the cornea.Citation8 The cytotoxicity of β-CD derivatives was investigated by several research groups on different cell lines. In ophthalmology, the hydroxypropyl derivatives of β- and γ-CDs, the randomly methylated β-CD and sulfobutyl-ether-β-cyclodextrin are tolerated because of the preferential cytotoxic properties against cornea epithelial cells.Citation4,Citation9,Citation10 Now, licensed CD-containing products are widely used in medical practice.Citation5,Citation6
The reflex mechanisms of the eye, such as blinking and lachrymal secretion, result in rapid drug elimination from the surface. To maintain the optimal, therapeutic drug level, more frequent application is needed, which can induce many side effects and decrease patient compliance. This problem can be solved by increasing the contact time of API on the surface of the cornea by increasing the viscosity with inserts, microspheres or mucoadhesive polymers. With longer residence, the penetration rate of API can be increased.Citation11 At a needlessly high viscosity level, the reflex mechanisms of the eye, blinking and lachrymation, are induced until the physiological viscosity of the tear is regained. Some viscosity increasing compounds have a mucoadhesive effect. With these materials optimal residual time can be achieved, without increasing viscosity to an unnecessarily high level. The mechanism of mucoadhesion involves tight contact and interpenetration between the mucoadhesive component and the proteoglycan chains of the mucin. Bioavailability can be improved through this mechanism.Citation12,Citation13 Hyaluronic acid is a linear anionic polysaccharide, a main component in the extracellular matrix of connective tissue. This biocompatible polymer can aid tissue manipulation and protect the corneal endothelium due to its proliferative effect. It interacts with mucin covering the conjunctival and corneal surfaces of the eye, and as a result ocular mucoadhesion is achieved.Citation14–Citation16
Benzalkonium chloride (BK) is a cationic surfactant additive, which is widely used as a microbiological preservative agent in eye drop formulations. BK may destroy the cell membrane of microorganisms, which results in an antimicrobial effect. Toxicity for corneal and conjunctival epithelial cells and incompatibility with contact lenses were reported earlier.Citation17–Citation19 BK causes DNA single- and double-strand breaks in corneal epithelial cells, so the barrier of the eye surface may be damaged. Allergic reaction, eye irritation and increased tear secretion may be caused by application.Citation17–Citation19 It is also known that resistance of Pseudomonas aeruginosa against BK appears due to decreasing the permeation through the cell wall.Citation20 The antimicrobial properties of Zn2+ ion-containing compounds are favorable in pharmaceutical formulations. Marketed products, like Ophylosa® (Gedeon Richter Plc, Budapest, Hungary) contain zinc-hyaluronate (ZnHA) and zinc-gluconate (ZnGlu) for replacing BK. The antimicrobial effect depends on the reactive oxygen species generating mechanism, the cell wall destabilizing effect of cytotoxic, dissolved Zn2+ ion in a water-based environment.Citation21 Zinc-containing polymers like ZnHA could be acceptable, combined with a zinc salt of gluconic acid, ZnGlu, to reach the suitable antimicrobial stability. Further investigation is needed to confirm the capability of these compounds as replacements of the unfavorable BK. ZnHA could be a useful antimicrobial and mucoadhesive additive in ophthalmic formulations.Citation22
The aim of this study was to develop an innovative, water-soluble PR-containing eye drop formulation with infrequent application, adequate microbiological stability and acceptable physiological (surface tension, pH, osmolality), rheological and mucoadhesive parameters using a CD inclusion complex, and preservative, mucoadhesive ZnHA and ZnGlu.
Material and methods
Materials
PR was purchased from Henan Lihua Pharmaceutical Company (Henan, China). Hydroxypropyl-β-cyclodextrin (HPBCD) was obtained from Wacker-Chemie GmbH (Munich, Germany), hydroxypropyl-γ-cyclodextrin (HPGCD) was kindly donated by Cyclolab Ltd. (Budapest, Hungary), ZnHA and ZnGlu from Gedeon Richter Plc (Budapest, Hungary). BK, sodium chloride (NaCl), boric acid and borax (for borate buffer) were obtained from Molar Chemical Ltd. (Halásztelek, Hungary). Mucin (porcine gastric mucin type II) was purchased from Sigma-Aldrich (St Louis, MO, USA). Lachrymal fluid of pH=7.4 was prepared by dissolving 2.2 g L−1 NaHCO3, 6.26 g L−1 NaCl, 1.79 g L−1 KCl, 96.4 mg L−1 MgCl2·6H2O and 73.5 mg L−1 CaCl2·H2O in distilled water, the pH being adjusted with 1 M HCl.Citation23
Methods
Phase solubility test
The phase solubility of PR was measured by adding it in excess amount to HPBCD- and HPGCD-containing solutions (purified water was used as a solvent) with different concentrations (0–150 mM) and allowing it to be intermixed for 48 hours. Thereafter, the solutions were filtered with a 0.45 µm membrane filter (Millex-HV Syringe Driven Filter Unit, 0.45 µm, EMD Millipore, Billerica, MA, USA) and analyzed with UV spectrophotometry (wavelength: 248 nm, Unicam UV/Vis Spectrometer, ATI Unicam, Cambridge, UK).
The type of diagrams and the ratio of complexes were determined and the stability constants of complexes (Ks) were calculated by EquationEquation (1)(1) :Citation24,Citation25
Preparation of products
The eye drops in the market contain 1% or 0.12% PR-acetate in suspension formulations. According to these products, we use 0.1% PR as API. Considering the probable improvement of the bioavailability, this amount is suitable and proper therapeutic effect can be expected. Defined amounts of HPGCD or HPBCD was dissolved in borate buffer and 0.5% ZnHA–ZnGlu-containing aqueous solutions. According to Horvát et al, this amount of ZnHA could not create a viscous, gel-formulation, therefore the unfavorable attributes of high viscosity are not expected.Citation26 PR was dissolved in these solutions. Products were put into an ultrasonic bath for 10 minutes. Osmolality was set with NaCl to about 300 mOsm kg−1; the pH was about 6.20 in every product. Every eye drop was prepared in aseptic environment.
Study of diffusion through dialysis membrane
The penetration of API depends on the concentration of CD. Overly high or low amounts of CD can cause a decreased absorption of API, therefore its determination is important. With the investigation of the diffusion of PR through a dialysis membrane, the optimal CD quantity as a function of drug penetration can be adjusted.
The amount of CD for the optimal penetration of API was determined by drug diffusion monitoring. Zellutrans/Roth cellulose dialysis membrane tube (10 mm wide, 6.4 mm diameter, MWCO: 12,000–14,000 D) was used for the experiment. The membrane pouches were closed with Spectra/Por Closures. The sample (2.00 mL) was injected into the pouches and put into 25 mL of borate buffer-containing aqueous acceptor phase (pH=7.4) tempered at 35°C. At various time intervals (15, 30, 60, 120, 180, and 240 minutes), 1.00 mL of the sample was removed from the acceptor phase and refilled with the buffered solution. The length of the measurement is reasonable, due to the possible increased retention on the surface of the eye. Four samples were measured parallel at the same time. The PR content was analyzed with UV spectrophotometry.
Viscosity
A Physica MCR 101 rheometer with cone-plate measuring device (Anton Paar, Graz, Austria, CP25-1, cone angle 0.997°, 25 mm diameter) was used for the measurement. The formulations were investigated at 25°C; the shear rate was increased from 0.1 s−1 to 100 s−1, the means of the data at 100 s−1 shear rate were calculated at the evaluation. The viscosity values were illustrated as a function of the concentration of CD derivatives.
Surface tension
The surface tension of the samples was measured with OCA 20 contact angle system (Dataphysics Instruments GmbH, Filderstadt, Germany) by analyzing the shape of pendant drop. The values of surface tension were determined with SCA 20/22 software module using the Young-Laplace equation.Citation27
Efficacy of antimicrobial preservation
The applicability of ZnHA–ZnGlu as ophthalmic preservative system was investigated vs BK, because the other components in the formulation could affect its antimicrobial effect. The antimicrobial effectiveness of the ophthalmic samples was determined according to the standards of the European Pharmacopoeia (EP). ZnHA–ZnGlu and BK as preservatives were tested on control strains, Staphylococcus aureus (ATCC 6538), P. aeruginosa (ATCC 9027) and Candida albicans (ATCC 10231). Inoculum suspensions of the microorganisms were prepared by using a sterile suspending fluid containing 9 gL−1 NaCl. The number of colony-forming units (CFU) was determined with plate count. The microbial count was about 108 CFU per milliliter. Preserved samples were inoculated with the suspensions of bacteria and fungus by adding 106 CFU per milliliter. The volume of the inoculated suspensions of microorganisms did not exceed 1% of the volume of the product. According to the standard method, three parallel samples were removed at zero hours and at appropriate intervals (6 hours, 24 hours, 7 d, 14 d, 28 d), and plated to Sabouraud-dextrose fluid agar (fungus) or tryptic soy fluid agar (bacteria). Bacteria-containing samples were incubated at 30°C–35°C for 24 hours and fungus-containing samples at 20°C–25°C for 48 hours. The reduction of these values was converted to log10 and compared with requirements A and B of the EP (EP-A, EP-B). The requirement of preservative is determined by the EP as the logarithmic reduction of CFU. The effectiveness needed against bacteria and fungus is managed separately. The decrease of CFU needs to be in accordance with the EP-A criteria. In cases when adverse drug reaction can appear with the A criteria, the EP-B criteria are acceptable.Citation28 The aim was to determine whether the preservative effect of ZnHA meets the requirements of EP in the presence of CD derivatives.
Mucoadhesion
The mucoadhesion of CD-containing eye drops was determined by the tensile test method, based on the measurement of the forces of detachment and the total work of adhesion needed to separate the surfaces, resulting from the area under the force–distance curve.Citation29,Citation30 Samples contained two types of CDs (HPBCD and HPGCD) prepared with and without ZnHA–ZnGlu. The purpose was to determine the effect of ZnHA on mucoadhesion and to establish if the presence of the type of CD has an effect in mucoadhesion. The measurement was performed with a TA.XT Plus Texture analyzer (ENCO, Spinea, Italy) instrument equipped with a 1 kg load cell and a cylinder probe with a diameter of 1 cm. The sample (20 µL) was attached to the cylinder probe and placed in contact with a filter paper disc wetted with 50 µL of an 8% w/w mucin dispersion or simulated lachrymal fluid (blank, pH=7.4). The mucin dispersion was made with simulated lachrymal fluid.Citation26,Citation31
A 2,500 mN preload was used for 3 minutes. The cylinder probe was moved upward to separate the sample from the substrate at a prefixed speed of 2.5 mm min−1.
Statistical analysis
One-way and two-way analysis of variances were used to compare the mean values. Statistical analysis was performed by GraphPad Prism five statistical software (GraphPad Software, Inc., La Jolla, CA, USA). The level of significance was set to P<0.05.
Results and discussion
Phase solubility test
The phase solubility of PR in HPBCD- and HPGCD-containing aqueous solutions (0–150 mM) is shown in .
Figure 1 Phase solubility diagrams of PR in aqueous HPBCD (■) and HPGCD (▲) solutions at 25°C.
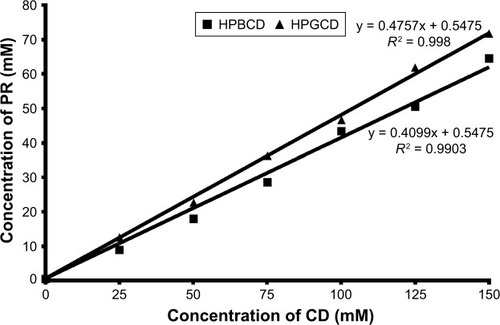
The solubility of PR was increased linearly by increasing the concentration of HPBCD or HPGCD. The diagrams are Higuchi AL type for both CDs, therefore the formation of 1:1 complexes can be assumed. In case of HPBCD, the apparent stability constant of the complex is 1,286.4 M−1, and the constant of the PR–HPGCD complex was measured to be 1,778.5 M−1.
It is stated that PR has greater affinity for complex-formation with HPGCD. With the equation of regression lines, the concentration of CD needed to solubilize the required amount of API can be determined. These calculated concentrations are the centers of intervals that were used in the drug diffusion study in case of both types of CD derivatives.
Study of diffusion through dialysis membrane
Eye drops with or without mucoadhesive polymer were formulated and examined. The concentrations of CD derivatives for the penetration of PR were optimized. The penetrated PR as a function of the concentration of CD is shown in .
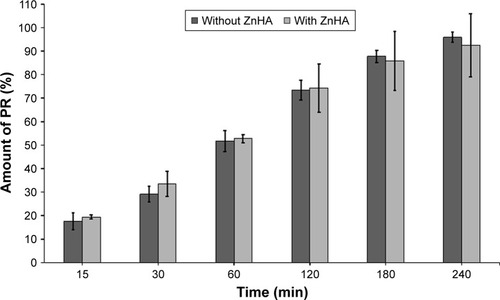
Figure 2 PR diffusion through dialysis membrane as a function of the concentration of HPGCD and HPBCD after 240 minutes.
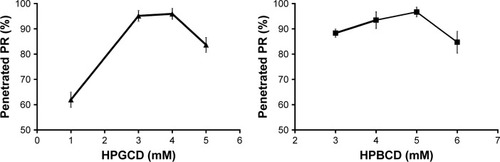
The results show that 4 mM HPGCD and 5 mM HPBCD induce the highest diffusion of PR through the dialysis membrane. Under the optimal CD concentration a part of free, hydrophobic drug remained in the pouches. Above the optimal CD level, the excess amount of CD keep the free PR in complex, therefore less amount of free API is detectable in the acceptor phase.
Thereafter, mucoadhesive ZnHA–ZnGlu additives were added to the eye drops, which ensure antimicrobial, preservative effect in the formulations. It was found that the application of biopolymer has no effect on the diffusion of PR. The same amount of drug penetrated through the dialysis membrane at each period in case of both compositions ().
Viscosity
The viscosity of ZnHA and PR-CD complex-containing ophthalmic formulations was measured. The results are shown in .
Table 1 Viscosity values of ZnHA-PR-HPGCD (I)- and ZnHA-PR-HPBCD (II)-containing products
According to previous reports, the viscosity should be under 30 mPa s.Citation32,Citation33 Above this level, blurred vision and discomfort appear, which result in faster elimination due to reflex mechanisms of the eye. The results show that the viscosity of our formulations is appropriate in the range of 9.2–24.2 mPa s.
Surface tension
The surface tension of normal tear is about 43 mN m−1.Citation34 It is not optimal if the surface tension of products is much higher than that of the lacrimal fluids because it has an impact on the therapeutic effect of pharmaceutics applied on the eye, through affecting the spreading of the eye drops on the ocular surface, although no regular critical parameter was found for the surface tension of eye drops in the EP. The surface tension of formulations preserved with ZnHA was measured by using an OCA 20 contact angle system. The results are shown in .
Table 2 Surface tension of ZnHA-PR-HPGCD (I)- and ZnHA-PR-HPBCD (II)-containing formulations
No significant difference was found between the values. The surface tensions of the eye drops are about 60 mN m−1, which is higher than the surface tension of lacrimal fluid. Ophthalmic products were investigated by Han et al, and the range of the surface tension values was between 34.3 mN m−1 and 70.9 mN m−1.Citation35–Citation37 According to this study, the surface tension of formulations meets the requirements for ophthalmic products.
Efficacy of antimicrobial preservation
In Samples I (with HPBCD) and II (with HPGCD), ZnHA–ZnGlu were used as preservative compounds. The results are shown in .
Table 3 Preservative effectiveness against Staphylococcus aureus, Pseudomonas aeruginosa and Candida albicans in Samples I and II
The logarithmic decrease of S. aureus was 1.5 after 6 hours, 2 after 24 hours, and no bacteria were detected in the samples after 7 days. In case of P. aeruginosa, the logarithmic decrease is higher at the earlier period, but the bacterium appeared in every sample. The logarithmic decrease of C. albicans was 1 after 6 hours, and no fungi were detected later. In summary, the preservative effect of ZnHA–ZnGlu-containing samples meets the EP-B criteria. The antimicrobial effectiveness of ZnHA–ZnGlu is lower against P. aeruginosa compared with the other microorganisms.
The microbiological stability of Samples III (with HPBCD) and IV (with HPGCD), which contained BK as a preservative agent, was tested ().
Table 4 Preservative effectiveness in Samples III and IV against Staphylococcus aureus, Pseudomonas aeruginosa and Candida albicans
The logarithmic decrease of S. aureus was 1 after 6 hours, 2 after 24 hours, and no bacteria were detected later in Sample III. For P. aeruginosa the logarithmic decrease was two and no change was detected later. In C. albicans-containing samples, no fungi were found after 7 days. In Sample IV, for S. aureus and C. albicans, the number of CFU was zero after 6 hours. In case of P. aeruginosa, the antimicrobial effect was lower due to the known resistance of the bacterium against BK. The microbiological stability of Samples III and IV meets the requirements of the EP. In Sample III, the antimicrobial effect of BK is lower than in Sample IV. It can be assumed that there is a competition between PR and BK for the cavity of HPBCD, so the preservative effect of BK is decreased by the inclusion complex formation.Citation38
According to the EP-B criteria, 0.5% ZnHA–ZnGlu compounds ensure the proper microbiological stability of eye drop formulations. In case of P. aeruginosa, the antimicrobial effect of the ZnHA–ZnGlu system is higher than the effect of BK. Considering these results with the irritative attribute of BK, application of ZnHA–ZnGlu as a preservative can be favorable in ophthalmic products.
Mucoadhesion
The measured adhesive force values are shown in . Lachrymal fluid was used as blank.
Figure 4 Adhesive force of eye drops with (white columns) and without mucin (black columns) (1, with HPBCD; 2, with HPGCD; 3, with HPBCD and ZnHA–ZnGlu; 4, with HPGCD and ZnHA–ZnGlu). The asterisks mark the significant difference between the results. The analysis was performed by the written statistical software and method.
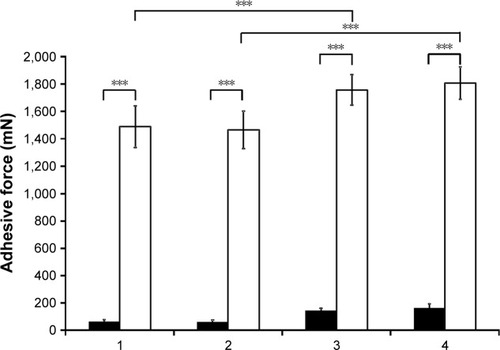
There is a large difference in the measured force between the blank and the mucin dispersion. All the samples show mucoadhesivity; samples prepared with ZnHA have significantly higher values than samples prepared without it. This proves the importance of the presence of ZnHA because the interpenetration between the ZnHA chains and mucin can be assumed. These samples can have better mucoadhesive properties and cause decreased administration frequency and a lower active ingredient concentration.
The type of CD does not play an important role in mucoadhesion because there is no significant difference between the samples prepared with HPBCD and HPGCD. According to the results, it can be established that ZnHA plays an important role in mucoadhesion.
Conclusion
To increase the bioavailability of steroid-containing ophthalmic products is a great challenge. Over the years, there have been numerous attempts to enhance the efficacy of eye drops. Our aim was to formulate PR-containing aqueous solutions by CD inclusion complex and to create mucoadhesive eye drops using antimicrobial ZnHA and ZnGlu, with suitable physiological parameters.
Aqueous solutions of PR were formulated by inclusion complexation with HPBCD and HPGCD. The investigation of the diffusion of PR through the dialysis membrane revealed that 5 mM of HPBCD, and 4 mM of HPGCD caused the highest penetration of API in in vitro circumstances. The addition of ZnHA and ZnGlu had no effect on the penetration properties. The measurement of viscosity showed that the 5-mM HPBCD- and 4-mM HPGCD-containing products had the lowest viscosity values, meeting the requirements of the EP. It was found that the concentration of CDs has no effect on the surface tension of the eye drops, and these values are optimal compared with previously investigated ophthalmic products. The mucoadhesive properties of ZnHA-containing formulations were proved with the tensile test, resulting in a higher retention time of the eye drop on the surface. The type of CD derivative has no influence on mucoadhesivity. During the preservative effectiveness test, it was proven that the ZnHA–ZnGlu combination is applicable as an antimicrobial, preservative compound. The microbiological stability of ZnHA-containing products meets the requirements of the EP in case of S. aureus, P. aeruginosa and C. albicans. It can be stated that BK with unfavorable toxicity properties for the corneal epithelial cells can be replaced with the more biocompatible ZnHA.
In summary, anti-inflammatory ophthalmic products containing PR with enhanced bioavailability were formulated in aqueous solutions by means of CD inclusion complex formation with optimal mucoadhesion and antimicrobial properties. Although further experiments such as toxicity and permeation studies are needed, these results are promising for the formulation of innovative eye drops with high therapeutic effect and sufficient patient compliance.
Acknowledgments
The project was supported by the European Union and co-financed by the European Social Fund: TAMOP-4.2.2.A-11/1/KONV-2012–0035. The authors would like to thank Cyclolab Ltd for their material support.
Disclosure
The author reports no conflicts of interest in this work.
References
- KaurIPKanwarMOcular preparations: the formulation approachDrug Dev Ind Pharm200228547349312098838
- LoftssonTStefánssonECyclodextrins in eye drop formulations: enhanced topical delivery of corticosteroids to the eyeActa Ophthalmol Scand200280214415011952479
- KunoNFujiiSRecent advances in ocular drug delivery systemsPolymers201131193221
- LoftssonTStefánssonEEffect of cyclodextrins on topical drug delivery to the eyeDrug Dev Ind Pharm1997235473481
- ChallaRAhujaAAliJKharRKCyclodextrins in drug delivery: an updated reviewAAPS PharmSciTech200562E329E35716353992
- LoftssonTDuchêneDCyclodextrins and their pharmaceutical applicationsInt J Pharm20073291–211117137734
- SzenteLSzejtliJHighly soluble cyclodextrin derivatives: chemistry, properties, and trends in developmentAdv Drug Deliv Rev1999361172810837706
- LoftssonTFriðriksdóttirHThórisdóttirS2-hydroxypropyl-β-cyclodextrin in topical carbonic anhydrase inhibitor formulationsEur J Pharm Sci199414175180
- Saarinen-SavolainenPJärvinenTAraki-SasakiKWatanabeHUrttiAEvaluation of cytotoxicity of various ophthalmic drugs, eye drop excipients and cyclodextrins in an immortalized human corneal epithelial cell linePharm Res1998158127512809706061
- KissTFenyvesiFBácskayIEvaluation of the cytotoxicity of beta-cyclodextrin derivatives: evidence for the role of cholesterol extractionEur J Pharm Sci201040437638020434542
- JärvinenKJärvinenTUrttiAOcular absorption following topical deliveryAdv Drug Deliv Rev1995161319
- AndrewsGPLavertyTPJonesDSMucoadhesive polymeric platforms for controlled drug deliveryEur J Pharm Biopharm200971350551818984051
- MansuriSKesharwaniPJainKTekadeRKJainNKMucoadhesion: a promising approach in drug delivery systemReact Funct Polym2016100151172
- GuterMBreunigMHyaluronan as a promising excipient for ocular drug deliveryEur J Pharm Biopharm2017113344927914235
- LaiJYTuIHAdhesion, phenotypic expression, and biosynthetic capacity of corneal keratocytes on surfaces coated with hyaluronic acid of different molecular weightsActa Biomater2012831068107922134163
- HorvátGGyarmatiBBerkóSzThiolated poly(aspartic acid) as potential in situ gelling, ocular mucoadhesive drug delivery systemEur J Pharm Sci20156711125445832
- ChapmanJMCheeksLGreenKInteractions of benzalkonium chloride with soft and hard contact lensesArch Ophthalmol199010822442462302109
- SwierczRHałatekTMajcherekWGrzelińiskaZWasowiczWToxic effect of benzalkonium chloride on animals and humansMed Pr200758213914217926503
- YeJWuHZhangHRole of benzalkonium chloride in DNA strand breaks in human corneal epithelial cellsGraefes Arch Clin Exp Ophthalmol2011249111681168721842132
- SakagamiYYokoyamaHNishimuraHOseYTashimaTMechanism of resistance to benzalkonium chloride by Pseudomonas aeruginosaAppl Environ Microbiol1989558203620402506813
- PasquetJChevalierYCouvalEBouvierDBolzingerMAZinc oxide as a new antimicrobial preservative of topical products: interactions with common formulation ingredientsInt J Pharm20154791889525527211
- IllésJJávorASzíjártóEZinc-hyaluronate: an original organotherapeutic compound of Gedeon Richter LtdActa Pharm Hung2002721152412426784
- SandriGBonferoniMCRossiSThermosensitive eyedrops containing platelet lysate for the treatment of corneal ulcersInt J Pharm20124261–21622248667
- HiguchiTConnorsKAPhase-solubility techniquesReilyCNAdvances in Analytical Chemistry and Instrumentation4New YorkInterscience1965117212
- ReptaAJAlteration of apparent solubility through complexationYalkowskiSHTechniques of Solubilization of DrugsNew YorkMarcel Dekker1985135157
- HorvátGBudai-SzűcsMBerkóSzCsányiEComparative study of nanosized cross-linked sodium-, linear sodium- and zinc-hyaluronate as potential ocular mucoadhesive drug delivery systemsInt J Pharm2015494132132826319587
- DataphysicsOperating Manual OCA (OCA 5, OCA 10, OCA 15, OCA 15 plus, OCA 20, OCA 30, OCAH 200 and OCAH 230)200271
- European Directorate for Quality of Medicines. Efficacy of Antimicrobial PreservationEuropean Pharmacopoeia9th edStrasbourgEuropean Directorate for the Quality of Medicines200651295130
- CappelloBde RosaGGianniniLCyclodextrin-containing poly(ethyleneoxide) tablets for the delivery of poorly soluble drugs: potential as buccal delivery systemInt J Pharm20063191–2637016650700
- WoertzCPreisMBreitkreutzJKleinebuddePAssessment of test methods evaluating mucoadhesive polymers and dosage forms: an overviewEur J Pharm Biopharm2013853 Pt B84385323851076
- SzűcsMSandriGBonferoniMCMucoadhesive behaviour of emulsions containing polymeric emulsifierEur J Pharm Sci2008344–522623518513929
- OechsnerMKeipertSPolyacrylic acid/polyvinylpyrrolidone bipoly-meric systems. I. Rheological and mucoadhesive properties of formulations potentially useful for the treatment of dry-eye-syndromeEur J Pharm Biopharm199947211311810234534
- SalzilloRSchiraldiCCorsutoLOptimization of hyaluronan-based eye drop formulationsCarbohydr Polym201615327528327561497
- TiffanyJMWinterNBlissGTear film stability and tear surface tensionCurr Eye Res1989855075152736956
- HanKWoghirenOEPrieferRSurface tension examination of various liquid oral, nasal, and ophthalmic dosage formsChem Cent J2016103127162532
- Hotujac GrgurevićMJuretićMHafnerALovrićJPepićITear fluid-eye drops compatibility assessment using surface tensionDrug Dev Ind Pharm201743227528227645109
- DoschiUXuJEffect of viscosity, surface tension and mucoadhesion on ocular residence time of lubricant eye dropsInvest Ophthalmol Vis Sci2009504641
- LoftssonTStefánsdóttirÓFriôriksdóttirHGuômundssonÖInteractions between preservatives and 2-hydroxypropyl-β-cyclodextrinDrug Dev Ind Pharm1992181314771484