Abstract
Objective
Lichen sclerosus (LS) is a chronic progressive inflammatory autoimmune-induced disease that primarily affects the epidermis and dermis of the external genital-anal region. Intense and recalcitrant pruritus is the hallmark of LS. Physical exam reveals thinning, hyperkeratosis, and parchment-like appearance. However, the classic symptom and signs of LS may not always be present and patients may be asymptomatic for pruritus. Hence, we describe 15 misdiagnosed cases with atypical clinical presentations. We believe that the absence of pruritus contributed to their initial misdiagnosis. The purpose of this paper is to increase awareness of atypical presentations of LS.
Methods
Data base review of de-identified clinical case pictures was performed. All patients had histopathology-confirmed diagnoses of LS. The data base file contains 800 cases of vulvovaginal disorders. The Institutional Review Board (IRB) considered that searching a de-identified data base of pictures did not require IRB approval.
Results
We identified 15 different atypical clinical cases. Patient ages were 18–75 years old. These patients were asymptomatic for pruritus and were misdiagnosed before they presented to the vulvovaginal specialized clinic.
Conclusion
Fifteen patients asymptomatic for pruritus with histopathology-confirmed diagnosis of LS were identified. They illustrate atypical clinical presentations that LS may have.
Introduction
Lichen sclerosus (LS) is a common unrecognized and misdiagnosed chronic progressive inflammatory vulvovaginal disease. The etiology is unclear, but some newer evidence suggests possible genetic predisposition or induction by autoimmune processes. The disease primarily affects the epidermis and dermis of the external anogenital region.Citation1–Citation5 LS may occur at any age but usually has a bimodal distribution occurring in prepubertal and postmenopausal women.Citation6 Intense and recalcitrant pruritus is the hallmark of LS. Pain is also a common complaint, which may present as dyschezia, dysuria, or dyspareunia. Affected patients may experience a significant decline in quality of life through severe discomfort and distress, as well as feelings of frustration and despair.Citation2
Upon clinical examination, we may observe thinning of the epidermis, hyperkeratosis, and parchment-like appearance. There could also be evidence of pale ivory-colored flat-topped papules that tend to coalesce into larger plaques.Citation7 Progressive atrophy of the epidermis may occur later, leading to scar tissue development with disappearance of the vulvar sulci, closure of the commissures, and phimosis of the clitoral hood.
The diagnosis of vulvar LS is based on the observation of the previously described characteristic clinical presentation and biopsy.Citation7 However, a handful of other disorders have similar presentations and are often confused with vulvar LS, which is why histological confirmation is highly recommended.
The first-line treatment for LS is topical high-potency steroids. Another commonly used therapy is pimecrolimus (topical calcineurin inhibitors).Citation4,Citation8 Failure to respond to treatment rarely occurs and may be caused by an incorrect diagnosis, a secondary problem (allergic contact dermatitis, bacterial or fungal infection), or the development of vulvar intraepithelial neoplasia or vulvar squamous cell carcinoma.Citation9 The addition of subdermal high-potency steroid injections in recalcitrant cases has been reported.Citation10 Surgery is reserved for cases with scarring that causes functional impairment.Citation4
We are presenting a series of 15 patients with histopathology confirmed anogenital LS to bring awareness to misdiagnosed atypical clinical presentations of this condition. We define these cases as being atypical because none of these patients presented with the classic symptom: pruritus.
Methods
Database review of clinical case pictures was performed. All patients had histopathology-confirmed diagnoses of LS with a lack of pruritus. Each picture was obtained after proper informed consent from patients attending general gynecology or vulvovaginal specialized faculty clinics for annual physical examinations or for unrelated vulvovaginal symptoms. The database contains 800 de-identified cases of vulvovaginal disorders with pertinent medical history classified as per International Classification of Diseases, 9th Revision (ICD 9) coding.
The Institutional Review Board (IRB) at Texas Tech Health Sciences Center determined that searching a de-identified data base of pictures did not require IRB approval.
Results
We identified 15 atypical clinical case presentations. Patient ages were 18–75 years old. These patients were asymptomatic for pruritus.
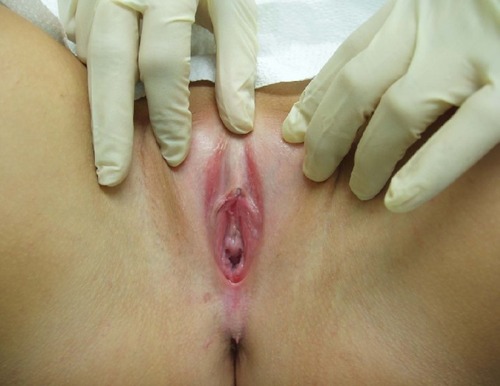
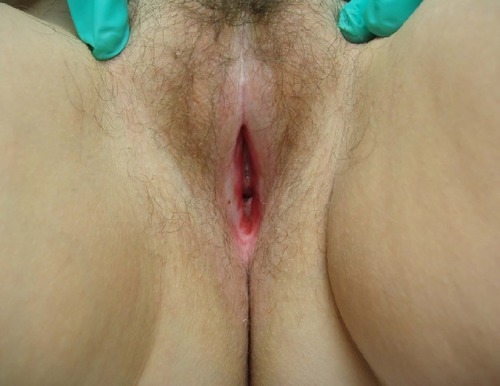
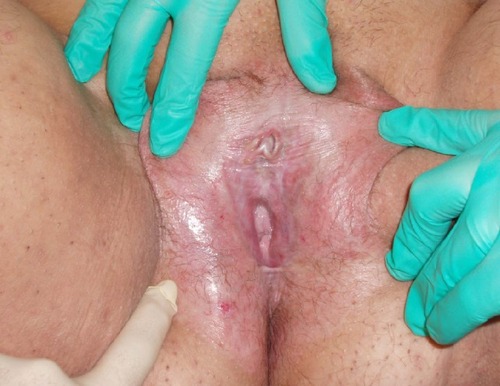
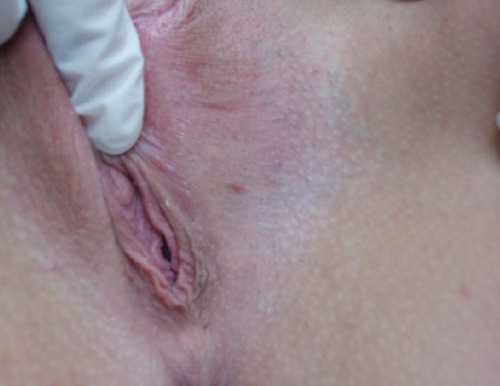
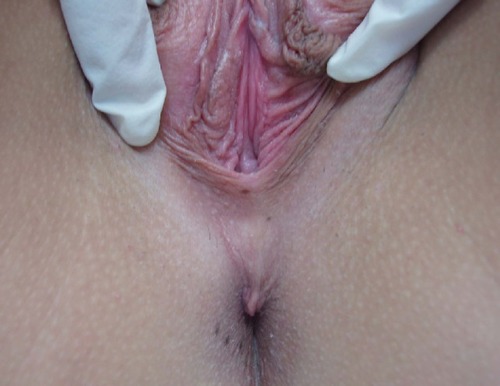
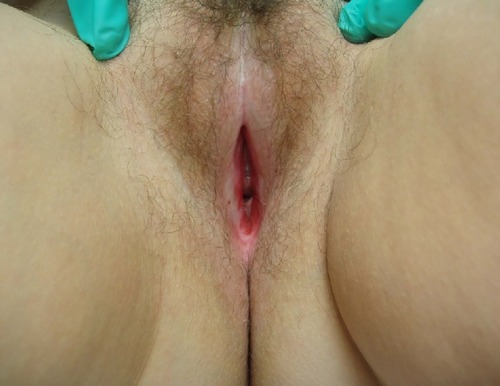
We had a wide array of atypical presentations, which included two patients complaining of sexual dysfunction. The first patient with sexual dysfunction complained of anorgasmia due to LS that involved the clitoral hood (). The second patient complained about dyspareunia resulting from LS related scarring and atrophy of the vaginal introitus ().
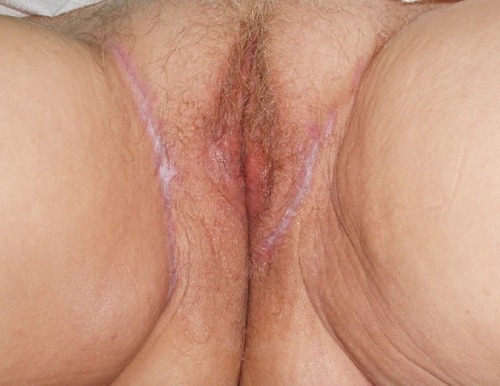
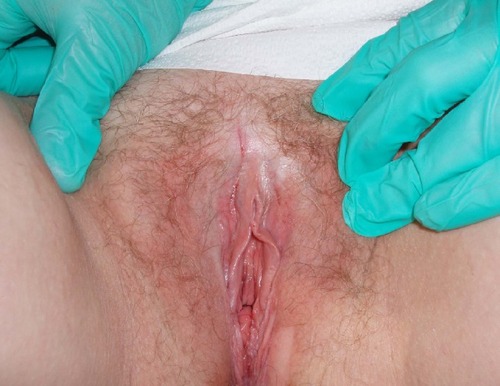
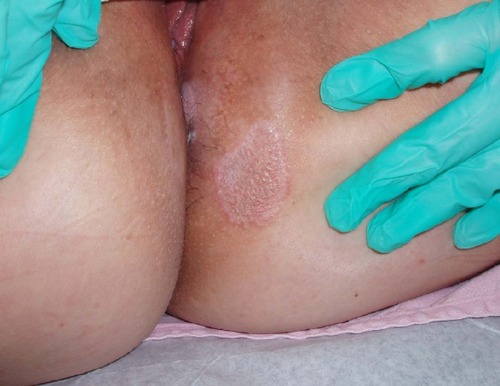
Additionally, three patients presented with complaints of tinea cruris or corporis. These patients were unresponsive to their prescribed antifungal therapy (, , and ).
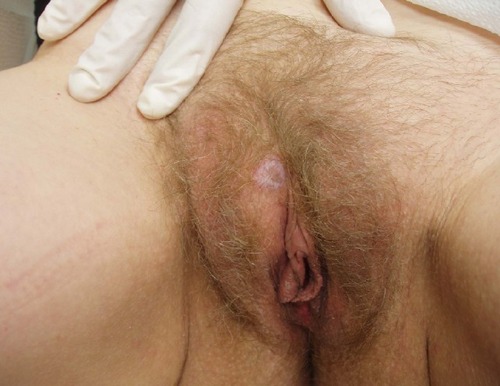
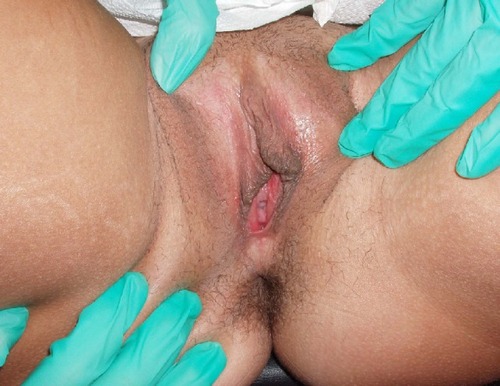
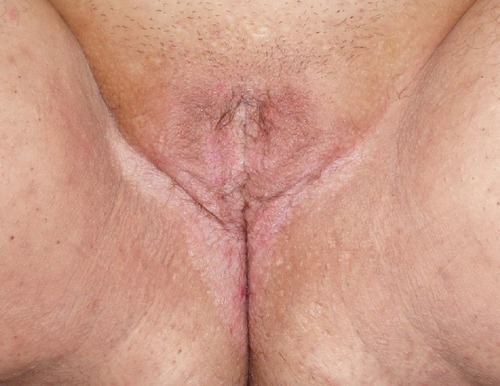
Other dermatological conditions that were inaccurately diagnosed included ulcerations and non-healing lesions. A patient with a non-healing ulcer of the vulva was tested extensively for infectious causes as well as autoimmune diseases before being referred to our specialty clinic for evaluation (). Another patient presented with similar complaints for a non-healing lesion in the suprapubic area (). Likewise, another patient was seen for evaluation of a pigmented lesion suspicious of malignancy despite being asymptomatic. The lesion was determined to be benign, but on physical examination her vulvar anatomy was already undergoing structural changes consistent with LS ().
Similarly, one patient complaining of excessive sweating in the perineum due to vulvar hyperhidrosis was diagnosed with LS (). Moreover, three of the patients included in this paper were evaluated for symptoms of recurrent lower urinary tract infections. One patient who complained of recurrent urinary infections had a biopsy that demonstrated evidence of LS and lichen planus (). Another patient who complained of recurrent urinary tract infections also had LS (). A third patient who presented with persistent symptoms of dysuria was repeatedly treated despite several normal urine analyses and cultures ().
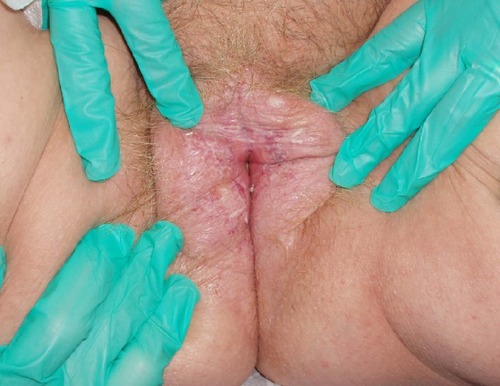
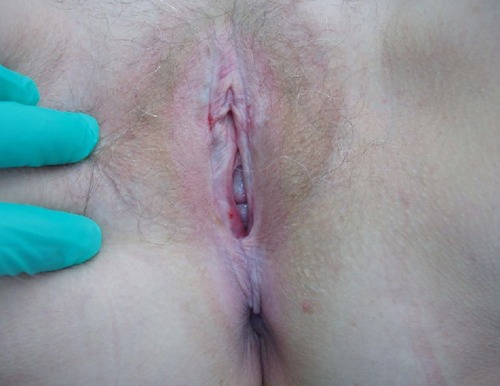
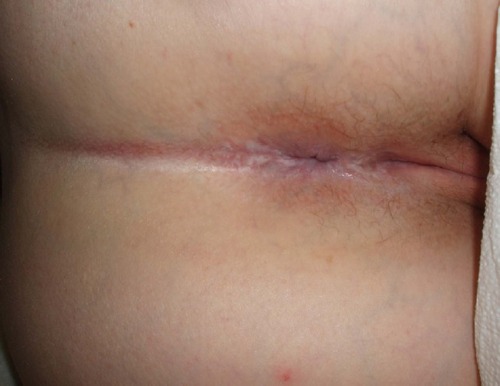
Finally, two patients presented with complaints of recurrent vulvovaginal bleeding. The first patient had numerous fissures on the vulva and vagina provoked by trauma from intercourse and exaggerated daily hygiene with an LS base (). The second patient suffered from recurrent vaginal and perianal bleeding. Her physical exam revealed a classic parchment-like appearance of the skin in the perianal and vulvar regions (). The last atypical case involved a patient who was squirting urine during micturition ().
All 15 patients described in this paper had a histopathology confirmed diagnosis of LS.
The majority of these patients reported a major improvement in their quality of life and their respective complaints and symptoms with the use of topical high potency steroids. The anorgasmic patient underwent clitoral hood circumcision that resolved the phimosis and improved her ability to achieve orgasm.
Conclusion
We are presenting a series of 15 patients with histopathology-confirmed vulvovaginal LS to report atypical clinical presentations of this medical condition. The unusual presentation of a lack of pruritus in these patients was probably a contributing factor that prevented earlier diagnosis and treatment.
Clinicians should consider LS and keep it in the differential diagnosis when faced with patients with vulvovaginal symptoms that are refractory to appropriate treatment of the previously diagnosed condition.
Disclosure
The authors do not have conflicts of interest to disclose. IRB approval waived due to de-identified database.
References
- ThomasRHRidleyCMMcgibbonDHBlackMMAnogenital lichen sclerosus in womenJ R Soc Med199689126946989014881
- Wehbe-AlamahHKornblauBLHadererJEricksonJSilent no more! The lived experiences of women with lichen sclerosisJ Am Acad Nurse Pract201224849950522845033
- ChanIOyamaNNeillSMWojnarowskaFBlackMMMcGrathJACharacterization of IgG autoantibodies to extracellular matrix protein 1 in lichen sclerosusClin Exp Dermatol200429549950415347336
- FistarolSKItinPHDiagnosis and treatment of lichen sclerosus: an updateAm J Clin Dermatol2013141274723329078
- CooperSMAliIBaldoMWojnarowskaFThe association of lichen sclerosus and erosive lichen planus of the vulva with autoimmune disease: a case-control studyArch Dermatol2008144111432143519015417
- McphersonTCooperSVulval lichen sclerosus and lichen planusDermatol Ther201023552353220868406
- FunaroDLichen sclerosus: a review and practical approachDermatol Ther2004171283714756888
- ChiCCKirtschigGBaldoMBrackenburyFLewisFWojnarowskaFTopical interventions for genital lichen sclerosusCochrane Database Syst Rev201112CD00824022161424
- MurphyRLichen SclerosusDermatol Clin201028470771520883914
- VentoliniGSwensonKGallowayMLichen Sclerosus: A 5-Year Follow-Up After Topical, Subdermal, or Combined TherapyJ Lower Genit Tract Dis2012163271274